Fiber-Reinforcing Materials for Dental Resins
Howard E. Strassler
The clinical success of adhesive composite-resin restorations has changed the way that dentists treatment plan and treat periodontally mobile teeth. While adhesive composite resin provides for strong, durable, and esthetic single-tooth restorations, when placed to join teeth together, these materials—which are chemically brittle by nature—are susceptible to fracture and are not durable. When supporting pontics or stabilizing mobile teeth, cracks within the connector areas lead to outright fracture; therefore, splinting teeth as part of fixed prosthodontic provisionalization also creates challenges when the temporary restoration must function over longer periods of time.
How can dentists minimize these clinical failures and still use conservative techniques for tooth stabilization with adhesive composites? How can they improve the durability of long-term provisional bridges, especially in cases of a missing tooth in an otherwise intact arch, where an implant is not desired or is contraindicated?
Over the past 15 years, a new class of materials designed for reinforcing dental resins has been introduced. These products are fiber-reinforcing ropes, braids, ribbons, and bundled fibers. Clinicians and researchers have investigated the embedding of these fiber-reinforcement materials into dental resins and found that they provided for an increase in certain physical properties and for more durable tooth stabilization.1,2
Before these fibers were introduced, tooth stabilization in the anterior region was accomplished using wires twisted around the teeth and covered with dental resins.3,4 In the posterior arch, stabilization was accomplished with channels prepared into the occlusal surfaces of the teeth, and then restorations which had either cast bars or thick wires placed in the channels were covered with resins.5 The placement of embedded wires, pins, nylon, and stainless-steel mesh into restorative resins improved the physical properties of the resins.6 A major problem with using these materials, however, was that they were never chemically joined to the dental resin, only embedded. Over time, composite-resin fractures and wear expose the fibers of the underlying reinforcing materials. The resin would then break away from the embedded metal or nylon because of a lack of chemical integration as well as the repeated loading stresses placed on the splint during normal and parafunction.4
In an attempt to minimize splint breakage, a greater bulk of composite resin was placed over the submerged wires and mesh, resulting in significant overcontouring of the restoration, higher rates of food and plaque retention, and increased difficulty in oral hygiene and periodontal maintenance of the splint. It was only with the introduction of chemically integrated, fiber-reinforced composite resins for tooth splinting and other clinical treatments that the problems associated with past attempts to reinforce composite resin were solved.
Components of Fiber-reinforced Composite Resins
In the early 1990s, several different types of fiber reinforcement materials were introduced. Kevlar, carbon, glass, ultra-high-molecular-weight polyethylene (UHMWPE), and silane-treated glass have been used to provide fiber reinforcement.2,7-12 The clinical successes with these materials have been varied.11-17
Many fiber types and architectures are available for clinical use to reinforce dental composites (Table 1). Currently, the most popular fiber types are UHMWPE and glass. All dental fiber-reinforcing materials provide similar levels of fiber reinforcement.18-20 Variations in dental composite reinforcement can be influenced by the type of veneering composite as well as the durability of the clinical performance of the fiber-reinforcement composite.11,19-26
UHMWPE is a linear homopolymer of ethylene with a density of 0.97 g/cm3 and a molecular weight in the range of 3 x 106 u to 6 x 106 u. The use of a UHMWPE leads to a very low friction coefficient, high wear resistance, and high impact strength.27 For the UHMWPE to be chemically integrated with dental resins, they are plasma treated.11,16 When used in dental fiber-reinforcing materials, UHMWPE is typically woven into a fabric ribbon (Ribbond® Reinforcing Ribbon, Ribbond, Seattle, WA; and Connect™, Kerr, Orange, CA) (Figure 1 A and Figure 1B A).
Glass fibers have a softening temperature of about 850° C, although the strength and modulus of elasticity of glass fibers decreases rapidly above 250° C.28 Glass fibers are used in different forms to strengthen dental composites, including woven short and loose fibers, woven long and loose fibers, and fiber bundles.28 Woven glass-ribbon fabric and unidirectionally oriented short fibers are typically used in dentistry.
