Porcelain Laminate Veneer Insertion Using a Heated Composite Technique
Porcelain laminate veneers are used routinely in cosmetic dentistry. The public usually refers to this mode of treatment simply as “veneers.” Their popularity has increased because of television makeover programs, commercials, and magazine advertisements. Porcelain laminate veneers have so increased in their attractiveness that the general public is demanding this type of instant makeover. Further, dental laboratories are competing in marketing their abilities as to how thin they can make their porcelain laminate veneers. Plus, certain manufacturers and laboratories advocate prepless laminate veneer techniques.
Porcelain laminate veneers were first introduced by Charles Pincus1 in the 1930s and used to change the appearance of movie actors’ teeth. Unfortunately, denture adhesive was the only means of attaching the veneers to the teeth, and they came off in a short period of time. It was not until after Buonocore2,3 introduced the concept of acid-etching enamel as a means of mechanical retention that composite resin restoratives had retentiveness. By 1982, Simonsen and Calamia4 discovered composite resin’s ability to bond to porcelain if the ceramic was treated with hydrofluoric acid. In 1983, using a refractory model technique, Calamia5 described a technique for fabrication and placement of porcelain laminate veneers. Around the same time, Horn6 described a technique of porcelain laminate veneer fabrication using platinum foil. Since that time there have been numerous articles describing tooth preparation protocols, techniques for fabrication, methods for placement, and the materials to be used for bonding.7-13
Initially, porcelain laminate veneers were placed with restorative composite resin. The same material used for anterior restorations was used to insert veneers because it was the only material available. A significant number of restorations would fracture at the time of placement because the composite was thick and had little flow. In pressing the veneer into place, clinicians sometimes used excessive force, resulting in cracks or complete fractures. Manufacturers recognized these problems and developed entire lines of composite resin luting materials solely for the placement of porcelain laminate veneers and posterior porcelain restorations. The various luting materials differ in color, flowability, film thickness, and volume percentage of filler material. To keep the viscosity at a lower level, both the size and amount of the filler particles are smaller than in restorative composite resins. The physical properties of these materials can lead to post-insertion situations, such as solubility, color change, and flexural strength.14
This article discusses a method and the advantages of thermal conditioning a restorative composite resin or commercial luting cement that can be used for placement of porcelain laminate veneers.
Luting Cements and Composite Resin Restoratives
Composite resin restoratives and luting cements share the same component parts. Each is made up of filler particles surrounded by a resin matrix and contain a photoinitiator; the basic difference is that they vary in the amount and configuration of the filler particles (volume percentage). The difference in filler amounts accounts for varying rates of flow or viscosity. For example, the low viscosity of a flowable composite is achieved by decreasing the filler concentration, which in turn, increases the amount of resin and polymerization shrinkage.15 On the other hand, increasing the percentage of filler particles increases the viscosity, thereby decreasing the flow and polymerization shrinkage.
The ideal material for inserting porcelain laminate veneers would be a composite resin material with a high filler concentration for strength, low polymerization shrinkage, high modulus of elasticity, and a high flowability that allows the ceramic restoration to be easily placed. This ideal luting material would have to allow the full seating of the restoration, without the excessive pressure that can result in a fracture to the restoration. The material would have low solubility, as well as high compressive and tensile strengths. The proportional limit would be high and have excellent adhesion to porcelain as well as tooth structure.
The question is: Which available material is the closest to ideal? There are many commercial luting cements for porcelain laminate veneers. Manufacturers provide ample advertising of their commercial products. For unsuspecting clinicians, these advertisements can sway their choices in selecting products. For the more discriminate clinician, the literature is filled with countless studies on different luting cements. But a relatively small number of properly conducted clinical trials have been reported, so clinicians must formulate their decisions from various sources.16 There are numerous laboratory studies available that show the differences of luting cements in regard to compressive strengths, diametral tensile strength, tooth structure adhesion, film thickness, flowability, translucency, and other physical factors of these materials. Does the improvement of these physical factors proportionally improve the clinical success of the material?
