A Dual-Cure Composite Core for Teeth to Be Restored with Full Crowns
Howard E. Strassler, DMD; Lyndsay C. Bare, DDS
Teeth that are significantly damaged with missing tooth structure from fracture, caries, or wear, or are structurally weakened from a restoration on multiple surfaces usually require definitive restoration with a full-coverage crown.1 Typically, before preparation and restoration with a crown, the existing defective restoration needs to be replaced or the missing tooth structure needs to be rebuilt so that the crown preparation can fulfill the retentive needs of the crown to be placed. In the case of an endodontically treated tooth, a number of studies have focused on functional stresses to the tooth crown when it is restored with a post and bonded composite resin vs restoring it with an integral cast metal post and core. The results of these studies have demonstrated that failure occurs at the interface between the restorative material and the tooth.2,3 Therefore, when preparing a tooth restored with a core that will receive a crown, the design of the crown preparation must have a ferrule of at least 1 mm to 2 mm beyond the core material and the ferrule must extend 360° around the crown margins.2,4
When a foundation restoration is to be placed, the clinician can choose from a variety of restorative materials. For teeth that are not endodontically treated, amalgam, composite resin, and glass ionomer may be used as direct-placement restorative materials to create the foundations. Because of its physical properties, amalgam has been described as the material of choice for most foundations on posterior teeth; however, in cases where the tooth is missing cusps, amalgam usually requires additional retention with pins, slots, and grooves. When amalgam and composite resin were compared as core materials under cast crowns, no significant differences in the degree of microleakage were found.5 When compared with amalgam and composite resin, glass ionomer has been found to exhibit comparatively weaker physical properties.6,7 Glass ionomer should be limited to restoring teeth when sufficient tooth structure remains to support and retain the crown.8,9
When used as a crown foundation, composite resin demonstrates advantages over both amalgam and glass ionomer. Composite resins are bondable to tooth structure, which minimizes the need for additional retention and cavity preparation before placing the core restoration. Also, composite resin, either as a light-cure or dual-cure formulation, is easy to place and adapt by syringing it into the cavity preparation as compared with amalgam condensation, and it sets rapidly so that the crown can be prepared in the same visit.1 Some formulations of composite resins release fluoride and may provide an anticariogenic effect.10 While shaded composite resins are used routinely to restore teeth, using a composite resin that is slightly different in color from the tooth’s shade can make the tooth‐composite resin junction visible during tooth preparation.1 For these cases, the tooth preparation should extend at least 1 mm past the core build-up.11
For the case described, the decision was made to use a composite core build-up material with unique properties. Comp-Core™ AF SyringeMix™ Stack & Twist (Premier Dental Products, Plymouth Meeting, PA) is a dual-cure composite core build-up material with hyper-branched polymer technology, fluoride release, and a high radiopacity. This composite core material is very radiopaque, making it easy to differentiate the tooth and composite material in radiographs. It is available in two colors that are easy to distinguish from tooth structure during crown preparation. Shade A3 is a dentin shade that can be used underneath all-ceramic restorations. The white shade can be used for any core build-up for metal and porcelain-fused-to-metal crowns. The stackable consistency of the composite allows it to be placed without fear of flow away from the cavity margins, yet its viscosity permits easy adaptation to the preparation cavity walls, margins, and matrix band.
Case Report
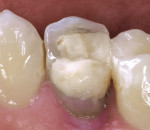
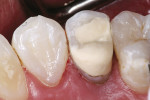
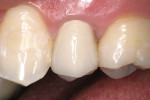
A 24-year-old patient presented with an endodontically treated maxillary second premolar that had a defective, pin-retained composite resin restoration that restored the lingual cusp (Figure 1). After a thorough periodontal, endodontic, and hard tissue evaluation, the tooth was treatment planned for a prefabricated post and, if at all possible during removal of the defective restoration, retention of the existing pin, followed by restoration with a composite resin core. The definitive restoration for the premolar was treatment planned as an all-ceramic crown.
