Active Fiber-Based Post-Supported Lithium Disilicate Restoration: A Case Study
By Gregg A. Helvey, DDS
When presented with a tooth with extensive hard tissue loss, a clinician must answer two questions: is the tooth restorable and, if yes, then what is the best option for doing so? Restoration of an endodontically treated tooth with extensive hard tissue loss is customarily treated with a post-and-core procedure.1 Over the last few decades, the cast post-and-core remained the gold standard for building up severely damaged teeth. It was even thought that this type of restoration actually strengthened the tooth and its use was highly advocated.2 In the 1980s, it was revealed that removing tooth structure for the process of placement of an indirect post-and-core might weaken the tooth.3-5Around the same time, direct posts were introduced because minimal tooth structure removal was required and undercuts could remain because bondable composite resins were used as the core material.2
Since that introduction, there has been a plethora of post systems that have come to market. Stainless steel was used for the first direct post systems, and was followed by titanium. Today, esthetic fiber posts are now currently marketed. This article will review the types of direct post- and-core systems and discuss newer products and the rationale behind them.
Direct posts can be divided into two main subgroups, passive and active,which is dependent on the type ofretention.6 The passive post is non-engaging and derives retention through a cementation process. The primary retention for active posts is the threaded design which engages into the root dentin.7 The shape of the post, tapered or parallel, further categorizes the post type. Generally speaking, active posts are more retentive than passive posts and parallel posts are more retentive than tapered ones.6
Passive posts have two basic shapes, tapered or parallel-sided. Tapered posts decrease in width from the coronal to the apical end. Several factors influence the success of a tapered post. These include the contact surface between the post and the radicular surface, the amount of taper and shape of the post, the surface roughness of the post and the width of the cementing medium.8 Because of the tapered configuration, they are self-venting, which allows excess cement to extrude as they are inserted.
Parallel-sided posts maintain the same diameter from the coronal to the apical end. They can be serrated to increase the contact surface area of the luting cement. To alleviate the build-up of hydrostatic pressure during the insertion, a vent is present along the entire length of the post. Even with the vented design, there is still strain in the outer root surface upon cementation.9 However, once cemented in place, the strain is likely dissipated.6
Active posts are categorized as either self-threading or pre-tapped techniques. Self-threading posts can be either tapered or parallel and have a shank with a particular diameter with external threads. The entire diameter of the post is slightly larger than the post channel that is placed into the root canal. As the post is screwed into place the threads cut their own counter-channel into the wall of the root canal. Even though the primary retentive means is created by embedding the threads into the root dentin, cement must also be used for secondary retention and the creation of a bacterial seal along the length of the post.10-12
The pre-tapped post is a two-step process where a thread cutter is used to place an internal counter-thread pattern. This is followed by the insertion of the threaded post mating with the thread configuration. The post is cemented into place for the same reasons previously mentioned. It is important that the post does not engage with the apical bevel created by the thread cutter because of the development of excessive stress.6
A literature search of the past finds a multitude of guidelines to determine the length of a post. Starting asfar back as 1961, Rosen13 recommended that the length of the post should be equal to the clinical crown length. Bartlett14 found that the length of the post should be equal to one half to two thirds of the length of the remaining root. According to Stearn and Hirschfeld,15 the post should extend to one half the length of the root that is supported by bone. Fernandes et al16 referenced numerous articles with other recommendations. For example, Hudis and Goldstein17recommended the length of the post to be three quarters the length of the tooth or even use the post as the root canal filling, thereby obliterating the entire root canal space. Johnson and Sakamura18 recommended that the post should be half the length of the tooth and half the length of the clinical crown. Finally, Parel and Muroff19 suggested that the ideal length of the post should be midway between the apex and the height of the alveolar crest.