To provide for chemical integration with dental resins, the glass is silanated using the same principles used to place glass filler particles into dental composites. Untreated (not silanated) glass fibers are weaker than treated glass fibers.9 Also, glass fiber-reinforcing materials are available as resin-impregnated (pre-preg), fiber-reinforcing materials (Splint-It®, Pentron, Wallingford, CT; everStick®, Stick Tech, Turku, Finland) or non-resin impregnated (GlasSpan®, GlasSpan, Inc, Exton, PA). For laboratory use, the glass fibers frequently are embedded into composite resins and prepolymerized as rods or beams (TESCERA™, BISCO, Schaumburg, IL; Vectris™,(Ivoclar Vivadent, Amherst, NY) (Figure 2A , Figure 2B , Figure 2C ). An example of a laboratory glass-fiber beam system is the TESCERA system, which is made from pre-tensed quartz fibers in a resin matrix as a "U" shaped beam further supported by a resin-glass fiber rod embedded in the TESCERA ATL dentin hybrid composite resin (Figure 3A and Figure 3B ).
Proving Grounds
Because of the nature of dental resins, the methods of testing these materials emphasize their brittle nature and their response to forces that would cause fracture.20,29 Testing methods and sample preparation can influence physical-property testing results. In many cases, the tests and interpretation of results are not suited to the class of fiber-reinforced composites because aspects of fiber orientation, the placement of fabric, and even scale effects are extremely important. Also, the placement of the fiber relative to the tooth being restored or—in the case of a fixed partial denture (FPD)—within the connector region may, in fact, reinforce the dental resin but because of its orientation and area of placement may not affect the surface characteristics of the resin. For example, a fiber beam placed on the tensile side of a composite bridge pontic is closer to the gingival ridge and will not inhibit the fracture of the composite on the occlusal surface of the abutment connectors.29-31 In the case of a unidirectional glass-fiber bundle, the fibers must be oriented in a longitudinal direction to impart their fiber-reinforcing capability. Glass fibers placed vertically within the composite will not inhibit resin fracture.20
The clinical use of the fiber also has an effect on how the fiber will perform. Using a fiber to reinforce a FPD is very different from using the same fiber to reinforce an endodontically treated tooth or to reinforce a cusp-replacement composite-resin restoration.
It is known that fibers used to reinforce composites and other resins respond differently as a result of their configuration (type of weave or fiber orientation) and their manipulation.30,32 Also, the cutting of the fiber and its ability to maintain its shape, dimensions, and architecture contribute to not only different degrees of physical enhancement but also to clinical success.20,32,33 When cut to length, a biaxial open-weave fabric ribbon will unravel, and when being placed its dimensions will change to be wider in some areas and narrower in others; the thickness of the fiber ribbon also changes with these other dimensional changes. In the case of a lock-stitched leno-weave, the fibers maintain their orientation and width and when cut, do not unravel. They also do not shift within the composite or resin that they are reinforcing. A consistent fabric configuration provides for more reliable resin reinforcement, greater ease of clinical management during direct placement of composites for splinting and tooth stabilization, and better composite resin crack-stopping capability.16,18,20
Also, a desirable aspect of any fiber-reinforcing material is its ability to adapt closely to the surface to which it is being bonded. In the case of UHMWPE fiber ribbons, they can be closely adapted to the tooth because of their inherent flexibility, lack of fiber configuration memory, and durability of fiber. In short, a UHMWPE fiber ribbon will stay where it is placed.
