The Smile Makeover
What do you do when a patient says no to orthodontics, imposing challenging restrictions on an already complex esthetic reconstruction?
Marc Lazare, DDS
Very often, we can envision the possibilities just by looking at our patients. We use our artistic eye to figure out ways to help transform their smiles, and by extension, their confidence and their lives. Our training and experience enables us to visualize how a broader smile would eliminate the dark buccal corridor spaces found in a narrow arch form. We can picture the incisal edges of the maxillary teeth following the natural form of the lower lip, with individual shape and characteristics that would complement the patient’s personality and appearance. We understand the psychological benefits of a whiter, straighter smile, and how we can use the rule of golden proportions and other smile design principles (such as the positioning of the incisal edge placement, the development of pleasing width/height ratios, and the development of esthetic gingival contours) to help achieve them.1,2
The art of esthetic dentistry relies heavily on a team approach between the cosmetic dentist and the specialists to whom he or she refers. To achieve ideal esthetics, smile makeovers often require this interdisciplinary collaboration. So, in our attempts to strive for perfection, what does a practitioner do when the patient is presented with a comprehensive plan, but then says “no” to undergoing treatment with the recommended specialist?
This article explores how to work up and execute a challenging smile makeover that was made even more challenging with the restrictions imposed by the patient.
Realistic Expectations
Even the most beautiful smile makeover can be considered a failure if the patient’s expectations are not met. When the patient is handed a mirror to approve of the smile transformation, there is a brief moment where the clinician forgets to breathe while waiting for the nod of approval. Once the patient says “I love it” or “they look amazing,” the clinician can exhale and share in the excitement. Now, imagine feeling proud of the beautiful smile that has just been created, handing that patient a mirror, and then hearing, “I do not like it…it is just not me” or being told the restorations look too bulky, or too small, or just not white enough. Then what does the clinician do? What could have been done differently?
The very first thing that the dental practitioner should do when planning for a smile makeover is to take the time to listen to the patient’s desires and to find out what is liked and not liked about his or her smile. It sounds so simple, but many dentists rush through or ignore this step completely. Take digital photographs, perform digital imaging, and create an esthetic wax-up that can serve as a template for the temporary restorations. Have the patient see the ceramist for a cosmetic consultation and custom shade selection. Encourage the patient to bring in photographs of smiles that he or she likes. The more information gathered from the patient, the more the clinician can guide the laboratory to create what will meet or exceed the patient’s expectations. Clinical results are directly proportional to the communication skills clinicians have with their laboratory.3
Additionally, it is very important to check and document the patient’s occlusal scheme to see where the teeth make or do not make contact before the teeth are prepared. This way it is easier to achieve occlusal stability, especially when the patient was asymptomatic and occlusally stable before treatment began. If the patient’s previous bite was comfortable and asymptomatic, then the clinician would want to duplicate that. If the bite needed to be opened up, or modified, temporaries could be used to help figure out and achieve a balanced and healthy occlusion.
The clinician needs to determine if the patient requires crown lengthening, orthodontics, orthognathic surgery, etc, to achieve his or her vision of the perfect smile. If so, then the patient should be referred for the appropriate consultations. It is imperative that the patient understand the limitations that could arise by refusing to do the recommended adjunctive treatments. Informed consent must be given by the patient before starting treatment, and documented well in the chart.
Case Presentation
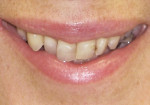
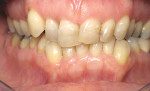
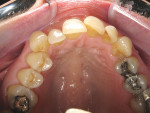
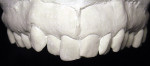
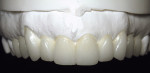
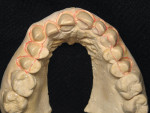
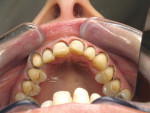
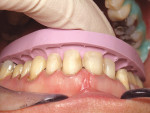
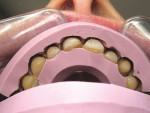
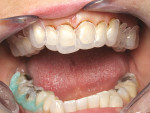
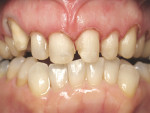
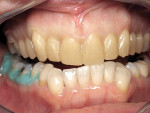
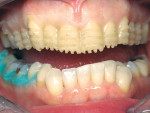
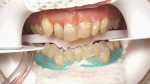
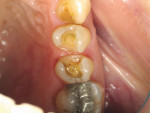
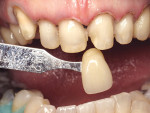
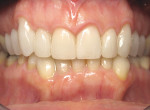
A 57-year-old woman presented to the author’s office with the chief complaint, “I am not happy with my smile, I would like it whiter and straighter” (Figure 1 and Figure 2). The patient was advised to see an orthodontist for a consultation to help correct the crowding, overlap, and position of her teeth and to give a more predictable end result with the veneers. The author was especially concerned with the prominence of tooth No. 6, which protruded buccally and cervically out of the arch form (Figure 3 and Figure 4). This tooth prevented her lip, on the right side, from hanging in the proper position at rest, causing an asymmetry when speaking and smiling. Orthodontics would enable that tooth to be brought back into the arch, allowing for better symmetry and harmony in her finished smile.
