Use of a Narrow-Diameter Implant in the Anterior Mandible: A Case Report
By Ajay Dhingra, MDS; Navid Baradarian, DDS; Howard Drew, DMD; Saul Weiner, DDS
As practitioners’ experience with implant-supported restorations expands, a number of situations that require special solutions have been identified. One of these situations arises when the mesiodistal space is restricted. In addition, these smaller intercoronal spaces frequently have a restricted osseous base near the root apices. Narrow-diameter implants offer solutions for these conditions. A number of implant systems currently offer implants narrower than 3 mm for provisional or permanent restorations.1 Most of these systems offer cementable units, but the Dentatus system is unique in providing a screw-retained restoration, which allows retrieval at any time without applying excess force on the implant.2,3 This is a significant advantage for periodontal maintenance where the anatomic limitations make treatment of the adjacent roots difficult. Because of the small diameter of the implant, rather than having a recess within the implant the screw is formed from the coronal aspect of the implant. A plastic nut that inserts over the screw and is recessed within the abutment stabilizes the abutment-crown. The implants are produced in titanium alloy for greater strength4 and are available in 10-mm, 14-mm, and 17-mm lengths and 1.6-mm, 1.8-mm, and 2.4 widths. These implants are prepared with an acid-etched surface for improved stability and osseointegration5 and packaged presterilized.
Originally, these implants were intended as provisional restorations during the healing phase of regular-diameter implants.6 However, with the changes made in alloy, surface, and packaging of these implants, they are now approved by the Food & Drug Administration for long-term use. There is histological and clinical data of osseointegration to support their use for a definitive prosthesis.7,8 The clinical case report describes the usefulness of this implant in a situation with a narrow mesiodistal space.
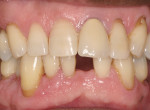
A 68-year-old man presented with the chief complaint of bleeding gums and the need for replacement ofmissing teeth. Thepatient’s medical history did not reveal any significant findings. His dental history dictated an irregularity in visiting his dentist. He had multiple extractions in the past because of advanced periodontitis and caries. On clinical examination it was found that he was missing teeth Nos. 1, 2, 14, 18, 19, and 31. Teeth Nos. 15, 16, 17, 20, 24, and 30 were beyond restoration and planned for extraction with socket preservation. There were numerous cervical abrasions and a small edentulous space between teeth Nos. 23and 25.
The treatment plan was to extract all of the hopeless teeth and follow with periodontal therapy. Then, teeth Nos. 4, 5, 12, 21, and 29 would be restored with composite resin for the cervical erosions. Implant-supported restorations were planned for site Nos. 14, 15, 18, 20, 24, and 30. Regular-diameter implants (4 mm to 5 mm) were chosen to replace all of the posterior teeth. Site No. 24 had 5.5-mm space available between the crowns and the roots of Nos. 23 and 25. Because of the reduced inter-radicular space, it was difficult to place the smallest of the standard implant systems in order to have adequate space between the roots of the natural teeth and the implant.9,10 Therefore, a narrow-diameter implant option was selected. An additional advantage of using a screw-retained system was that the crown could be readily retrieved for periodontal maintenance in the narrow space between the adjacent teeth.
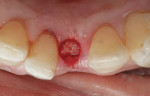
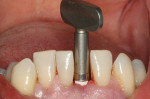
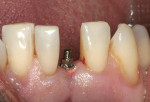
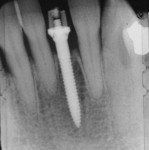
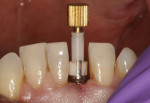
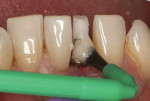
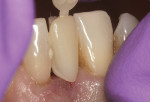
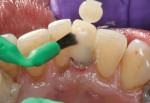
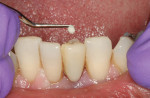
When Phase I periodontal treatment was completed, the extractions were done and regular-sized implants were placed at site Nos. 14, 15, 18, 20, and 30 (Figure 1). Because of the limited space between the crowns of the mandibular anterior teeth, mesial proximal slicing was done for teeth Nos. 23 and 25 (Figure 2). Before placing the implants, the area was anesthetized and bone sounding was performed to confirm adequate buccal-lingual width of the bone. Adequate attached keratinized tissue was present and, therefore, this area was an indication for a flapless procedure (Figure 3). The needlepoint drills and sizing reamers were used to create the osteotomy. This is a two-step process using first the profile drill followed by the refining reamer. Using copious amounts of sterile water or saline, the osteotomy is drilled at approximately 800 to 1,000 rpms to the laser-marked depth. The sterilized implant with the attached gingival protective sleeve is inserted with the driver at low speed and completed with the Manual Snap-In Key to intended length. An ANEW® implant (Dentatus, New York, NY) (Figure 4) was placed at site No. 24 using flapless surgery (Figure 5A, Figure 5B, Figure 5C).