There are differences as to how much of the remaining root canal filling material should be kept intact. Some authors have stated that to maintain the apical seal, 3 mm to 6 mm of gutta-percha at the apex should be preserved,20-22 whereas Eghtedari and Synnott stated23that in vivo studies have suggested that the clinical success of posts is directly proportional to their lengths, so it is rational to prepare a post channel as long as it is consistent with anatomical limitations while maintaining 4 mm to 5 mm of apical gutta-percha seal.24,25
Considering the various recommendations, achieving the longest possible post length with recognition of the curvature of the apical third—thereby avoiding dilacerations or perforations—while maintaining a 4-mm to 5-mm apical gutta-percha seal seems to be a prudent protocol. The greater the post length, the better the retention and distribution of stress.26,27 In situations where the root length is short, the use of a composite luting material may compensate for the reduced length.28 In the case of short, multi-rooted teeth, the addition of more than one post will increase the retention of the core foundation.28,29
Dentin removal within the canal space should be kept to a minimum. The widely used rotary-type instruments used today for cleaning andshaping can be more aggressive; therefore,enlargement of the canal should be kept to the smallest width.30 Photoelastic stress analysis has shown that a smaller diameter post will produce a smaller amount of internal stress.31 It was once considered that placing a post increased the fracture load of an endodontically treated tooth;32 however, more recent studies challenged that observation.33,34 Rosenstiel31 described that “a root could be compared to a ring. The strength of a ring is proportional to the difference between the fourth powers of its internal and external radii. This implies that the strength of a prepared root comes from its periphery, not from its interior, so a post of reasonable size should not weaken the root significantly.” He also stated that “the root canal should be enlarged only enough to enable the post to fit accurately yet passively while ensuring strength and retention.”
Generally, cast posts have always been fabricated in gold. Prefabricated posts have used a variety of materials that include stainless steel, titanium and titanium alloys, gold-plated brass, ceramic, and fiber-reinforcedpolymers.30 The prefabricated, active-type, threaded posts have always been made from metallic material, whereas passively retained posts have been metallic and fiber-based. The first non-metallic material used for posts was based on the carbon-fiber reinforcement principle.35 Duret et al36 had reported laboratory-based studies showing that this material had high tensile strength37 and an elastic modulus similar to dentin.38 It was thought that fiber posts flex under load and, as a result, distributed stresses between the post and dentin.35 In 1997, Sidoli et al39 published a study where they compared the in vitro performance and failure characteristics of an epoxy-based carbon fiber post (Composipost, RTD, St. Egreve, France), a composite core material, and a low-viscosity Bis-GMA bonding resin against existing post-and-core combinations. They concluded that the epoxy-based, carbon-fiber system exhibited inferior strength properties in comparison to the other post-and-core systems.
More recently, esthetic posts soon became available that included quartz fiber, glass fiber, and silicon fiber. They claimed to offer the same advantages as the carbon posts but not as much research is currently available.40 A study by Akkayan et al41 conducted failure load testing using titanium, glass fiber, quartz fiber, and zirconium. They found that the failure mode was more favorable with the fiber post than the stiffer titanium post. They supported the use of fiber posts over titanium and zirconium posts. Newman et al42 evaluated the failure mode of endodontically treated teeth using stainless steel posts, glass fiber posts, and polyethylene fiber-reinforced composite posts. They found that stainless steel had higher failure loads than the fiber posts for narrow or flared canals, but that the fiber post had more favorable failure modes. The failure mode with the metal-type post usually resulted in non-restorable conditions.
