Economics of the Team Approach: How-to Guide for the Minimally Invasive Dental Practice
Shirley Gutkowski, RDH, BSDH; Patti DiGangi, RDH, Marianne Harper
“Death spiral” is a secret term used by those adverse to the status quo of drilling and filling teeth. The tooth enters into a death spiral the first time a drill touches precious enamel. At some point practitioners find that their formal education has put them onto the treadmill of repair, restore, and redo until one day it becomes painfully obvious that another filling is not the answer.
As long ago as 1925, Dr. Evangeline Jordan, in her textbook Operative Dentistry for Children,1 wondered why dentistry was still filling holes in teeth, recognizing the futility of it back then. G.V. Black was a fan of minimal intervention and strove to address the cause of the disease. His extension for prevention was an attempt to address problematic architecture of occlusal surfaces. One has to wonder how his voice might change upon learning of the advances of resin and glass-ionomer sealants. Avoiding the first cavity—the first filling—must become a goal of dentistry. Minimally invasive/minimal intervention is a risk-based medical model for addressing dental disease. This model can be economically feasible with teamwork.
Drs. Jordan and Black’s thoughts resonated with a well-known physician of the same era. Charles Mayo, one of the founders of the famous Mayo Clinic, asserted in a 1928 presentation to the American Dental Association, “The practice of medicine includes dentistry and dentistry is the practice of a special branch of medicine, as is ophthalmology. It may be going too far to say that all dentists should be doctors of medicine, but certainly all dentists should know much about the practice of medicine as a whole; and, conversely, all physicians should know more about dentistry, its importance and possibilities.”2
Dental Benefit Carriers Change Coverage Base on Connections
Dental benefit carriers are learning to make use of the connections between oral and systemic health. In addition, the US Department of Health and Human Services, the issuers of the diagnosis code manuals (ICD-9-CM) for medical claims, embraced this connection when it added 30 new dentally related diagnosis codes to their 2007 ICD-9-CM manual.
New studies show that the cost of the dental death spiral has serious economic consequences. Northeast Delta reported the findings of the Data and Analysis Center, one of the largest dental health data warehouses, which analyzed 77 million claims and found that “the average cost to maintain a restored cavity in a single molar of a 10-year-old reaches $2,197 by the age of 79” from the year 2000.3 Third-party payers are in the business of saving money, not spending it.
Research reported in 2006 and conducted by Aetna and Columbia University College of Dental Medicine of a retrospective study of 145,000 of their members found a relationship between the treatment of periodontal disease and lower medical costs for members with diabetes, coronary artery disease (CAD), and cerebrovascular disease (CVD) or stroke.4 Aetna changed the frequency of coverage for preventive procedures because of the reduction in cost and risk. Dental benefit carriers understand risk; the insurance industry is based on risk assessment and actuarial tables. In July 2005, DentaQuest, a dental benefits management company and one of the largest administrators of government dental benefits programs, began covering prescription-strength fluoride toothpaste and chlorhexidine. They also extended sealant coverage for members if they had a recent cavity and are at risk for decay;5 other carriers have made similar changes.
An example of dental-medicine co-management is the treatment of sleep apnea. Sleep apnea is a serious, potentially life-threatening sleep disorder affecting approximately 18 million Americans. Sleep apnea predisposes patients to impaired daytime functioning, high blood pressure, heart attack, possible stroke, and many dental problems.6,7 An elongated palate and uvula, obesity (especially round bellies), large tonsillar pillars with redundant lateral pharyngeal wall mucosa, history of snoring, high blood pressure, and excessive tiredness during the day are all signs that dental professionals can readily observe. For a proper diagnosis, an overnight sleep study may be needed. Yet a quick neck circumference can give us clues; if greater than 16 inches in a woman or greater than 17 inches in a man there is increased risk for the disorder. For severe sleep apnea, a continuous positive airway pressure (CPAP) may be needed. Many others can be treated with weight loss and dental devices that modify the position of the tongue or jaw. This medical/dental care is often covered under both medical and dental benefits.