Glass fiber-reinforcing materials, especially those using unidirectional glass fibers, are more rigid and cannot easily adapt closely to the teeth.20 In trying to manipulate the fibers to be more closely adapted, glass fibers will have separation with some visible fractures of the brittle glass fibers.16,20 Also, when the fiber cannot be as closely adapted to the teeth, it leaves the composite material thicker on the tooth, providing for a decrease in durability of the reinforced composite in clinical function.16,34,35 Placing the fiber as close to the tooth as possible provides for better reinforcement and stabilization of the laminated structure.20,24
In clinical trials with fiber-reinforced composites, the survivability of the overlaying veneering composite resin is not much different than has been reported with the composite resin alone.36-38 Investigations of the degradation of the fiber-resin interface have described a variety of behaviors that contribute to failure. Bouillaguet et al investigated the hydrothermal and mechanical stresses that degrade the fiber-composite interface with glass fibers.39 They reported that glass fiber-reinforced composites had a degradation of their mechanical properties primarily as a result of the loss of interfacial bond strength between the glass and resin phases. They noted glass-fiber pullout when breaking specimens after water storage. They attributed these failures to degradation at the resin and glass interface combined with hydrolytic degradation of the glass. Also, when comparing unidirectional glass fibers to UHMWPE in flexural strength tests, the failure mode of the fiber-reinforced beam is different for both fiber types. Unidirectional glass fibers and unreinforced composite specimens had catastrophic fracture: the unidirectional glass fibers exhibited pullout and the glass fibers broke as well.20 In the case of the UHMWPE fiber-reinforced specimens, the composite cracks but the beam is intact—evidence of the role of fibers in reinforcing composites. Of interest, the UHMWPE braid and leno-weave-reinforced specimens did not fail through rupture; rather, there was a deflection and bending of the beam.20 This mode of bending is evidence of high levels of strain energy absorbed by the specimens and a greater toughness. Also, the lock-stitch weave of the UHMWPE is the tight weave that allows the ribbon to maintain a structural integrity by minimizing weave and fabric shifting within the composite. This imparts a multidirectional reinforcement to restorative polymeric resins that acts as a crack stopper.15,20,40
Clinical Uses of Fiber-reinforcing Materials
The clinical uses of fiber-reinforcing materials fall into three categories: direct-placement splints and FPDs, direct-placement single-restoration reinforcement, and indirect restorations.
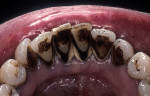
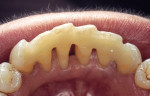
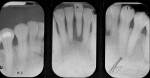
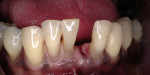
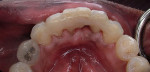
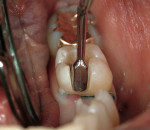
When fiber-reinforcing materials were introduced, the focus for their use was for periodontal splinting and stabilization resulting from tooth mobility.6,10,16,41-43 There is no doubt that splinting does reduce tooth mobility while the splint is in place.44 In the last decade, research supports the use of periodontal splinting as recommended therapy to stabilize those teeth to improve long-term prognosis.45-47 In a long-term clinical evaluation of splinting over a period of 48 to 96 months, using the original Ribbond Reinforcement Ribbon in fiber-reinforced composite resins was highly successful.17 The success of these splints can be attributed to close adaptation of the fiber ribbon to the tooth surface combined with cross stabilization of the mobile teeth by placing adhesive composite resin on the facial surfaces (Figure 4A, Figure 4B, Figure 4C, Figure 4D, Figure 4E).34,35 Splinting of traumatized teeth with fiber-reinforcing materials and adhesive composite resin has also been reported.48,49 When using fiber to stabilize the traumatized tooth or teeth or for tooth stabilization after re-implantation, the tooth must be allowed to have some movement and not be fixed in place.50,51
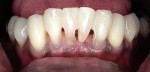
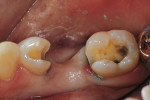
Fiber-reinforced composite resins also can be used to fabricate direct-placement FPDs. Both UHMWPE and glass fibers can be used for direct-placement fiber-reinforced restorations (Table 2). In cases of the replacement of a single anterior tooth resulting from trauma, severe periodontal disease, or for endodontic reasons, the patient often finds this event to be catastrophic and there is urgency for the tooth to be replaced in a single visit. For these clinical situations, direct-placement pontics fabricated from composite resin, a denture tooth, or using the patient’s natural tooth with fiber reinforcement has been reported (Figure 5A, Figure 5B, Figure 5C, Figure 5D, Figure 5E, Figure5F, Figure 5G).52,53 The same technique can be used as an interim fixed restoration during implant placement and restoration.54 In some cases, after orthodontic treatment of the patient with congenitally missing maxillary lateral incisors, a direct-placement, fiber-splint FPD can be used to restore the missing tooth and provide for fixed orthodontic retention. This is especially pertinent for the young patient (teenager) in whom a conventional FPD or an implant is not yet indicated or practical for the given clinical situation.55,56 In orthodontics, fiber-reinforced composite resins have also been described for use a directly placed space maintainer and for fixed orthodontic retention.57-60
Fiber-reinforcing materials are being used by dental laboratories in the fabrication of FPD resin-composite restorations, with single-crown restorations, dentures, and orthodontic and occlusal appliances.12,22,23,30,61-65 The primary use of fiber-reinforced composites by the dental laboratory is for the fabrication of fiber-reinforced FPDs to replace both anterior and posterior missing teeth.