The most frequent reason for post failure is the loss of retention43-45 that results from microleakage leading to caries in the post channel.46 There are numerous factors that influence post retention, including the type of post, the cement, and the interaction of the dentin to the cement and the cement to the post.25,43,47-49 Several studies have demonstrated superior post retention with resin cement compared to zinc-phosphate cement.28,50-54 Adhesive resin cements have a reinforcing effect with the ability to adhere to dentin and the post.55
Nissan et al28 compared the retentive value of metal posts cemented with zinc- phosphate cement and a titanium-reinforced composite resin cement (Flexi-Flow, Essential Dental Systems, Hackensack, NJ). Metal parallel and tapered posts were cemented into extracted human teeth of similar size. The posts were subjected to axial tensile force using an Instron universal testing machine (Model 1026, MFG, Canton, MA) at a crosshead speed of 2 mm/min. The results of their study revealed a significant increase in retention of metal parallel and tapered posts when compared to zinc-phosphate cement. Examination of the dislodged posts showed that zinc-phosphate cement had disintegrated, whereas Flexi-Flow cement was still present on the canal walls and between the threads of the posts. The authors concluded that the high compressive strength (43,100 psi) and diametric tensile strength (6,000 psi) was responsible for the increased retention. The strength of the cement is close to the strength of dentin, which is three times greater than zinc-phosphate cement.56
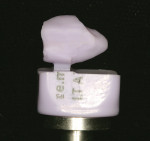
As previously mentioned, metal active posts are the most retentive, but at the same time they introduce more stress than passive posts.57-59 On the other hand, fiber posts are the least retentive but introduce a lesser amount of stress to the root. One manufacturer has combined an active threaded design and applied it to a fiber-based material. The Flexi-Post® Fiber (Essential Dental Systems) is an S-glass fiber material with a threaded shaft (Figure 1).
Glass fibers are made from liquid glass, which is a combination of sand, kaolin, limestone, and colemanite that is heated to 1,600°C. The liquid is passed through microfine bushings and simultaneously cooled, producing glass filaments ranging in size from 5 µm to 24 µm. By changing the formula, different types of glass fibers with different physical attributes are manufactured. Lowering the alkali content, E-glass (electrical) is produced, which has good tensile and compressive strength and is commonly used as a reinforcing fiber in a polymer resin matrix. The E-glass fiber is susceptible to most acids. C-glass (chemical) is resistant to acids and is used as an outer layer laminate for both chemical and water pipes and tanks. Fibers that have higher tensile strengths include R, S, and T fibers. They have a higher interlaminate shear strength with a smaller filament diameter. The R, S, and T fibers are the same but are labeled differently depending on the area in which they are manufactured. For example, the S-glass fiber is made in the United States, the R-glass fiber is made in Europe, and the T-glass fiber is made in Japan.
The Flexi-Post Fiber post is a pre-tap design. The tapping tool has the patented split-shank that absorbs the stresses as the internal threads are created in the post channel (Figure 2). The shank design includes a vent slot that extends the entire length of the shank. This allows the cement to escape as the post is threaded into place, thereby preventing the build-up of hydraulic forces in the apical area. The second tier of the fiber post has two configurations that include a parallel shank and a flange. The amount of space of the canal opening determines which design should be used. A close adaptation of the post and the natural tooth increases the stability of the post and decreases the surface area of exposed cement. Therefore, the Flexi- Post Fiber would be used in conjunction with a smaller orifice, whereas the Flexi-Flange Fiber, having a wider secondtier flange, would be better suited for a larger canal orifice. The width of the secondtier flange counters lateral stresses, which dissipates forces applied to the apical region.
Shah et al60 compared the retentive strength of a number of active and passive fiber posts. The active posts used in their study included Flexi-Post Fiber and Flexi-Flange Fiber. The passive posts used were ICEPost (Danville Materials, San Ramon, CA), ParaPost® Fiber White (Colténe Whaledent, Cuyahoga Falls, OH) and FibreKor® (Pentron Clinical Technologies, Wallingford, CT). The study parameters incorporated both a post-core and a post-tooth sample to be submitted to a tensile force. The post-tooth debonded in all subjects before the post-core interface. The post-tooth retentive strengths for both active posts were significantly higher than the passive posts.
Using the testing samples mentioned in the previous study, Rasimick et al61conducted a study to determine whether the 45° failure strength of a fiber post can be predicted based on shape alone. They found no significant differences in the bending stress between the different brands of fiber posts. However, their study did find superior failure strength of the Fiber-Flange and Fiber Flexi-Post. They concluded that the increased failure strength was attributed to the posts’ design rather the strength of the material.
