Esthetic Treatment: Soft Tissue Management and Functional Mock-Ups
Gregori M. Kurtzman, DDS; and Lee H. Silverstein, DDS, MS
Patients desiring a cosmetic smile improvement can present treatment planning challenges.1 An excessive display of gingiva resulting from a high lip line often complicates treatment planning and can compromise the final esthetic result. As we evaluate the patient, we often have to ask ourselves, do we "lower the river" (increase tooth length incisally), "raise the bridge" (increase tooth length gingivally) or use a combination of both approaches?
This article addresses this issue using a methodological approach to treatment planning and the execution of a functional mock-up to fine-tune the esthetics and achieve the patient's desires before finalization of the definitive restorations.
Functional Mock-ups
Anterior esthetic changes can pose challenges in communication between the patient and the dentist and between the dentist and the laboratory.2,3 The use of a functional mock-up permits development of the patient's esthetic goals intraorally.4-8 Modifications can be made and occlusion refined before finalization of the prosthetics.
Unlike temporary restorations, the functional mock-up can be placed before the removal of enamel and dentin and can be considered a reversible procedure. Should the patient and dentist be unable to reach a mutually agreeable esthetic conclusion before fabrication of the final prosthetics, the functional mock-up can be removed from the teeth and the patient is where he or she was before initiation of the esthetic treatment.
Soft Tissue Recontouring
When altering the soft tissue there are several surgical options. Traditionally, scalpels and periodontal knives (eg, Orban and Kirkland) were used to make the incisions and sculpt the soft tissue.9 This provides precise incisions but the resulting bleeding may complicate placement of resin restorations at the same appointment. Another option, monopolar electrosurgery, requires a dry field during treatment; this may increase tissue inflammation during the initial healing period and subsequent tissue shrinkage. "Charring" of the tissue margins at surgery has also been reported with monopolar electrosurgery and may be a result of the need for operating in a dry field.10,11
Bipolar electrosurgery was developed to overcome the obstacles associated with monopolar electrosurgery. The technology used today in dentistry is a crossover from neurosurgery, where delicate incisions are required in wet fields with no lateral heat generation. The Bident™ Bipolar Intraoral Surgical Unit (Synergetics™, Inc, King of Prussia, PA) transfers those neurosurgical requirements to the dental environment, allowing intraoral soft tissue surgery in wet fields with char-free, non-bleeding incision margins, thus permitting placement of immediate resin restorations without contamination of the resin by hematologic byproducts.12
When using the bipolar surgical unit, because the tips have two electrodes which are either straight wires or loops, one must remember that the first electrode to touch the tissue acts as the return and the second electrode does the cutting or coagulating depending on which foot pedal is depressed. As the bipolar surgical unit is fully isolated, a ground is not required. When cutting tissue, the authors advise that the assistant, while using the high-volume evacuation, constantly spray water from the air/water syringe to keep the field wet. This improves efficiency with the handpiece as well as preventing charring. Another benefit of the bipolar surgical unit is that even during cutting there is some coagulation that occurs, so the wound edges do not ooze and interfere with the procedures.13
Case Presentation
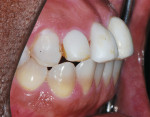
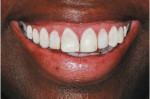
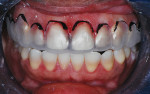
The patient, a 40-year-old woman, presented with a history of previous direct bonding to correct moderate tetracycline discoloration of the teeth and generalized diastemas. Examination revealed an excess display of gingiva when the patient smiled,14-16 as well as bulky, chipped, and discolored direct-resin restorations on the maxillary anterior teeth (Figure 1 and Figure 2). The patient expressed a desire for a less "gummy smile" and an overall improvement in the esthetics. A full series of radiographs was taken and a periodontal examination was performed. It was noted that a wide band of attached gingiva was present. Examination of the radiographs coordinated with intraoral probing determined that removal of 2 mm to 3 mm of gingival tissue would not encroach on the crestal margin of bone and an osseous component to the gingival surgery would not be needed.
The initial step in the planning process involved alteration of a full-smile photograph using software (Adobe® Photoshop®, Adobe, San Jose, CA) to assist in communication between the patient and clinician to determine what could be offered to achieve the patient's goals. It was decided that to eliminate the excessive gingival display the incisal edges of the maxillary teeth would be kept at their current position and the teeth lengthened at the expense of the gingiva. Alteration of the photograph closed the diastemas and attempted to provide ideal tooth proportions with a pleasing gingival contour. Ideal tooth proportions require a width-to-length ratio of 78%. In many cases, this may not be achievable, but an esthetic result that both the patient and practitioner are pleased with can still be arrived at.17 In this case, the width was altered to close the diastemas, and then the length was altered to achieve as close to a 78% ratio as possible with consideration to the overall esthetics and the soft tissue. No attempt was made to make the altered teeth appear natural in coloration in the photograph, as the altered photograph was to serve as a preliminary step in the planning process (Figure 3 and Figure 4).