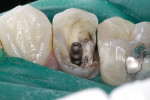
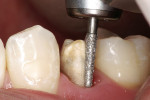
During endodontic treatment, a post space was made that left at least 5 mm of remaining gutta-percha to maintain the apical seal of the endodontic filling. The length of a post space should be at least half the root length while still maintaining the apical seal of gutta percha.12,13 The defective composite resin was removed using a 245-GW Great White bur (SS White Burs, Inc, Lakewood, NJ). The Great White bur was selected because its fluted blades were more dentate than crosscut burs. These burs have a unique geometry in the design of their blades, which creates a bur that cuts quickly and more efficiently with less vibration when cutting into tooth structure or dental materials. This translates into less stress on the tooth, its supporting periodontal structures, and pulp. During endodontic treatment, the endodontist had placed a cotton pellet and conventional glass ionomer (Fuji IX, GC America, Inc, Alsip, IL) to fill the access opening. During preparation, the pin previously placed was maintained and the endodontic access to the root canal was visualized easily when the glass ionomer and cotton pellet were removed. A prefabricated parallel-sided, serrated post with a retentive head design (IntegraPost™, Premier Dental Products) was selected to provide additional retention to the composite core.14,15 The post space was sized with the endodontic post reamer in the post kit, and the post was then tried in (Figure 2).
Post Cementation
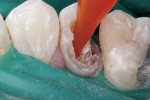
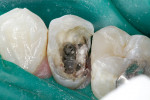
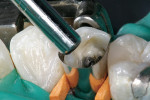
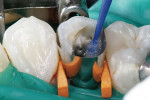
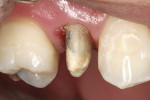
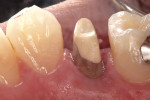
A self-etching adhesive technique was used to cement the post. Using a micro-applicator brush, a self-etching bond enhancer (Bond Boost SE™, Premier Dental Products) was thinly painted on all the walls of the root canal. Bond Boost SE can be used with any etch-and-rinse adhesive system as a substitute for acid-etching of dentin. After 20 seconds, the bond enhancer was gently air-dried. A single-bottle, fifth-generation adhesive was mixed with its dual-cure activator (IntegraBond™, Premier Dental Products) and thinly applied to the root canal. A dual-cure composite resin cement (IntegraCem™, Premier Dental Products) was injected into the root canal using an application tube (Centrix, Inc, Shelton, CT) (Figure 3) and the post was cemented (Figure 4).
Core Build-up
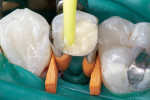
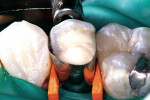
After post cementation, a matrix band and wedges were applied to the tooth preparation. Bond Boost SE was reapplied to the cavity preparation for 20 seconds and air-dried (Figure 5). IntegraBond was mixed with its activator to make it dual-cure and was applied to the cavity preparation with a disposable micro-brush applicator (Figure 6). The dual-cured, fluoride-releasing composite core material (CompCore AF SyringeMix Stack & Twist) was applied directly from its dual-barreled syringe using an automixing tip with applicator (Figure 7). For snap polymerization, the core was light-cured for 30 seconds with a quartz halogen curing light (Optilux 500, Kerr Corp, Orange, CA), keeping the light probe as close to the preparation as possible at right angles to the tooth preparation. The composite core was restored in one application (Figure 8). The matrix was removed and the composite resin core was finished. The occlusion was adjusted and evaluated because it would be used to make the template for the provisional crown restoration (Figure 9). For fabrication of the provisional restoration, a bite impression template was made with a fast-setting regular body vinyl polysiloxane (VPS) impression material.
Crown Restoration
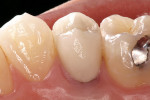
The maxillary premolar was prepared for an all-ceramic zirconia core crown using a shoulder preparation diamond (Piranha, SS White Burs, Inc) (Figure 10). The final crown preparation demonstrated sufficient ferrule with the composite core, and the CompCore AF shade A3 provided a differentiation in color from the tooth to be certain the margins were on sound tooth structure (Figure 11A and Figure 11B). An impression was made using a bite impression technique with a fast-setting regular body VPS impression material (ExaFlex, GC America, Inc). A provisional restoration was fabricated using the bite-impression template technique with a bis-Acryl provisional resin material (Integrity™, DENTSPLY Caulk, Milford, DE). The provisional restoration was adjusted and polished, and then cemented on the premolar with an automixing, neutral-shaded, eugenol-free temporary resin cement that contained fluoride, potassium nitrate for desensitizing, and antimicrobial chlorhexidine (NexTemp™, Premier Dental Products).
The impression was sent to the dental laboratory for fabrication of the all-ceramic crown with a zirconia coping (Procera®, Nobel Biocare USA, LLC, Yorba Linda, CA). The crown was returned by the laboratory, and was tried in and adjusted for proximal contact and occlusion. The margins were evaluated and determined to be very well-fitting. The Procera crown was ce-mented using the same adhesive technique as was described for the post system—self-etching bond enhancer (Bond Boost SE) applied for 20 seconds and dried, dual-cure fifth-generation adhesive (IntegraBond), and a dual-cure composite resin cement (IntegraCem). The cement was applied in a thin layer into the cavity of the crown, and the crown was cemented, having the patient gently bite down on a saliva ejector to provide mechanical force to fully seat the restoration. The cement was cleaned away, and the occlusion was checked again. The final restoration was highly esthetic (Figure 12A and Figure 12B).
Conclusion
With the latest generation of composite core materials, restoring structurally deficient teeth with an adhesive composite resin is an acceptable alternative to traditional amalgam cores. Major benefits of using a composite core material are rapid set for immediate preparation for a crown, no need for additional retention because of adhesive technique, and acceptable physical properties to support a crown.
Disclosure
Dr. Strassler has received grant and research support from Centrix, Inc; GC America, Inc; and SS White Burs, Inc. He is a current consultant for Centrix, Inc, and SS White Burs, Inc.
References
1. Land MF, Rosenstiel SF. Mouth preparation. In: Rosenstiel SF, Land MF, Fujimoto J. Contemporary Fixed Prosthodontics. 4th ed. St. Louis, MO: Elsevier-Mosby; 2006:174-205.
2. Libman WJ, Nicholls JI. Load fatigue of teeth restored with cast posts and cores and complete crowns. Int J Prosthodont. 1995;8(2): 155-161.
3. Freeman MA, Nicholls JI, Kydd WL, et al. Leakage associated with load fatigue-induced preliminary failure of full crowns placed over three different post and core systems. J Endod. 1998;2491): 26-32.
4. Cheung W. Properties of and important concepts in restoring endodontically treated teeth. Dental Asia. 2004;5:40-47.
5. Yesil ZD. Microleakage of four core materials under complete cast crowns. N Y State Dent J. 2007;73(4):32-38.
6. Cho GC, Kaneko LM, Donovan TE, et al. Diametral and compressive strength of dental core materials. J Prosthet Dent. 1999;82(3): 272-276.
7. Coltak KM, Hanikolu ND, Bayindir F. A comparison of the fracture resistance of core materials using different types of posts. Quintessence Int. 2007;38(8):e511-e516.
8. Plasmans PJ, Kreulen CM, Creugers NH. A preliminary study on resin-modified glass-ionomer cement for transitional restorations and subsequent core buildups. Int J Prosthodont. 2000;13(5):373-377.
9. Wilson NH, Cowan AJ, Crisp RJ, et al. A short-term clinical evaluation of a tricure glass-ionomer system as a transitional restoration and core buildup material. Quintessence Int. 1999;30(6): 405-411.
10. Cohen BI, Pagnillo MK, Deutsch AS, et al. A five year study. Fluoride release of four re-inforced composite resins. Oral Health. 1998;88(4):81-86.
11. Fokkinga WA, Kreulen CM, Le Bell-Rönnlöf AM, et al. In vitro fracture behavior of maxillary premolars with metal crowns and several post-and-core systems. Eur J Oral Sci. 2006;114(3): 250-256.
12. Goodacre CJ, Spolnik KJ. The prosthodontic management of endodontically treated teeth: a literature review. Part III. Tooth preparation considerations. J Prosthodont. 1995;4(2):122-128.
13. Cheung W. A review of the management of endodontically treated teeth. J Am Dent Assoc. 2005;136(5):611-619.
14. Pettiette MT, Phillips C, Trope M. Effect of endodontic instrument taper on post retention. J Endod. 2003;29(1): 65-68.
15. Hew YS, Purton DG, Love RM. Evaluation of pre-fabricated root canal posts. J Oral Rehabil. 2001;28(3):207-211.
About the Authors
Howard E. Strassler, DMD
Professor and Director of Operative Dentistry
Department of Endodontics, Prosthodontics and Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland
Lyndsay C. Bare, DDS
Resident
AEGD Program
University of Maryland Dental School
Baltimore, Maryland