Creating the Reality
The time has finally come to create the everyday reality of the prophetic ideas of Drs. Jordan, Black, and Mayo. Dental and medical benefits carriers are ready, so how can we prepare our teams? The team approach to avoiding the first cavity can quickly gain ground through the mobilization of the entire dental team when healing is still possible before enamel cavitation. The dentist must take on the role of director and does not need to have a wet-finger approach.
With the majority of the process performed by the support team, this medical model philosophy can be embraced without trepidation for future earnings. Many clinicians who are already practicing this model report that their preventive practice is supporting not only itself, it is also becoming as or more profitable than their restorative practice. Their restorative practice is more relaxed as procedures become more elective—in other words, the fun stuff.
Once the entire team is on board with the philosophy, delegated data gathering can streamline the dentists’ and the dental hygienists’ time, making the entire process cost-effective for the practice and the patient. An example is caries. As a multi-factorial disease, all aspects of the infection should be known before treatment begins. Gathering diagnostic data can be the first delegable duty. The breadth of processes delegated in this philosophy brings forth the notion of a new title within the dental practice: The risk factor manager (RFM.) A position of data gathering, coordinating, and keeping up to date on new procedures and processes may be indicated in the near future. While there are no educational requirements at this time for a person with this title, this person could easily be a dental hygienist or dental assistant. Some of the data-gathering processes are to be carried out by a licensed professional; for instance, periodontal charting. On the other hand, saliva gathering and evaluation does not need to be carried out by a licensed professional.
The traditional surgical model would include examination using explorers, a dental history, dietary history, plaque assessment, and radiographs. Though still part of the overall assessment, these techniques play a smaller or different role. The explorer as a diagnostic tool is losing favor in many venues. It became obsolete in Europe in the early 1990s. It is not mentioned or is disallowed as a diagnostic tool for the Western Regional Examining Board (WREB)8 and other testing agencies. New York University has also retired the explorer as a diagnostic tool early in 2008.9 Radiographs are not dynamic or predictive and only show breakdown as it has already occurred. Options for the data gathering and tests are shown in Table 1.
Established patients are often more difficult to approach with a new philosophy, unless the practice is always evolving. Starting the new philosophy with new patients is often easier. In most instances the patient will be amazed at the philosophy and feel comfortable with the medical model risk-based approach to caries management. Excitement over the potential of saving enamel and extending into saving lives, the team will relate to the patients in a way that fosters confidence.
Dental and Medical Coding
The second most important way to make this practice philosophy successful is the proper coding for benefit reimbursement. The dental coding manual CDT (Current Dental Terminology) is updated every 2 years. More codes are still needed to embrace this medical model philosophy. Several codes were submitted and declined by the Code Revision Committee (Table 2), yet one significant change was the addition of codes for the collection and analysis of saliva.
Many dental procedures can and should be filed with patients’ medical insurance plans. Dental practices embracing this medical model philosophy can learn the mechanics. At least one team member must be trained in medical coding through the purchase of a medical coding manual, taking a dental-medical cross-coding course, and/or having a dental-medical cross-coding expert train the risk factor manager or the team as a whole. The most significant difference between dental and medical claims filing is medical carriers’ requirement of diagnostic codes. ICD-9-CM (International Classification of Diseases, Clinical Modification) is the manual listing medical diagnostic codes. Without showing the medical necessity for a procedure through the use of at least one diagnosis code, a medical claim will not be paid. This idea will soon be an integral part of dental coding and will be covered later in this article. Every medical claim must list at least one ICD-9-CM code and then a CPT® (Current Procedural Terminology) code for each procedure performed. The following case studies illustrate how this can happen and be economically feasible using both dental and medical coding.
Case Study 1
Traditional Approach: The patient is a 10-year-old named Janae who had six areas of explorer-stick cavities. All six areas were restored with amalgam restorations. No alternatives were offered. The death spiral for six teeth had begun. The teeth were given a fluoride treatment and the parents and child were admonished to brush better and start flossing.