Polymerization Behavior of Composite Resins
Composite resins shrink when polymerized and the amount of shrinkage is proportional to the filler type, shape, and volume of that material.17-20 Shrinkage, in the form of bulk reduction, occurs during the polymerization process as a result of the monomer molecules packing closer together, forming a polymer network.20-23 In short, the higher the filler content of a composite resin, the less shrinkage occurs.24 Mechanical properties and the wear resistance of a composite resin are predisposed by the filler content.25,26 The filler volume of a composite resin has an effect on the elastic modulus and volumetric shrinkage and is a key component in the development of polymerization contraction stress.27 According to Hooke’s Law (volumetric shrinkage x elastic modulus = stress), the greater the polymerization shrinkage and the higher the elastic modulus of a composite resin, the larger the contraction stress.
Another factor is the degree of conversion or the amount of free radical monomers in the resin matrix that bond together, forming a polymer network. The greater the number of monomer-to-polymer formations that occur, the higher the degree of conversion a composite is said to have. There is a correlation between the degree of conversion and shrinkage.23,28 Shrinkage manifests as stress.20 This stress can have adverse effects on the composite resin material (internal crack formation),29 the surrounding tooth structure (flexure or deformation),30-32 and/or failure of the adhesive layer interface between the tooth and the composite material (gap formation).33 Factors that effect these manifestations include: the flexibility of the sur-rounding tooth structure, the bond strength of the adhesive interface layer, and the temperature of the composite resin during the polymerization stage.
Interestingly, the temperature of the composite resin at the point of insertion has been the subject of discussion in the literature.34-37 As previously mentioned, the amount of monomer conversion to a polymer network of a composite resin when photoactivated is less than 100%. In fact, it can vary from 50% to 75%.38 The problem with incomplete polymerization is the effect of unreacted monomer on the physical and mechanical properties of the composite resin. Unreacted monomers act as plasticizers, reducing the mechanical strength and increasing swelling of the composite resin.39,40 Monomer conversion is effected by the temperature, which in turn affects the composite resin properties.34-36 An elevation in temperature increases monomer mobility, which results in additional polymerization and lessened composite viscosity.34,35,41,42 Trujillo et al43 found that an increase in the temperature of composite resin could significantly influence resin polymerization. These increased conversion rates could lead to improved properties of composite restorative materials.43 Daronch et al44 found similar results in their study, which showed an increase in conversion rates that were attributed to pre-warming composites before photopolymerization. An increase in conversion rates was also found in the study by Prasanna et al.45 Using the manufacturer’s required amount of light exposure to the composite resin, they not only found an increase in the conversion rates, but also an increase in residual stress in the bulk of the material.45 This increase in residual stress can lead to reduced resistance to wear, resulting in surface cracks.
On the other hand, Daronch et al37 found the duration of light exposure could be reduced by 50% to 75% with preheated composite, which yielded the same or significantly higher conversion (P = .001) than with a control (22°C, 20 sec). They concluded that preheating a composite before photoactivation provided greater conversion, requiring reduced light exposure than with room-temperature composite. They also found that the reduced light exposure of heated composite lowered the contraction stress more than the control.
Increasing the Flow Rate with Temperature Elevation
In their study, Blalock et al46 found that preheating composite resin did yield higher flow rates for some composite resins. They also found that there was no correlation between the composite resin classification, filler content or shape, and film thickness.
In the study described in this article by this author, to simplify the effect of increasing the flow of the composite, the author placed several commercially available composite resins between two glass slabs at room temperature (Figure 1). The weight of the top glass slab was a constant pressure applied to each sample. After 4 minutes, the amount of flow was noted by measuring the diameter of the sample. Together, the glass slabs were then placed into an oven at 150.3°F for 4 minutes (Figure 2). Then, the flow rate or the amount that the composite resin spread out was noted by measuring the diameter. A percentage increase was then calculated for each sample. The elevation in temperature did affect some composite resins more than others. The following list shows the percentage increase for several different composite resin products.
