Immediate Loading of Endosseous Dental Implants: A Review of the Evidence
Frederic J. Norkin; Jeffrey Ganeles; Julio Sekler; Samuel Zfaz
Immediate functional loading of dental implants is an attractive option to patients and dentists when contemplating implant dentistry, provided the outcomes are as successful as conventional loading protocols. Scientific and clinical data confirm the judicious use of these procedures and are supported and documented in dental and scientific literature.1-4
Most publications that discuss immediate and early loading or restoration of dental implants demonstrate success rates for these procedures similar to or better than conventional loading protocols. However, it should be recognized that this observation could be an unintentionally mis-leading statistical phenomenon of many authors. This literature has largely been written by exceptionally qualified, highly skilled practitioners working under tightly controlled clinical conditions on a relatively small number of implants or patients. Often their success rates exemplify the outcomes optimally achieved after considerable experience and may not reflect routine practice.
Successfully providing these kinds of services to patients in routine treatment requires strict adherence to rigid protocols and meticulous attention to countless details.5 It can be argued that these procedures are among the most demanding and meticulous types of dental implant services that can be provided, with the least margin for error. Surgical procedures must be precise. Occlusal control must be exact, and restorations should be highly refined in a compressed time frame. Each member of the therapeutic team must be fully aware, skilled, and coordinated in his or her specific role in the treatment.6
In 2004, the International Team of Implantology (ITI)7 defined loading categories based on the time of surgical implant placement to attachment of a prosthetic restoration and whether or not the prosthesis was in occlusion. The ITI definitions of the various categories are as follows.
• Conventional loading: a prosthesis attached to the implants in a second procedure for a minimum of 3 months healing after implant placement;
• Immediate restoration: a restoration inserted within 48 hours of implant placement, but not in direct occlusion with the opposing dentition;
• Immediate loading: a restoration placed in occlusion with the opposing dentition within 48 hours of implant placement;
• Early loading: placement of a restoration in occlusion with the opposing dentition at least 48 hours after implant placement, but no later than 3 months afterward; and
• Delayed loading: placement of a prosthesis on implants in a second procedure some time after the conventional healing period of 3 to 6 months.
In the short history of the evolution of implant loading protocols, it is clear that osseointegration can occur with all healing time periods under certain conditions. Clinical reports by many authors comparing conventional, early, and immediate protocols have not shown significant differences within the limits of their studies. Histologic observations8-13 clearly demonstrated that osseointegration could occur under loaded conditions.
Summarizing the knowledge obtained through research and clinical observations, it can be stated that for a dental implant to achieve osseointegration, three factors are important. They are:
• Placement of an implant composed of or coated with a suitable biocompatible material, such as titanium, tantalum, hydroxyapatite, zirconium oxide, or others;
• Site preparation without excessive thermal, traumatic, bacterial, or biological injury to the host bed; and
• Adequate stabilization of the implant to eliminate movement below the threshold of deleterious micromovement, estimated to be 50 µm to 150 µm.14
Furthermore, rough-surface dental implants are more desirable for immediate and early loading situations. In their comparison of success rate data with different implant surfaces, Del Fabbro et al15 noted statistically significant differences in both maxillary and mandibular arches when rough-surface implants were compared with smooth implants for immediate loading/restoration. They noted that success for the mandibular arches was approximately 93% for smooth-surface implants and 99% for rough-surface implants. Similar comparison for the maxillary arch was 91% vs 97%. Posterior sites were found to be particularly vulnerable to implant failure with smooth-surface implants, with 88% success for mandibular posterior sites and 80% for maxillary posterior sites. Significant discrepancies were not noted with threaded, rough-surface implants.