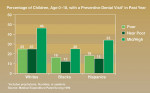
Risk Factor Management Approach: An average 10-year-old presenting with six areas of carious breakdown should be seen as unusual for many dental practices except those serving the very poor. The Surgeon General’s groundbreaking report, published in 2000, identified 20% of the population as having 80% of the dental problems.10 The report also noted the striking disparities in dental disease by income, race, and ethnicity (Figure 1).10 This did not seem to be Janae’s circumstances; both parents were physicians and he had had routine dental care in the past. There appeared to be something going on that was not lack of care, a fluoride deficiency, or toothbrush neglect.
The dental assistant as the risk factor manager could take the task of collecting and testing the child’s saliva (D0425 caries susceptibility test, CPT code 89240 unlisted miscellaneous pathology test); bacterial counts on the family (D0421, CPT code 87901 for genotype and 87797 for microtype); and preparing the teeth for laser caries detection (D0425 use narrative). Laser caries detection may be delegated to the dental assistant as well, depending on the state. This team person will also take intra- and extraoral photographs (D0350; CPT code 99070), identifying white spots and biofilm accumulations. The biofilm may or may not be stained before the photographs.
A cursory dietary evaluation also can take place before the dentist enters the treatment room. The risk factor manager can address issues of soft or sports drinks for the family if necessary, and can also make recommendations for substitutions. Once the data is collected, the dentist will evaluate it; the risk factor manager will have flagged items of interest.
Radiographs were sent from Janae’s previous practice and areas were noted for clinical evaluation. The clinical evaluation by the dentist revealed white-spot infections on the facials of the upper anterior teeth. Because the teeth were not covered in biofilm, the dentist did not remark on better brushing or flossing. Instead, the saliva evaluation gave the dentist a more precise answer to the dilemma: a resting pH of 6. This patient could brush and floss all day and not win with a pH so low. The treatment plan for glass-ionomer sealants for the second molars as they erupted to protect them was entered into the computer. Further evaluation of the caregivers and family gave enough information for a treatment plan for Janae. The hygienist placed fluoride varnish (D1206; CPT code 41899 unlisted procedure, dentoalveolar structures) on Janae’s teeth and the family was escorted to the front office. The business office support team took the reins and made appointments for an initial visit for the rest of his family.
Case Study 2
Traditional Approach: A long-term patient, Sally, came to the office for a prophylaxis, examination, and four bitewing radiographs. She was admonished for her flossing habits and scheduled for a 6-month recall.
Risk Factor Management Approach: Sally arrived and was greeted by the business team and thanked for recently sending her neighbors as new patients. Benefits information and address were updated, including medical insurance information. Sally was given a medical profile/history update, including key questions from the risk assessment forms. Data was entered into the computer and Sally was invited to the data-gathering room of the practice by the dental hygienist operating as a risk factor manager. Sally’s responses to two questions indicated a shift in her risk for caries. The information was relayed to the risk factor manager by the business office intake person. Sally had been diagnosed with type 2 diabetes, a risk factor for caries and periodontal consequences, and told she may have sleep apnea. The risk factor manager modified Sally’s plan for that day to include a conversation about the changes in her risk profile and also to include a salivary examination and additional radiographs.
The risk factor manager then asked Sally when she had her last meal or snack. Upon learning it had been 2 hours, the risk factor manager proceeded to set up for salivary evaluation (D 0425 and CPT code 89240) and collected the data. Blood pressure and other vital signs were taken, including a blood glucose level which measured 103. The risk factor manager noticed that the patient had dropped a lot of weight and, with questioning, found out that Sally had taken up cross country biking, and logged more than 150 miles/week. The exercise was prompted by her diabetes diagnosis. The hygienist risk factor manager took a neck circumference measurement, which was not over the critical line of 16 inches for a woman. Her weight loss may have affected her sleep apnea positively. The risk factor manager, well versed in risk assessment, took updated films based on Sally’s risk profile 18 months earlier. The risk factor manager also took anterior bitewings because of the new risk profile (D0277; CPT code 70310 radiologic examination, teeth, partial examination, less than full mouth [use this code only if no other radiographs are taken]).
In a typical continuing care appointment, Sally’s appointment time was nearly half over, and her teeth had not been cleaned. She had not even seen the dentist yet. This is the problem—often the prophylaxis is considered the productive part of hygiene appointments. However, to this point, the production numbers are identical, because of the extra films and saliva evaluation. A savvy reader will already know that this appointment changed from a prophy appointment to a risk management appointment, and that the patient will be likely thankful for it. The prophy could be done at a subsequent appointment.
