Fabrication and Evaluation of Ceramic Template Components for Precision Implant Placement
Sean W. Meitner DDS, MS
Many types of surgical templates have been described in the literature.1-7 The objective of this article is to describe the fabrication of surgical templates for partially edentulous patients using Guide Right™ Ceramic Guide Sleeves, which can be verified with 3-dimensional (3D) radiography with minimal scatter and distortion. There are several advantages to using these templates, including in-office/laboratory fabrication, reduced cost, and shorter turnaround time. Surgical templates are the most predictable and safe when fabricated from or evaluated with 3D radiography data, and they ensure that the implant placement is seated in the bone and adjacent anatomical structures are avoided.6-9
Surgical guides can be produced from CT scans with various diameters of metal sleeves for different sized drills.8,9 In some cases surgical implant placement can be completed with flapless surgical techniques.7,10,11 However, investigators have shown there are angular deviations between the planned and actual axes of the implants placed.12
Cone-beam imaging technology is relatively inexpensive, offers minimal radiation exposure to the patient, and is currently the standard of care for placing dental implants. This technology with radiopaque ceramic guide sleeves is useful to validate the proposed position of a virtual implant and the planned prosthetic trajectory.
The use of surgical template components to fabricate a surgical guide (Guide Right™, DePlaque, Victor, NY) is an alternative to a computer-generated template. The process begins with a prosthetic set-up; holes are drilled with a 3/32” drill through the set-up into the cast to capture the proposed prosthetic trajectory or the long axis of the implant.2,3 A straight guidepost is placed in the hole and used to position the guide sleeve on the partially edentulous cast. The body of the template is constructed with a light-cured acrylic (Triad Gel, DENTSPLY, York, PA). The template is indexed and stabilized on the remaining teeth on the cast. After the template is completed, it is placed in the patient’s mouth to validate the template. In the past, a combination of periapical, panoramic, or tomographic radiographs were used.13,14 Today, CT scans or cone-beam imaging can be used for verification. If the scan indicates that the radiopaque guide sleeves have been incorrectly placed, it should be corrected and a new template should be made. The angle of correction can be determined by placing a protractor over the radiograph or scan or by using computer software. The Guide Right Bending Tool (Figure 1) is calibrated in 2° increments to assist in accurately altering the angle of the post. If the direction of the post is correct but the horizontal position is inaccurate, an offset guidepost (available in various millimeter intervals) can be used.15
Once the difference in the initial angle and the desired angle of the sleeve is corrected and/or the horizontal position is evaluated and corrected, the template can be remade immediately with the altered post and sleeve.
Case Report
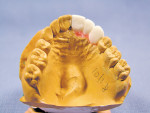
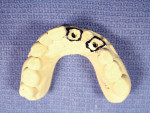
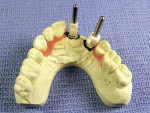
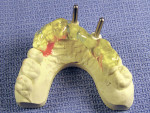
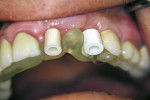
A 45-year-old woman presented for replacement of her maxillary left central, lateral incisor, and cuspid. A cast was received from the referring dentist with a diagnostic set-up (Figure 2). The cast was duplicated in dental stone and a thermal formed shell was made on the cast. A line was inscribed at the cementoenamel junctions of the two teeth that were to be replaced with implants to serve as the abutments, the central incisor and the cuspid. The three crowns from the set-up were removed from the cast. A spot was marked in the center of the root of the teeth where the crowns were removed and shallow holes were drilled with a 3/32” drill (Figure 3). The thermal formed shell was placed back on the cast and the 3/32” drills placed through a hole in the incisal edge of the central incisor and the cingulum of the cuspid into the shallow holes. The holes were extended 10 mm deep into the stone cast (Figure 4). The holes in the cast marked the long axes of the planned implant trajectory. The drills were removed and the undercuts were blocked out with red wax and the cast was lubricated with petroleum jelly. Two 3-mm guideposts were placed in the holes. Two ceramic guide sleeves were placed on the posts with the brackets rotated toward the palatal surface (Figure 5). Triad Gel was applied to the palatal and incisal surfaces in layers (Figure 6) and cured. The template was tried in and verified for fit and evaluation of the position and angle of the surgical ceramic sleeves radiographically (Figure 7). The patient was scanned with a Galileos volumetric cone-beam radiograph machine (Sirona Dental Systems, Charlotte, NC). The tangential view of the ceramic sleeve and the underlying bone for the proposed implant placement in the cuspid site indicated the position of the guide sleeve to be acceptable mesiodistally (Figure 8).