The patient had a class I molar relationship on both right and left sides, with a class II cuspid relationship on the left side. There was a 30% overbite, 2 mm of overjet, and maxillary and mandibular crowding with lingually inclined teeth in both arches. Additionally, she was in buccal crossbite on the mandibular left cuspid, second premolar, and first molar, with a maxillary midline that had shifted to the right 4 mm and a mandibular midline that had shifted to the left 4 mm.
It was predicted that she would need to undergo 18 to 24 months of orthodontic treatment to achieve the alignment objectives, followed initially by full-time retainers, and then slated for night time retention. The patient seemed hesitant to undergo orthodontics, and was then referred for a consultation with a periodontist to evaluate for gingival and osseous recontouring to create a more even gingival line when smiling. The patient was advised on how the periodontal tissues play an important role in establishing ideal smile esthetics. It was explained to her that in smile design, the labial gingival margin is a major determinant of the tooth smile display, as it helps to determine the length of anterior teeth and the smile proportion and symmetry.4
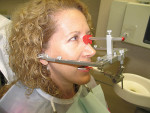
After consulting with these specialists, she decided that she would prefer not to have orthodontics at her age, nor undergo a surgical periodontal procedure. At this point she was educated enough to understand the limitations that she was imposing on her smile makeover. The next step was to take comprehensive records (including diagnostic impressions, bite records, a preoperative facebow record (Figure 5), a full-mouth series of x-rays, and a complete set of photographs) and to have the laboratory create an esthetic wax-up (Figure 6, Figure 7, Figure 8) to more accurately depict what could be achieved without enlisting the services of the specialists.
Case Evaluation
Visual, periodontal, and occlusal assessments were performed. The patient’s case was analyzed following the requirements for occlusal stability as outlined by Dawson,5 which include: stable stops on all teeth when in centric relation, anterior guidance in harmony with the movements within the envelope of function, full posterior disclusion in protrusive movement, and no posterior interferences on the working or non-working side in canine guidance. When the treatment planning sequence begins with esthetics, there should first be an appraisal of the maxillary central incisors relative to the upper lip.6 The author determined the length and horizontal edge position of her maxillary incisors, which would be tested and modified during the provisional stage as derived from this diagnostic wax-up. Taking time to set up this incisal edge position is one of the most important diagnostic steps, and saves time and headaches later on. An error in the incisal position can cause restorations to break and a sore musculature from an uncomfortable envelope of function.7 The author strived to create an incisal edge that would contact the inner vermillion border of the lower lip when pronouncing the letters “F” and “V.”8 The correct position would also allow for air to flow naturally between the upper and lower incisors when creating the “S” sound.9
In an effort to create a more youthful appearance, the patient’s smile was designed such that her two maxillary central incisors were just slightly longer than the laterals. Her cuspids supported the corners of her mouth, and were approximately the same length as the central incisors.10 The distals of her incisors were rounded to create a softer, more feminine appearance.
Once the diagnostic wax-up was created, putty stints were fabricated to guide in tooth preparation. Buccal and incisal putty stints were made to show proper reduction in those planes (Figure 9 , Figure 10 , Figure 11 ). A clear periodontal stint was made to guide gingival reshaping (Figure 12 and Figure 13). Additionally, a putty stint was fashioned from the wax-up to create a matrix for creating an exact replica to be used for the provisionals. The diagnostic wax-up, preparation model, and guides were fabricated by JK Dental Laboratory, and all served as a “cookbook” guide to verify esthetic design, phonetics (while wearing temporaries), and adequate tooth reduction to achieve restorative needs (Figure 14 and Figure 15).