MANDIBULAR FULL-ARCH IMMEDIATE RESTORATION
Consider treatment options for the following healthy 64-year-old female patient who presented for treatment with a failing mandibular fixed partial denture (FPD) (Figure 1A through Figure 1C). The patient demonstrated recurrent caries, periodontal bone loss, recurrent endodontic pathology, and insufficient support for a new fixed prosthesis. While corrective procedures and techniques exist for each specific problem, the principles of evidence-based decision-making must be applied and tempered with critical judgment. For example, it is theoretically possible to perform regenerative periodontal procedures for the lower right molar, but consideration must be given to prognosis and relevance of treatment within the context of an appropriate treatment plan. Similarly, it is clearly possible to perform endodontic re-treatment for the lower left bicuspid, but again, this violates objectives of high predictability and good long-term prognosis. Dentists must look beyond the objective of “tooth repair” or “tooth retention” and instead consider what is best for the dentition and patient as a whole. If the sum of the efforts of conventional treatments will not yield enough adequate abutments with sufficiently positive prognoses (ie, critical dental mass), then implant dentistry must be considered.
Once the decision has been made to convert the patient to an implant-supported fixed restoration, other questions become apparent. How is she to be transitioned from her current condition to her new restoration? Will she need to wear a removable appliance during treatment? How much time is involved for the doctors and patient? How many provisional restorations are necessary? Options include:
• Retain key abutments and transition her provisional restoration from tooth support to implant support after the implants are allowed to heal over a conventional healing period.
• Extract all teeth and have the patient wear a full denture until the implants conventionally heal.
• Place transitional, temporary implants to support a provisional restoration while endosseous implants heal over a conventional interval.
• Combine procedures of extraction of teeth with placement of dental implants and immediate provisionalization in an immediately loaded fixed restoration.
CONSIDERATIONS TO DETERMINE BENEFIT/RISK FOR AN APPROPRIATE LOADING PROTOCOL
Whether contemplating immediate, early, or conventionally/delayed loading of implants, the factors to be considered include case type, anatomic characteristics, occlusal control, esthetic requirements, patient cooperation, clinician skill, and support team coordination. While each modality might have an appropriate indication, it is more efficient and desirable to consider the last option (ie, immediate loading), presuming predictability and anticipated results are similar. The contrast of treatment time for different protocols was shown by Chee and Jivraj,16 who documented a startling difference in the number of appointments between immediately loading implants with provisional restorations and conventional sequencing using full dentures. They found that with both techniques, success rates for implant integration were 100%. Yet, the group that received interim full dentures required a mean of 38 dental appointments for treatment, while the im-mediately loaded group required only one appointment.
Immediate loading of dental implants was initiated in the 1980s with mandibular overdentures by Babbush in 1986.17 The greatest amount of literature to support this treatment modality lies with mandibular full-arch fixed restorations. Initially, Schnitman et al,18 Salama et al,19 and Tarnow et al4 demonstrated treatment to fully edentulous mandibles where multiple implants were placed in dense bone, particularly in the symphyseal region. By nature, these implants supported or retained restorations replacing the complete arch of the dentition and, therefore, they were automatically considered to be loaded, as occlusal forces were transmitted directly to the implants from contact with the opposing dentition.
These fixed restorations were reinforced full-arch, one-piece provisional restorations. Caveats common to most publications include selection of dense bone for the implant sites, rigid splinting of the implants, careful occlusal management to minimize or avoid lateral force application, and maintenance of the provisionals in the mouth for the duration of healing and creating a physiologic occlusal scheme. Adhering to these principles, numerous authors documented hundreds of mandibular treatments and implants with success rates in the 96% to 100% range, generally equaling those expected of conventional or delayed loading protocols for edentulous mandibles.20-23
Occlusal schemes were created to conform to principles of “periodontal prosthesis” cases designed to minimize lateral movement of mobile abutment teeth using crossarch stabilization and rigid splinting. Additional principles from periodontal prostheses that were incorporated into these immediately loaded implant restorations include:
• shallow anterior overbite;
• reduced incisal guide angle;
• reduced posterior cusp height;
• reduced posterior occlusal table width; and
• anterior guidance to prevent nonfunctional or balancing occlusal contacts in lateral jaw movements.