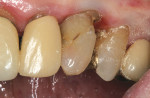
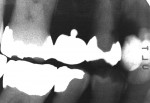
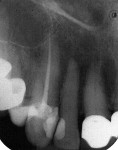
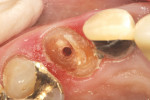
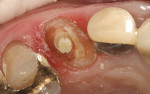
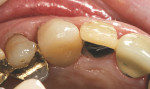
A healthy 90-year-old woman presented with decay in the maxillaryleft canine (Figure 3). The tooth hada large restoration present with secondarymarginal decay (Figure 4). After excavation, only the enamel shell remained and acarious exposure was noted. Endodontic therapy was then completed (Figure 5). Restorative options were discussed with the patient; given her ageand her excellent health, the patient desired to restore the tooth with a full-coverage crown. Because of the significant amount ofhard tissue loss, it was necessary to place apost-and-core to increase retention of therestoration.1,28 An esthetic post is preferred in the anterior region when an all-ceramic crown restoration is anticipated. In this case, a Flexi-Flange Fiber post was selected.
Several factors should be considered in the selection of the size and design of the fiber post, such as the width of the orifice of the canal, the amount of tooth structure remaining to provide a ferrule design,24,62-64 and the length, curvature, and width of the root, especially in the apical third. The manufacturer provides a transparent plastic depth gauge with silhouettes of different post sizes to aid in selection of the proper size. Placing the gauge over an accurate radiograph allows the clinician to verify the amount of tooth structure that remains between the post and the root boundaries laterally and apically. Caputo and Standlee65 recommended that at least 1 mm of sound dentin be maintained around the entire circumference. Trabert and Cooney66 also concluded that the post should have at least 1 mm of sound root structure after post channel preparation.
In this case, the height of the ferrule was not ideal in the interproximal areas; sufficient height was still present in the buccal and lingual aspects. The compromised tooth could be restored but with limited occlusal function. In this case, the adjacent occlusion lent itself to creating an anatomical design of the restoration that would eliminate contact with the opposing teeth during lateral excursive movements, thus shifting the role of canine guidance to the first bicuspid. When a tooth is structurally or periodontically incapable of handling levels from lateral excursive movements, then adding the load to the premolars can be advantageous.67
Once the post size was selected, the gutta-percha filling material was removed to the level of the post length with a series of Gates-Glidden reamers. The width of the reamer was progressively increased until 90% of the post width was achieved (Figure 6). When using the Flexi-Flange Fiber post, a countersinking is necessary for correct seating of the flange portion. A counter-sinking drill (provided by the manufacturer) was used to create this space (Figure 7). Next, the threads along the channel wall were created (Figure 8). A 17% EDTA chelating solution was irrigated for 1 minute before thread-tapping the channel and during the actual tapping as an aid for debris removal. The selected post was then inserted to verify complete seating (Figure 9).
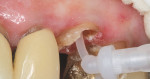
The post channel was thoroughly dried. Composite resin cement (Flexi-Flow) was used for the cementing procedure. Nissan et al28 found superior retentive values with the use of a titanium-reinforced composite resin. Cohen et al68 reported the use of a composite-resin luting cement having greater retention of metal posts over conventional cements. A bonding agent is not required when using this cement because of the threaded design. According to the manufacturer, Flexi-Flow is a patented titanium- and lanthanide-reinforced, self-curing resin cement. It has a higher compressive strength than dentin and is fluoride-releasing.69 The Flexi-Flow kit provides a tip that allows insertion of the cement into the channel space (Figure 10). The post, secured with the correct wrench size, was then screwed into place using light pressure. The excess cement was then removed.
Next, the core was fabricated using a compatible resin material, Ti-Core® (Essential Dental Systems) (Figure 11). This core material is also reinforced with titanium and lanthanide (lanthanum). Lanthanides are included in the rare-earth metals. According to the manufacturer, these metals provide strength and radiopacity.
