The Dental Operating Microscope
The most valuable (and profitable) technology a dentist can own.
Donato Napoletano, DMD
While magnification in general undoubtedly offers many benefits to both the practitioner and patient, dental loupes do have some distinct limitations associated with them when compared to microscopes, the most obvious being that loupes are restricted to a single level of magnification. Additionally, by design, loupes are a convergent lens optical system, which basically means that the clinician’s eyes must converge to view the operative field, possibly resulting in eyestrain and fatigue, especially at higher levels of magnification or after prolonged periods of use. With loupes, as the level of magnification increases so does their weight as well as the need for an adjunctive light source to help improve visualization, which further adds additional weight to the system which, in turn, can result in increased strain and fatigue of head, neck, and back muscles after prolonged use. Compared to microscopes, however, the limitations of loupes are dramatically offset by their significantly lower cost and ease of portability.
Despite their higher price tags, however, when the dental operating microscope is fully integrated into a practice and used to its fullest potential, a return on investment can be realized rather quickly. The three key factors which contribute to a microscope’s income-generating ability is increased visualization, digital documentation capabilities, and improved ergonomics.
Advantages and Benefits of Dental Operating Microscopes
Increased Visualization
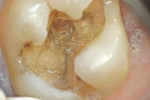
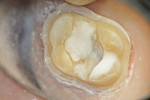
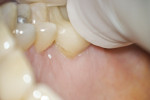
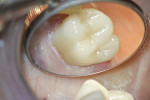
In addition to having up to six levels of magnification ranging from 2x to 20x available at one’s fingertips, illumination is a critical component in increasing visualization. Most microscopes are equipped with an integrated coaxial light source that allows for unobstructed, shadow-free illumination of the operating field. With coaxial illumination, the path of light is directed parallel to the microscope’s optical axis, which allows for significantly improved visualization of even the most difficult to access areas of the oral cavity.
With enhanced visualization, the clinician’s ability to diagnose problems in the earlier stages of a disease process is possible. Treatments also can be performed with a greater level of precision, thereby reducing the occurrence of failures and the need for redos. Enhanced visualization can also allow for treatment to be provided more comfortably to the patient because of lighter, more refined hand movements which occur naturally when one is accustomed to operating in a well-illuminated magnified field. Increased visualization can ultimately result in greater efficiency and productivity because less time is wasted with tactile exploration and confirmation that all decay has been removed. When one can see all areas of the mouth or of a preparation perfectly, the level of efficiency and precision in diagnosis and treatment naturally increases.
Digital Documentation Capabilities
This is perhaps the most significant advantage that microscopes offer over loupes, and where a significant return on investment can potentially be realized provided that they are fully integrated and used to their fullest potential. With the optional addition of a beam-splitting device, one is able to integrate various types of digital recording devices, such as an SLR and/or video camera. Digital documentation capabilities enable the clinician to efficiently capture and share with patients what is seen during an examination preoperatively, intraoperatively, and postoperatively.
Images captured during an examination, for instance, are an excellent communication and education tool in helping patients to better understand their diagnostic findings and why certain treatments may be necessary, especially for problems or conditions that produce no obvious symptoms to the patient. This can lead to greater rates of case acceptance, and significantly streamline the amount of time required in gaining it.
During treatment, images can be efficiently captured, shared, and stored in the patient’s chart. This is especially useful when unforeseen problems are encountered. This not only helps to increase a patient’s level of trust and confidence in the treating doctor (especially with newer patients), but can also aid in reducing one’s medical-legal risk.
Additionally, a live video source can be attached to the microscope and fed to a TV or computer monitor, strategically positioned so that it can be easily viewed by the dental assistant. When the assistant is able to see exactly what is being done during a procedure, not only does his or her level of efficiency increase, but the level of interest and motivation also rises dramatically since he or she tends to feel more involved during the procedure.
Once treatment is completed, a great way one can internally market one’s practice is by providing patients with preoperative, intraoperative, and postoperative color photographs of their treatment. This has the great potential of stimulating new patient referrals of friends and family members.