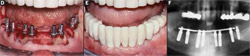
The aforementioned patient was treated with extraction of her mandibular teeth, along with simultaneous implant placement following standard surgical protocol (Figure 1D through Figure 1F). In this case, solid abutments (Straumann USA, LLC, Andover, MA) were hand-tightened on the day of surgery and impressed. The vertical dimension of occlusion was registered using an occlusal registration device. Protective caps were provisionally cemented, and appropriate models were sent to the laboratory for fabrication of a provisional restoration. The following morning, a laboratory-processed, metal-reinforced, cement-retained provisional restoration was delivered for the patient. Occlusion was adjusted to eliminate balancing contacts. The patient was re-evaluated according to standard follow-up procedures. Three months postsurgically, the restorative dentist removed the provisional restoration and fabricated a ceramometal restoration for the mandibular arch.
To facilitate delivery of these immediately loaded implant restorations, manufacturers created integrated surgical and prosthetic systems (eg, Novum™, Nobel Biocare, Yorba Linda, CA; All-on-Four, Nobel Biocare; and DIEM™, 3i,West Palm Beach, FL). Reported success rates for the first two systems were initially consistent with previously described standard prosthodontic approaches. Subsequently, De Bruyn et al24 reported loss of one of three implants in 15% of patients, leading to prosthetic failure, and recommended that a minimum of four implants be used for these types of cases.
It must be recognized that the opportunities for failure with immediate-function implant procedures are theoretically increased because of their potential complexity. Similarly, the consequences for failure are magnified as compared to conventional treatment protocols because of heightened patient expectations and the frequent lack of a secondary treatment plan.
MAXILLARY FULL-ARCH IMMEDIATE RESTORATION
Although far fewer in number of cases or implants, several authors reported immediate loading treatment of edentulous maxillas.25-27 Reading the review papers on loading, it can be seen that documentation for full maxillary arch immediate loading has been performed by far fewer authors in far fewer cases than mandibular immediate loading. Still, these authors indicate that, with proper protocols and patient selection, high predictability of restorations and cases can be achieved.
While strategies for maxillary immediate loading seem similar to the mandibular cases, it should be recognized that these cases present significant challenges and circumstances that are not encountered in the mandible. The greatest differences are seen in the quantity and quality of supporting bone available for implant stabilization. Edentulous maxillary arches generally have more trabecular bone posteriorly, with thinner cortical plates, often classified as poorer quality bone than is generally seen in the mandible. Maxillary sinuses typically limit implant length posteriorly, while horizontal resorption frequently restricts placement anteriorly, where good ridge height is more often available. Additionally, bone quality in the maxilla is generally poorer than in the mandible and is particularly diminished posteriorly, where masticatory forces are concentrated. These factors conspire to diminish implant stability and resistance to movement under loading, which is deleterious to successful osseointegration. To compensate for the inadequacies of maxillary bone, a number of authors suggest the following remedies:
• During implant site preparation, the osteotomy can be underprepared in diameter.
• Threaded, rough-surface implants should be placed to achieve the greatest degree of primary stability and maximize surface area.
• It is often necessary to place a greater number of implants in the maxilla than in the mandible for similar loading protocols.
• The use of longer, wider implants is recommended with all immediate loading protocols to achieve the greatest degree of primary stability.
• The use of osteotomes to compress bone at the osteotomy walls is recommended. Note: this is unsubstantiated in histologic reviews as to its ability to create “denser” bone; in fact, it is unknown if this is deleterious to healing.
• The use of three-dimensional imaging presurgically aids clinicians in identifying areas of greater cortication and trabeculation, thereby facilitating the selection of appropriately dense regions for implant placement. Using 3-dimensional planning, implants may require angulated positioning and compensatory abutments to maximize available bone.