After a 5-minute auto-polymerization, the core and the remaining tooth structure were prepared (Figure 12). A polyvinyl siloxane impression (EXA’lence™ Fast, GC America, Alsip, IL) was then taken. Unlike most conventional polyvinyl impression materials, this material is capable of immediate pouring because of the hydrogen gas scavenger property. Using a reflective bite registration material (Occlufast® CAD, Zhermack, Eatontown, NJ) the patient was guided into centric occlusion to record the bite.
The restorative material options included conventional ceramo-metal, conventional CAD/CAM ceramo-zirconia, and CAD/ CAM lithium disilicate. The latter was chosen for strength and esthetics (author’s personal preference). The impression was poured using a V2 Articulation system (MonoTrac Articulation, Salt Lake City, UT) with light-reflective stone (Elite Rock Fast Silver Grey, Zhermack). After the model was separated from the impression, the prepared tooth was scanned using a CEREC® acquisition unit (Sirona Dental Systems, Charlotte, NC). The crown was designed using the CEREC software. A lithium-disilicate block (IPS e.max CAD LT, Ivoclar Vivadent, Amherst, NY) was inserted into the milling machine and milled (Figure 11). The milled crown was returned to the solid working model and fittedfor correct seating (Figure 12).
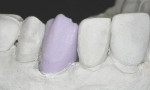
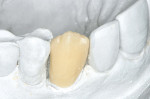
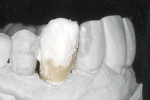
Although this ceramic material can routinely be milled to full contour, stained, glazed, and inserted, the author chose to use the cut-back technique, which enhanced the esthetic result. The incisal third was then cut back to allow for layering of enamel porcelains. According to the manufacturer, the CAD LT material in its pre-crystallized form (lithium metasilicate), has a flexural strength of 130 MPa, which is comparable to leucite-reinforced CAD/CAM (ProCAD, Ivoclar Vivadent) blocks and the feldspathic CAD/CAM blocks (VITABLOCS Mark II, Vident, Brea, CA).70 The restoration is then crystallized during a 27-minute firing cycle using a two-step ceramic furnace (Figure 13). Although there is 0.2% shrinkage during the crystallization process, the computer software accounts for this in the milling process. During the crystallization cycle, the lithium metasilicate restoration reaches a temperature of 840°C to 850°C (1,544°F to 1,562°F). During the temperature rise, a controlled growth of lithium-disilicate crystals occurs, producing a transformation of the microstructure resulting in an increase of the final flexural strength of 360 MPa. This flexural strength is approximately three to four times stronger than leucite-reinforced glass ceramics.71
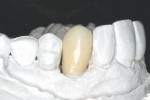
The first step in the application of the layering ceramic is to apply a thin wash coat of enamel porcelain and then bake at the appropriate temperature. The second step is to apply the desired enamel porcelains and bake (Figure 16). Finally, a glaze-and-stain step is applied and baked, completing the laboratory steps (Figure 17).
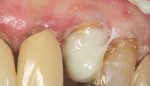
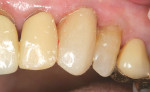
The crown was then returned to the patient for insertion (Figure 18 and Figure 19). The advantage of using this type of all-ceramic material is that it can be conventionally cemented. Although a resin cement does increase the strength of ceramics,72 a resin-modified glass-ionomer cement can be used in situations where the restorative margin is beyond the cemento-dentin junction. The occlusion was then verified. As previously mentioned, contact in lateral excursive movement was concentrated on the first bicuspid.
The first step in the restoration of an endodonticallytreated tooth is determining the requirement of a post and core, and thendeciding on the type and method of retention. Guidelines have beenpresented in terms of the selection of the width and length of the postsystem. In the anterior region, fiber-type posts offer a greater estheticresult.
The author would like to extend a special thanks to Ruth Egli for her editorial contribution, and also acknowledge Oakley Helvey for his support.
