A Transformation-Toughened Polycrystalline Ceramic Posterior Inlay/Onlay Fixed Partial Denture
Richard Trushkowsky
Esthetic fixed partial dentures (FPDs) containing no metal are desired by patients and clinicians. The fine-grained, solid-sintered engineering ceramics provide the best alternatives to FPDs with metal in the substructure.1,2 Metal is used for posterior FPDs because of its dependability and sturdiness. Full coverage when using ceramic material for abutments is usually recommended but inlays and onlays may also be used. Partial coverage reduces the amount of tooth structure that is removed. This is especially important in the young patient, as full coverage may result in a compromised pulp. Approximately 63% to 73% of the coronal tooth structure is removed when a tooth is prepared for an all-ceramic crown.3 Patients with active caries are contraindicated when partial coverage is used. Inlays/onlays can be fabricated of metal alloys and cemented with non-adhesive techniques. The dark shadows created by some of these restorations are objectionable to patients. In addition, caries and loss of retention may result in a remake of the restoration. The loss of retention suggests the need for retentive boxes and grooves but these devices result in the removal of additional tooth structure.
High-strength ceramics and fiber-reinforced composites have been introduced in the last several years as alternative materials.4,5 High-strength pressed ceramics are characterized by corrosion resistance and less plaque accumulation.2 They often present better esthetics, biocompatibility, high wear resistance, and low thermal conductivity.6 However, the longevity of the restoration is predicated upon a dependable bond between the porcelain, the luting agent, and tooth structure.7 All-ceramic materials are brittle and adequate bonding increases the fracture resistance of the tooth and the restoration and minimizes microleakage. Preparations usually have enamel margins and are conducive to adhesive cementation, which would reduce the possibility of dislodgement.
The more esthetic porcelains are mainly glassy, while higher-strength substructures are usually crystalline. Feldspathic porcelains are aluminosilicate glasses that are resistant to crystallization during firing. Feldspathic porcelain provides excellent optical properties that are extremely important in the esthetic zone. Feldspathic porcelain has reduced physical properties and requires reinforcement with a high-strength framework or adhesive cementation to the underlying tooth structure.8
The connector shape, size, veneering ceramic, aging behavior, and continuing performance need to be evaluated before routine use can be recommended.9 Filler particles that are usually crystalline can be added to glasses to improve their mechanical properties. Leucite was the first filler used because its high thermal expansion coefficient/contraction coefficient allowed it to be fired on metal substructures. Leucite also has an index of refraction close to that of feldspathic glasses and etches faster than glass, which allows selective etching and creation of a good micromechanical bond to resin cements (eg, IPS Empress®, Ivoclar Vivadent, Amherst, NY). Dispersion strengthening allows fillers to be added and dispersed throughout the glass. Crystalline filler particles also can be added to the glass. These particle-filled ceramics are called glass-ceramics. Dicor® (DENTSPLY Caulk, Milford, DE) and crystalline lithium disilicate as a core material (e.max® CAD, e.max Press, Ivoclar Vivadent) are examples.