Improved Ergonomics
With dental microscopy, improved ergonomics is realized on many levels, the most obvious being improved posture. By operating in a more upright, comfortable posture, the operator is less likely to experience strain or fatigue of neck and back muscles and is, therefore, able to work comfortably for extended periods of time. This can enable the practitioner to provide more dentistry in fewer visits, increasing the clinician’s productivity and making for very happy patients. Ergonomics is also improved during digital documentation because intraoperative images can be captured very efficiently by the assistant so that the clinician does not have to stop treatment.
Integrating Dental Operating Microscopes
The successful integration of any technology usually requires a commitment of time and sometimes money. Motivation and persistence are also key ingredients for successful integration of technology. As is the case with any new technology or procedure, formal hands-on training will significantly decrease the amount of time required to attain complete, successful integration. It is important to realize that when incorporating anything new to one’s practice that problems will arise along the way. To minimize the occurrence and frequency of potential problems and ensure that the integration process proceeds smoothly, an implementation plan is critical.
A properly structured implementation plan should consist of a series of subplans that address many critical aspects of the integration process. These should include the following: a staff training and motivation plan, a scheduling plan, and a procedural execution plan.
The staff training and motivation plan should be deployed long before the technology even arrives or is installed in the office. In addition to educating the staff of all the potential benefits a technology may offer patients, the staff needs to understand that things may not proceed smoothly initially and that this is normal. The staff also needs to understand that they will be playing a pivotal role during the integration process and should be allowed to participate in helping to solve integration-related problems. This will not only help to keep staff members interested and motivated during the integration process, but they may ultimately offer input and suggestions that are of great value to the clinician. When implementing any new technology or procedure, many would agree that the practice staff is our strongest asset. Taking the necessary time to educate and motivate staff members is, therefore, time well spent.
The scheduling plan merely involves scheduling additional needed time for procedures during the initial phases of the integration process. Not allowing for sufficient time is perhaps the major reason why many technologies never get integrated fully and used to their fullest extent and potential. The drawback here, obviously, is an initial decrease in production. However, one needs to consider that if a substantial monetary investment in acquiring any technology is going to be made, the only way to ensure an acceptable rate of return from that investment is if the technology is used routinely, proficiently, and to its fullest potential. Without an appropriate investment in time, frustration levels are likely to rise and the integration of any technology will be close to impossible.
The procedural execution plan involves making a list of specific procedures organized by degree of difficulty with the simplest being performed first. In the case of dental operating microscopes, the arch and area of the mouth also needs to be taken under consideration. For instance, with microscopes, the maxillary arch and anterior segments of the oral cavity are the easiest to start with. A crown preparation on a lower second molar, for instance, may not be a desirable procedure or location of the mouth to start with.
An example of an acceptable procedural execution plan for a restorative dentist learning to integrate dental microscopy might include starting out with simple filling restorations in the facial anterior segments because this is the easiest area to visualize through direct vision. One should preferably start out using the lowest to low-medium powers of magnification before advancing to higher powers of magnification to allow sufficient time for one’s hand-eye coordination to adapt to operating under a magnified field. Once a point is reached where one feels comfortable in working under various levels of magnification in the facial anterior segments of the oral cavity, he or she can then proceed to crown or veneer preparations on the maxillary anterior segments where the use of a mirror would be necessary. As the use of the mirror becomes integrated with the use of a microscope in the anterior maxillary region, one can then advance posteriorly on the maxillary arch only, until an adequate level of proficiency is reached. The posterior mandibular region is generally considered to be the most difficult area of the mouth for an inexperienced microscope user to operate in and should, therefore, be avoided during the very early stages of the integration process.
While operating with a microscope does involve a bit of a learning curve, the author personally has not found it to be as difficult as some may perceive it to be; it only requires practice, persistence, and time. As mentioned earlier, formal training would help in significantly reducing the amount of time needed to fully integrate microscopes into a practice and may be well worth the additional cost for many new users or existing owners who have not been able to successfully integrate microscopes fully. A formal training course may also be a very valuable learning experience for those just contemplating adding dental microscopy to their practices before making an actual purchase. Dental microscopy may not be suitable for everyone, but until one tries, one may never know what they have been missing.
About the Author
Donato Napoletano, DMD
Private Practice
Middletown, New York