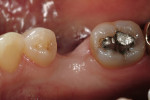
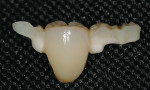
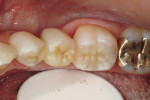
In vitro studies have demonstrated that the use of unidirectional glass-fiber reinforcement in the connector areas of FPDs contributes to significant composite reinforcement.29,36-38,66-68 Similar findings have been reported with a leno-weave UHMWPE and triaxial weave UHMWPE fiber.20,33,36 Fiber-reinforcing materials used by a dental laboratory are either resin pre-impregnated glass fibers, pre-polymerized composite resin surrounding glass fibers, biaxial braid UHMWPE, leno-weave UHMWPE, or a triaxial weave UHMWPE (Table 3). Typically, the preparation designs for the abutment teeth are inlay or onlay preparations (Figure 6A, Figure 6B, Figure 6C, Figure 6D). They are highly successful and can provide the patient with clinical service for more than 5 to 10 years.69 These restorations must be cemented using an adhesive resin technique with resin cements. Both etch-and-rinse adhesives with a self-cure or dual-cure composite resin cement or with a self-adhesive resin cement are indicated for cementing these restorations (Figure 7).36-38,70 Also, fiber-reinforcing materials are being used by dental laboratories in the fabrication of provisional restorations to reinforce and strengthen acrylic and composite-resin provisional materials.15,40,71
While the primary uses of fiber-reinforcing materials were for splinting and direct FPDs, in recent years some expanded uses of fiber-reinforcing materials have been reported in the dental literature. Esthetic fiber posts fabricated from fiber ribbons to restore endodontically treated teeth provide for root reinforcement and retention of composite resin cores.72,73 In an evaluation comparing the microleakage of different fiber-reinforcing materials in overflared root canals, the individually shaped polyethylene-reinforced dowel showed the least overall microleakage.74 This parallels two clinical studies of fiber-reinforced custom posts-and-cores reporting 95% success over 97 months and 98% success over 11 months.75,76 Other studies have evaluated the use of fiber reinforcement embedded within composite for direct restorations to provide for the cross-splinting of teeth with large composite restorations and demonstrated an improvement in fracture resistance of the teeth and restorations.76,77
Conclusion
Fiber-reinforcing materials need to be part of the armamentarium of a restorative dentist. When appropriately treatment planned, fiber-reinforced resin restorations can be highly successful. Patients with periodontally compromised dentitions and tooth mobility are excellent candidates for the use of fiber-reinforced direct-composite resins. In the case of the sudden loss of an anterior tooth or for the patient who is not a candidate for an implant, fiber-reinforced composite FPDs can be a viable alternative to a conventional FPD with crown preparations. Fiber-reinforcing materials can also be used to reinforce teeth that are endodontically treated or have significant missing tooth structure when a full crown is not affordable for a patient.