Polycrystalline ceramics have no glassy components and the regularly aligned atoms are densely packed, making it more difficult to create a crack. However, despite the increased durability, polycrystalline ceramics are more difficult to shape into prostheses. The advent of CAD/CAM systems allowed 3-D data of a prepared tooth or a wax model of the framework to be used in creating an enlarged die (Procera®, Nobel Biocare, Yorba Linda, CA) or for machining blocks (Cercon®, DENTSPLY Ceramco, York, PA; Lava™ 3M-ESPE, St. Paul, MN). Polycrystalline ceramics are formed from powders that can be packed only to about 70% of their theoretical density and shrink about 30% by volume when they are fired. The amount of shrinkage has to be precisely predicted and allowed for. Powders that can be homogeneously packed are required to precisely predict the shrinkage.10
Prostheses can be fabricated by two methods. The first involves the creation of an oversized die and the pressing of aluminum oxide or zirconium oxide onto this die. The substructure shrinks during firing to become a well-fitting restoration (Procera). Partially fired zirconium oxide can be machined into greenware for firing as substructures (Cercon and Lava). D.C. Zircon (DCS Dental AG, Allschwil, Switzerland) is completely sintered. Individual blocks are bar-coded, providing the actual density of the block and allowing accurate shrinkage calculations. Milling machines change milling tools after a specified number of blocks have been milled to maintain accuracy.10
Zirconia provides the best mechanical properties compared to other ceramic materials used for FPDs. Glass-ceramic material (eg, Empress 1, Ivoclar Vivadent) has a bending strength of 182 MPa and 1.77 fracture toughness. Alumina has a bending strength of 547 MPa and fracture toughness of 3.55.11 Cercon has a biaxial flexural strength upwards to 1,320 MPa.8
Case Selections
When selecting cases appropriate for ceramic inlay/onlay restorations, it is important to remember that ceramic inlays can be used when only a modest amount of tooth structure has been destroyed. Ideally, an outer enamel margin should remain to provide a reliable seal. The margins of inlays/onlays should not occur in areas of occlusal contact. If this occurs, the restoration should be extended and an onlay preparation prepared. Bruxism and other parafunctional behaviors are contraindicated, and lack of good hygiene can lead to recurrent decay, necessitating a new restoration.12
Clinical Report
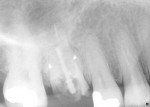
The patient, a 40-year-old man, had an upper right first molar that had endodontic treatment with a perforation in the palatal root that required extraction (Figure 1). He was given the option of implant placement, a porcelain-fused-to-metal FPD, or an inlay/onlay FPD. Previously, most of his extensive amalgam restorations had been replaced by ceramic or composite inlays or onlays. He was very happy with the esthetics and the function of these restorations. He also appreciated that these restorations required less reduction of tooth structure compared to full coverage with crowns. He elected to have an all-ceramic inlay/onlay FPD.
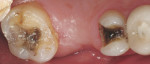
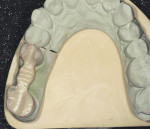
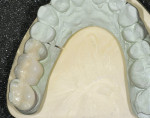
Full-mouth study models were obtained and mounted on a semi-adjustable articulator. The amalgam restorations were removed from teeth Nos. 2 and 4. The occlusal-lingual amalgam on tooth No. 2 was converted to an onlay preparation with a mesial box. The distal-occlusal amalgam in tooth No. 4 was modified to an inlay preparation with flared walls that were parallel to the box created on tooth No. 2 (Figure 2A and Figure 2B). A polyether impression (Impregum™ Penta™ Soft Quick Step and Impregum Garant™ Soft Light Body, 3M ESPE) was obtained. A bite registration was recorded with Jet Bite microSystem™ (Coltène/Whaledent, Cuyahoga Falls, OH). A shade was selected from the gingival and mid-buccal of tooth No. 2 using the VITA® 3D-Master® Shade Guide (Vident, Brea, CA). The case was then sent to the laboratory for fabrication.
The following guidelines should be kept in mind: The full-coverage abutment is prepared conventionally, with a minimum of 1-mm axial and 1.5-mm occlusal reduction, and smooth line angles. The full-coverage abutment may be conventionally cemented or adhesively bonded.
With an inlay abutment, care must be taken to ensure sufficient width of the prox-imal boxes (4 mm) and appropriate height (4 mm to 5 mm). The connector area should not be less than 9 mm2, and a preparation angle divergence of 2° to 3° is recommended. The preparation should have smooth, rounded line angles, and be free of retentive elements (no undercuts).
The angle between the facial and lingual aspects of the proximal box and the tooth’s external surface should be between 70° and 90°. Vestibular or lingual extensions, as well as beveling of cavosurface margins, are not recommended.
The Zirconia Process
Cercon zirconia offers several advantages over other all-ceramic alternatives. Because of the strength and reliability of the core material, zirconia, a coping wall thickness of 0.3 mm is sufficient in most cases. The margin area in the anterior may be finished down to 0.2 mm for esthetic purposes.13 In the area of connector sizes, Cercon offers an unparalleled esthetic advantage. Connector sizes of 9 mm2 to 11 mm2 are sufficient to create esthetic restorations with harmonious dimensions.
