Operating Microscopes and Restorative Excellence
David J. Clark, DDS
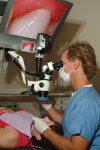
Operating microscopes are celebrating their 25th anniversary in dentistry. Initially resisted by endodontists and mainstream dentists, there has been a recent surge of interest in microscope-enhanced dentistry. In endodontics, the microscope is becoming standard equipment (Figure 1). At a recent opinion leader’s forum, the question was posed: “Should microscopes be required for all endodontic treatment?” This incredible swing in endodontic opinion also is being felt in general dentistry. As dental schools begin to integrate the microscope into the curriculum, two new frontiers in dentistry will be realized: minimally traumatic dentistry and zero-defect dentistry.
This brief article discusses a change in the endodontic-restorative protocol and then highlights a clinical case that demonstrates the tremendous advantage of advanced magnification when married with other forward-thinking techniques. The article concludes with an exploration of the rationale and science of zero-defect restorative dentistry, dentinal caries removal, and finally a review of the science of microscope-enhanced dentistry.
Modern Decision Making for the Compromised Tooth
Microscope-enhanced dentistry is changing the endodontic-restorative protocol, altering the thought process when determining when to save or extract a tooth. Microscopes offer additional methods for caries assessment and endodontic therapy, moving the profession closer to zero-defect restorative dentistry.
The decision to “extract or save” is a constantly evolving art form. In microscope-enhanced dentistry, the thought process in the endodontic-restorative protocol is often inversed. Rather than “endodontics then restorative, it is often restorative, then endodontics” as clinicians can assess the likely outcome and use this information in decision-making. Today’s finished case should be sealed exquisitely, pleasing esthetically, and accompanied by regenerated papillae. With advanced magnification, the additional visual information afforded to the clinician with the benefit of shadowless, coaxial light combined with infinity-corrected optics enhances the clinician’s ability to create clean, caries-free margins, which, in turn, can create an optimal restorative seal. Clinicians also can assess the actual invasion of the biologic width and potential for healthy and esthetic soft-tissue contours.1 For example, in the case presented, caries removal, margin identification, and the potential for papilla regeneration could be verified by restorative investigation. “Restorative investigation” is an important concept that is defined as “the clinical practice of prosthodontic disassembly, restoration removal, caries excavation, microsurgical access, and tissue retraction; the goal of which is to assess the true extent of dental pathology combined concurrent with the long-term restorative potential of the tooth.” 2 Only after these issues were deemed satisfactory was the pulp chamber re-accessed and endodontic therapy initiated. This evolution in triage has the potential to become the standard of care in the modern era of dentistry
Case Report
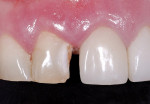
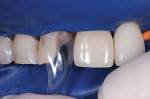
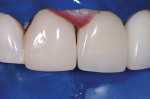
The patient, a 56-year-old woman, was vacillating between treatment plans for her upper arch: a full immediate upper denture or restorative reconstruction. While the treatment for the lower arch was proceeding, she began to experience pain with the upper right central incisor (Figure 2). She had a class reunion that was a week away. She desperately wanted to attend this important function without pain and with a smile that did not embarrass her.
Implants were not an option for the upper arch for financial reasons. The patient was faced with a decision of either removing the tooth and receiving a temporary partial denture or initiating restorative treatment combined with endodontic therapy. The patient chose the latter because it allowed for retention of the tooth as an interim treatment until a final decision was reached for the maxillary arch.
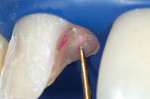
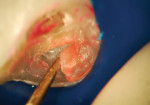
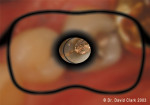
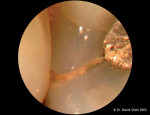
Figure 3 demonstrates the tooth after caries removal was thought to be complete. Although the dentin did not stain with caries-indicator solution, in the author’s experience the use of high magnification to evaluate hardness is the ultimate test of sound dentin. Magnification (16x) revealed that gross caries was still present. Figure 4 demonstrates exploration of the deepest layer of “noodle dentin.” Final evaluation of the nuances of sound dentin is demonstrated in Figure 5. A coarse diamond can be used to assess dentin because at 20x to 24x magnification the scratches can be used as clues to assess dentin hardness.3 Carr has shown that the unaided eye cannot distinguish between two lines that are closer together than 200 µm.3 With the microscope, 20-µm assessment is possible.