The majority of commercially available fiber-reinforcing materials are made from either UHMWPE fiber woven into either a biaxial braid or triaxial braided fabric ribbon or a lock-stitch leno-weave ribbon, or glass fibers that are either pre-impregnated with resin (as either a woven fabric or ribbon or as bundled unidirectional fibers) or non-resin impregnated (as a braided biaxial weave or rope that has been silane-treated for resin wetting). Whichever fiber-reinforcing material is chosen, it should be easy to use intraorally in whatever clinical condition is being treated. Clinical research supports using these materials as long-term provisional restorations; they should provide 5 to 10 years of service with some need for composite resin repair and resurfacing. Correct patient selection and proper treatment planning will ensure success with fiber-reinforcing materials.
Acknowledgments
Jonathan C. Meiers, DMD, MS, of the University of Connecticut School of Dental Medicine provided Figure 1A, Figure 1B, Figure 2A, Figure 2B, and Figure 2C. Figure 7 is reprinted with permission from: Strassler HE, Dzakovich JJ. High-strength fiber-reinforced fixed partial dentures with a wear-resistant composite resin. Compend Contin Educ Dent. 2005;26(10):716-724.
Disclosure
The author has received grant/research support from and is a current consultant for BISCO, Pentron Clinical, and Ribbond.
References
1. Miller TE, Barrick JA. Pediatric trauma and polyethylene reinforced composite fixed partial denture replacement: a new method. J Can Dent Assoc. 1993;59(3):252-256.
2. Goldberg AJ, Burstone CJ. The use of continuous fiber reinforcement. Dent Mater. 1992;8(3):197-202.
3. Strassler HE, Serio FG. Stabilization of the natural dentition in periodontal cases using adhesive restorative materials. Periodontal Insights. 1997;4(3): 4-10.
4. Pollack RP. Non-crown and bridge stabilization of severely mobile, periodontally involved teeth—a 25 year perspective. Dent Clin North Am. 1999;43(1):77-103.
5. Liatukas EL. An amalgam and composite resin splint for posterior teeth. J Prosthet Dent. 1973;30(2):173-175.
6. Miller TE. A new material for periodontal splinting and orthodontic retention. Compend Contin Educ Dent. 1993;14(6):800-806.
7. Powell DB, Nichols JI, Yuodelis RA, Strygler H. A comparison of wire- and Kevlar-reinforced provisional restorations. Int J Prosthodont. 1994;7(1): 81-89.
8. Malquarti G, Berruet RG, Bois D. Prosthetic use of carbon fiber-reinforced epoxy resin for esthetic crowns and fixed partial dentures. J Prosthet Dent. 1990;63(3):251-257.
9. Solnit GS. The effect of methyl methacrylate reinforcement with silane treated glass fibers. J Prosthet Dent. 1991; 66(3):310-314.
10. Miller TE, Hakimzadeh F, Rudo DN. Immediate and indirect woven polyethylene ribbon- reinforced periodontal-prosthetic splint: a case report. Quintessence Int. 1995;26(4):267-271.
11. Rudo DN, Karbhari VM. Physical behaviors of fiber reinforcement as applied to tooth stabilization. Dent Clin North Am. 1999;43(1): 7-35.
12. Kangasniemi I, Vallittu P, Meiers J, et al. Consensus statement of fiber-reinforced polymers: current status, future directions, and how they can be used to enhance dental care. Int J Prosthodont. 2003;16(2):209.
13. Freilich MA, Karmaker AC, Burstone CJ, Goldberg AJ. Development and clinical applications of a light-polymerized fiber-reinforced composite. J Prosthet Dent. 1998;80(3): 311-318.
14. Goldberg AJ, Freilich MA. An innovative pre-impregnated glass fiber for reinforcing composites. Dent Clin North Am. 1999; 43(1):127-133.
15. Samadzadeh A, Kugel G, Hurley E, Aboushala A. Fracture strengths of provisional restorations reinforced with plasma-treated woven polyethylene fiber. J Prosthet Dent. 1997;78(5):447-451.
16. Strassler HE, Haeri A, Gultz JP. New generation bonded reinforcing materials for anterior periodontal tooth stabilization and splinting. Dent Clin North Am. 1999;43(1): 105-126.
