The Tunnel Technique in the Periodontal Plastic Treatment of Multiple Adjacent Gingival Recession Defects: A Review
Henry Salama, DMD; Maurice Salama, DMD; David Garber, DMD
The generally accepted properties of an esthetic smile include harmony, balance, and continuity of form. Gingival recession within the esthetic zone is a primary disruptor of these properties and often must be corrected if an esthetic smile is to be achieved. Periodontal plastic therapeutic surgical techniques are the clinician’s tools for correcting such defects. Many surgical protocols have been described to achieve root coverage successfully. This article reviews and describes the tunnel technique with subepithelial connective tissue grafts for the coverage of multiple adjacent gingival recessions.
The axiomatic goal of reconstructive therapy is the restoration of health, function, and esthetics, which often requires correcting gingival recession defects within the esthetic zone. To that end, periodontal plastic procedures generally are used. Several surgical techniques have been described in the literature to correct gingival recession defects successfully.1-10 Langer and Langer1 used a subepithelial connective tissue graft (CTG) covered by a coronally positioned flap to achieve root coverage. Raetzke2 described the envelope technique to place the CTG without the vertical incisions required in a coronally positioned graft. Zabalegui et al6 were the first to combine these techniques in the treatment of multiple adjacent gingival recession defects through the use of a mucosal partial-thickness “tunnel,” spanning multiple teeth, to introduce the CTG. Zuhr et al10 recently suggested the incorporation of specialized microsurgical periodontal plastic protocols and instruments for the application of similar techniques in reconstructing gingival defects. This article reviews the surgical protocol required to use the tunnel technique in the treatment of multiple adjacent recession defects.
Case Report
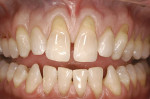
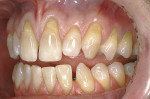
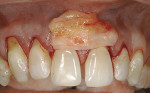
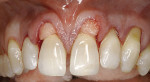
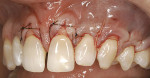
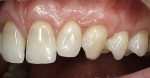
A 55-year-old man presented with significant gingival recession in all three of the maxillary sextants (Figure 1a and Figure 1b). Previously placed and failing Class 5 restorations were present on several of the exposed root surfaces. Minor toothbrush abrasion was present on the left maxillary canine, with the patient exhibiting minor tooth sensitivity. No mobility or fremitus was evident in any of the maxillary sextants in question. The patient’s desire was to improve the esthetics of his smile as well as control what had been an increasing degree of recession.
Treatment Design—Part 1: Preparation
In preparation for treatment of a patient with generalized patterns of gingival re-cession, clinicians must first rule out or identify and control any occlusal etiology that may be a contributing factor to the progression of the recession patterns. In addition, instruction in proper toothbrushing and hygiene must be undertaken before, during, and after therapy to ensure that any periodontal plastic procedures that are undertaken will not be traumatized by the patient’s oral hygiene regimen.
Before commencing with any surgical intervention, any questionable restorations must be removed and replaced if necessary. If these restorations are extremely shallow, their influence can be eliminated by root planing in the process of flattening the root convexity, which actually aids the process of root coverage. If the restorations to be replaced are deeper, the authors prefer to replace them with the newest class of glass-ionomer restorative material, which exhibits the properties of being densified, condensable, and viscous (GC Fuji IX GP, GC America Inc, Alsip, IL).
Treatment Design—Part 2: Flap Design and Choice of Graft Material
Given the patient’s midline diastema and multiple adjacent recession defect, the authors decided on an envelope tunnel6,8 type of flap design that would preserve the level of the midline papilla best. This design also would maintain the best available vascularity for the tissue grafts that will be used to cover the defects. This surgical approach has the advantage of not incising into or reflecting many of the papillae within the surgical site, thereby minimizing the risk of losing papilla height in critical areas.
The type of graft to be used when the roots will be covered using a tunnel flap design depends on the decision of whether the surgeon decides to position the flap coronally. When deep recession defects exist and a coronally positioned flap is contraindicated because of the desire to maximize the zone of keratinized attached gingiva, the authors prefer the use of subepithelial CTGs as described by Langer and Langer in 19851. This type of graft is chosen because of its increased ability to survive when a portion of the graft is left exposed. This survivability often negates the need to reposition the flap coronally and altering the position of the mucogingival margin.