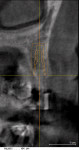
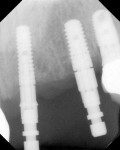
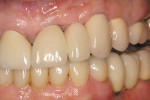
The cross-sectional view of the guide sleeve for the virtual implant in the cuspid position showed an 8° discrepancy. This error was corrected by using a pre-bent 8° guidepost to remake the template with the ceramic guide sleeve at the correct angle (Figure 9). The radiograph of the final implant positions indicates mesiodistal placement (Figure 10). The final restorative results are shown in Figure 11.
Conclusion
Precision guided implant placement in partially edentulous patients can be successfully accomplished using surgical guide sleeves and template components to make templates that are indexed on the adjacent natural teeth. Three-dimensional radiographs should be used to verify the positioning and angulations of surgical guides before the surgical preparation of osteotomies and the placement of dental implants. Ceramic guide sleeves do not produce as much scatter as metal guide sleeves. Thicker-walled ceramic guide sleeves should be used whenever possible for better radiographic definition (Figure 8). Corrections in the angle and positions of the guide sleeves can be made by using offset guideposts or pre-bent guideposts or a combination of both. All are available from Guide Right at www.deplaque.com.
Disclosure
Dr. Meitner is a current consultant for, has received material support from, and is part-owner of DePlaque.
References
1. Adrian ED, Ivanhoe JR, Krantz WA. Trajectory surgical guide stent for implant placement. J Prosthet Dent. 1992:67:687-691.
2. Higginbottom FL, Wilson TG Jr. Three-dimensional templates for placement of root-form dental implants: a technical note. Int J Oral Maxillofac Implants. 1996;11: 787-793.
3. Almog DM, Torrado E, Meitner SW. Fabrication of imaging and surgical guides for dental implants. J Prosthet Dent. 2001;85:504-508.
4. Sarment DP, Sulovic P, Clithorne N. Accuracy of implant placement with a stereolithographic surgical guide. Int J Oral Maxillofac Implants. 2003;18:571-577.
5. Babush CA. Dental Implants: The Art and Science. 2nd ed. NewYork, NY; Saunders; 2001:100-103.
6. Sergio JJ, Valdir M, de Oliveirg RR, Novaes B. Optimization in multi-implant placement for immediate loading in edentulous arches using a modified surgical template and prototyping a case report. Int J Oral Maxillofac Implants. 2008;23: 759-762.
7. Klien M, Abrams M. Computer-guided surgery utilizing a computer-milled surgical template. Pract Proceed Anesthet Dent. 2001;13: 165-169.
8. Brief J, Edinger D, Hassfield S, Eggers G. Accuracy of image guided implantology. Clin Oral Implants Res. 2006;31:234-241.
9. Di Giacomo GA, Cury PR, de Araujo NS, et al. Clinical application of stereolithographic surgical guide for implant placement; preliminary results. J Periodontol. 2005;76: 503-507.
10. Engelke W, Capobianco M. Flapless sinus floor augmentation using endoscopy combined with CT-scan-designed surgical templates: Method and report of 6 consecutive cases. Int J Oral Maxillofac Implants. 2005; 20:891-897.
11. Cannizzaro G, Leonem C, U Ferri. Exposition immediate functional loading of implants placed with flapless surgery verses conventional implants in partially edentulous patients: A 3-yer randomized controlled clinical trial. Int J Oral Maxillofac Implants. 2008;23:867-875.
12. Terzioglu H, Akkaya M, Ozan O. The use of computerized tomography-based software program with a flapless surgical technique in implant dentistry: A case report. Int J Oral Maxillofac Implants. 2009;24:137-142.
13. Almog DM, Onufrak JM, Hebel K, Meitner SW. Comparison between planned prosthetic trajectory and residual bone trajectory using surgical guides and tomography: A pilot study. J Oral Implantol. 1995;21: 275-280.
14. Almog DM, Sanchez R. Correlation between planned prosthetic and residual bone trajectories in dental implants. J Prosthet Dent. 1999;81:562-567.
15. Meitner SW, Talents RH. Surgical templates for prosthetically guided implant placement. J Prosth Dent. 2004;92:567-573.
About the Author
Sean W. Meitner DDS, MS
Associate Professor
Department of Periodontology Eastman Dental Center
University of Rochester
Rochester, NY
Private Practice in Periodontics
Pittsford, New York