SINGLE-TOOTH AND PARTIAL-ARCH IMMEDIATE PROVISIONALIZATION
Immediate loading or restoration of dental implants in single-tooth and partial-arch applications can be defined as attachment of a restoration in or out of direct occlusal function within 48 hours of surgical implant placement. Demographic evidence suggests that the opportunity to provide implant-supported tooth replacement for patients missing a single tooth significantly exceeds the needs for those who are fully edentulous.28
The biomechanical forces on implants for single-tooth situations are significantly different than for mandibular fully edentulous cases.29 For single teeth, occlusal forces can be controlled on implants by using the neighboring dentition to prevent direct functional loading during the osseointegration period. This is clearly not possible in full-arch, full-function applications.
A review of available evidence yields clinical data drawn from case series employing a variety of different techniques. Reported success rates for most publications on immediately restored single implants indicate that osseointegration can be achieved predictably.29 Not surprisingly, lower success rates were noted in studies in which machined-surface implants were used. When rough-surface implants were employed, most authors report greater than 96% success rates.2,30 Little or no difference was found between immediate restoration of single teeth located in anterior and posterior regions, although few publications specifically address posterior sites. Criteria for immediate placement and provisionalization in extraction sockets may be complex, requiring evaluation of local pathology, socket morphology, local anatomy, and esthetic demands.31-33
Further, excellent initial implant stability is critical to successful osseointegration. Measurement of initial implant stability can be determined in a number of ways (eg, insertion torque values and resonance frequency index). It should be noted that authors reporting success with posterior single-tooth immediate restoration cases require particularly high measurements for implant stability.34
For example, a 56-year-old healthy man presented missing the clinical crown of tooth No. 10 (Figure 2A through Figure 2E). After a comprehensive intraoral and radiographic evaluation, it was determined that surgical crown lengthening to increase available clinical crown length would further jeopardize the patient’s anterior esthetics. Thus, the treatment plan called for extraction of tooth No. 10 with simultaneous implant placement, abutment connection, and immediate provisionalization. The tooth was extracted atraumatically, without elevating a flap, under local anesthesia. The socket was curetted thoroughly, and the buccal plate walls were noted to be intact. An osteotomy was created toward the palatal wall of the socket and an implant (Straumann 4.1 mm x 12 mm RN SLA, Straumann USA) was inserted with a 35 Ncm insertion torque. A solid abutment (Straumannn) was hand-tightened, and an immediate provisional restoration was fabricated. The occlusion was adjusted to ensure that there were no centric or excursive contacts. All occlusal forces were directed on adjacent teeth.
After 2 months of healing, the patient returned to his restorative dentist, who torqued the abutment to 35 Ncm, per the manufacturer’s protocol, and took a final impression. A ceramometal cemented restoration was delivered in normal occlusion with the opposing teeth.
Note that in the final restoration of this case, a small amount of gingival recession can be appreciated. This is a common finding in almost all cases involving immediate placement in extraction sockets, particularly where the patient has a thin biotype. The gingival form and height also were preserved in this single-tooth case.
When considering treatment options in the esthetic zone, patients and clinicians should be aware of the likelihood of at least a minor amount of gingival recession after tooth extraction and implant placement. This will occur whether or not a provisional restoration is also placed. Optimized implant design, precise surgery, and gingival and bone augmentation procedures may reduce this tendency, but they have not yet been shown to be predictable. In cases where a minor amount of gingival recession can be tolerated, immediate restoration of implants can result in more optimal gingival contours.
Immediate rehabilitation of short-span edentulous segments presents similar biomechanical challenges to single-tooth conditions. Generally, the clinicians’ therapeutic strategy is to direct occlusal forces to adjacent teeth, leaving the immediately restored implant sections out of occlusal contact. As the restorations grow to include larger edentulous spaces, the ability to eliminate occlusal function diminishes. Additionally, the opportunity for non-occlusal loading by oral musculature and food bolus increases with larger spans. Partial-arch applications often present a more demanding biomechanical environment than either single-tooth or full-arch applications because of less efficient splinting possibilities and higher bending moments.35 However, the limited clinical evidence currently available to support this treatment modality indicates high success rates.34,36,37
Caution should be emphasized when considering immediate rehabilitation in the esthetic zone. The same concerns about gingival recession on the facial of immediate implants may be magnified when multiple implants are considered in the esthet-ic zone. This concern becomes most acute in patients with a high smile, thin biotype, and high esthetic demands. Unlike the single-tooth cases in which adjacent teeth tend to support the proximal papillas, multiple-tooth implant cases carry the additional difficulty and potential complication of significantly blunted papillas.