Deep bleaching was performed on her lower arch before a custom shade was taken. The lower teeth were isolated and three rounds of in-office whitening were carried out without a light source to initiate the bleaching process and to condition her teeth for further whitening with her custom home trays (Figure 16). After 2 weeks of overnight whitening, the patient returned for a full in-office whitening treatment using ZOOM! Advanced Power (www.discusdental.com). Initially she was a D2 shade; after the initial in-office procedure she lightened to a C2 shade. She was then given the custom home trays and NiteWhite® (Discus Dental), which she used each night for 2 weeks. She achieved a B1 shade after using these trays, and then advanced to shade somewhere between BL4 and BL3 on the Ivoclar Vivadent bleached shade guide. Arrangements were made to have the patient meet the ceramist for a custom shade taking 2 weeks after bleaching was completed and her shade was stable.
The Restorative Phase
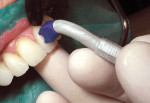
The old amalgam restorations were removed from teeth Nos. 12 and 13 to eliminate the possibility of any gray showing through the veneers (Figure 17). Upon close examination of the patient’s wax-up and preparation model, it was determined that the labial position of the maxillary right cuspid could make her smile transformation more challenging without the possibility of devitalizing the cuspid. The patient was then referred to the endodontist for preventative root canal therapy for tooth No. 6 in anticipation that this tooth would either undergo irreversible pulpitis or become hypersensitive from the aggressive tooth preparation necessary to bring it back into alignment. Tooth No. 6 was prepared for a 360° butt-joint ceramic crown, and teeth Nos. 4, 5, and 7 through 13 were prepared for porcelain veneers. A stump shade was taken and the photograph was sent to the laboratory (Figure 18) to allow for a predictable final shade result. The veneers and ceramic crown were positioned and seated with the Veneer Styx positioning tool (Cosmetic Innovations, Inc), and using a neutral shade of cement (Figure 19). Excess cement was removed, the contacts were checked with floss, and the occlusion was checked in all excursions. A nightguard was later fabricated to help the patient protect her investment.
Conclusion
Patients who seek esthetic dental services may have different perceptions of how their smile should look.11 It is important to present all of the treatment possibilities and limitations to the patient, including any and all possible sequella that can arise from either performing or not performing those recommended procedures. Patients should be encouraged to seek a consultation from the recommended specialties, even if they are not keen on going that route, to become educated and to develop realistic expectations of the outcomes that will arise from their decisions. Dentists should be aware that among patients seeking esthetic services, there is a difference between the perceived need and the normative need for treatment between the patient and the clinician.12 All recommendations and decisions should be well documented, and, when appropriate, signed off on by the patient. Once the parameters are set, any smile makeover that meets or exceeds realistic expectations will be considered a success (Figure 20 and Figure 21 ).
Disclosure
The author is the founder and president of Cosmetic Innovations, Inc, and the inventor of Veneer Styx, a product mentioned in this article.
Acknowledgment
The author would like to thank Dr. Raymond Mehlman for taking such wonderful care of his patient’s endodontic needs. Additionally, he would like to thank his ceramist, Peter Kouvaris, and the entire JK Dental Laboratory team for their guidance and support throughout the planning and execution of this challenging smile makeover.
References
1. Rufenacht CR. Fundamentals of Esthetics. Chicago, IL: Quintessence Publishing; 1990.
2. Levin EI. Dental esthetics and the golden proportion. J Prosthet Dent. 1978;40(3):244-252.
3. Griffen Jr JD. How to build a great partnership with the technician: simplified and effective laboratory communication. Contemporary Esthetics and Restorative Practice. 2006;10(7):26-34.
4. Bitter RN. The periodontal factor in esthetic smile design—altering gingival display. Gen Dent. 2007;55(7):616-622.
5. Dawson P. Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2006:345-349.
6. Spear F, Kokich VG, Mathews D. Interdisciplinary management of anterior dental esthetics. J Am Dent Assoc. 2006;137(2):160-169.
7. Hess L. The relevance of occlusion in the golden age of esthetics. Inside Dentistry. 2008; 4(2):36-44.
8. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Hanover Park, IL: Quintessence Pub. Co. 1994;21.
9. Dawson P. Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby. 2006;181.
10. Goldstein RE. Change Your Smile. Chicago, IL: Quintessence Publishing. 1984:6-22.
11. Jørnung J, Fardal Ø. Perceptions of patients’ smiles: A comparison of patients’ and dentists’ opinions. J Am Dent Assoc. 2007;138(12):1 544-1553.
12. Hamdan A. The relationship between patient, parent and clinician perceived need and normative orthodontic treatment need. Eur J Orthod. 2004;26(3):265-271.
About the Author
Marc Lazare, DDS
Clinical Attending— General Dentistry
North Shore University Hospital
Manhasset, New York
Private Practice
Cosmetic and General Dentistry
Manhattan and Great Neck, New York