17. Strassler HE, Karbhari V, Rudo D. Effect of fiber reinforcement on flexural strength of composite. J Dent Res. 2001;80(Special Issue):221(abstract no. 854).
18. Christensen G. Reinforcement fibers for splinting teeth. CRA Newsletter. 1997;21(10):1-2.
19. Ellakwa AE, Shortall AC, Marquis PM. Influence of fiber type and wetting agent on the flexural properties of an indirect fiber reinforced composite. J Prosthet Dent. 2002;88(5): 485-490.
20. Karbhari VM, Strassler HE. Effect of fiber architecture on flexural characteristics and fracture of fiber reinforced composites. Dent Mater. 2007; 23(8): 960-968.
21. Ellakwa A, Shortall A, Shehata M, Marquis P. Influence of veneering composite composition of the efficacy of fiber reinforced restorations (FRR). Oper Dent. 2001; 26:467-75.
22. Gohring TN, Schmidlin PR, Lutz F. Two-year clinical and SEM evaluation of glass-fiber reinforced inlay fixed partial dentures. Am J Dent. 2002;15(1):35-40.
23. Freilich MA, Meiers JC, Duncan JP, Eckrote KA, et al. Clinical evaluation of fiber-reinforced bridges. J Am Dent Assoc. 2002;133(11): 1524-1534.
24. Karhbari VM, Rudo DN, Strassler HE. The development and clinical use of leno-woven UHMWPE ribbon in dentistry. Proceedings of the Society for Biomaterials (abstract issue). 2003;29: 15(abstract no. 529.)
25. Bohlsen F, Kern M. Clinical outcome of glass-fiber-reinforced crowns and fixed partial dentures: a three-year retrospective study. Quintessence Int. 2003;34(7): 493-496.
26. Monaco C, Farrari M, Miceli GP, Scotti R. Clinical evaluation of fiber-reinforced composite inlay FPDs. Int J Prosthodont. 2003;16(3): 219-225.
27. Rose RM, Crugnola A, Reis M, et al. On the origins of high in vivo wear rates in polyethylene components of total joint prostheses. Clin Orthop Relat Res. 1979;145:277-286.
28. Hull D. Fibers and matrices. In: Hull D, Clyne TW, eds. An Introduction to Composite Materials. 2nd edition. Cambridge, UK: Cambridge University Press; 1996;9-38.
29. Dyer SR, Sorensen JA, Lassila LV, Vallittu PK. Damage mechanics and load failure of fiber-reinforced composite fixed partial dentures. Dent Mater. 2005;21(12):1104-1110.
30. Potter KD. Deformation properties of uncured reinforcements—a reappraisal. Int J Mater Prod Technol. 2004;21(1): 4-23.
31. Nakamura T, Ohyama T, Waki T, Kinuta S. Finite element analysis of fiber-reinforced fixed partial dentures. Dent Mater. 2005; 24(2): 275-279.
32. Vallittu PK. Compositional and weave pattern analyses of glass fibers in dental polymer composites. J Prosthodont. 1998;7(3): 170-176.
33. Karbhari VM, Wang Q. Influence of triaxial braid denier on ribbon-based fiber reinforced dental composites. Dent Mater. 2006;23(8):969-976.
34. Strassler HE, Tomona N, Spitznagel JK Jr. Stablizing periodontally compromised teeth with fiber-reinforced composite resin. Dent Today. 2003;22(9):102-109.
35. Strassler HE, Brown C. Periodontal splinting with a thin, high-modulus polyethylene ribbon. Compend Contin Educ Dent. 2001;22(8):696-704.
36. Ayna E, Celenk S. Polyethylene fiber-reinforced composite inlay fixed partial dentures: two-year preliminary results. J Adhes Dent. 2005;7(4): 337-342.
37. Vallittu PK. Survival rates of resin-bonded, glass fiber-reinforced composite fixed partial dentures with a mean follow-up of 42 months: a pilot study. J Prosthet Dent. 2004;91(3):241-246.