To create an ideal embrasure form, a Bioclear matrix (Bioclear, Tacoma, WA) was used (Figure 6 and Figure 7). This anatomically shaped matrix encourages the papilla to regenerate.4 The composite was cured, then shaped and polished. Modern porcelain polishers, such as the Jazz™ series (SS White Burs, Inc, Lakewood, NJ) or DuFine™ (Clinician’s Choice, New Milford, CT), yield a finish that is absolutely breathtaking (Figure 8).
Zero-defect restorative dentristy
Caries removal is a fundamental task of traditional dentistry. Although there are many ways in which a clinician can assess carious dentin, today’s most common approaches include radiographs, caries-indicator dye, spoon excavator or explorer tip (tactile hardness) tests, and laser fluorescence detection.5,6
The presumption that healthy dentin is “harder” is supported by extensive research.7 The most predictable clinical indicator of sound vs unsound dentin is hardness.8 The Knoop hardness scale of infected dentin ranges from 0 to 30, affected dentin from 30 to 70, and healthy dentin from 70 to 90. Ideally, dentin removal should be terminated once the affected dentin has been reached, in the 40 to 50 Knoop hardness range. Microscopic evaluation at extreme levels of magnification provides additional visual information to assess the texture and hardness of dentin that can augment the traditional tactile approach to dentin hardness.
Maintaining areas of affected dentin that may be discolored will not compromise the tooth-restoration complex.9 However, some studies have shown a compromised long-term resin bond to discolored, affected, and amalgam-contaminated dentin.10 In these cases, the use of a glass-ionomer sandwich technique is an option, which can have a more stable long-term bond (glass-ionomer–dentin interface) to compromised dentin.11 Alternatively, an enhancement of other, more predictable surfaces (ie, creating longer enamel margins or dentinal undercuts) could be used in lieu of a glass-ionomer sandwich.
Dentin color is one of the least predictable indicators of sound dentin, ie black, brown, and green dentin in previously restored teeth is often noncarious and should not be removed.12 Conversely, normal-colored dentin can be soft and grossly infected but appear normal at low magnification. In these cases, caries-indicator dye often can give a “false negative” to stain uptake. In other words, the dentin can have a normal color, and yet be so soft that no absorption of caries-indicator solution occurs. A study comparing different diagnostic approaches to occlusal caries assessment found that visual techniques without advanced magnification were correct only 53% of the time and caries-disclosing dyes were accurate only 43% of the time.13 While laser fluorescence can be very accurate,14 its use in most practices is for initial diagnosis. Use of such instruments such as a DIAGNOdent (KaVo, Lake Zurich, IL) for on-the-fly diagnosis during cutting of the tooth is both impractical and nonspecific (a positive reading of 20 or above indicates that caries is present but not precisely where the carious and noncarious tooth structures are). In the case presented, the dentin in Figure 2 was treated with caries-indicator dye and had no stain uptake. It is the author’s opinion that without the microscope he could have easily been lulled into a false sense of security that caries removal was complete. Leaving gross residual caries at the margin areas contradicts many restorative principles and could have doomed this case to premature failure.
Clinical Microscopes—Luxury or Necessity?
The operating microscope is not just simply higher magnification than oculars (loupes). It is better magnification. Oculars have been very helpful and may always have a role in dentistry, but the optics are crude when compared to the infinity-corrected optics of a stereoscopic microscope (Figure 9, Figure 10, Figure 11 and Figure 12). When combined with the shadowless coaxial light source, they transform the clinician’s potential for accuracy of nearly every aspect in the different disciplines in dentistry.