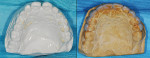
After a consultation with the patient and a discussion using the modified photograph, treatment progressed to a wax-up phase on the casts. A duplicate cast of the maxillary arch was altered to give the teeth normal thickness and eliminate the bulky composite that was present. This was followed by application of a dentin adhesive (Bond 1, Pentron Clinical Technologies, Wallingford, CT) to the cast to aid in retention of the wax-up to the cast. Next, composite (Simile®, Pentron Clinical Technologies) was applied to the cast and shaped with composite instruments so that contour and tooth proportions developed. Material was placed over the gingival aspect of the cast to position the tooth's cervical line where it would be positioned clinically using the modified photograph as a guide. When the contour and position of the composite were finalized the casts were cured with a hand-held curing light (Figure 5 and Figure 6).
The modified maxillary model was then placed into Futura floor wax and allowed to soak for 5 minutes, followed by bench drying for 30 minutes to seal the cast. Kromopan alginate (Kromopan, Des Plaines, IL) was mixed to a runny consistency with more water then normally used and placed into a rubber base-former. The modified cast was inserted tooth side down into the material and allowed to set. Upon setting, the model was separated from the alginate and a stone cast was poured. After the stone cast had completely set it was removed from the alginate and trimmed to eliminate the palatal area of the cast. This was performed to permit better adaptation of the vacuform material to fabricate stents.
Using a Druformat™ pressure-forming machine (DENTSPLY Raintree Essix, Metairie, LA) two separate stents were fabricated using Tray-Rite sheet material (DENSTPLY Raintree Essix). The first stent was trimmed to follow the gingival margins on the cast and would act as a guide during gingival surgery.18 To aid in visualization during surgery, a black sharpie marker was used to color the scalloped gingival margin of the surgical stent. The second stent was trimmed to be used as an intraoral form to fabricate the functional mock-up.
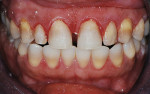
After application of local anesthetic, the first step at the clinical appointment was to strip the old composite using a diamond bur in a high-speed handpiece with water. Care was taken to avoid removal of any enamel at this time. Upon removal of the old composite, it was noted that the teeth had moderate tetracycline staining with a banded appearance. The maxillary lateral incisors were also noted to be in slight cross-bite orientation (Figure 7). The cross-bite situation was mild with no negative overbite, presenting with no contact between tooth No. 7 and the lower teeth when the teeth were moved into lateral excursions. The mock-up would be able to determine if during normal function, the resin at the incisal of tooth No. 7 would chip, which would then require consideration of a full-coverage restoration vs a labial veneer. When the maxillary tooth is "locked" behind the mandibular tooth, the cross-bite would not allow a more normal positioning of the maxillary tooth without drastic preparation of the tooth in cross-bite and would require orthodontic intervention to correct.
The surgical stent was inserted and assessment of the new gingival margins was made following the black edge of the surgical stent to ensure that adequate attached gingiva would remain after gingival recontouring (Figure 8). Using the bipolar surgical unit, a 3304 gingivectomy pen (Synergetics, Inc) was used to follow the edge of the surgical stent while the assistant sprayed a constant stream of water spray with one hand and used the high-volume evacuation device with her other hand. This allowed the tissue to remain hydrated and eliminated any tissue charring during the procedure. This permits improved healing with a lack of inflammatory response often seen with mono-polar soft tissue surgery. Healing time for a gingivectomy is approximately 3 weeks before the tissue is in a stable position and all associated inflammation is concluded.19-23 The Bident, because of the lack of heat at the cut margin and lack of inflammatory response, would permit progress to impressions or final restorations immediately with no healing change in the position of the new margin position. Osseous surgery requires longer periods of healing because of the manipulation of the osseous crestal position and greater amounts of soft tissue manipulation before a stable position is achieved. An additional benefit of the Bident Bipolar unit is a lack of tissue bleeding after treatment that could discolor the composite that is being placed. The stent was removed and gingival margins were further refined with the gingivectomy pen. Tissue was then planned back to develop good papilla contours using a 3302 gingivoplasty pen (Synergetics, Inc). Completion of the gingival recontouring did not result in exposure of the crestal bone and non-bleeding gingival margins were noted (Figure 9). The position of the crestal bone was determined through sulcular sounding with a periodontal probe. The information gathered indicated that some passive eruption issues were present and with the wide band of attached gingiva present would allow removal of 3 mm of gingival tissue and still provide a normal sulcular depth after healing.24-27 The restoration margins were placed at the new gingival margin position.