The risk factor manager brought Sally to the hygiene room, where she further discussed Sally’s health profile, including a dietary discussion, and found out that Sally was in a diabetes support group and her dietitian was part of the group (D1301; CPT code 99401). The hygienist then performed the first of two extra- and intraoral cancer screening examinations. Sally’s periodontal evaluation included a chairside microbiological BANA test (D0502 use narrative, CPT code 89240) and microscopic evaluation of biofilm (D0415 CPT code 89240) to indicate the presence of active disease or if the disease manifestations were caused by something else. She also entered the periodontal charting information into the systematized online risk assessment tool (D0999 narrative needed, CPT code 41899 narrative needed) for an active disease and risk assessment scores. The hygienist also suggested that a PCR-DNA probe test (D0421; CPT code 88299 narrative needed) be completed yet decided to first consult with the dentist and Sally’s physician. Her risk seemed low as her history of problems was short-term. A number of areas of proximal decay were noted on the films, including the anterior films. Because Sally had embarked on an intensive exercise regimen, the change in salivary composition had created a hostile environment for her teeth. Sally had taken up chewing gum to keep her mouth moist, and used sports drinks to keep hydrated. This makes for an emergency lesson in oral health management along with the new lifestyle (D1330, CPT code 99401 preventive medicine counseling, approximately 15 minutes). The hygienist risk factor manager prepared and scanned Sally’s teeth using laser caries detection, recording all readings (D0425 use narrative; CPT code 41899 with narrative). The hygienist took photographs (D0350 oral/facial photographic images; CPT code 99070) paying particular attention to white-lesion areas. The hygienist presented to Sally the idea of a sleep apnea dental device and made a note for the dentist to consult with Sally’s physician for possible sleep studies. If the office is computerized, which is more and more likely as the 2015 target date for mandatory electronic health records approaches,11-14 the dentist will have already checked the films/images, photographs, risk assessment form, health profile, and the likely areas of cavitation needing restoration.
The results of Sally’s saliva evaluation, vital signs, blood glucose, and neck circumference readings were all recorded in her chart, as well as a note from the business office support team that Sally planned on retiring by the end of the year, just 7 short months away, increasing the need to get her oral puzzle under control. The dentist did the second oral cancer chemiluminescent/autofluorescense screening (D0431; CPT code 82397). The dentist made a preliminary diagnosis of dental decay resulting from salivary composition but told Sally he would consult with her medical practitioner as the hygienist suggested. The dentist and hygienist, with Sally, decided that a prophylaxis was the least important care needed that day. The hygienist discussed the lifestyle modifications Sally had already made and made suggestions to fit into Sally’s new life health plan. Sally then went to the insurance coordinator, the treatment options were mapped out, and estimates of both dental and medical benefits were printed. The support team in the business office was able to answer questions regarding the treatment and benefits.
Diagnosis Codes
Most dental practices are unfamiliar with using both diagnosis codes and treatment codes. Based on the traditional repair, restore, redo model, CDT currently has few diagnosis codes as compared to medical coding. In the 1990s, the ADA Council on Dental Benefits created a system called Structured NOmenclature of DENTistry (SNODENT), designed as a diagnostic companion to the CDT treatment codes. In 2006, the ADA SNODENT Editorial Panel was charged with updating clinical terminology to make SNODENT interoperable with the rest of the electronic health record.14 Diagnostic dental coding is on its way.
The most important point to remember when filing medical claims is that the same procedure can be performed on different patients resulting in the same CPT code for each, but each patient can require different diagnosis codes (CD-9-CM).
A Place to Start
These case studies and dental/medical coding are only examples. Current coverage under a dental policy does not mean that appropriate coding and documentation is unnecessary. As pointed out earlier, carriers are changing what they offer. As more employers grasp the cost-savings of this model, policy choices will also change. Medical coding in the dental office is still underused. The first few months of using unfamiliar medical or dental codes can bring a level of frustration to the business office team. Many claims may initially be denied. Filing an appeal should be the next step. Creating simple narratives showing the medical/dental necessity of the procedure can create a definite turnaround with successful dental/medical claims. Encourage your patients to become the “squeaky wheels” for insurance plan improvements.
The take-home message here is that operating this way with team support and cooperation brings about an enormous change for patient and practice care. Using a team approach is so much more productive on every level than just another prophy for a patient like Sally. With Sally’s changes, the status quo might even be considered a form of neglect if the other issues are not addressed. Most hygienists and teams would not get burned out practicing this medical model, as there is something new to learn or practice nearly every day. Which begs the question: How do you stay on top of the new technologies? The risk factor manager could be in charge of new science at monthly team meetings. PubMed and Google alerts keep filtered news on the top of the pile. If everyone chips in and brings back information from courses, then smooth, profitable implementation is not only feasible, it can happen soon. The death-spiral model can be replaced with the risk-based medical model.
References
1. Jordan E. Operative Dentistry for Children. Dental Items of Interest Pub Co; 1925 (out of print).
2. Gibilisco JA. The role of dentistry at Mayo Clinic. Minn Med. 2005;88(8): 39-41.
3. Northeast Delta Dental. “The True Cost of a Cavity.” Available at: https://www.admin.state.nh.us/wellness/PDF/Resources/Dental%20True_Cost_of_a_Cavity.pdf. Accessed October 8, 2008.
4. “Aetna and Columbia Announce Results from Study Showing Relationship Between Periodontal Treatment and a Reduction in the Overall Cost of Care for Three Chronic Conditions.” March 20, 2006. Available at: https://www.aetna.com/news/2006/pr_20060317.htm.
5. DentaQuest Taking a Proactive Approach to the Oral Health of its Members. Dental Quest Press Release April 28, 2006. Available at: https://www.dentaquest.com/news/press2.asp?id=15.
6. Lyle V. Obstructive sleep apnea. American Academy of Family Physicians. 1999. Available at: https://www.aafp.org/afp/991115ap/2279.html.
7. “What is Sleep Apnea?” American Academy of General Dentistry. March 2007. Available at: https://www.agd.org/public/oralhealth/Default.asp?IssID=330&Topic=S&ArtID=1321#body.
8. Dental Candidate Guide 2008. Western Regional Examining Board. Available at: www.wreb.org.
9. “Guidelines for Caries Risk Classification Treatment and Prevention.” New York University College of Dentistry; 2008.
10. Summary of Code Revision Committee Report CRC Actions on Batch 3 February 8-9, 2008 CRC Meeting. American Dental Association. Available at: https://www.ada.org/prof/resources/topics/cdt/crc_report_0802.pdf.
11. Oral Health in America: A Report of the Surgeon General. May 2000. U.S. Dept. of Health & Human Services. Available at: https://www.surgeongeneral.gov/library/oralhealth.
12. Palmer C. Seeds for the NHII are sown. January 22, 2007. ADA News. Available at: https://www.ada.org/prof/resources/pubs/adanews/adanewsarticle.asp?articleid=2305.
13. Flucke J. Get Ready for 2015 HER (Electronic Health Record). June 25, 2008. Dental Technology Blog. Available at: https://www.dentaltechnologyblog.blogspot.com/2008_06_01_archive.html.
14. Jakush J. Health standard setting: If the DDSs don’t do it, the MBAs will. October 20, 2006. ADA News. Available at: https://www.ada.org/prof/resources/pubs/adanews/adanewsarticle.asp?articleid=2177.
15. Furlong A. 2015 EHR deadline just around the corner. ADA News. June 18, 2008. Available at: https://www.ada.org/prof/resources/pubs/adanews/printarticle.asp?articleid=3069.
About the Authors
Shirley Gutkowski, RDH, BSDH
Owner
CrossLink Presentations, LLC
Exploring Transitions, LLC
Sun Prairie, Wisconsin
Patti DiGangi, RDH, BS
Owner
Professional Directions Conferences
Addison, Illinois
Marianne Harper
Owner
The Art of Practice Management
New Bern, North Carolina