CONCLUSION
Evidence-based evaluation of numerous peer-reviewed studies confirms the predictability of immediate functional loading of dental implants in all clinical applications. To achieve a high level of success, it is imperative that clinicians adhere to rigid surgical, restorative, and laboratory protocols.
Recurring key elements to success include meticulous attention to maximizing primary implant stability. Strategies to accomplish this include selecting longer, wider, rough-surface, threaded implants and surgically placing them in denser alveolar sites. Particularly in full-arch maxillary immediate function cases, implant angulation coupled with angled abutments provides better use of available alveolar bone. Restorations must be designed to protect the early healing implant interface and minimize the possibility for implant movement. In fully loaded conditions, rigid splinting with cross-arch stabilization and minimization of horizontal forces is suggested. In partial-arch or single-tooth segments, all intentional occlusal contact is eliminated to prevent direct loading.
While immediate loading and restoration of implants may provide significant benefits to patients, the techniques may also potentially compromise results. Immediate restoration eliminates the need for removable appliances, enhances treatment efficiency, and enhances patient satisfaction. However, these techniques may also increase risk for implant loss, reduce the opportunities for bone and gingival augmentation, and compromise esthetics, particularly in cases of high risk or patient expectations. Because these procedures are considered more difficult, clinician experience and skill are also important factors in the decision-making process. As with all procedures, careful evaluation, consideration, and discussion should be accomplished before beginning treatment.
DISCLOSURE
Jeffrey Ganeles, DMD, is a speaker for Straumann USA, LLC, and receives honoraria from the International Team of Implantology.
REFERENCES
1. Chiapasco M, Gatti C, Rossi E, et al. Implant-retained mandibular overdentures with immediate loading. A retrospective multicenter study on 226 consecutive cases. Clin Oral Implants Res. 1997;8:48-57.
2. Degidi M, Piattelli A. Immediate functional and non-functional loading of dental implants: a 2- to 60-month follow-up study of 646 titanium implants. J Periodontol. 2003;74:225-241.
3. Ganeles J, Rosenberg MM, Holt RL et al. Immediate loading of implants with fixed restorations in the completely edentulous mandible: report of 27 patients from a private practice. Int J Oral Maxillofac Implants. 2001;16:418-426.
4. Tarnow DP, Emtiaz S, Classi A. Immediate loading of threaded implants at stage 1 surgery in edentulous arches: ten consecutive case reports with 1- to 5-year data. Int J Oral Maxillofac Implants. 1997;12:319-324.
5. Morton D, Jaffin R, Weber HP. Immediate restoration and loading of dental implants: clinical considerations and protocols. Int J Oral Maxillofac Implants. 2004;19(Suppl):103-108.
6. Landro L. Health-care industry supports use of ‘practice guidelines.’ The Wall Street Journal. May 11, 2001.
7. Cochran DL, Morton D, Weber HP. Consensus statements and recommended clinical procedures regarding loading protocols for endosseous dental implants. Int J Oral Maxillofac Implants. 2004;19(Suppl):109-113.
8. Sagara M, Akagawa Y, Nikai H, et al. The effects of early occlusal loading on one-stage titanium alloy implants in beagle dogs: a pilot study. J Prosthet Dent. 1993;69:281-288.
9. Piattelli A, Paolantonio M, Corigliano M, et al. Immediate loading of titanium plasma-sprayed screw-shaped implants in man: a clinical and histological report of two cases. J Periodontol. 1997;68:591-597.