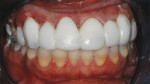
The functional mock-up stent was tried in and the gingival position was assessed (Figure 10). Teeth were isolated with cotton rolls and the facial and interproximal of teeth Nos. 5 through 12 were etched with a 37% phosphoric acid-etchant gel for 30 seconds then rinsed and dried. Bond 1 dentin adhesive was applied to all surfaces and light-cured for 20 seconds per tooth. The patient requested a very white bleaching shade and Artiste® nano composite (Pentron Clinical Technologies) Super Bleach dentin shade and Bleach enamel were selected for the functional mock-up. A thin layer of Bleach enamel shade was placed into the stent in the area of the incisal edge and incisal half of the coronal of teeth Nos. 4 through 13. Next, the Super Bleach dentin shade was placed into the stent and the facial aspect of each tooth was filled with material. The stent was then carried intraorally, seated, and adapted to the teeth with finger pressure. Each tooth was then light-cured for 30 seconds on the cervical followed by 30 seconds on the incisal. The stent was removed, leaving the bonded functional mock-up on the teeth, and additional light curing was performed. A needle finishing diamond (Brasseler USA, Savannah, GA) was used in a high-speed handpiece with water to remove the cervical flask and provide contours without any overhanging margins. Cervical embrasures were also opened and definition given to the interproximal line angles. Occlusion was checked in centric occlusion and lateral excursions and adjusted for proper anterior guidance. Polishing was accomplished using Fini™ polishing paste and a cloth buffer tip (Pentron Clinical Technologies) (Figure 11).
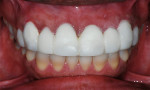
The patient was recalled 24 hours later to check soft tissue healing and assess the occlusion. At this time, minor refinement of the esthetics was accomplished and the patient indicated no irritation gingivally where tissue had been treated with the bipolar surgical unit. Slight sloughing of the keratinized layers of the tissue was observed but a lack of inflammation was noted (Figure 12). The patient was next seen at 2 weeks posttreatment. At this visit, it was noted that the soft tissue had a normal appearance in color and tone and no inflammation was observed. Further refinements in the esthetics were made in the functional mock-up, opening the incisal and gingival embrasures, shortening the incisal edges of the lateral incisors and working with the patient to achieve her view of ideal esthetics that would serve as a blueprint for the final restorations (Figure 13).
Figure 14 depicts the patient before and after correction of the "gummy" smile and placement of the functional mock-up. After a period of use of the functional mock-up to verify that the anterior guidance was not causing any chipping or damage to the functional mock-up, final restorations would be planned and a determination between ceramic veneers and full-coverage restorations would be made. The teeth would be prepared, stripping off all of the functional mock-up and the stent used to fabricate the functional mock-up would then be used to make a temporary prosthesis while the laboratory was fabricating the final restorations.
Conclusion
Often, when a patient presents seeking a cosmetic improvement we focus on the teeth and do not factor in the gingiva. To draw an artistic analogy, we need to consider the gingiva the frame and the teeth the picture. The frame accents and augments the picture it surrounds, taking a good result and making it better. A poor frame can also detract from the image, making a good result a poor outcome. As such, the gingiva may need to be trimmed and reshaped to provide better, more natural appearing contours.
The functional mock-up described here permits the practitioner and patient to fine tune the esthetics and test drive the occlusion before finalizing the case. An impression of this functional mock-up taken intraorally can help communicate to the laboratory what goals are desired. This also will help to eliminate a potential re-do of the prosthetics after delivery because of the patient's esthetic objections. Occlusal issues, such as inadequate anterior guidance or interferences in lateral cross-over, can be worked out before the final prosthetics, decreasing the chance of chipping and fracturing the ceramic.
Authors' Note
For a more detailed discussion and video capture of this case, please visit: www.kurtzman.bident.com.
Disclosure
Dr. Kurtzman is a current, non-financially compensated consultant for Synergistics USA.
References
1. Levine RA, Randel H. Multidisciplinary Approach to Solving Cosmetic Dilemmas in the Esthetic Zone. Contemporary Esthetics and Restorative Practice. 2001;5(6):62-67.