Increasing levels of magnification produce a squared, not linear, relationship to visual acuity. In other words, a clinician working at 3.5x sees 10 times more visual information; 10x magnification allows 100 times more information; and 20x magnification allows 400 times the visual information (Table 1).15 Improved outcomes from the use of magnification have been well documented in the medical literature, and scientific validation in dentistry is beginning to emerge.16-24
Many studies have shown that magnification plays an important role in clinical accuracy, such as the ability to access and shape complex root canal anatomy. In a compelling study, the use of a microscope enabled the author, an endodontist, to improve his ability to find a fourth canal system from 73% to 93% of maxillary first molars.25,26 Other studies show that the use of an operating microscope can lead to less postoperative discomfort.27 In periodontics, the microscope enhances the surgeon’s visual acuity,28 allowing better manipulation and more accurate suturing of the soft tissues.29 Low tissue trauma, excellent flap control, and a micro-suturing technique that allows primary wound closure may be responsible for improved clinical success.30,31 Reduced operator mistakes in endodontics have been reported as a benefit of clinical microscopes.32 The ergonomics of the microscope clinician’s proper posture have shown a remarkable reduction in back pain and disability, a priceless benefit to the practitioner, for that pervasive and serious problem can destroy our health and diminish the daily enjoyment of our craft.33-35
Conclusion
Excellence in dentistry is both a choice and a journey, and magnification can be a powerful asset for those who seek absolute clinical accuracy. The testimony of dentists who use the microscope daily in their practices confirms its value. An overwhelming majority affirms that it has improved their clinical skills. The microscope, with instantaneous magnification from 2.5x to 24x, with no visual noise and shadowless coaxial light, offers the best means for achieving complete visual information in dentistry. It can nurture great confidence, healthier posture, and better and surer hands for the clinician. And in the end, the excellent visual information it offers can help the dentist to create more precise, more healthful, and more esthetically pleasing dentistry.
Disclosure
Dr. Clark has no financial interest in any microscope company. Dr. Clark has a financial interest in the Bioclear Matrix System. He is also the co-developer of the CK endodontic access burs currently in prototype stage at SS White Burs, Inc.
References
1. Clark DJ, Kim J. Optimizing gingival esthetics; a microscopic perspective. Oral Health. 2005;April:116-126.
2. Clark DJ, Sheets CG, Paquette JM. Definitive diagnosis of early enamel and dentinal cracks based on microscopic evaluation. J Esthet Restor Dent. 2003;15 (special issue):7:391-401.
3. Carr GB, Magnification and illumination in endodontics. In: Hardin JF. Clark’s Clinical Dentistry. Vol 4. New York, NY: Mosby; 1998:1-14.
4. Clark DJ. Restoratively driven papilla regeneration. Canadian Journal of Restorative Dentistry and Prosthodontics. 2008;August(1-2):40-46.
5. Chong MJ, Seow WK, Purdie DM, et al. Visual-tactile examination compared with conventional radiography, digital radiography, and Diagnodent in the diagnosis of occlusal occult caries in extracted premolars. Pediatr Dent. 2003;25(4):341-9.
6. Magid KS. Caries diagnosis: the necessity for a new standard of care. Review. Alpha Omega. 1996;89(3):6-10.
7. Hosoya Y, Marshall SJ, Watanabc LG, Marshell GW. Microhardness of carious deciduous dentin. Oper Dent. 2000;25(2):81-89.
8. Meredith N, Sherriff DJ, Swanson SAV. Measurement of the microhardness and Youngs’s modulus of human enamel and dentin using an indentation technique. Arch Oral Biol. 1996;41:539-545.
9. Terashima S, Watanabe M, Kurosaki N, Kono A. Hardness of dentin remaining after clinical excavation of soft dentin. Japanese J Conserv Dent. 1969;11: 115-120.
10. Erhardt MC, Toledano M, Osorio R, et al. Histomorphologic characterization and bond strength evaluation of caries affected dentin/resin interfaces: Effects of long term water exposure. Dent Mater. 2008; 24(6):786-798.
11. Mount GJ. Clinical performance of glass ionomers. Biomaterials. 1998;19(6):573579.
12. Fusayama T, Okuse K, Hosada H. Relationship between hardness, discoloration and microbial invasion in carious dentin. J Dent Res. 1966;45(4):1033-1046.
13. Antonson DE, Antonson SA, Jataba A. Occlusal caries diagnosis comparing visual and caries detection solution. J Dent Res. 2000;79(Special Issue):198, abstract no. 439.
14. Summitt JB, Shin DH, Garcia-Godoy F, Gor GK. Accuracy of various diagnostic methods in detecting fissure caries lesions. J Dent Res. 2000;79(Special Issue):198, abstract no. 433.
15. Clark DJ. Advanced techniques for diastema closure: A microscopit perspective. 2007; September:36-41.
16. Friedman MF. Magnification in a restorative dental practice: From loupes to microscopes. Compend Cont Educ Dent. 2004; 25(1):48-55.
17. Jacobsen JH, Suarez EL. Microsurgery in anastomosis of small vessels. Surgery Forum. 1960;11:243-245.
18. Kleinert HE, Kasdan ML. Anastomosis of digital vessels. J Ky Med Assoc. 1965;63;106-108.
19. McClean DH, Buncke HJ. Autotransplant of omentum to a large scalp defect with a microsurgial revascularization. Plast Reconstr Surg. 1972;49(3):268-274.
20. Simonsen FJ. The use of field magnification. Quintessence Int. 1985;16:445
21. Chau TM, Pameijer CH, The application of microdentistry in fixed prosthodontics. J Prost Dent. 1985;54(1):36-42.
22. Whitehead SA, Wilson NH. Restorative decision-making behavior with magnification. Quintessence Int. 1992;23: 667-671.
23. Leknius C, Geissberger M. The effect of magnification on the performance of fixed prosthodontic procedures. J Calif Dent Assoc. 1995;23(12):66-70.
24. Michaelides PL. Use of the operating microscope in dentistry. J Calif Dent Assoc.1996;24(6):45-50.
25. Stropko JJ. Canal morphology of maxillary molars: clinical observations of canal configurations. J Endod. 1999 Jun;25(6):446-450.
26. Saunders WP, Saunders EM. Conventional endodontics and the operating microscope. Dent Clin North Am. 1997;41(3): 415-428.
27. Pecora G, Andrena S. Use of the dental operating microscope in endodontic surgery. OralSurg Oral Med Oral Pathol. 1993;75(6):751-775.
28. Francetti L, Del Fabro M, Testori T, Weinstein RL. Periodontal microsurgery: Report of 16 cases consecutively treated by the free rotated papilla autograft technique combined with the coronally positioned flap. Int J Periodontics Restorative Dent. 2004:24(3): 272-279.
29. Belcher JM. A perspective on periodontal microsurgery. Int J Periodontics Restorative Dent. 2001;21(2):191-196.
30. Akimoto K, Becker W, Persson R, et al. Evaluation of titanium implants placed into simulation extraction sockets: A study in dogs. Int J Oral Maxillofac Implants. 1999; 14(3):351-360.
31. Hurzler MB, Quinones CR, Hutmacher D, Schupbach P. Guided bone regeneration around dental implants in the atrophic alveolar ridge using a bioresorbable barrier. An experimental study in the monkey. Clin Oral Implants Res. 1997;8(5): 323-331.
32. Carr GB. Common errors in peri-radicular surgery. Endod Rep. 1993;8(1):12-18.
33. Murphy DC. Ergonomics and dentistry. NY State Dent J. 1997;63(7): 30-34.
34. Lehto TU, Helenius HY, Alaranta HT. Musculoskeletal symptoms of dentists assessed by a multidisciplinary approach. Community Dent Oral Epidemiol.1991; 19(1):38-44.
35. Rucker LM. Surgical magnification: posture maker or posture breaker? In: Murphy D, ed. Ergonomics and the Dental Care Worker. Washington DC: American Public Health Association; 1998:191-213.
About the Author
David J. Clark, DDS
Founder
Academy of Microscope Enhanced Dentistry
Fort Wayne, Indiana
Course Director
Newport Coast Oral Facial Institute
Newport Beach, California