- Tetric EvoCeram® A-2 (Ivoclar Vivadent, Inc, Amherst, NY; Figure 3): 108%
- Prodigy™ B-1 (Kerr Corp, Orange, CA; Figure 4): 85%
- Venus™ B-1 (Heraeus Kulzer, Inc, Armonk, NY; Figure 5): 76%
- Point 4™ T-2 (Kerr Corp; Figure 6): 74%
- Gradia® A-2 (GC America Inc, Alsip, IL; Figure 7): 41%
- Filtek™ Supreme A-1 (3M ESPE, St. Paul, MN; Figure 8): 40%
Preheating some composite resins that demonstrate a significant increase in flow rate should allow them to be used as luting agents. The choice of the type of luting agent and its filler loading becomes more important when the marginal gap distance between the restoration and the tooth structures increases.47 Torii et al48 found that cements with a higher filler content had an increased wear resistance and worked remarkably better in wider gaps.
One flowable composite (Clearfil Majesty™ Flow, Kuraray America, Inc, New York, NY) that has an extremely high filler content of 81% by weight was also tested and found to have an increased flow of 5 mm after heating (Figure 9).
Raising the Temperature of Silane
The literature cites several studies on the effectiveness of the use of silane application to ceramic surfaces creating higher bond strengths of composite resins to ceramic surfaces.49-52 Silane improves the wettability and adds to the covalent bond formation between ceramic and resin composite.51 It provides a bi-functional attachment to both the resin and the ceramic.52 The adhesive bond of composite resin to enamel is purely mechanical and is solely dependent on the quality of the etch pattern created by phosphoric acid. However, the adhesive bond of composite resin to a ceramic surface is not only generated through mechanical means (hydrofluoric acid conditioning53,54), but also by chemical means through the use of the silane coupling agent.55
Several studies have shown that warm-air drying of the silane improves the adhesive-ceramic bond.51,56,57 After the silane is applied to the ceramic surface, heat treatment causes a condensing effect of the coupling silane molecules on the ceramic surface.58,59 The heat treatment can be accomplished through several methods. Magne described placing the silanated ceramic restoration in a dry furnace at 100°C for 1 minute or using the warm air from a hair dryer for 2 minutes.60 Improved microtensile bond strengths have been reported using a drying temperature less than 100°C (212°F) but greater than room temperature.56,61 High-temperature air-drying (50°C to 100°C) has been proven to increase ceramic-composite bond strength in luting ceramic restorations.62 Silane solutions contain water and solvents that, when present, decrease the condensation polymerization reaction that chemically bonds the silane to the ceramic. Evaporation of water and solvents contributes to the bond strength of the composite resin to the ceramic surface. Water, alcohol, acetone, acetic acid, and other by-products, if not completely removed by air-drying, may remain hydrogen-bonded to the hydroxyl-rich silica fillers of the composite substrate and decrease the number of bond sites available for reacting with silane, thus compromising the final degree of siloxane bond formation.55-58,63 Therefore, the heat treatment of silane accomplishes several things: It drives the silane/ silica surface condensation reaction toward completion; it promotes silane/silica formation; and it advances the evaporation of water and solvents.58
Technique Sequence
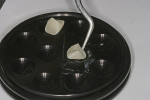
After the provisional restorations are removed, clean the prepared teeth carefully, using 50-µm aluminum oxide with light pressure. Wet the veneers with water and try them in for verification of fit and patient approval. After the try-in, clean the bonding surfaces of the restorations with phosphoric acid for 5 seconds to remove salivary proteins that can interfere with the ceramic etching with hydrofluoric acid (Figure 10). Rinse the restorations with water and dry them. Then, etch the internal surfaces with a 10% hydrofluoric acid for the appropriate conditioning time. Each type of porcelain has a specific etching time, which should be recognized and followed by the clinician to prevent improper conditioning. After the acid is rinsed off, place the restorations into a distilled water ultrasonic bath for 4 minutes.62 This bath will remove the ceramic residue of sodium, potassium, aluminum, and remineralized salts53,64 (Figure 11).Then, dry the porcelain veneers, and apply two coats of silane to the bonding surface. Next, place the veneers in the preheated (155°F) veneer warming tray (Figure 12 and Figure 13), then cover and warm for 2 minutes (CalSet™ veneer warming tray, AdDent Inc, Danbury, CT).
