Realizing Minimal Preparation with Pressed Ceramic Veneers
Thomas E. Dudney, DMD
Tooth preparation for porcelain veneers has undergone a cyclical evolution. It began in the early 1980s with minimal or no preparation, progressed to more aggressive tooth reduction in the 1990s, and today, has returned to very little, if any, tooth reduction when possible.
When porcelain laminate veneers were first introduced, the technique of acid-etching the internal surface of a thin porcelain veneer and then adhesively bonding it to the acid-etched enamel surface was new and untested. Most clinicians reduced very little, if any, tooth structure to keep the preparations within the enamel layer.1 Doing so enabled them to achieve the high bond strengths necessary to attach the thin porcelain shell to the facial surface of the tooth.2-4
Time and research have demonstrated that the early success of porcelain veneers was most likely because of minimal or no preparation. An often-cited advantage of feldspathic porcelain is its need for only a 0.4-mm to 0.5-mm reduction in tooth structure, an amount that is considered minimally invasive.5
In the 1990s tooth preparation philosophies began to change when pressed ceramics were introduced and dentin bonding agents proved clinically successful. Pressed ceramics became tremendously popular, but the materials and the techniques for their placement required more tooth reduction than the placement of feldspathic veneers.6 Their minimal thickness should be 0.6 mm to 0.8 mm, which sometimes can result in aggressive tooth preparation.7
Today, preparation philosophies have come full circle, and the emphasis again is being placed on minimal or no tooth reduction. This trend most likely is caused by such factors as the successful marketing to both dentists and the general public of the “prepless” veneer, thus creating a greater demand; the teachings of respected clinicians who advocate minimal or no tooth preparation whenever possible (ie, depending on the clinical condition and the desired result8); and the ability of technicians to cut back, layer, and thin down pressed ceramic veneers to dimensions that require minimal or, in some cases, no tooth reduction. In fact, some ceramists are now pressing laminate veneer restorations as thin as 0.4 mm.
There are many benefits of minimally invasive preparations, including the preservation of tooth structure, less postoperative sensitivity, less flexibility of the prepared tooth, healthy soft-tissue response, higher bond strengths, and longer lasting restorations. This article provides an example, through the case presentation, of the use of a pressable ceramic in conjunction with very minimal tooth preparation to achieve a beautiful, natural-looking restorative result. It also emphasizes the importance of the provisional restorations and laboratory communication to ensure the overall success of a case.
Case Presentation
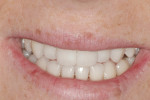
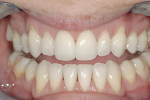
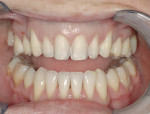
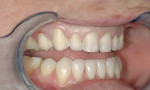
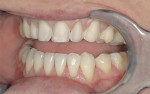
A 28-year-old woman presented for a consultation because she was unhappy with the appearance of her smile (Figure 1). She specifically felt that she did not display enough of her teeth when she smiled (Figure 2), and she wanted her teeth to be lighter in color. Thorough clinical and periodontal examinations were performed, radiographs were taken, and an esthetic analysis of the patient’s smile was conducted. The composition elements necessary for an esthetic and functional smile that were evaluated included the symmetry across the midline, anterior and central dominance, and regression proportion.9 Additionally, the overall esthetic analysis included an evaluation of the patient’s lip thickness, incisal curvature, tissue positions, tooth shape and texture, occlusal relationship, and other factors that would lend themselves to determining whether minimal preparations would be appropriate for this case.8
Based on the examination findings, a treatment plan was developed and the restorative options were discussed with the patient. The patient agreed to the placement of 10 maxillary pressed ceramic veneers, which would increase incisor display,9 decrease the negative space in the buccal corridors, and improve the color of her teeth to a lighter shade (Figure 3). The pressable material selected for this case (IPS Empress® Esthetic, Ivoclar Vivadent, Inc, Amherst, NY) requires significantly less tooth preparation than previous materials in its category.7
Impressions for study models were taken, along with a face-bow transfer (artex®, Jensen Industries, Inc, North Haven, CT), centric relation bite registration, and several photographs. This information enabled the laboratory technician to work through the case in the most predictable manner possible to achieve the patient’s desired esthetic and functional results.10 This information was forwarded to the dental laboratory with a prescription requesting a diagnostic wax-up of the anticipated restorations.10,11According to Gürel, using mock-ups, wax models, temporaries, and silicone indices provide the best esthetic, phonetic, and functional outcomes and enables better communication with the patient and the laboratory technician.12
Preparation and Temporization
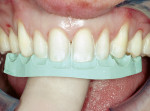
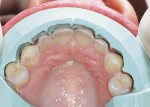
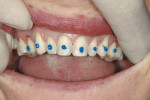
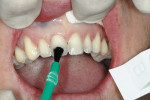
During the preparation appointment, a 0.4-mm depth-cutting bur was used as a guide to ensure minimal facial reduction13,14 (Figure 4). Incisal reduction was also minimal because the incisal length would be increased (Figure 5 and Figure 6). Preparation guides made from the diagnostic wax-up were used to verify the facial and incisal reduction (Figure 7 and Figure 8), as well as to ensure uniformity in the thickness of the porcelain.15 Using a combination of a depth-cutting bur and preparation guides helped to conserve tooth structure and achieve predictable results.13,14
Supragingival margins, which would promote gingival health,16 were formed because the natural teeth demonstrated a light shade. Although interproximal elbows were created in the preparations, none of the interdental contacts were broken, and all internal line angles were rounded and smoothed.
