CAD/CAM Today: A 22-Year Retrospective
Daniel J. Poticny, DDS
Patient demands, new materials and techniques, and the costs of doing business are influencing the dental profession to adopt computer-aided design/computer-aided manufacture (CAD/CAM) restorations, metal-free substitutes, and digital techniques in both offices and laboratories. This article discusses dental CAD/CAM technology from the advent of the first successful system to current trends, touching on the rationale for digital dentistry and its continued growth within the profession.
CAD/CAM Reshapes the Profession
Change is inevitable...growth and learning is a choice. Any dentist who has practiced for more than 20 years would agree that dentistry is being practiced much differently today than when he or she graduated from dental school. Much has changed in terms of the methods and devices used to accomplish daily tasks. With the maturation of adhesion dentistry, clinicians can confidently restore teeth to form, function, and natural appearance. Regardless of the amount of time a dentist has practiced, it is becoming quite apparent that the profession is being reshaped through the introduction and adoption of new technologies. CAD/CAM is chief among these, and its future implications are becoming clearer as the 21st century unfolds.
The Beginning
CAD/CAM restorative dentistry is still not well understood. The pioneering concept was initially proposed in 1973 by Dr. Francois Duret, who diagrammatically sketched the mechanism for the use of a charged-coupled device (CCD) sensor to digitally capture a tooth preparation and machine the restoration with cutting tools.1 This sketch led to the creation of the first functioning prototype. Around 1980, with a parallel effort by a persistent Swiss prosthodontist, Dr. Werner Mörmann, and Dr. Marco Brandestini, an electrical engineer, the basis for the first mass-produced system was born.2 Dr. Mörmann’s reasoning was simple: People want naturally appearing dental restorations. He also reasoned that composites, at that time, were of limited usefulness in this regard. Composites of the late 1970s were known to have the problems of polymerization shrinkage with the ensuing formation of marginal gaps, not being resistant to wear, and less than ideal longevity.3 He concluded, through research of pressed and heat-processed materials, that if the aforementioned could be fashioned to the cavity preparation and adhesively luted, it could solve the problem of large gap formation during polymerization of resin fillings to provide a long-lasting, wear-resistant restoration.4 He felt that industrially produced, pressure-formed, fine-grained porcelains had properties similar to human enamel, making them the best suited for the restoration of teeth. If these inlays made of ceramic could be proven to survive by incorporating a tight adhesive interface between the inlay and the tooth, which was later confirmed through a variety of studies,5,6 he reasoned that patients and dentists would prefer to have them done in one visit rather than two visits, which was typically necessary.
In short, he set out to accomplish the world’s best direct restoration. He and Dr. Brandestini produced a device that used an optical system to capture an image as a substitute for a stone die, and a computer and a milling machine to grind and fashion an insert made from an ingot of feldspathic porcelain that could be placed into a cavity preparation and adhesively joined to dentin and enamel. Coining the acronym CEREC (CEramic REConstruction), the first working unit was produced in 1985.2
As adhesively placed posterior restorations were not new, these early ceramic restorations were placed using adhesion between enamel and the restoration surface itself. While questions arose about using a brittle material like ceramic and expecting it to hold up well under the demands of the oral environment, the CEREC CAD/CAM process pioneered by Mörmann and Brandestini has consistently proven itself to create some of the world’s finest and most durable direct restorations.7 And like any computerized system, the technology has evolved and been enhanced to meet a variety of restorative needs, from the simple inlays that were its original intent to nearly any type of restoration. Today, this technology’s documented long-term success appears to have paved the way for an increasing number of systems, providing both chairside and laboratory applications.8 The increasing pervasiveness of the original CEREC CAD/CAM and other systems is gradually removing the disconnect that has existed for years in the dental profession between CAD/CAM technology and its importance to the profession.
The Present
At this year’s largest west coast exhibit for the laboratory industry, LMT Lab Day West, many of the breakout sessions were dominated by words like “digital impressioning,” “zirconia,” “CAD/CAM,” and others. Every session was standing-room only, and the buzz was obvious, with catchphrases like “CAD/CAM is here to stay” and “total ceramics is the future.” So what is going on and what does it mean for today’s dentists? Perspective can be gained by examining what is changing about materials and the day-to-day operations in dental offices and laboratories alike.
The Material Challenge
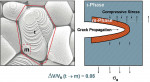
Dentistry’s past is littered with failed promises of laboratory-fabricated ceramic materials that would perform well, such as castable glasses.9 Although cements were not adequate to support these all-ceramic materials, research and development continued and success was realized with the introduction of IPS Empress® (Ivoclar Vivadent, Inc, Amherst, NY) for anterior crowns and posterior partial-coverage restorations.10 Laboratory technicians using a lost-wax process with multiple pressings and ceramic layering could fabricate a restoration that was more dense and metal-free. If these restorations were placed using specific bonding agents and adhesives, success could be realized. Of note is that the original material for the CEREC method was the VITA MK I feldspathic ceramic (Vita Zahnfabrik, distributed by Vident, Brea, CA) the precursor to VITA MK II ceramics widely used today. Subsequently developed materials include ProCAD (now EmpressCAD by Ivoclar Vivadent) and Paradigm C and Paradigm MZ-100, a full ceramic and compomer respectively (3M ESPE, St. Paul, MN) which are also in widespread use. Materials such as the EmpressCAD are compositionally identical materials to laboratory Empress with decidedly different methods. Empress as a laboratory product uses a pressed technique mentioned above while CEREC® (Sirona Dental Systems, LLC, Charlotte, NC) incorporates digital design and full-contour milling, with both achieving success.11,12 The key element was bonding or adhesive placement rather than the use of conventional cementation techniques, which had caused the problem with castable glass restorations. Adhesion to the tooth and the intaglio surface of the restoration supported the otherwise brittle material in much the same way affixing tile to concrete strengthens the inherently weak material. Following these successes, efforts continued to develop metal-free alternatives for bridge frameworks and crown copings that would be rigid enough to support veneering porcelains and yet allow for conventional cementation, much like veneered metals.13 These new materials were alumina, zirconia, and lithium disilicate. Chief among these, and the one creating the most interest, is zirconia. This ceramic material is regarded as having the highest strength and fracture toughness in dentistry.14 While in its elemental form it is identical from manufacturer to manufacturer, meticulous processing is essential to maximize its strength potential by virtue of a porosity-free, dense microstructure. Zirconia’s unique ability to undergo a process known as transformation toughening makes it a logical choice as a viable option to metal cores.15,16 After a crack starts in zirconia, the energy supplied by the crack permeates the surrounding crystal (Figure 1 and Figure 2). This action results in a volume expansion that creates compression to seal and arrest the crack. Ongoing studies begun in 2000 (Piwowarczyk A and Lauer HC; Pospeich P; 3M ESPE) are confirming that it performs to a standard comparable to ceramic-veneered metal and exhibits excellent marginal adaptation. Today its use is increasing annually as more dentists experience successful outcomes.17
The Business of Dentistry
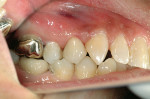
Courtesy of the proliferation of electronic media, today’s dental consumer is more knowledgeable than ever. People expect to die chewing, and look good while they are at it. Because of the pervasive nature of technology, the majority of patients today expect modern treatment that is not cosmetically disfiguring, using materials, instruments, and techniques that are current by today’s standards, not something that may be nearly 100 years old. Because they expect 21st-century solutions to ancient dental problems, patients are more and more reluctant to accept metal. The buzz, so to speak, is “metal-free,” and while not a comment on the appropriateness of metal, dentists are feeling the pressure to deliver a higher level of functional and esthetic care.
Furthermore, the general public has a higher awareness of what CAD is, and its use in the fabrication of many consumer items. CAD/CAM has already left its mark in medicine, with everything from artificial joints to hearing aids being fabricated through this process. Scant few prostheses used in current medicine are fabricated by hand or by lost-wax processes, except for specialty items that correct cosmetic disfigurement. Prosthetic joints, limbs, and tooth implants are machined for reasons of consistency and precision.
According to 3M ESPE, more than 50 million impressions were taken in dental offices across the United States in 2007, with the demand for elective services at an all-time high. And even in these economically cautious times, dentistry still fairs quite well. Time is valuable to everyone, and there are things that patients still do not like about coming to the dental office, with impressions and multiple appointments high on their lists. The word “value” is commonly used to describe what consumers shop for. Patients expect their dentists to invest in technology that improves their lives, and dentists must continually balance quality with cost control.
From the perspective of dental laboratories, technicians have to service the 50 million impressions. Yet higher demand is being challenged by diminishing manpower in laboratories. Despite higher demand for their services, laboratories are increasingly finding it more difficult to deliver consistent, high-quality services. This is directly attributable to the scarcity of skilled ceramists and other laboratory personnel. Talented technicians are paid a premium, driving costs higher. Being heavily invested in manual labor, laboratories are seeking systems that reduce fabrication times with no sacrifice in end-product quality.
Outsourcing is a common practice used by laboratories to lower costs by using offshore sources. Recently, the public was alerted by an investigative report by WBNS TV in Cleveland, Ohio, to the potential for lead contamination in restorations being outsourced to overseas laboratories (China and others) and even within the United States.18,19 While not a comment on the quality of these restorations (many overseas sources are reputable), it is more of a comment on the uncertainties that none of us wish to confront. Dentists’ need for certainty, along with the need for laboratories to remain profitable, places laboratories in an unenviable position. When high demand, diminishing manpower, and the expectation for cost control are combined, the industry may be reaching critical mass, and solutions are needed.
Solutions for Laboratories
These incongruities may be addressed through automated processes. The key word here is “automated.” Most industries have automated their production processes, and dentistry appears to be headed in this direction. Henry Ford did it more than 100 years ago with the assembly line, which is in large part an automated process. One machine can do the work of many men. Digitalization allows for virtual assembly, saving time and improving quality. Everything from aircrafts to children’s toys exemplify where CAD/CAM has been used to design products without the costs associated with models and the time it takes to produce them. With CAD design, some products have gone from years to months in development time.
CAD/CAM systems, ceramics (zirconia, alumina, lithium disilicates, and milled feldspathics), and digital impressioning techniques are redefining how technicians perform their art. Laboratories are investing heavily in CAD/CAM and laser scanning devices for models. Using these systems reduces production time from that of hand labor, saving money as well. Many dentists are partnering with larger laboratories with centralized milling capabilities. CEREC inLab® (Sirona Dental Systems), Lava™ (3M ESPE), Everest® CAD/CAM (KaVo Dental Corp, Lake Zurich, IL), and many others are being used in laboratories worldwide. Some of these systems have abilities to create “virtual linkage” through the Internet between laboratories and dental offices. This electronic transfer of information allows for models to be created off-site, without the need for physical impressions. Virtual linkage is enabling better dentist–laboratory technician relationships, allowing for excellent treatment outcomes, improved patient experiences, and streamlined assembly of dental restorations.
Advantages for Dentists
Clinically, the ability to predictably treat one or two teeth using high-quality ceramics with the convenience of one operative incursion is a distinct advantage for those dentists having or considering a CAD/CAM system. In essence, through automation these systems reduce the time necessary to complete one of the most time-inefficient procedures dentists perform—the single-unit crown or onlay. For example, in an office using CEREC 3D, the patient arrives, and the dentist completes the crown (standard ceramic preparation) or onlay preparation and then uses a camera to capture instantaneous images digitally, much like using a “point and click” camera, to record an impression of the preparation. The system’s software can stitch together successive still captures to record as much of the arch as desired. The information then is rendered virtually on a monitor. A restoration is designed with an automated and patented “biogeneric” process. The patented biogeneric process provides consistent restoration proposals that are anatomically correct and in close occlusal approximation to the opponent. Unlike previous versions of the software, the occlusal design schematics including contact intersection with the opposing teeth are rapidly established with little change to the morphology in many cases. The restoration design is generated quickly, with little need for additional operator input. Design time and milling of the restoration occurs in 10 minutes or less for many cases.
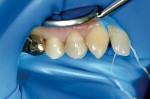
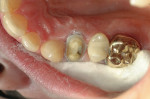
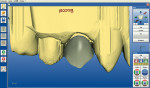
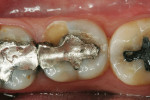
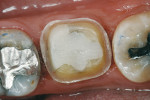
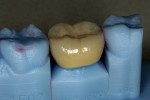
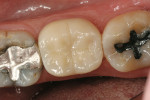
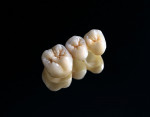
Using polychromatic blocks to simulate the optical properties of teeth, the restoration is milled on the in-office unit. The operator treats the intaglio surface of the restoration with hydrofluoric acid-etch followed by silane, which improves the “wettability” and contributes to covalent bond formation between porcelain and composite resin. Additionally, it bonds silicone dioxide and methacrylates to the porcelain surface, which react with composite resin to form a tight seal. The restoration(s) is then placed in the patient’s mouth and adhesively luted. Whether polished or glazed (operator choice) the duplication of nature is easily within reach in the dental office, in the constraints of one visit and without the need for temporaries (Figure 3, Figure 4, Figure 5 and Figure 6). Time savings, predictability, and the creation of value to the patient are obvious caveats and exactly what today’s patients are asking for. Clinically, the restorations show excellent marginal adaptation and well-received esthetics.20
For clinicians who do not want to design and fabricate restorations in the office or for situations where laboratory support is necessary, digital impression technology is available to replace traditional impression making. The Cadent iTero™ digital impression system (The Cadent Co, Carlstadt, NJ) was the first device that enabled dentists to take digital scans of the teeth and the bite and transmit this information file over the Internet to a Cadent-partnering laboratory, where the physical restoration is created from a solid model milled from the digital information.
Lava™ Chairside Oral Scanner (C.O.S) (3M ESPE) is an impressive impression-less technology that uses revolutionary “3D-in-Motion” technology to capture continuous video images while the small camera is in constant motion, unlike “point-and-click” methods used by CEREC. The camera automatically takes the image when it reaches the proper distance from the teeth. The virtual model appears in real time and is “stitched” together in a continuous fashion on a touch-screen monitor, letting the dentist manipulate it for viewing in all three dimensions.
The dentist then can create a digital prescription and send it electronically to the laboratory for a Lava metal-free zirconia bridge or crown restoration. This system will permit the laboratory technician to work virtually without models or conventionally with them. This system’s “open architecture” gives it the potential for a myriad of uses beyond its original intent. For clinicians who do not want to leave their comfort zones, the advantages are obvious: Much of the traditional workflow pattern is maintained with a familiar two-visit procedure, including traditional cementation. There is value to both dentists and patients in the elimination of the physical impression, and because of electronic acquisition and submittal, there are no models to disinfect, package, and await pickup. The restorations show excellent fit and esthetics, owing to carefully processed zirconia using shaded translucent cores (Figure 7, Figure 8, Figure 9, Figure 10, Figure 11 and Figure 12).
Lastly, Sirona Dental Systems has recently announced the capability (CEREC® Connect) to scan preparations using its proven impression-free techniques to digitally transmit information to laboratories using CEREC inLab for the construction of zirconia cored and full-contour restorations. This capability gives dentists options for in-office restorations and impression-free laboratory-fabricated restorations—the best of both worlds.
In development for some time and recently announced, the E4D Dentist system (D4D Technologies LLC, Dallas, TX) also promises another in-office variant for the dentist (no laboratory link is available as of this writing). While clinical data is not yet available on this system, by now one thing should be clear: digital is everywhere and choices, in terms of in-office or off-site techniques, are becoming blurred.
The Future
Simply stated, the dental world has changed. Just as automation and machines have transformed nearly every industry, technology is changing dentistry as well. Many dentists are already using digital laboratories without even knowing it. This labor-intensive business is being transformed. To be sure, there will be capitalization costs, but the payoffs will be handsome. If precision can be enhanced while simultaneously improving productivity, lowering the cost per unit, what is the result? The effect is two-fold: it lowers the need to outsource, with cost savings realized by both laboratories and dentists. If a technician can improve his or her daily production with no sacrifice in quality, then it is easy to understand why 69% of all general practitioners in the United States today use laboratories with some form of CAD/CAM equipment.21
Some of the advantages that digital devices offer are the ability to eliminate bad impressions, lower costs, and provide predictable results. While technology alone cannot improve poor technique, sound operative methods along with CAD/CAM and other technologies can make technicians’ lives easier and laboratories more profitable. Patients will be happier and treatment outcomes will be enhanced. Although machines cannot replace a pair of good hands, certainly they can augment them. Digital tools are here to stay. With proven systems, such as CEREC, Lava C.O.S., and others, it is not a matter of if dentists will go digital, but when. The future of digital is very bright. Educate yourself and explore the possibilities.
References
1. Duret F, Blouin JL, Duret B. CAD-CAM in dentistry. J Am Dent Assoc. 1988;117(6):715-720.
2. Mörmann WH. The evolution of the CEREC system. J Am Dent Assoc. 2006;137(9 Suppl):7S-13S
3. Jörgensen KD, Matono R, Shimokobe H. Deformation of cavities and resin fillings in loaded teeth. Scand J Dent Res. 1976;84(1): 46-50.
4. Mörmann WH. The origin of the CEREC method: a personal review of the first 5 years. Int J Comput Dent. 2004;7(1):11-24.
5. Schmalz G, Federlin M, Reich E. Effect of dimension of luting space and luting composite on marginal adaptation of a Class II ceramic inlay. J Prosthet Dent. 1995;73(4):392-399.
6. Mörmann WH, Krejci I. Computer-designed inlays after 5 years in situ: clinical performance and scanning electron microscopic evaluation. Quintessence Int. 1992;23(2):109-115.
7. Fasbinder DJ. Clinical performance of chairside CAD/CAM restorations. J Am Dent Assoc. 2006;137(Suppl);22S-31S.
8. Rekow ED. Dental CAD/CAM systems: A 20-year success story. J Am Dent Assoc. 2006;137(9 Suppl):5S-6S
9. Malament KA, Socransky SS. Survival of Dicor glass-ceramic dental restorations over 14 years: Part I. Survival of Dicor complete coverage restorations and effect of internal surface acid etching, tooth position, gender, and age. J Prosthet Dent. 1999;81(1):23-32.
10. Krämer N, Frankenberger R. Clinical performance of bonded leucite-reinforced glass ceramic inlays and onlays after eight years. Dent Mater. 2005;21(3): 262-271.
11. Guess PC, Stappert CF, Strub JR. Preliminary clinical results of a prospective study of IPS e.max Press- and Cerec ProCAD-partial coverage crowns [in German]. Schweiz Monatsschr Zahnmed. 2006;116(5):493-500.
12. Posselt A, Kerschbaum T. Longevity of 2328 chairside CEREC inlays and onlays. Int J Comput Dent. 2003;6(3):231-248.
13. Giordano R. Materials for chairside CAD/CAM-produced restorations. J Am Dent Assoc. 2006;137(9 Suppl):14S-21S.
14. Dornhofer R, Arnetzl GV, Koller M, Arnetzl G. Comparison of the static loading capacity of all-ceramic bridge frameworks in posterior teeth using three hard core materials. Int J Comput Dent. 2007;10(4): 315-328.
15. Williams D. Ceramics transformed: manipulating crystal structures to toughen bioceramics. Med Device Technol. 1997;8(8):6-8.
16. Christel P, Meunier A, Heller M, et al. Mechanical properties and short-term in-vivo evaluation of yttrium-oxide-partially-stabilized zirconia. J Biomed Mater Res. 1989;23(1):45-61.
17. CAD/CAM technology restorative market expected to show marked increase over next seven years. Dental Lab Products. October 1, 2007. Available at: www.highbeam.com/doc/1P3-1371275601.html. Accessed September 12, 2008.
18. Gills D. Dental lab outsourcing. AGD Impact. 2006;34(4):24-28.
19. Christensen G. Coping with the offshore dental laboratory challenge. Clinician’s Report. 2008;1(4):1.
20. Estefan D, Dussetschleger F, Agosta C, et al. Scanning electron microscope evaluation of CEREC II and CEREC III inlays. Gen Dent. 2003;51(5): 450-454.
21. Goff S. Dental Products Report. 2008;April:54-62.
About the Author
Daniel J. Poticny, DDS
Co-founder
21st Century Practice Solutions
Dallas, Texas Private Practice
Dallas, Texas