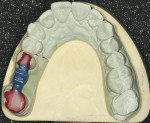
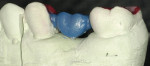
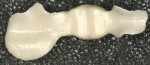
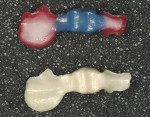
The laboratory duplicates the preparation and the technician designs a restoration in wax (Figure 3 and Figure 4). The wax model is placed in the Cercon Brain scanning and milling unit and scanned by a precision confocal laser (Figure 5). Non-contact scanning of the wax model and generation of the corresponding data record occurs and the pattern is then machined out of a Cercon Base blank of presintered zirconia in an enlarged size depending upon whether a single crown or four-unit FPD is being made (Figure 6). The enlargement factor compensates for the sintering shrinkage (~18% linear) and is contained in a bar code on each blank. There is a zirconium oxide blank in the appropriate size: 12 mm, 30 mm, 38 mm, or 47 mm. Each Cercon blank bears a printed-on bar code to automatically instruct the Cercon scanning and milling unit about the history of the blank being loaded, such as size and thickness. After the Cercon Brain reads the printed bar code, the cutting frame containing the Cercon base and the scanning frame containing the wax carving is inserted in the rotating and turning unit. The milled coping or framework is sintered in the furnace at 1,350°C for 6 hours. The zirconium oxide framework shrinks evenly in all three spatial directions in the Cercon heat furnace, ideally reaching the exact size in a linear fashion (Figure 7).14 After sintering, the dimensions of the Cercon framework match the dimensions of the wax pattern (Figure 8). Two shades of Cercon framework material, in neutral white and a natural, tooth-colored shade, are available for an esthetic range.13 The framework is evaluated on the model (Figure 9) and intraorally.
After sintering, any adjustments are carried out using a water-cooled turbine and diamond abrasive tool either in the laboratory or chairside. Conventional veneering with Cercon Ceram S, the ceramic specifically tailored to the zirconium-oxide framework material, is then accomplished. The finished FPD is evaluated on the model (Figure 10 ).
To lute the FPD into position, a material that will bond to the intaglio of the Cercon FPD and to the prepared teeth should be used (Figure 11). However, because the FPD is not silica-based, it cannot be acid-etched and treated with a silane-coupling agent. Sandblasting with aluminum oxide may result in increased surface energy but microcracks may form that will be detrimental to the longevity of the restoration.15
Some clinicians have felt that resin-luting agents may heal minor surface flaws and actually strengthen the restoration. Kumbuloglu et al demonstrated that air abrasion caused a transformation of the monoclinic phase of zirconia, and a layer of compressive stresses on the surface counteracts flaws resulting from air abrasion.16
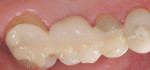
After luting with Panavia™ F 2.0 (Kuraray America Inc, New York, NY), the pontic was veneered with feldspathic porcelain for increased esthetics and blended well with the adjacent dentition (Figure 12). The rest of the FPD was more opaque because of the zirconia that was kept in bulk for increased strength (Figure 13).
Discussion
Many patients desire metal-free restorations mainly for esthetic reasons. They also prefer to minimize further reduction in tooth structure to replace teeth. In the author’s opinion, implants should always be considered as the first choice to replace missing teeth. However, expense, medical problems, smoking, or lack of necessary bone may preclude their use unless the patient is willing to undergo various surgical procedures to improve the bone topography.
Posterior areas of the mouth necessitate high-strength restorative materials for the replacement of missing teeth. Metal-based systems are usually recommended, but alternatives are fiber-reinforced composites and ceramics.17 The development of stronger ceramic core materials has resulted in the increased use of oxide ceramics for shorter all-ceramic FPDs.18 All-ceramic, resin-bonded FPDs were introduced years ago as a means of maintaining more tooth structure compared to a conventional FPD.19,20
With conventional ceramic materials, the distribution of flaws in a particular area, not the thickness of the material, is the main factor contributing to fractures. Yttria-tetragonal zirconia polycrystal (Y-TZP) does not possess a glass phase at the crystalline border. Tensile stress reduces matrix pressure on the tetragonal particles of Y-TZP and shear stress found in the particles results in martensitic transformation. The addition of 3% yttrium oxide as a stabilizing agent allows the sintering of fully tetragonal-phase ceramic to partially stabilized zirconia. When a crack starts to form, high-energy stress is created at the leading edge of the crack. The high energy created in this area causes the change of the tetragonal configuration to a monoclinic formation. Because the monoclinic configuration is 3% to 5% larger, the area where the crack is initiated is placed under compression, which hinders crack propagation. This prevents the opening of cracks and increases the energy required for crack propagation.
These factors are important in appropriate grinding mechanisms after sintering. Theoretically, the grinding of ceramics can act in a variety of directions. Grinding may result in residual compressive stress, which may increase the strength of the zirconia-toughened ceramic. However, flaws can be introduced that may impact the strength if they are greater than the depth of the grinding-induced surface layer. Grinding and sandblasting can introduce two primary strength-reducing flaw systems: deeper median cracks that occur parallel to the grinding direction and cracks that occur perpendicular to the tensile axis that are 60% deeper than those of parallel grinding. Curtis et al found that coarse grinding (120 mm to 150 mm) reduced biaxial flexural strength and may induce surface flaws that may cause surface degradation.21 That is the reason that the grinding of Y-TZP needs to be carefully monitored to achieve the greatest strength in CAD/CAM restorations.
FPDs possessing several units are subject to high tensile stresses at the gingival side of the connector during mastication. Tensile loads, unfortunately, may result in failure of a ceramic material but, in the author’s opinion, zirconia-based ceramics are the best material to endure the high tensile stresses on FPDs. Ceramics are also susceptible to subcritical crack growth as a result of water aiding in the breakage of metal oxide bonds at the crack tip while stress is being applied.22 The moisture of the mouth and cyclic loading that occurs during mastication lend themselves to the formation of subcritical crack propagation. This may reduce the effectiveness of the materials’ toughening mechanism and failure may result when no fracture is expected.23 In addition, abutment conditions, such as fixed or mobile, may affect the strength and stress distribution of all-ceramic FPDs.24 A ceramic laminate will always exhibit a constant strain system that results from the mismatch of elastic moduli at the interface between the core and the veneer. This occurs because of wettability factors and trapped air bubbles that often form over the core before firing.6 In addition to existing flaws, small alternating forces taking place all through mastication and the presence of water in a crack tip cause slow, time-dependent growth of cracks.6 The relationship between the inherent strength of all-ceramic restorations, residual and loading stresses, and existing structural flaws and their location is very complex. The fracture mechanisms of all-ceramic restorations include cone cracking, sub-surface quasi-plastic deformation, and radial cracking. The main mechanism of failure of all-ceramic crowns under occlusal load is cone cracking.25
Conclusion
A crown preparation always has the possibility of causing a loss of pulp vitality. If an implant is not a viable alternative, an inlay FPD should be considered. Wolfart et al found that zirconia frameworks presented adequate strength for replacing posterior teeth, with the veneering porcelain being the restrictive feature.26 Connector size should be between 3 mm x 3 mm and 4 mm x 4 mm. Although zirconia has come into wide use as a restorative material, its long-term clinical use may be affected by low-temperature aging, grain size, the amount of stabilizer, the presence of moisture, and chipping of the veneering porcelain.27,28
Acknowledgment
The author would like to thank Glen Adams CDT, MDT, of Americus Dental Laboratory for the excellent laboratory work and the slides of the laboratory fabrication.
References
1. White SN, Miklus VG, McLaren EA, et al. Flexural strength of layered zirconia and porcelain dental all-ceramic system. J Prosthet Dent. 2005;94(2):125-131.
2. Potiket N, Chiche G, Finger IM. In vitro fracture strength of teeth restored with different all-ceramic crown systems. J Prosthet Dent. 2004;92(5):491-495.
3. Edelhoff D, Sorensen JA. Tooth structure removal associated with various preparation designs for posterior teeth. J Prosthet Dent. 2002;22(3): 241-249.
4. Edelhoff D, Spiekermann H, Yildirim M. Metal-free inlay-retained fixed partial dentures. Quintessence Int. 2001;32(4):269-281.
5. Trushkowsky RD. Ceramic optimized polymer: the next generation of ceramic optimizes polymer - Part 1. Compend Contin Educ Dent. 1997;18(11):1101-1106.
6. Vult von Steyern P, Carlson P, Nilner K. All-ceramic fixed partial dentures according to the DC-Zirkon® technique. A two year clinical study. J Oral Rehabil. 2005;32(3):180-187.
7. Cekic I, Ergun G, Lassila LVJ, Vallittu PK. Ceramic-dentin bonding: effect of adhesive systems and light-curing units. J Adhes Dent. 2007;9(1):17-23.