10. Ledermann PD, Schenk RK, Buser D. Long-lasting osseointegration of immediately loaded, bar-connected TPS screws after 12 years of function: a histologic case report of a 95-year-old patient. Int J Periodontics Restorative Dent. 1998; 18:552-563.
11. Meyer U, Joos U, Mythili J, et al. Ultrastructural characterization of the implant/bone interface of immediately loaded dental implants. Biomaterials. 2004;25:1959-1967.
12. Testori T, Szmukler-Moncler S, Francetti L, et al. Immediate loading of Osseotite implants: a case report and histologic analysis after 4 months of occlusal loading. Int J Periodontics Restorative Dent. 2001;21:451-459.
13. Romanos GE, Testori T, Degidi M, et al. Histologic and histomorphometric findings from retrieved, immediately occlusally loaded implants in humans. J Periodontol. 2005;76:1823-1832.
14. Szmukler-Moncler S, Piattelli A, Favero GA, et al. Considerations preliminary to the application of early and immediate loading protocols in dental implantology. Clin Oral Implants Res. 2000;11:12-25.
15. Del Fabbro M, Testori T, Francetti L, et al. Systematic review of survival rates for immediately loaded dental implants. Int J Periodontics Restorative Dent. 2006;26:249-263.
16. Chee W, Jivraj S. Efficiency of immediately loaded mandibular full-arch implant restorations. Clin Implant Dent Relat Res. 2003;5: 52-56.
17. Babbush CA, Kent JN, Misiek DJ. Titanium plasma-sprayed (TPS) screw implants for the reconstruction of the edentulous mandible. J Oral Maxillofac Surg. 1986;44:274-282.
18. Schnitman PA, Wohrle PS, Rubenstein JE. Immediate fixed interim prostheses supported by two-stage threaded implants: methodology and results. J Oral Implantol. 1990;16:96-105.
19. Salama H, Rose LF, Salama M, et al. Immediate loading of bilaterally splinted titanium root-form implants in fixed prosthodontics— a technique reexamined: two case reports. Int J Periodontics Restorative Dent. 1995;15: 344-361.
20. Testori T, Del Fabbro M, Szmukler-Moncler S, et al. Immediate occlusal loading of Osseotite implants in the completely edentulous mandible. Int J Oral Maxillofac Implants. 2003;18:544-551.
21. Wolfinger GJ, Balshi TJ, Rangert B. Immediate functional loading of Branemark system implants in edentulous mandibles: clinical report of the results of developmental and simplified protocols. Int J Oral Maxillofac Implants. 2003;18:250-257.
22. Horiuchi K, Uchida H, Yamamoto K, et al. Immediate loading of Branemark system implants following placement in edentulous patients: a clinical report. Int J Oral Maxillofac Implants. 2000;15: 824-830.
23. Cooper LF, Rahman A, Moriarty J, et al. Immediate mandibular rehabilitation with endosseous implants: simultaneous extraction, implant placement, and loading. Int J Oral Maxillofac Implants. 2002;17:517-525.
24. De Bruyn H, Kisch J, Collaert B, et al. Fixed mandibular restorations on three early-loaded regular platform Branemark implants. Clin Implant Dent Relat Res. 2001;3: 176-184.
25. Levine R, Rose L, Salama H. Immediate loading of root-form implants: two case reports 3 years after loading. Int J Periodontics Restorative Dent. 1998;18:333-343.
26. Jaffin RA, Kumar A, Berman CL. Immediate loading of dental implants in the completely edentulous maxilla: a clinical report. Int J Oral Maxillofac Implants. 2004;19:721-730.
27. Ibanez JC, Tahhan MJ, Zamar JA, et al. Immediate occlusal loading of double acid-etched surface titanium implants in 41 consecutive full-arch cases in the mandible and maxilla: 6- to 74-month results. J Periodontol. 2005;76:1972-1981.