2. Rufenacht C. Fundamentals of Esthetics. Carol Stream, Il: Quintessence, 1960.
3. Morley J. A multidisciplinary approach to complex esthetic restoration with diagnostic planning. Pract Periodontics Aesthet Dent. 2000;12(6):575-577.
4. Chiche G, Kokich V, Caudill R. Diagnosis and treatment planning of esthetic problems. In: Pinault A, Chiche G, eds. Esthetics in Fixed Prosthodontics. Chicago: Quintessence; 1994.
5. Studer S, Zellweger U, Scharer P. The esthetic guidelines of the mucogingival complex for fixed prosthodontics. Pract Periodontics Aesthet Dent. 1996;8(4):333-341.
6. Smukler H,Chaibi M. Periodontal and dental considerations in clinical crown extension. A rational basis for treatment. Int J Periodont Rest Dent. 1997;17(5):464-477.
7. Garber DA, Salama MA. The aesthetic smile: diagnosis and treatment. Periodontal 2000. 1996;11(Jun):18-28.
8. Levine RA, McGuire M. Diagnosis and treatment of the gummy smile. Compend Contin Educ Dent. 1997;18(8):757-764.
9. Glassman S. Cosmetic treatment of the gummy smile. Contemporary Esthetics and Restorative Practice. 2001;5(1):58-61.
10. Livaditis GJ. Comparison of monopolar and bipolar electrosurgical modes for restorative dentistry: a review of the literature. J Prosthet Dent. 2001;86(4):390-399.
11. Malis LI. Electrosurgery and bipolar technology. Neurosurgery. 2006;58(1 Suppl):1-12.
12. Malis LI. Atraumatic bloodless removal of intramedullary hemangioblastomas of the spinal cord. J Neurosurg. 2002;97(1 Suppl):1-6.
13. Tucker RD, Hollenhorst MJ. Bipolar electrosurgical devices. Endosc Surg Allied Technol. 1993;1(2):110-113.
14. Coslet JG, Vanarsdall R, Weisgold A. Diagnosis and classification of delayed passive eruption of the dentogingival junction in the adult. Alpha Omegan. 1997;70(3): 24-28.
15. Pulliam RP, Melker D. Altered passive eruption: diagnosis and treatment. Contemporary Esthetics and Restorative Practice. 2002;6(4):20-30.
16. Dolt AH 3rd, Robbins JW. Altered passive eruption: an etiology of short clinical crowns. Quintessence Int. 1997;28(6):363-372.
17. Chu SJ. A biometric approach to predictable treatment of clinical crown discrepancies. Pract Proced Aesthet Dent. 2007;19(7): 401-409.
18. Spear F. Construction and Use of a Surgical Guide for Anterior Periodontal Surgery. Contemporary Esthetics and Restorative Practice. 1999;():12-20.
19. Landsberg CJ, Sarne O: Management of excessive gingival display following adult orthodontic treatment: A case report. Pract Proced Aesthet Dent. 2006;18(2):89-96.
20. Robbins JW. Esthetic gingival recontouring—caveat emptor. Contemporary Esthetics and Restorative Practice. 2002;6(4):666-674.
21. Allen EP. Surgical crown lengthening for function and esthetics. Dent Clin North Am. 1993;37(2):163-179.
22. Wolffe GN, vander Wejden FA, Spanauf AJ, de Quincey GN. Lengthening clinical crowns—a solution for specific periodontal, restorative and esthetic problems. Quintessence Int. 1994;25(2):81-88.
23. Townsend CL: Resective surgery: an esthetic application. Quintessence Int. 1993;24(8):535-542.
24. Silverstein LH, Shatz PC, Baker K: Subgingival technology to enhance the therapeutic outcome during surgical and restorative phases of smile reconstruction. Contemporary Esthetics and Restorative Practice. 2002;: 40-47.
25. Kois JC. Altering gingival level: the restorative connections. Part I: biological variables. J Esthet Dent. 1994;6(1): 3-9.
26. Morley J. Altering gingival level: The restorative connections part I: biologic variables. J Am Dent Assoc. 2001;132(1):39-45.
27. Silness J. Treated with dental bridges III. The relationship between the location of the crown margin and the periodontal condition. J Periodont Res. 1970;5(3): 225-229.
About the Author
Gregori M. Kurtzman, DDS
Private Practice
Silver Spring, Maryland
Lee H. Silverstein, DDS, MS
Associate Professor of Periodontics
Medical College of Georgia
Augusta, Georgia
Private Practice
Marietta, Georgia