8. Sailer I, Fehér A, Filser F, et al. Prospective clinical study of zirconia posterior fixed partial dentures: 3-year follow-up. Quintessence Int. 2006;37(9):685-693.
9. Att W, Stamouli K, Gerds T, Strub JR. Fracture resistance of different zirconium dioxide three-unit all-ceramic fixed partial dentures. Acta Odontol Scand. 2007;65(1):14-21.
10. Kelly JR. Dental ceramics: current thinking and trends. Dent Clin North Am. 2004;48(2):513-530.
11. Beuer F, Erdelt KJ, Schweiger J, et al. Flexural strength of coloured and aged zirconia. Quintessenz Zahntech. 2004;30: 942-954.
12. Ceramic Inlays and Onlays. In: Esthetic Dentistry and Ceramic Restorations. Touati B, Miara P, Nathanson D, eds. London, UK: Martin Dunitz; 1999: 259-291.
13. Sundar V, Kennedy CR, Ewoldsen NO. Cercon® Zirconia: Conservative Options in Metal-Free Dentistry. Dentsply Prosthetics, York, PA.
14. Raidgrodski AJ. All-ceramic full coverage restorations: Concepts and guidelines for material selection. Pract Proced Aesthet Dent. 2005;17(4): 249-256.
15. Zhang Y, Lawn BR, Malament K, et al. Damaging accumulation and fatigue life of particle-abraded ceramics. Int J Proshodont. 2006;19(5):442-448.
16. Kumbuloglu O, Lassila LV, User A, Vallittu PK. Bonding of resin composite to zirconium by two air particle methods. Oper Dent. 2006:31(2)248-255.
17. Rosentritt M, Behr M, Handel G. Fixed partial dentures: all-ceramics, fibre-reinforced composites and experimental systems. J Oral Rehabil. 2003;30(9):873-877.
18. Vult von Steyern P. All-ceramic fixed partial dentures. Studies on aluminum oxide and zirconium dioxide-based ceramic systems. Swed Dent J Suppl. 2005;173:1-69.
19. Kern M. Clinical long-term survival of two-retainer and single retainer all ceramic resin-bonded fixed partial dentures. Quintessence Int. 2005;36(2):141-147.
20. Sailer I, Fehér A, Filser F, et al. Five year clinical results of zirconia frameworks for posterior fixed partial dentures. Int J Prosthodont. 2007;20(4): 383-388.
21. Curtis AR, Wright AJ, Fleming GJP. The influence of surface modification techniques on the performance of Y-TZP dental ceramic. J Dent. 2006;34(5):317-325.
22. Studart AR, Filser F, Kocher P, Gauckler LJ. Fatigue of zirconia under cyclic loading in water and its implications for the design of dental bridges. Dent Mater. 2007;23(1):106-114.
23. Luthardt RG, Holzhter M, Sandkuhl O, et al. Reliability and properties of ground Y-TZP zirconia ceramics. J Dent Res. 2002;81(7):487-491.
24. Kou W, Kou S, Liu H, Sjögren G. Numerical modeling of the fracture process in a three-unit all-ceramic fixed partial denture. Dent Mater. 2007;23(8):1042-1049.
25. Aboushelib MN, de Jager N, Kleverlaan CJ, Feilzer AJ. Effect of loading method on the fracture mechanics of two layer all-ceramic restorative systems. Dent Mater. 2007;23(8):952-959.
26. Wolfart S, Ludwig K, Uphaus A, Kern M. Fracture strength of all-ceramic posterior inlay-retained fixed partial dentures. Dent Mater. 2007;23(12): 1513-1520.
27. Kelly JR. Stabilized zirconia as a structural ceramic: An overview. In: Proceedings of Conference on Adhesion, Ceramics and Bleaching—A Critical Evaluation. Brazil Academy of Dental Materials Transactions. 2006.
28. Aboushelib MN, de Jager N, Kleverlaan CJ, Feilzer AJ. Microtensile bond strength of different components of core veneered all-ceramic restorations. Dent Mater. 2005;21(10):984-991.
About the Author
Richard Trushkowsky, DDS
Associate Professor
New York University College of Dentistry
New York, New York
Private Practice
Staten Island, New York