28. Oral Health in America: A Report of the Surgeon General. U.S. Department of Health and Human Services/National Institute of Dental and Craniofacial Research. 2000. NIH publication 00-4713.
29. Ganeles J, Wismeijer D. Early and immediately restored and loaded dental implants for single-tooth and partial-arch applications. Int J Oral Maxillofac Implants. 2004;19(Suppl):92-102.
30. Lorenzoni M, Pertl C, Zhang K, et al. Immediate loading of single-tooth implants in the anterior maxilla. Preliminary results after one year. Clin Oral Implants Res. 2003;14:180-187.
31. Lazzara RJ. Immediate implant placement into extraction sites: surgical and restorative advantages. Int J Periodontics Restorative Dent. 1989;9:332-343.
32. Novaes AB Jr, Vidigal GM Jr, Novaes AB, et al. Immediate implants placed into infected sites: a histomorphometric study in dogs. Int J Oral Maxillofac Implants. 1998;13:422-427.
33. Novaes AB Jr, Novaes AB. Immediate implants placed into infected sites: a clinical report. Int J Oral Maxillofac Implants. 1995;10:609-613.
34. Glauser R, Lundgren AK, Gottlow J, et al. Immediate occlusal loading of Branemark TiUnite implants placed predominantly in soft bone: 1-year results of a prospective clinical study. Clin Implant Dent Relat Res. 2003;5(Suppl 1):47-56.
35. Brunski JB, Puleo DA, Nanci A. Biomaterials and biomechanics of oral and maxillofacial implants: current status and future developments. Int J Oral Maxillofac Implants. 2000;15:15-46.
36. Rocci A, Martignoni M, Gottlow J. Immediate loading of Branemark System TiUnite and machined-surface implants in the posterior mandible: a randomized open-ended clinical trial. Clin Implant Dent Relat Res. 2003;5(Suppl 1):57-63.
37. Nikellis I, Levi A, Nicolopoulos C. Immediate loading of 190 endosseous dental implants: a prospective observational study of 40 patient treatments with up to 2-year data. Int J Oral Maxillofac Implants. 2004;19:116-123.
This article was originally published in Functional Esthetics and Restorative Dentistry. 2007;1(2):38-44.
 | |
| Figure 1A through Figure 1C A healthy 64-year-old patient presented for treatment with a failing mandibular FPD . She demonstrated recurrent caries, periodontal bone loss, recurrent endodontic pathology, and insufficient support for a new fixed prosthesis. | Figure 1D through Figure 1F The patient’s mandibular teeth were extracted, followed by immediate implant placement. Solid abutments were handtightened. The vertical dimension of occlusion was registered and protective caps were provisionally cemented. Models were sent to the laboratory for provisional restoration fabrication. |
| Figure 2A through Figure 2E Ahealthy patient presented missing the crown of tooth No.10.Treatment involved the extraction of tooth No.10 with simultaneous implant placement,abutment connection,and immediate provisionalization.Under local anesthesia,the tooth was extracted atraumatically,without elevating a flap.An osteotomy was created toward the palatal wall of the socket and an implant was insert-ed with a 35 Ncm insertion torque.A solid abutment was hand-tightened,and an immediate provisional restoration was fabricated.The occlusion was adjusted to ensure there were no centric or excursive contacts.All occlusal forces were directed on adjacent teeth.Two months posthealing,the patient returned to the restorative dentist,who torqued the abutment and took the final impression.A ceramometal cementedrestoration was delivered in normal occlusion with the opposing teeth.Note that in the final restoration,a small amount of gingival recession can be appreciated; gingival form and height were also preserved. |
| About the Author |
Frederic J. Norkin, DMD Private Practice Limited to Periodontics and Dental Implants Jeffrey Ganeles, DMD Clinical Assistant Professor Private Practice Julio Sekler, DMD, MMSc Samuel Zfaz, DMD Private Practice |