After the tooth preparation was completed, a polyether impression (Impregum™, 3M ESPE, St. Paul, MN) was made, along with a stick bite for horizontal reference. A shade of the prepared teeth and an occlusal bite registration were also taken.
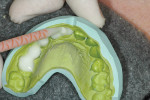
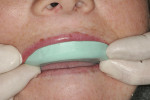
Because the preparations were very conservative, an intraoral, lock-on technique was used to provide the patient with provisional restorations. A provisional material that in the author’s opinion demonstrates excellent handling properties, favorable tissue response, and esthetics (Luxatemp®, Zenith/DMG Brand Division, Foremost Dental LLC, Englewood, NJ) was selected for this case in shade BL. A putty matrix (Sil-Tech® putty, Ivoclar Vivadent, Inc) made from the diagnostic wax-up was used to fabricate the temporaries (Figure 9; Figure 10; Figure 11 and Figure 12).
Provisional Restorations and Laboratory Communication
A significant amount of information can be gained from provisional restorations. For this reason, the closer the clinician can get them to resemble the desired definitive restorations, the better his or her communication will be with the laboratory technician.11,12 For example, the incisal edge position and length of central incisors can be determined from the provisional restorations and communicated to the laboratory. This information is invaluable information for the ceramist and critical to the success of the case.
Therefore, it is very important to evaluate the patient in provisionals during a follow-up visit so that more accurate information can be obtained. Having the patient smile naturally when not numb and speaking phonetic sounds such as “F,” “V,” “S,” and “E” will aid the dentist in determining the proper length and incisal edge position. Furthermore, the dentist will be able to evaluate the anterior guidance of the new incisal edge position, as well as important smile design features such as gingival symmetry, arch form, smile arc, axial inclination, and buccal corridor during this appointment.
Also at this appointment, valuable information and insight can be gained from patient feedback. The patient should be encouraged to let the dentist know if he or she likes or dislikes any aspect of the temporaries, including the color, size, shape, and appearance of the teeth, in addition to whether or not the bite feels comfortable. After the patient approves of these various aspects of the “preview” of the final restorations, an impression and pictures of the temporaries can be taken. Any necessary changes that have been made can be noted and sent to the laboratory to aid the ceramist in achieving optimal results.
In this case, all of the treatment goals—increasing incisor display, decreasing negative space, and lightening the tooth shade—were realized with the provisionals (Figure 13). As a result, they were an excellent blueprint for the laboratory technician when fabricating the final restorations.10
Delivery of the Final Restorations
The cementation appointment was uneventful. The provisional restorations were carefully removed, and the preparations were cleaned with hydrogen peroxide and disinfected with a chlorhexidine rinse (Consepsis®, Ultradent Products, Inc, South Jordan, UT). The veneers were individually tried in with water and then all together to evaluate fit, marginal integrity, color, and esthetic integration. After approval from the patient, the veneers were set aside to be etched, rinsed, dried, and silanated in preparation for cementation while the teeth were isolated with a rubber dam.
The veneers were bonded to the teeth using a total-etch technique with a fifth-generation bonding agent (Prime and Bond® NT™, DENTSPLY Caulk, Milford, DE) and a light-cured luting cement (Variolink® Veneer, Ivoclar Vivadent, Inc) in shade +1. Excess cement was cleaned from the facial surfaces with cotton rolls and brushes. The restorations were then tacked in place at the gingival margin using a 3-mm curing-light tacking tip for 5 seconds per tooth.5 Then, the interproximal excess cement was removed with dental floss, after which the restorations were light-cured for 1 minute each from the facial and lingual surfaces using a light-emitting diode curing light (bluephase® 16i, Ivoclar Vivadent, Inc).