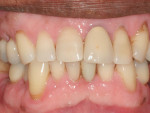
The silicon sleeve remained inserted over the shaft of the implant during the fabrication of the provisional crown. This sleeve prevents the self-cure resin from entering the sulcus and is removed before the provisional crown is screwed down. The screw cap assembly was tightened with a short brass driver. This assembly was composed of a metal index coping, a silicon connector sleeve, and a screw cap (Figure 6). Self-cure acrylic was added to close the gaps between the coping and the screw cap in the assembly (Figure 7). An appropriate sized polycarbonate crown shell was adapted to the screw cap assembly (Figure 8). The lingual aspect of the polycarbonate crown was adjusted to allow the screw cap to project out of the crown. More acrylic was added to join the shell and the screw cap assembly to produce physiologic, cleansable contours (Figure 9A and Figure 9B). The screw-retained provisional crown was finished and polished and the silicone sleeve removed before it was hand-torqued. The screw cap was adjusted so that it did not project above the lingual contours of the crown. The access hole of the provisional crown was plugged with a cotton pellet and temporary restorative material (Figure 9). The implant-supported crown was adjusted for non-functional loading with no direct occlusal contact (Figure 10).
Five months after implant placement, second-stage surgery was performed and healing abutments were placed on all of the posterior implants. Fixture-level impressions were made; the implants were provisionalized and the final restorations were made for the posterior implants.
Currently, the patient is being treated for an intestinal tumor and he requested that the final restoration be inserted after completion of tumor therapy. The provisional crown has been in for more than 10 months and remains stable.
There is a need to expand the use of implants for restorations when the standard protocols cannot be employed. Compromised situations may include narrowed ridgewidths in either arches and reduced bone volume in the posterior mandible. The use of an implant with a retrievable screw- retained restoration is an exciting development for narrow-diameter implants. The recognition thatthese implants could osseointegrate and beused for permanentrestorations, and the development of a screw-retained profile allows predictable surgical andrestorative results ata reasonable cost. The judicious use ofnarrow-diameter implants can reduce theneed for extensive grafting procedures.11 It is important to recognize, however, that the use of this narrow-design implant should be in an appropriate situation. Narrow-diameter implants are best used in Type I cortical bone with a minimum of 10 mm of height. Use in situations with a large crown-to-root ratio is contraindicated. A restricted occlusal table and avoidance of lateral excursive contacts where the occlusion in the opposing arch is in natural dentition should be planned. In conclusion, judicious use of narrow-diameter implants can provide a predictable, cost-effective service for patients in situations where conventional-sized implants cannot be used.
References
1. Mazor Z, Steigmann M, Leshem R, Peleg M. Miniimplants to reconstruct missing teeth in severe ridge deficiency and smallinterdental space: A 5-year case series. Implant Dent. 2004; 13:336-341.
2. Andersen E, Saxegaard E, Knutsen BM, Haanaes HR. A prospective clinical study evaluating the safety and effectiveness of narrow diameter threaded implants in the anterior region of the maxilla. Int J Oral Maxillofac Implants. 2001;16:217-224.
3. Comfort MB, Chu FCS, Chai J, et al. A 5-year prospective study on small diameter screw-shaped oral implants. J Oral Rehabil. 2005;32:341-345.
4. Kanie T, Nagata M, Ban S. Comparison of the mechanical properties of 2 prosthetic mini-implants. Implant Dent. 2004;13(3): 251-256.
5. Froum S, Simon H, Cho SC, et al. Histologic evaluation of bone-implant contact of immediately loaded transitional implants after 6 to 27 months. Int J Oral Maxillofac Implants. 2005;20(1): 54-60.
6. Nagata M, Nagaoka S, Mukunoki O. The efficacy of modular transitional implants placed simultaneously with implant fixtures. Compend Contin Educ Dent.1999; 20(1):39-42.
7. Zubery Y, Bichacho N, Moses O, Tal H. Immediate loading of modular transitional implants: a histologic and histomorphometric study in dogs. Int J Perio Rest Dent. 1999;19(4): 341-352.
8. Cehreli MC, Akca K. Narrow diameter implants as terminal support for occlusal three-unit FDP’s: a biomechanical analysis. Int J Periodontics Restorative Dent. 2004; 24:513-519.
9. Tarnow DP, Eskow RN. Considerations for single-unit esthetic implant restorations. Compend Contin Educ Dent.2001;16:746-761.
10. Kois JC. Predictable single tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2001;22:199-206.
11. Gniffitts T, Collins C, Collins P. Mini dental implants: An adjunct for retention, stability, and comfort for the edentulous patient. Oral Surg, Oral Med, Oral Pathol, Oral Radiol Endod. 2005; 100:E81-E84.
About the Authors
Ajay Dhingra, MDS
Post Graduate Student, Prosthodontics
University of Medicine and Dentistry of New Jersey
Newark, New Jersey
Navid Baradarian, DDS
Post Graduate Student, Prosthodontics
University of Medicine and Dentistry of New Jersey
Newark, New Jersey
Howard Drew, DMD
Clinical Associate Professor
Department of Periodontics
University of Medicine and Dentistry of New Jersey
Newark, New Jersey
Saul Weiner, DDS
Department of Restorative Dentistry
University of Medicine and Dentistry of New Jersey
Newark, New Jersey