References
1. Fokkinga WA, Kreulen CM, Vallittu PK, CreugersNJ. A structured analysis of in vitro failure loads and failure modes offiber, metal and ceramic post-and-core systems. Int J Prosthodont. 2004;17: 476-482.
2. Creugers HJ. No conclusive evidence favouring cast post over direct post and core preparations. Evidence Based Dentistry. 2003;4:89-90.
3. Guzy GE, Nicholls JL. In vitro comparison of intact endodontically treated teeth with and without endo-post reinforcement. J Prosthet Dent. 1979;42:39-44.
4. Mattison GD. Photoelastic stress analysis of cast-gold endodontic posts. J Prosthet Dent. 1982;48:407-411.
5. Tjan AH, Whang S. Resistance to root fracture of dowel channels with various thickness of buccal dentin walls. J Prosthet Dent. 1985;53:496-500.
6. Ricketts DNJ, Tait CME, Higgins AJ. Post and core systems, refinements to tooth preparation and cementation. Br Dent J. 2005;198:533-541.
7. Ingle JI, Bakland LK. Endodontics. London: Williams and Wilkins, 4th ed. 1994:884.
8. Nergiz I, Schmage P, Platzer U, Ozcan M. Bond strengths of five tapered root posts regarding the post surface. J Oral Rehabil. 2002;29:330-335.
9. Ross RS, Nichols JI, Harrington GW. A comparison of strains generated during placement of five endodontic posts. J Endod. 1991;17: 450-456.
10. Reid LC, Kazemi RB, Meiers JC. Effect of fatigue testing on core integrity and post microleakage of teeth restored with different post systems. J Endod. 2003;29:304-308.
11. Bachicha WS, DiFiore PM, Miller DA, et al. Microleakage of endodontically treated teeth restored with posts. J Endod. 1998; 24:703-708.
12. Mannocci F, Ferrari M, Watson TF. Microleakage of endodontically treated teeth restored with fiber posts and composite cores after cyclic loading: a confocal microscopic study. J Prosthet Dent. 2001;85: 284-291.
13. Rosen H. Operative procedure on mutilated endodontically treated teeth. J Prosthet Dent. 1961;11(5):973-986.
14. Bartlett SO. Construction of detached core crowns for pulpless teeth in only two sittings. J Am Dent Assoc. 1968;77: 843-845.
15. Stearn N, Hirschfeld Z. Principles of preparing endodontic dowels: effects of cement, dowel length, diameter, and design. J Prosthet Dent. 1973;30:162-165.
16. Fernandes A, Rodrigues S, SarDessai G, Mehta A. Retention of endodontic post: A review. Endodonto. 2001;13:11-18.
17. Hudis SL, Goldstein FR. Restoration of endodontically treated teeth: A review of the literature. J Prosthet Dent. 1986;55:33-38
18. Johnson JK, Sakamura JS. Dowel form and tensile force. J Prosthet Dent. 1978;40: 645-649.
19. Parel ML, Muroff F. Clinical criteria for posts and cores. J Prosthet Dent. 1972;28:405-411.
20. Zillich RM, Corcoran JF. Average maximum posts length in endodontically treated teeth. J Prosthet Dent. 1984;52: 489-491.
21. Shillingburg HT, Hobo S, Whitsett LD, et al. Fundamentals of Fixed Prosthodontics. 3rd ed. Chicago: Quintessence. 1997:194-204.
22. Kvist T, Rydin E, Reit C. The relative frequency of periapical lesions in teeth with root canal-retained posts. J Endod. 1989; 15:578-580.
23. Eghtedari M, Synnott S. Foundation restorations for pulpless teeth. Clinical Update. National Naval Dental Center. 2001; 23(10):18-19.
24. Morgano SM, Brackett SE. Foundation restorations in fixed prosthodontics: current knowledge and future needs. J Prosthet Dent. 1999;82:643-657.