After the silane heat treatment is completed, apply a filled adhesive resin (OptiBond® FL, Kerr Corp). The elevated temperature of the ceramic surface will increase the flow of the adhesive resin into microporosities and any surface flaws present. The surface flaws on a ceramic surface may increase the potential of crack propagation.65 Unseen microscopic flaws can develop at the laboratory, during the try-in phase, or during conditioning steps. Magne has presented a case scenario where prebonding cracks existed in a porcelain veneer and remained invisible after 5 years.62 He attributed the phenomenon to the efficient sealing of the flaw by the adhesive resin. Only the heated ceramic condition could have increased the flowability of the adhesive resin and aided in the ceramic flaw repair.
After the adhesive resin application (Figure 14), apply a composite resin to the bonding surface of the porcelain veneers (Figure 15). Then, arrange the “loaded” veneers in the wells in the order of placement, cover them, and allow them to reach the desired insertion temperature.37
Conditioning the Teeth and Inserting the Restorations
Isolate the prepared teeth, etch them with phosphoric acid, rinse them with water, and then suction them dry (no air-water syringe used). Using a three-step bonding system (OptiBond FL), apply the primer to the teeth and suction them dry. Then, apply the adhesive resin. Thinning the resin with the air-water syringe is not necessary.
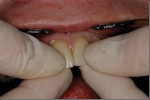
Starting with the central incisors, pick up each veneer with a college pliers instrument (Figure 16), placing each veneer on the appropriate tooth. Because the composite luting material is warm (increasing both the conversion rate and flow of the resin66), light finger and thumb pressure is all that is necessary to place the restoration in the correct position. Even though there is a reduction in temperature after restoration placement and before photoactivation, benefits still may be seen in comparison with room-temperature composites.39,45
Moving in a distal direction, insert the remaining veneers. A cotton roll can be used to wipe away the gross excess before starting light polymerization. Beginning with the central incisors, place the index fingers on the incisal edges while placing the thumbs on the labial surfaces (Figure 17). Exert light pressure to expel the remaining excess composite luting material, and fully seat the restorations. The dental assistant can position the light source between the clinician’s thumbs and activate the light for 5 seconds. The hands of the clinician shield the other veneers from any light exposure. Next, the clinician moves to the lateral incisors and repeats the same procedure. Carry out this procedure until all the restorations are secured in place. Using two light sources, complete the light polymerization of each restoration. Then, clean the margins of excess composite material using hand instruments such as scalers and 12-b surgical blades.
Conclusion
Elevating the temperature of composite resin has been shown to improve the flow characteristics of composite resin, increase the degree of monomer-to-polymer conversion, and reduce the amount of polymerization contraction stress by reducing the light exposure time. All of these benefits have been made available through the use of a unit for warming composite resin material. A veneer warming tray has been manufactured that can be used in conjunction with this unit to warm preloaded porcelain veneer restorations using tested composite resins. The same effects that are seen for composite restorative materials now can be achieved for composite resins used to bond porcelain laminate veneers.
Acknowledgment
Special thanks to Ruth Egli for her editorial contribution.