The interproximal contacts were polished using diamond finishing strips (Brasseler USA, Savannah, GA), and the occlusion was checked and adjusted where necessary. Finally, the restorations were polished using rubber points (Ceramisté™, Shofu Dental Corp, San Marcos, CA) and polishing paste (Porcelize™, Cosmedent Inc, Chicago, IL) on a felt wheel, and the patient was scheduled for a postoperative appointment.
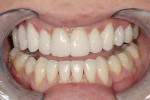
During the follow-up visit, the results were evaluated, and it was agreed that the treatment goals had been achieved (Figure 14; Figure 15; Figure 16 and Figure 17). The pressed ceramic veneers (IPS Empress Esthetic) were fabricated sufficiently thin to enable minimal preparation techniques, yet create a natural-looking and esthetically pleasing smile.
Conclusion
In recent years, greater emphasis has been placed on the conservation of tooth structure and minimal preparation during smile-enhancement cases. Such an approach is beneficial to the patient and to the long-term predictability of the esthetic restorations that are part of the treatment plan. While it is possible to achieve predictable results with no tooth preparation, careful case selection is required and ongoing and detailed communication with the laboratory is of paramount importance to ensuring a successful endeavor. The willingness of clinicians to be as conservative as possible when preparing teeth for porcelain veneers—and their conscientious attention to detail when providing information to the laboratory— will most likely contribute to the success of the case and to the longevity of the restorations. This case demonstrated the use of very minimal tooth preparation to accomplish subtle changes that improved the appearance of the smile, as well as the importance of provisional restorations for communicating with the patient and the laboratory.
Acknowledgment
The author wishes to thank Frontier Dental Laboratories, Inc, and their technical team for fabricating the beautiful restorations featured in this case presentation.
References
1. Calamia JR, Calamia CS. Porcelain laminate veneers: reasons for 25 years of success. Dent Clin North Am. 2007;51(2):399-417.
2. Strassler HE, Weiner S. Seven to ten-year clinical evaluation of etched porcelain veneers [abstract]. J Dent Res. 1995;74(Spec Iss);176. Abstract 1326.
3. Calamia JR. Clinical evaluation of etched porcelain veneers. Am J Dent. 1989;2(1):9-15.
4. Strassler HE, Weiner S. Long-term clinical evaluation of etched porcelain veneers [abstract]. J Dent Res. 1998;77(Spec Iss A):223. Abstract 1017.
5. Cho GC, Donovan TE, Chee WWL. Clinical experiences with bonded porcelain laminate veneers. J Calif Dent Assoc. 1998;26(2):121-127.
6. Friedman MJ. Porcelain veneer restorations: a clinician’s opinion about a disturbing trend. J Esthet Restor Dent. 2001;13(5):318-327.
7. Nash RW. Porcelain veneers: a clinical perspective. Contemporary Esthetics and Restorative Practice. 2006;10(12):52-58.
8. Javajeri D. Considerations for planning esthetic treatment with veneers involving no or minimal preparation. J Am Dent Assoc. 2007;138(3): 331-337.
9. Snow SR. Esthetic smile analysis of maxillary anterior tooth width: the golden percentage. J Esthet Dent. 1999;11(4):177-184.
10. Trinkner TF, Roberts M. A systematic approach to anterior esthetics. Contemporary Esthetics and Restorative Practice. 2003;7(1):42-49.
11. Magne P, Magne M. Use of additive wax-up and direct intraoral mock-up for enamel preservation with porcelain laminate veneers. Eur J Esthet Dent. 2005;1(1):10-19.
12. Gürel G. Porcelain laminate veneers: minimal tooth preparation by design. Dent Clin North Am. 2007;51(2):419-431.
13. Rosenthal L. Preparation guidelines for less-invasive cosmetic restorations. Gen Dent. 2007;55(7):624-630.
14. Bassett JL. A cognitive systematic approach to analyzing preparation design for a difficult space management case. Gen Dent. 2007;55(7):664-668.
15. Brunton PA, Aminian A, Wilson NH. Tooth preparation techniques for porcelain laminate veneers. Br Dent J. 2000;189(5):260-262.
16. Orkin DA, Reddy J, Bradshaw D. The relationship of the position of crown margins to gingival health. J Prosthet Dent. 1987;57(4):421-424.
About the Author
Thomas E. Dudney, DMD
Private Practice
Esthetic, General, and Restorative Dentistry
Alabaster, Alabama