However, if the recession is shallow and/or a wide zone of keratinized, attached gingiva exists beyond the recession defects, then a coronally positioned flap may be contemplated to cover an acellular collagen matrix (AlloDerm®, LifeCell Corp, Branchburg, NJ) completely. The use of an acellular collagen matrix as a graft material eliminates the requirement for an additional donor site, which is necessary when harvesting autologous soft-tissue grafts, and thereby reduces the trauma to the patient. However, the authors have found that predictable success with this type of graft material requires complete flap coverage to maximize the potential for re-vascularization of the graft and is, therefore, not always the best option when coronal repositioning of the labial flap is not possible or desired.
While subepithelial CTG usually heal with a greatly reduced postoperative sequela when compared to free gingival grafts, it is still prudent to prepare a retainer with a palatal stent to protect the potential donor site(s) during the first week of healing.
Treatment Design—Part 3: Surgical Procedure
After the preparation phase, the surgical visit began with local infiltration of anesthesia in the vestibule and in the palate. Care was taken not to inject intrapapillary or intrasulcularly, especially because of the use of an epinephrine-infused anesthetic, so as not to compromise vascularity to those areas during or after the surgery.
The root surfaces were planed and treated for 4 to 5 minutes with a tetracycline HCL paste, which was made by mixing the antibiotic with saline. The literature suggests that treating the root surface before connective tissue grafts with any of several substances, such as tetracycline HCL, citric acid, or enamel matrix derivative, can impart a positive effect on successful outcomes.11-13
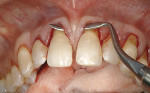
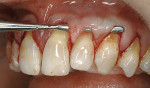
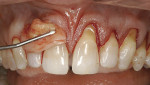
Sulcular incisions on the labial and buccal only were performed with a Bard-Parker™ No. 15 blade (Becton, Dickinson, and Co, Franklin Lakes, NJ) to begin the partial-thickness dissection. The split-thickness dissection then was extended until continuity was established between all the recession sites without raising the papillae (Figure 2a and Figure 2b).
When using standard straight-cutting instruments, it is often difficult, if not impossible, to extend the dissection effectively and to navigate the rounded transitional line angles of the teeth, as well as release the papillae, without perforating the labial flap. To enhance the efficacious performance of periodontal plastic procedures in these difficult areas, specialized curved microsurgical instruments and knives were used (Tunneling Kit, Stoma USA Inc, Melville, NY) (Figure 2c and Figure 2d). These instruments not only have the curvature required to hug the root surfaces during dissection, but also are small enough to cut safely in the restricted areas of the papillae.
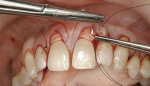
Subepithelial CTGs were harvested from both sides of the palate and measured for dimensional appropriateness in the areas of the defects (Figure 3a). The CTGs were trimmed to size using sharp surgical blades. After the size of the re-quired graft was established, the access for the graft to the subgingival space was ascertained (Figure 3b). If the graft is significantly large, alternating papillae may require release to facilitate the placement of the graft. Of course, critical papillae, such as at the midline, should never be compromised (Figure 3c).
After the grafts were in place, microsurgical instruments were used to suture and stabilize the grafts with the overlying gingival flap. In the papillae regions, vertical mattress monofilament sutures of 5-0 and 6-0 were used for this purpose (Monocryl™, Ethicon, Inc, Somerville, NJ) (Figure 4a and Figure 4b). This periodontal plastic microsurgical approach to flap dissection and suturing is much less traumatic to the surrounding tissue and is, therefore, more likely to better maintain the vascularity of the surgical site during the critical early healing period. No periodontal dressings are used if adequate stability of the graft and flap is achieved.
The patient was instructed not to brush the surgical sites for the first 2 weeks. Instead, during that time, he was instructed to rinse with 0.2% chlorhexidine digluconate for 2 to 3 times per day. Anti-inflammatory and pain control medications were prescribed for use as needed. At the 2-week postoperative visit, any remaining sutures were removed and oral hygiene and plaque control was reviewed and reinforced.
Discussion
The generally accepted properties of an esthetic smile include harmony, balance, and continuity of form. Gingival recession within the esthetic zone is a primary disruptor of these properties and often must be corrected if an esthetic smile is to be achieved. Periodontal plastic therapeutic surgical techniques are the clinician’s tools for correcting such defects. The number one advantage of a surgical solution to denuded roots, if it is achievable, is the ability to minimize restorative intervention in many instances. In addition to regaining an esthetic gingival profile through root coverage, the increased zone of keratinized, attached gingiva creates a more maintainable periodontal environment, usually with significantly less sensitivity.