References
1. Pincus C R. Building mouth personality. J Calif S Dent Assoc.1938;14:125-129.
2. Buonocore MG. A simple method of increasing the adhesion of acrylic filling material to enamel surfaces. J Res Dent. 1955; 34:849-853.
3. Buonocore MG. Principles of adhesive retention and adhesive restorative materials. J Am Dent Assoc. 1963;67:382-391.
4. Simonsen R.J, Calamia JR. Tensile bond strengths of etched porcelain [abstract]. J Dent Res. 1983;62(Spec Iss):1099.
5. Calamia JR. Etched porcelain facial veneers: a new treatment modality based on scientific and clinical evidence. N Y J Dent. 1983;53(6): 255-259.
6. Horn HR. A new lamination, porcelain bonded to enamel. N Y State Dent J. 1983; 49(6):401-403.
7. Calamia JR, Simonsen RJ. Effect of coupling agents on bond strength of etched porcelain [abstract]. J Dent Res. 1984;63 (Spec Iss):79.
8. Calamia JR. Etched porcelain veneers: the current state of the art. Quintessence Int. 1985;16(1):5-12.
9. Quinn F, Mc Connell RJ, Byrne D. Porcelain laminates: a review. Br Dent J. 1986;161(2): 61-65.
10. Calamia JR. Clinical evaluation of etched porcelain veneers. Am J Dent. 1989;2(1): 9-15.
11. Strassler HE, Nathanson D. Clinical evaluation of etched porcelain veneers over a period of 18 to 42 months. J Esthet Dent. 1989;1(1):21-28.
12. Friedman MJ. A 15-year review of porcelain veneer failure—a clinician’s observations. Compend Contin Educ Dent. 1998;19(6): 625-638.
13. Barghi N, Overton JD. Preserving principles of successful porcelain veneers. Contemporary Esthetics. 2007;11(1):48-51.
14. Pace LL, Hummel SK, Marker VA, et al. Comparison of flexural strength of five adhesive resin cements. J Prosthdont. 2007; 16(1):18-24.
15. Freedman G, Krejci I. Warming up to composites. Compend Contin Educ Dent. 2004; 25(5): 371-378.
16. Donovan TE. The selection of contemporary restorative materials: anecdote vs. evidence-based? J Calif Dent Assoc. 2006; 34(2):129-134.
17. Filho HN, Nagem HD, Francisconi PAS, et al. Volumetric polymerization shrinkage of contemporary composite resins. Journal of Applied Oral Science. 2007;15(5): 448-452.
18. Fleming GJ, Khan S, Afzal O, et al. Investigation of polymerisation shrinkage strain, associated cuspal movement and microleakage of MOD cavities restored incrementally with resin-based composite using an LED light curing unit. J Dent. 2007;35(2):97-103.
19. Cattani-Lorente M, Godin C, Bouillaguet S, et al. Linear polymerization shrinkage of new restorative composite resins. Eur Cell Mater. 2003;5(Suppl 1):40-41.
20. Giachetti L, Scaminaci Russo D, Bambi C, et al. A review of polymerization shrinkage stress: current techniques for posterior direct resin restorations. J Contemp Dent Pract. 2006;7(4):79-88.
21. Loshaek S, Fox TG. Cross-linked polymers: factors influencing the efficiency of cross-linking in copolymers of methyl methacrylate and glycol methacrylates. J Am Chem. 1953;75:3544-355.
22. Patel MP, Braden M, Davy KW. Polymerization shrinkage of methacrylate esters. Biomaterials. 1987;8(1): 53-60.
23. Venhoven BA, de Gee AJ, Davidson CL. Polymerization contraction and conversion of light-curing bisGMA-based methacrylate resin. Biomaterials. 1993;14(11): 871-875.
24. Munksgaard EC, Hansen EK, Kato H. Wall-to-wall polymerization contraction of composite resins versus filler content. Scand J Dent Res. 1987;95(6):526-531.