25. Sorensen JA, Martinoff JT. Clinically significant factors in dowel design. J Prosthet Dent. 1984;52:28-35.
26. Holmes DC, Diaz-Arnold AM, Leary JM. Influence of post dimension on stress distribution in dentin. J Prosthet Dent. 1996; 75:140-147.
27. Davy DT, Dilley GI, Krejci RF. Determination of stress patterns in root-filled teeth incorporating various dowel designs. I. Dent Res. 1981;60: 1301-1310.
28. Nissan J, Dmitry Y, Assif D. The use of reinforced composite resin cement as compensation for reduced post length. J Prosthet Dent. 2001;86: 304-308.
29. Fernandes AS, Shetty S, Coutinho I. Factors determining post selection: A literature review. J Prosthet Dent. 2003;90: 556-562.
30. Cheung W. A review of the management of endodontically treated teeth. J Am Dent Assoc. 2005;136:611-619.
31. Rosenstiel SF, Land MF, Fujimoto J. Contemporary Fixed Prosthodontics. 4th ed. St Louis, Mo: Mosby. 2006:276.
32. Sokol DL. Effective use of current core and post concepts. J Prosthet Dent. 1984;52: 231-234.
33. Sorensen JA. Preservation of tooth structure. J Calif Dent Assoc. 1998;16:15-22.
34. Torpe M, Maltz DO. Resistance to fracture of desired endodontically treated teeth. Endod Dent Traumatol. 1985;1: 108-111.
35. Bateman G, Ricketts DNJ, Saunders WP. Fibre-based post systems: a review. Br Dent J. 2003;195:43-48.
36. Duret B, Reynaud M, Duret F. New concept of coronoradicular reconstruction: the Composipost. Chir Dent FR.1990;60: 131-278.
37. King PA, Setchell DJ. An in vitro evaluation of a protype CFRC prefabricated post developed for the restoration of pulpless teeth. J Oral Rehabil. 1990;17:599-609.
38. Amussen E, Pentzfeld A, Heitmann T. Stiffness, elastic limit, and strength of newer types of endodontic posts. J Dent. 1999; 27:275-278.
39. Sidoli GE, King PA, Setchell DJ. An in vitro evaluation of a carbon fiber-based post and core system. J Prosthet Dent. 1997;78:5-9.
40. Schwartz RS, Robbins JW. Post placement and restoration of endodontically treated teeth: A literature review. J Endod. 2004;30: 289-301.
41. Akkayan B, Gulmez T. Resistance to fracture of endodontically treated teeth restored with different post systems. J Prosthet Dent. 2002;87:431-437.
42. Newman MP, Yamen P, Dennison J, et al. Fracture resistance of endodontically treated teeth with composite posts. J Prosthet Dent. 2003;89:360-367.
43. Torbjorner A, Karlsson S, Odman PA. Survival rate and failure characteristics for two post designs. J Prosthet Dent. 1995;73: 439-444.
44. Bergman B, Lundquist P, Sjögren U, Sundquist G. Restorative and endodontic results after treatment with casts posts and cores. J Prosthet Dent. 1989;61:10-15.
45. Hatzikyriakos AH, Reisis GI, Tsingos N. A 3-year postoperative clinical evaluation of posts and cores beneath existing crowns. J Prosthet Dent. 1992;67:454-458.
46. Sahafi A, Peutzfeldt A, Asmussen E, Gotfredsen K. Retention and failure morphology of prefabricated posts. Int J Prosthodont. 2004;307-312.
47. Standlee JP, Caputo AA, Hanson EC. Retention of endodontic dowels: Effect of cement, dowel length, diameter and design. J Prosthet Dent. 1978;39: 400-405.
48. Chapman KW, Worley JL, von Fraunholfer JA. Retention of prefabricated posts by cements and resins. J Prosthet Dent. 1985; 54:649-652.
49. Cohen BI, Pagnillo MK, Newman I, et al. Retention of four endodontic posts cemented with composite resin. Gen Dent.2000: 320-324.