The tunnel technique is an approach that optimizes esthetics and predictability because of its ability to avoid releasing critical papillae and maintaining a high level of vascularity at the surgical site to support the grafts.
Conclusion
The extent and predictability of root coverage procedures for the treatment of recession defects are dependent on the quality of the vascularity that is maintained at the surgical site. The tunnel, or envelope, technique optimizes vascularity by eliminating the need for vertical releasing incisions. Furthermore, when adjacent recession defects are present and are connected by an esthetically critical papilla, the tunnel technique is an excellent approach to protect the positional height of the papilla.10 This flap design, in combination with partial-thickness dissection, creates the most optimal and vascular sub-gingival environment for the placement of subepithelial or acellular collagen matrix type of grafts.
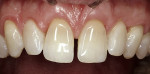
However, this surgical protocol is more technique-sensitive than standard full-thickness flap approaches because the clinician must work in a more confined environment. Microsurgical instruments, therefore, are required to navigate and adequately release the flap and papillae around small curved surfaces. Using proper protocols, this ap-proach is a very successful and predictable method of treating multiple adjacent root recession defects without compromising the height of critical papillae (Figure 5a and Figure 5b).
References
1. Langer B, Langer L. Subepithelial connective tissue graft technique for root coverage. J Periodontol. 1985;56(12):715-720.
2. Raetzke PB. Covering localized areas of root exposure employing the “envelope” technique. J Periodontol. 1985;56(7): 397-402.
3. Tarnow DP. Semilunar coronally repositioned flap. J Clin Periodontol. 1986;13(3):182-185.
4. Harris RJ. The connective tissue and partial thickness double pedicle graft: a predictable method of obtaining root coverage. J Periodontol. 1992;63(5): 477-486.
5. Allen AL. Use of a supraperiosteal envelope in soft tissue grafting for root coverage. I. Rationale and technique. Int J Periodontics Restorative Dent. 1994;14(3):216-227.
6. Zabelgui I, Sicilia A, Cambra J, et al. Treatment of multiple adjacent gingival recessions with the tunnel subepithelial connective tissue graft: a clinical report. Int J Periodontics Restorative Dent. 1999;19(2): 199-206.
7. Guiha R, el Khodeiry S, Mota L, et al. Histological evaluation of healing and revascularization of the subepithelial connective tissue graft. J Periodontol. 2001;72(4): 470-478.
8. Azzi R, Etienne D, Takei H, et al. Surgical thickening of the existing gingiva and reconstruction of interdental papillae around implant-supported restorations. Int J Periodontics Restorative Dent. 2002;22(1):71-77.
9. Burkhardt R, Lang NP. Coverage of localized gingival recessions: comparison of micro- and macrosurgical techniques. J Clin Periodontol. 2005;32(3): 287-293.
10. Zuhr O, Fickl S, Wachtel H, et al. Covering of gingival recessions with a modified microsurgical tunnel technique: case report. Int J Periodontics Restorative Dent. 2007;27(5):457-463.
11. Trombelli L, Scabbia A, Wikesjö UM, Calura G. Fibrin glue application in conjunction with tetracycline root conditioning and coronally positioned flap procedure in the treatment of human gingival recession defects. J Clin Periodontol. 1996;23(9):861-867.
12. Bouchard P, Nilveus R, Etienne D. Clinical evaluation of tetracycline HCl conditioning in the treatment of gingival recessions. A comparative study. J Periodontol. 1997;68(3):262-269.
13. Castellanos A, de la Rosa M, de la Garza M, Caffesse RG. Enamel matrix derivative and coronal flaps to cover marginal tissue recessions. J Periodontol. 2006;77(1): 7-14.
About the Authors
Henry Salama, DMD
Private Practice,
Atlanta, Georgia
Maurice Salama, DMD
Clinical Assistant Professor Periodontics
Medical College of Georgia
Augusta, Georgia
Private Practice
Atlanta, Georgia
David Garber, DMD
Clinical Professor
Department of Periodontics
Medical College of Georgia School of Dentistry
Augusta Georgia
Clinical Professor
Department of Oral Rehabilitation
Medical College of Georgia School of Dentistry
Augusta Georgia
Visting Professor
Department of Prosthodontics
Louisiana State University
Baton Rouge, Louisiana