25. Chung KH, Greener EH. Correlation between degree of conversion, filler concentration and mechanical properties of posterior resins. J Oral Rehabil. 1990;17(5): 487-494.
26. Condon JR, Ferracane JL. In vitro wear of composite with varied cure, filler level, and filler treatment. J Dent Res. 1997;76(7): 1405-1411.
27. Condon JR, Ferracane JL. Assessing the effect of composite formulation on polymerization stress. J Am Dent Assoc. 2000; 131(4):497-503.
28. Silikas N, Eliades G, Watts DC. Light intensity effects on resin-composite degree of conversion and shrinkage strain. Dent Mater. 2000;16(4):292-296.
29. Davidson CL, van Zeghbroeck L, Feilzer AJ. Destructive stresses in adhesive luting cements. J Dent Res. 1991;70(5):880-882.
30. Jensen ME, Chan DCN. Polymerization shrinkage and microleakage. In: Vanherle G, Smith DC, eds. Posterior Composite Resin Dental Restorative Dental Materials. Utrecht, The Netherlands: Peter Szulc Publishing Co; 1985:243-262.
31. Sullivan AH, Boyer DB, Lakes RS. Polymerization shrinkage of composite resins: comparison with tooth deformation. J Prosthet Dent. 1994;71(1): 7-12.
32. Meredith N, Setchell DJ. In vitro measurement of cuspal strain and displacement in composite restored teeth. J Dent. 1997; 25(3-4):331-337.
33. Davidson CL, de Gee AJ, Feilzer A. The competition between the composite-dentin bond strength and the polymerization contraction stress. J Dent Res. 1984;63(12): 1396-1399.
34. Bajaj P, Gupta DC, Babu GN. The temperature dependence of monomer reactivity ratios in the copolymerization of styrene with vinyl methyldiacetoxysilane. Eur Polym J. 1977;13:623-624.
35. Bausch JR, de Lange D, Davidson CL. The influence of temperature on some physical properties of dental composites. J Oral Rehabil. 1981;8(4):309-317.
36. Lovell LG, Lu H, Elliott JE, et al. The effect of cure rate on the mechanical properties of dental resins. Dent Mater. 2001;17(6): 504-511.
37. Daronch M, Rueggeberg FA, De Goes MF. Monomer conversion of pre-heated composite. J Dent Res. 2005;84(7):663-667.
38. Cook WD, Beech DR, Tyas MJ. Resin-based restorative materials—a review. Aust Dent J. 1984;29(5):291-295.
39. Nie J, Linden LA, Rabek JF, et al. A reappraisal of the photopolymerization kinetics of triethyleneglycol dimethacrylate initiated by camphorquinone-n,n-dimethyl-p-toluidine for dental purposes. Acta Polymer. 1998; 49: 145-161.
40. Lovell LG, Newman SM, Bowman CN. The effects of light intensity, temperature, and comonomer composition on the polymerization behavior of dimethacrylate dental resins. J Dent Res. 1999;78(8):1469-1476.
41. Maffezzoli A, Della Pietra A, Rengo S, et al. Photopolymerization of dental composite matrices. Biomaterials. 1994;15(15): 1221-1228.
42. Cook WD, Simon GP, Burchill PJ, et al. Curing kinetics and thermal properties of vinyl ester resins. Journal of Applied Polymer Science. 1997;64(4):769-781.
43. Trujillo M, Newman SM, Stansbury JW. Use of near-IR to monitor the influence of external heating on dental composite photopolymerization. Dent Mater. 2004;20(8):766-777.
44. Daronch M, Rueggeberg FA, De Goes MF, et al. Polymerization kinetics of pre-heated composite. J Dent Res. 2006;85(1):38-43.
45. Prasanna N, Pallavi Reddy Y, Kavitha S, et al. Degree of conversion and residual stress of preheated and room-temperature composites. Indian J Dent Res. 2007;18(4): 173-176.
46. Blalock JS, Holmes RG, Rueggeberg RA. Effect of temperature on unpolymerized composite resin film thickness. J Prosthet Dent. 2006;96(6):424-432.
47. Guzman AF, Moore BK, Andres CJ. Wear resistance of four luting agents as a function of marginal gap distance, cement type, and restorative material. Int J Prosthodont. 1997;10(5):415-425.
48. Torii Y, Itou K, Itota T, et al. Influence of filler content and gap dimension on wear resistance of resin composite luting cements around a CAD/CAM ceramic inlay restoration. Dent Mater J. 1999;18(4):453-461.
49. Della bona A, Anusavice K, Shen C. Microtensile strength of composite bonded to hot pressed ceramics. J Adhes Dent. 2000;2(4):305-313.
50. Hooshmand T, van Noort R, Keshvad A. Bond durability of the resin-bonded and the silane treated ceramic surface. Dent Mater. 2002;18(2): 179-188.
51. Jivraj SA, Kim TH, Donovan TE. Selection of luting agents, part 1. J Calif Dent Assoc. 2006;34(2):149-160.
52. Plueddemann EP. Adhesion through silane coupling agents. In: Lee LH, ed. Fundamentals of Adhesion. New York, NY: Plenum Press;1991: 279-290.
53. Canay S, Hersek N, Ertan A. Effect of different acid treatments on a porcelain surface. J Oral Rehabil. 2001;28(1):95-101.
54. Sadoun M, Asmussen E. Bonding of resin cements to aluminous ceramic: a new surface treatment. Dent Mater. 1994;10(3): 185-189.
55. Barghi N. To silanate or not to silanate: making a clinical decision. Compend Contin Educ Dent. 2000;21(8):659-666.
56. Shen C, Oh WS, Williams JR. Effect of postsilanization drying on the bond strength of composite to ceramic. J Prosthet Dent. 2004; 91(5): 453-458.
57. Papacchini F, Monticelli F, Hasa I, et al. Effect of air-drying temperature on the effectiveness of silane primers and coupling blends in the repair of microhybrid resin composite. J Adhes Dent. 2007; 9(4):391-397.
58. Roulet JF, Söderholm KJ, Longmate J. Effects of treatment and storage conditions on ceramic/composite bond strength. J Dent Res. 1995;74(1):381-387.
59. Barghi N, Berry T, Chung K. Effects of timing and heat treatment of silanated porcelain on the bond strength. J Oral Rehabil. 2000;27(5):407-412.
60. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Chicago, IL: Quintessence Publishing Co Inc; 2002: 342-346,366.
61. Monticellia F, Toledanob M, Osoriob R, et al. Effect of temperature on the silane coupling agents when bonding core resin to quartz fiber posts. Dent Mater. 2006; 22(11):1024-1028.
62. Nakamura S, Yoshida K, Kamada K, et al. Bonding between resin luting cement and glass infiltrated alumina-reinforced ceramics with silane coupling agent. J Oral Rehabil. 2004;31(8): 785-789.
63. Berg J, Jones FR. The role of sizing resins, coupling agents and their blends on the formation of the interphase in glass fiber composites. Composites Part A. 1998; 29A(9-10):1261-1272.
64. Jones GE, Boksman L, McConell RL. Effect of etching technique on the clinical performance of porcelain veneers. Quintessence Dent Technol. 1989;10(10): 635-637.
65. Mitchell CA, Douglas WH, Cheng YS. Fracture toughness of conventional, res™n-modified glass ionomer and composite luting cements. Dent Mater. 1999;15(1):7-13.
66. Holmes RG, Blalock JS, Rueggeberg FA. Composite film thickness at various temperatures [abstract]. J Dent Res. 2004; 83(Spec Iss A): 3265.
About the Author
Gregg A. Helvey, DDS
Adjunct Associate Professor
Virginia Commonwealth University School of Dentistry
Richmond, Virginia
Private Practice
Middleburg, Virginia