The Replacement of Small-Diameter Teeth in the Esthetic Zone Using Narrow-Diameter Implants
Maurice A. Salama, DMD; David A. Garber, DMD; Henry Salama, DMD
The management of small restorative spans in the esthetic zone has posed significant problems for the implant team. The lack of bone available for the surgeon as well as the lack of restorative space available between the adjacent teeth makes tooth replacement with implants challenging for both the restorative dentist and the laboratory technician. In the past, patients with congenitally missing teeth or microdontia have been treated with resin-bonded bridges or cantilever crowns to avoid the use of standard-diameter implants and prosthetics in this area.
Too often, surgeons attempting to place standard-diameter implants have forced the restorative team to manage these small dimensions with a lack of adequate prosthetics because of the size and diameter of the fixture head. In addition, surgical complications, such as contact with the adjacent roots, dehiscences of the labial plate, or the “show through” of the titanium through thin soft tissues, has posed a significant complication risk in attempting to use implants for tooth replacement in these situations.
Recently, the implant industry has offered a 3-mm diameter implant design to address these challenges. Most of the implants available in the 3-mm size have been one-piece or unibody implants, which often necessitate conventional tooth preparation techniques by the restorative team as well as standard cord-impression techniques for indexing the restorative margins. Some recent Zimmer TSV Unibody implants (Zimmer Dental, Carlsbad, CA) offer straight and 17° angled options with contour abutments that have pre-machined preparations and chamfer margins that do not necessitate further intraoral rotary reduction. The two cases that follow will highlight the straight Zimmer Unibody as well as the 3.3-mm diameter, two-piece conventional implant that allows the implant team to use conventional implant techniques with a two-piece implant and smaller-diameter contour abutment prosthetics for the final restorative phase.
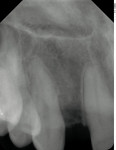
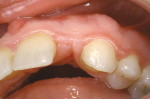
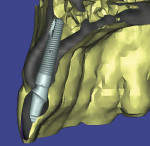
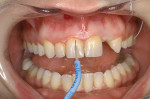
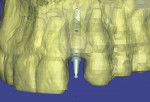
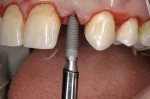
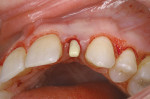
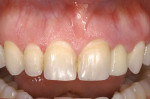
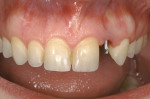
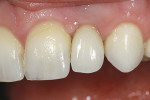
A young patient presented to the authors’ office for replacement of her congenitally missing maxillary lateral incisor following orthodontic treatment (Figure 1). Based on the lack of mesial-distal space for a normal lateral incisor as well as the lack of distance between the adjacent natural tooth roots, it was apparent that only a small-diameter implant would facilitate tooth replacement in this region. A preliminary bone graft procedure was performed (Figure 2), and after 6 months of healing a CT scan was taken and formatted for the computer treatment plan software (Figure 3). Note the accuracy of the implants’ anatomic contour in relation to the future crown. Before implant placement, a gingivectomy was performed to increase the clinical crown length of the adjacent teeth for better esthetics (Figure 4).
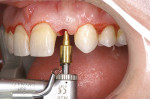
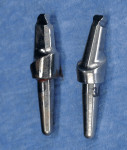
SimPlant software (Materialise Dental, Glen Burnie, MD) was used to precisely plan the placement of the Unibody implant (Figure 5). Even more so with this one-piece implant, accuracy of placement in all three dimensions is imperative to a successful outcome. A pilot drill was used in an incisionless approach based on the iCAT® CT scan (Imaging Sciences International, Hatfield, PA) (Figure 6). Straight and 17° implant analogs are available for the surgeon to test placement accuracy (Figure 7).
Based on the preoperative clinical diagnosis using stone models, a wax-up, surgical guide, and CT scan, the authors were able to accurately treatment plan this case to make certain that no complications would arise from the conservative non-flap approach. Cosmetic crown lengthening was performed first using a simple gingivectomy with a radiosurgical device and microtips.
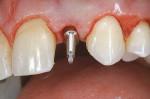
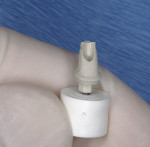
A straight analog test was performed for verification before final drilling and insertion of the Unibody implant (Figure 8 and Figure 9). Note that the anatomic location of the chamfer of the abutment on the facial is more apical than on the palatal, just as it would be on a normal cemento-enamel junction.1-3
After the 3-mm Unibody implant was placed, a temporary plastic snap cap was placed on the one-piece abutment (Figure 10). No screws were needed for the restorative phase. A polycarbonate crown former was relined over the temporary cap and finished outside of the mouth on an implant analog (Figure 11).
Figure 12 shows the immediate non-occlusal loaded temporary at day 1 of the combined implant and crown-lengthening surgery, and Figure 13 shows the result 1 week post-operatively. Note the excellent healing and esthetics.
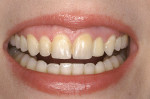
The surgical guide stent by Materialise Dental was used to accurately place the implant and a one-piece Zimmer Unibody 3-mm implant was inserted in the area of tooth No. 10 without complication. The connected abutment was accurately placed with the chamfer margin approximately 2 mm below the future gingival margin. The procedure was performed without a flap reflection and an immediate non-loaded temporary restoration was placed onto the implant. Figure 14 shows the smile view at 2 months. Esthetics is especially key in a patient with a high smile line.
After 2 months of healing, a pre-machined snap impression coping for the 3-mm Zimmer Unibody series of implants was inserted onto the one-piece abutment and sent off to the laboratory for indexing and fabrication of the final restoration.
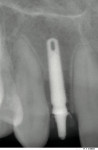
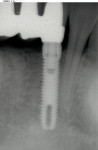
Note the bone preservation at the crest in the radiograph taken at 3 months (Figure 15). This may be a result of the lack of a microgap present with Unibody one-piece implants.4-7 Bone appears to be present above the neck of the implant and just below the chamfer margin of the abutment.
The laboratory was able to proceed with standard implant prosthetics, and the final cementable single-unit crown was fabricated on a smaller prosthetic table. This allowed the restorative team to address the contours of the soft tissue and to develop the subtle esthetics necessary for small-diameter tooth replacement (Figure 16).
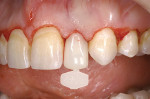
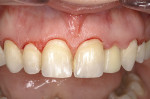
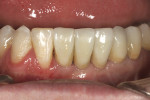
The final all-ceramic, single-implant restoration was cemented (Figure 17). A slightly lighter shade was selected because the patient desired to whiten her teeth through bleaching or pursue veneers for optimal esthetics.
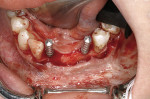
In this case, multiple mandibular incisors (teeth Nos. 22 through 25) needed to be replaced after being lost to trauma. After orthodontic tooth movement and the establishment of proper spacing, a CAT scan was completed and a Materialise surgical stent was fabricated to assist the authors in proper placement of two 3.3-mm Zimmer implants into a thin residual alveolar ridge.
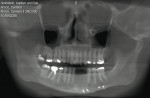
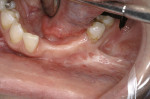
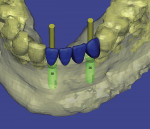
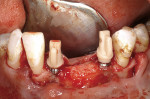
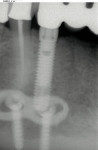
Figure 18 shows the Panorex of the patient after a traumatic accident to the lower jaw. Note the loss of teeth Nos. 22 through 25 and the sympheseal screws for fixation of fracture. Figure 19 shows the clinical view of the edentulous span after extraction and ridge augmentation, and Figure 20 shows the 3D treatment plan with the precise selection of 3.3-mm implants and placement in the areas of the missing teeth, leaving space for teeth Nos. 23 and 24 to be pontics.
After the SurgiGuide (Materialise Dental) and verification processes were completed, the implants were placed (Figure 21).
Once the implants were inserted into the areas of teeth Nos. 22 through 25, soft tissue augmentation was performed using an AlloDerm® allograft acellular dermal soft tissue matrix (LifeCell, Branchburg, NJ). The same contour abutments featured in the Zimmer Unibody one-piece system featured in the first case also can be used with the standard two-piece Zimmer TSV implant. These abutments can be selected and tried in the day of surgery and can assist in immediate temporization.8,9 The advantage is also that the components, once selected, can remain engaged with the implant body without removal for the prosthetic phase. This is critically important from a biologic standpoint because it minimizes the bone remodeling that may occur from the microgap. This concept of “one abutment, one time” may be used to mimic the crestal bone response seen around Unibody one-piece implants that entirely lack a microgap between the head of the implant and the prosthetic components. It is this connection or lack thereof that may be most critical to the long-term maintenance of the bone around the implant. This bone preservation may enhance the long-term soft response and minimize recession.
Hex-Lock™ Contour Abutment analogs (Zimmer Dental), which are identical to the ones used in the Unibody system, were used in this case (Figure 22). These can be placed by the surgeon on the day of surgery to verify and select the appropriate angulation and gingival height of the abutment. After 2 months of healing, standard snap-impression copings were placed onto the Hex-Lock Contour Abutment analogs and sent off to the laboratory for fabrication of the final restoration. Once again, no screws or drivers are required for the prosthetic phase with this system, making it easy and efficient for both the patient and implant team.
A cast framework was fabricated and an all-ceramic Cercon® bridge (DeguDent/DENTSPLY International, York PA) was placed and cemented over the abutments. The soft tissue contours were managed with small-diameter prosthetics and, once again, no vital structures were infringed upon by the use of these small-diameter components.
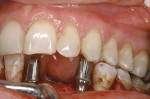
Once the analogs were inserted into the implant bodies and the correct ones verified, permanent titanium Hex-Lock Contour Abutments that corresponded to the plastic try-ins were permanently inserted to allow for immediate non-functional loading on the day of surgery (Figure 23 and Figure 24). Note how the authors check for proper occlusal clearance and restorative space. The final restoration at 3 months is shown in Figure 25.
The final radiographs, taken at 8 months postoperatively, are shown in Figure 26 and Figure 27. Note the excellent bone response at the crest of the ridge around the implants as a result of the placement of the abutments on the day of the surgery. A rigid connection may biologically perform like a one-piece system in minimizing bone remodeling and resorption at the head of the implant.
The replacement of small incisor teeth in the estheticzone has posed a challenge for many years inimplant dentistry. Today, the availability ofsmaller-diameter implants and Unibody one-piece implants withpre-machined contour abutments have assisted the dental team in restoringthese challenging areas with dental implantsrather than conventional prosthetic dentistry. The 3-mm one-piece ZimmerUnibody implant and the 3.3-mm two-piece conventional Zimmer implants with similar stock contour abutments andsnap-cap components have allowed clinicians tomeet this challenge safely and accurately in an efficient, biologically sound, and esthetic fashion.
These clinical case reports highlight the use of these smaller-diameter implants as an important and vital part of the implant team’s armamentarium in treating small-incisor replacement dilemmas. It is important to note that these one-piece Unibody implants are not to be used as small-diameter abutments for significant long-span bridge work, but have been designed specifically for the replacement of small-diameter incisors in the esthetic zone where they are to support single teeth. The authors have had much success with this form of tooth replacement and believe that it is an excellent option for our patients.
The authors have received material support from DENTSPLY International, Imaging Sciences International, Materialise Dental, and Zimmer Dental.
References
1. Sierraalta M,Razzoog ME. Restoring a severely resorbed maxillary anterior partiallyedentulous space using a one-piece titanium implant fixed partial denture:a clinical report. J Prosthet Dent. 2007;97(4):187-190.
2. Finne K, Rompen E, Toljanic J. Clinical evaluation of a prospective multicenter study on 1-piece implants. Part 1: marginal bone level evaluation after 1 year of follow-up. Int J Oral Maxillofac Implants. 2007;22(2): 226-234.
3. Glauser R, Schpbach P, Gottlow J, Hämmerle CH. Periimplant soft tissue barrier at experimental one-piece mini-implants with different surface topography in humans: A light-microscopic overview and histometric analysis. Clin Implant Dent Relat Res. 2005;7(Suppl 1):S44-S51.
4. Hermann JS, Buser D, Schenk RK, et al. Biologic width around one- and two-piece titanium implants. Clin Oral Implants Res. 2001;12(6):559-571.
5. Hermann JS, Buser D, Schenk RK, et al. Biologic width around titanium implants. A physiologically formed and stable dimension over time. Clin Oral Implants Res. 2000;11(1):1-11.
6. Sennerby L, Rocci A, Becker W, et al. Short-term clinical results of Nobel Direct implants: a retrospective multicentre analysis. Clin Oral Implants Res. 2008;19(3):219-226.
7. Ostman PO, Hellman M, Albrektsson T, Sennerby L. Direct loading of Nobel Direct and Nobel Perfect one-piece implants: a 1-year prospective clinical and radiographic study. Clin Oral Implants Res. 2007;18(4): 409-418.
8. Rocci A, Martignoni M, Gottlow J. Immediate loading in the maxilla using flapless surgery, implants placed in predetermined positions, and prefabricated provisional restorations: a retrospective 3-year clinical study. Clin Implant Dent Relat Res. 2003;5(Suppl 1):29-36.
9. Ostman PO, Hellman M, Sennerby L. Immediate occlusal loading of implants in the partially edentate mandible: a prospective 1-year radiographic and 4-year clinical study. Int J Oral Maxillofac Implants. 2008;23(2): 315-322.
About the Authors
Maurice A. Salama, DMD
Clinical Assistant Professor Periodontics
University of Pennsylvania
Philadelphia, Pennsylvania
Medical College of Georgia
Augusta, Georgia
Private Practice
Atlanta, Georgia
David A. Garber, DMD
Clinical Assistant Professor Periodontics
University of Pennsylvania
Philadelphia, Pennsylvania
Medical College of Georgia
Augusta, Georgia
Private Practice
Atlanta, Georgia
Henry Salama, DMD
Clinical Assistant Professor Periodontics
University of Pennsylvania
Philadelphia, Pennsylvania
Private Practice,
Atlanta, Georgia
Luke Kahng, CDT
Founder and Owner
Capital Dental Technology Laboratory
Naperville, Illinois