38. Unlu N, Belli S. Three-year clinical evaluation of fiber-reinforced composite fixed partial dentures using prefabricated pontics. J Adhes Dent. 2006;8(3):183-188.
39. Bouillaguet S, Schutt A, Alander P, et al. Hydrothermal and mechanical stresses degrade fiber-matrix interfacial bond strength in dental-reinforced composites. J Biomed Mater Res B Appl Biomater. 2006;76(1):98-105.
40. Ramos V Jr, Runyan DA, Christensen LC. The effect of plasma-treated polyethylene fiber on the fracture strength of polymethyl methacrylate. J Prosthet Dent. 1996;76(1):94-96.
41. Scharf J. Presurgical prosthetic management of the periodontal patient- a modern adhesive approach. Alpha Omegan. 1994;87(4):17-25.
42. Strassler HE, Serio CL. Esthetic considerations when splinting with fiber-reinforced composites. Dent Clin North Am. 2007;51(2): 507-524.
43. Meiers JC. Chairside applications of FRC. In: Fiber Reinforced Composites in Clinical Dentistry. Freilich MA, Meiers JC, Duncan JP, Goldberg AJ, eds. Hanover Park, IL: Quintessence Publishing Co, Ltd; 2000;49-72.
44. Laudenbach KW, Stoller N, Laster L. The effects of periodontal surgery on horizontal tooth mobility. J Dent Res. 1977;56(Special Issue): abstract no. 596.
45. Wheeler TT, McArthur WP, Magnusson I, et al. Modeling the relationship between clinical, microbiologic, and immunologic parameters and alveolar bone levels in an elderly population. J Periodontol. 1994;65(1):68-78.
46. McGuire MK, Nunn ME. Prognosis versus actual outcome. II. The effectiveness of clinical parameters in developing an accurate diagnosis. J Periodontol. 1996;67(1):666-674.
47. Bernal G, Carvajal JC, Munoz-Viveros CA. A review of the clinical management of mobile teeth. J Contemp Dent Pract. 2002;3(4):10-22.
48. Yildirim Oz G, Ataoglu H, Kir N, Karaman AI. An alternative method for splinting of traumatized teeth: case reports. Dent Traumatol. 2006; 22(6):345-349.
49. Rudo DN. Treatment option for dentoalveolar trauma. Quintessence Int. 2000;31(9):610.
50. Trope M. Clinical management of the avulsed tooth. Dent Clin North Am. 1995;39(1):93-112.
51. McDonald N, Strassler HE. Evaluation for tooth stabilization and treatment of traumatized teeth. Dent Clin North Amer. 1999;43(1): 135-149.
52. Strassler HE, Serio CL. Single-visit natural tooth pontic fixed partial denture with fiber reinforcement ribbon. Compend Contin Educ Dent. 2004;25(3):224-230.
53. Strassler HE, Taler D, Sensi LG. Fiber reinforcement for one-visit single-tooth replacement. Dent Today. 2007;26(6): 120-125.
54. Meiers JC, Freilich MA. Use of a prefabricated fiber-reinforced composite resin framework to provide a provisional fixed partial denture over an integrating implant: a clinical report. J Prosthet Dent. 2006;95(1): 14-18.
55. Trushkowsky R. Fiber reinforced composite bridge and splint. Replacing congenitally missing teeth. NY State Dent J. 2004;70(5): 34-38.
56. Strassler HE. Bauman G. Current concepts in polishing composite resins. Pract Periodontics Aesthet Dent. 1993;5(3 Suppl 1):12-17.
57. Kargul B, Caglar E, Kabalay U. Glass fiber reinforced composite resin space maintainer: case reports. J Dent Child. 2003;70(3): 258-261.
58. Geserick M, Ball J, Wichelhaus A. Bonding fiber-reinforced lingual retainers with color-reactivating flowable composite. J Clin Orthod. 2004;38(10):560-562.