50. O’Keefe KL, Powers JM, Mcguckin RS, Pierpont HP. In vitro bond strength of silica-coated metal posts in roots of teeth. Int J Prosthodont.1992;5:373-376.
51. Ferrari M, Mannocci F, Vichi A, et al. Bonding to root canal: Structural characteristics of the substrate. Am J Dent. 2000; 13:255-260.
52. Chapman KW, Worley JL, von Fraunhofer JA. Effect of bonding agents on retention of posts. Gen Dent. 1985;33:128-130.
53. Utter JD, Wong BH, Miller BH. The effect of cementing procedures on retention of prefabricated metal posts. J Am Dent Assoc. 1997;128:1123-1127.
54. Rosin M, Splieth C, Wilkens M, Meyer G. Effect of cement type on retention of a tapered post with a self-cutting double thread. J Dent. 2000;28: 577-582.
55. Mendoza DB, Eakle SW, Kahl EA, Ho R. Root reinforcement with a resin-bonded preformed post. J Prosth Dent. 1997;78: 10-14.
56. Cohen BI, Deutsch AS, Condos S, et al. Compressive and diametral tensile strength of titanium-reinforced composites. J Esthet Dent. 1992;4:50-55.
57. Felton DA, Webb EL, Kanoy BE, Dugoni J. Threaded endodontic dowels: effect of post design and incidence of root fracture. J Prosthet Dent. 1991;65:179-187.
58. Burns DA, Krause WR, Douglas HB, Burns DR. Stress distribution surrounding endodontic posts. J Prosthet Dent. 1990;64: 412-419.
59. Standee JP, Caputo AA. The retentive and stress distributing properties of split threaded endodontic dowels. J Prosthet Dent. 1992;68:436-442.
60. Shah RP, Musikant BL, Deutsch AS, Rasimick BJ. Retentive strengths of fiber posts. J Dent Res.2008;87(Spec Iss B):1755.
61. Rasimick BJ, Shah RP, Musikant BL, Deutsch AS. 45 degree failure strength and stress of fiber posts. J Dent Res. 2008; 87(Spec Iss B):1860.
62. McLean A. Predictably restoring endodontically treated teeth. J Can Assoc. 1998;64: 782-787.
63. Freeman MA, Nicholls JI, Kydd WL, Harrington GW. Leakage associated with load fatigue-induced preliminary failure of full crowns placed over three different post and core systems. J Endod. 1998;24:26-32.
64. Barkhordar RA, Radke R, Abbasi J. Effect of metal collars on resistance of endodontically treated teeth to root fracture. J Prosthet Dent. 1989;61:676-678.
65. Caputo A, Standlee J. Pins and posts: Why, when and how. Dent Clin North Am.1976; 20:229-311.
66. Trabert K, Cooney J. The endodontically treated tooth: restorative concepts and techniques. Dent Clin North Am.1984;28: 923-954.
67. Spear F. Science and Practice of Occlusion. McNeill C, ed. Chicago, Ill: Quintessence Publishing Co Inc; 1997:428.
68. Cohen BI, Pagnillo MK, Newman I, et al. Retention of three endodontic posts cemented with five different types of dental cements. J Prosthet Dent. 1998;79(5): 520-525.
69. Cohen BI, Musikant BL, Deutsch AS. Ten year fluoride release from four reinforced composite resins. Oral Health. 2002;92(9): 44-52.
70. Giordano R. Materials for chairside CAD/ CAM-produced restorations. J Am Dent Assoc. 2006;137(Suppl 1):14S-21S.
71. Seghi RR, Sorensen JA. Relative flexural strength of six new ceramic materials. Int J Prosthodont. 1995;8: 239-246
72. Blatz MB, Sadan A, Kern M. Resin-ceramic bonding: a review of the literature. J Prosthet Dent. 2003;89:268-274.
About the Author
Gregg A. Helvey, DDS
Adjunct Associate Professor
Virginia Commonwealth University School of Dentistry
Richmond, Virginia
Private Practice
Middleburg, Virginia