59. Iniguez I, Strassler HE. Polyethylene ribbon and fixed orthodontic retention and porcelain veneers: solving an esthetic dilemma. J Esthet Dent. 1998;10(2):52-59.
60. Karaman AI, Kir N, Belli S. Four applications of reinforced polyethylene fiber material in orthodontic practice. Am J Orthod Dentofacial Orthop. 2002;121(6):650-654.
61. Behr M, Rosentritt M, Handel G. Fiber reinforced composite crowns and FPDs: a clinical report. Int J Prosthod. 2003;16(3):239-243.
62. Cha YJ, Yang JH, Lee SH, Jan JS. Comparative study on the fracture strength of Empress 2 ceramic and Targis-Vectris crown. J Korean Acad Prosthodont. 2001;39:599-610.
63. Minami H, Suzuki S, Kurashige H, et al. Flexural strengths of denture base resin repaired with autopolymerizing resin and reinforcements after thermal stressing. J Prosthodont. 2005;14(1): 12-18.
64. Nakamura M, Takahashi H, Hayakawa I. Reinforcement of denture base resin with short-rod glass fiber. Dent Mater J. 2007; 26(5):733-738.
65. Mullarky RH. Aramid fiber reinforcement of acrylic appliances. J Clin Orthod. 1985;19(9):655-658.
66. Ahlstrand WM, Finger WJ. Direct and indirect fiber-reinforced fixed partial dentures: case reports. Quintessence Int. 2002;33(5): 359-365.
67. Magne P, Perakis N, Belser UC, Krejci I. Stress distribution of inlay-anchored adhesive fixed partial dentures: a finite element analysis of the influence of restorative materials and abutment preparation design. J Prosthet Dent. 2002;87(5):516-527.
68. Ootaki M, Shin-Ya A, Gomi H, et al. Optimum design for fixed partial dentures made of hybrid composite with glass fiber reinforcement by finite element analysis: effect of vertical reinforced thickness on fiber frame. Dent Mater J. 2007;26(2):280-289.
69. Strassler HE, Dzakovich JJ. High-strength fiber-reinforced fixed partial dentures with a wear-resistant composite resin. Compend Contin Educ Dent. 2005;26(10): 716-724.
70. Powers JM. Self-adhesive resin cements: characteristics, properties, and manipulation. Functional Esthetics and Restorative Dentistry. 2008;2(1):34-37.
71. Dixon DL, Fincher M, Breeding LC, Mueninghoff LA. Mechanical properties of a light polymerizing provisional restorative material with and without reinforcement fibers. J Prosthet Dent. 1995;73(6):510-514.
72. Hornbrook DS, Hastings JH. Use of bondable reinforcing fiber for post and core build-up in an endodontically treated tooth: maximizing strength and aesthetics. Pract Periodontics Aesthet Dent. 1995;7(5):33-42.
73. Newman MP, Yaman P, Dennison J, Rafter M, et al. Fracture resistance of endodontically treated teeth restored with composite posts. J Prosthet Dent. 2003;89(4): 360-367.
74. Erkut S, Gulsahi K, Imirzahoglu P, et al. Microleakage in overflared root canals restored with different fiber reinforced dowels. Oper Dent. 2008;33:92-101.
75. Piovesan EM, Demarco FF, Cenci MS, Pereira-Cenci T. Survival rates of endodontically treated teeth restored with fiber-reinforced custom posts and cores: a 97 month study. Int J Prosthodont. 2007;20(6):633-639.
76. Turker SB, Alkumru HN, Evren B. Prospective clinical trial of polyethylene fiber ribbon-reinforced, resin composite post-core build-up restorations. Int J Prosthodont. 2007;20(1): 55-56.
77. Belli S, Erdemir A, Ozcopur M, Eskitascioglu G. The effect of fibre insertion on fracture resistance of root filled molar teeth with MOD preparations restored with composite. Int Endod J. 2005;38(2):73-80.
About the Author
Howard E. Strassler, DMD
Professor and Director of Operative Dentistry
Department of Endodontics
Prosthodontics and Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland