Replacing Unesthetic Anterior Class IV Restorations According to Minimal Intervention and Visual Ergonomic Principles
Frank J. Milnar, DDS, AAACD
Dental treatments today are guided by principles of minimal intervention and biomodification. According to these principles, the goal is to limit the restoration/re-restoration cycle, conserve as much healthy tooth structure as possible, and remove as little tooth structure as possible. Also, the materials that are used for restorations are placed and/or manipulated in such a way that they reproduce the color, shape, and texture of the missing natural tooth structure. This article describes how old and unesthetic composite restorations for Class IV fractures in the maxillary central incisors of a 17-year-old beauty pageant contestant were replaced according to the principles of minimal intervention and visual ergonomics. The manner in which these restorations were placed is presented in detail.
Minimal Intervention
Increased emphasis is being placed on the importance of conserving sound tooth structure during restorative procedures. Whether for the replacement of worn or discolored restorations, or for the correction of unesthetic form or malalignment, treatments are now guided by principles of minimal intervention and biomodification.1-3 Specifically, today’s forward-thinking clinicians are being called to embrace minimally invasive techniques when providing patients with necessary and/or elective dental treatments.
It is therefore incumbent upon clinicians to consider treatment alternatives critically, so that the outcomes of these efforts can be as esthetic, durable, and predictable as possible. Fortunately, today’s clinicians are practicing in an era when biomodification and biomimetics are driving product developments, and the consequence is that treatments can be applied in less technique-sensitive manners to answer clinical challenges in “naturally” esthetic and functional ways.4
The rationale behind a minimal intervention approach is ultimately to curtail the restoration/re-restoration cycle and conserve as much healthy tooth structure as possible to benefit a patient over his or her lifetime.5 Minimal intervention suggests that restorative procedures be undertaken as a last resort, and with the removal of the least amount of tooth structure necessary.6 It should be clearly understood that restorations will not prevent or eliminate disease, only correct the defect or arrest the disease process.6
Treatments that are particularly well suited to minimal intervention techniques and that can take advantage of the biomimetic direct composite materials now available include restoration of Class IV fractures. Although a variety of treatment options exists with which to restore the Class IV fracture—including indirect restorations (eg, crowns or veneers) or directly placed composite materials—what must be selected is the most appropriate treatment alternative that will ultimately contribute to as little future intervention as possible, as previously noted.7 Today’s biomimetic direct composite materials demonstrate improved physical properties, durability, and strength for long-term function, as well as polychromatic qualities for the creation of restorations that essentially “reproduce” natural tooth structure.8
However, producing a minimally invasive Class IV restoration that best maximizes the biomimetic properties of a material requires that it be placed according to visual ergonomics. This encompasses all tasks and properties contributing to the morphological and optical characteristics of the restorations so that they will mimic natural teeth. Paying attention to these details enables the durable and predictable reproduction of the tooth, not just the creation of a restoration.9 Additionally, it facilitates the selection of a material capable of providing a surface texture that mimics that of natural enamel and its high polishability. Visual ergonomics also determines the manner in which biomimetic materials will be placed to reproduce the color, shape, and texture of the missing natural tooth structure.9
Gradia™ Direct (GC America, Alsip, IL) is among the biomimetic and naturally shaded composites available today (eg, 4 Seasons®, Ivoclar Vivadent, Amherst, NY; TPH®3, DENTSPLY Caulk, Milford, DE) that mimic the optical characteristics seen in natural teeth. It is a microfilled hybrid composite that, according to the manufacturer, resembles natural tooth structure in its composition (eg, a microfilled matrix of resin composite and compounds of silica, prepolymerized fillers, and a urethane dimethacrylate commoner matrix). Available in a range of shades matched to the VITA® Classical Shade Guide (Vident, Brea, CA), Gradia Direct increases the clinician’s ability to recreate natural light dynamics and esthetics in the restorations produced.
For example, when different layers of composite are selected and appropriately placed, different interplays occur between the material’s reflective properties—essentially acting as a reproduction of what happens among the layers of natural tooth structure. So, for direct restorations, the use of Gradia Direct in a visually ergonomic way produces restorations with the internal reflectivity and optical properties that replicate those of natural teeth.
Therefore, the argument can easily be made that now is the time when both minimally invasive and visually ergonomic principles can be applied simultaneously to the treatment of anterior Class IV fractures. These restorations can be placed in such a way that they will impact only the affected tooth structure and preserve the patient’s right to pursue conservative and/or alternative treatment options in the future.
Case Presentation
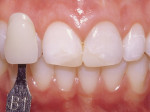
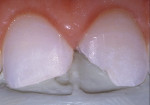
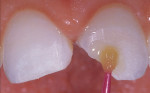
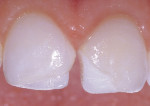
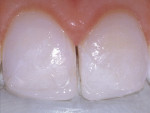
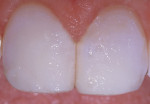
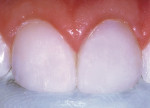
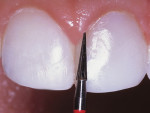
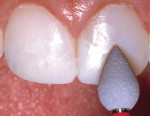
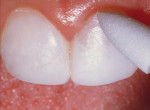
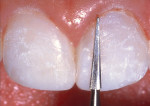
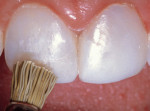
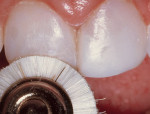
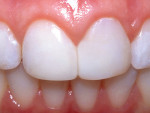
A 17-year-old girl—a contestant entered into the Dream Girl USA contest—presented with discolored Class IV composite restorations on teeth Nos. 8 and 9 (Figure 1; Figure 2; Figure 3). These restorations had been placed approximately 5 years earlier. Neither the patient, nor her mother, was interested in irreversible, indirect treatment options, and instead they wanted to revisit conservative restorative alternatives (eg, direct composite restorations). A complete intraoral examination was performed and an oral history was taken that included radiographs and photographs. The patient was in good health; no pathologies were found to contraindicate direct composite restoration of the maxillary central incisors.
Treatment Planning
A visual assessment was performed, and the patient’s occlusion was analyzed. Additionally, the morphologic, histologic, and optical characteristics of the adjacent teeth were noted.
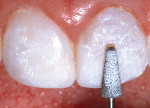
To determine the appropriate composite shades, a shade guide based on the Vitapan Classic shades (Vident)was used. It was determined that the ideal dentin composite shade would be B1 (Figure 4). The shade identified visually was verified using a digital spectrophotometer (Easyshade®, Vident) (Figure 5).
Diagnostic Wax-up
Before removing the old composite restorations and preparing the teeth, an impression was taken to create a high-viscosity putty stent (Exafast™ Putty, GC America).8 The putty stent, once placed in the patient’s mouth, would be used for spatial reference and as a volumetric guide for placing the composite. It would also help to preserve the facial/lingual line angle.10
Preparation Protocol
The old restorations were removed, and teeth Nos. 8 and 9 were prepared with diamond burs to create a 0.5-mm modified lingual shoulder, in addition to a 2-mm facial bevel. An infinite/virtual bevel was also placed that would facilitate transitioning of the enamel shade of composite into the remaining tooth structure.11 This long bevel was approximately 0.3 mm in depth, extending 2 mm to 3 mm around the margins of the teeth. These preparations would support the fracture resistance and durability of the restorations, enabling the placement of a layer of composite at the restorative margins (Figure 6).11
Composite Layering Technique
After preparation, the teeth were pumiced, rinsed, and dried. Then, a single-component, self-etching bonding agent (GC G-Bond™, GC America) was brushed onto the preparations for 10 seconds (Figure 7) and air-thinned with high pressure. The bonding agent was light-cured for 10 seconds per tooth with an LED curing light (UltraLume™ LED 5, Ultradent Products, Inc, South Jordan, UT). This light was used throughout the restorative process.
After the putty stent was positioned in the patient’s mouth, build-up of the restorations began with the placement of a 1.5-mm-thick layer of the selected A20 Opaque shaded composite on teeth Nos. 8 and 9 to form the lingual enamel layer (Figure 8). This shade was selected to control opacity and eliminate show-through. The composite was carefully sculpted into place and light-cured for 20 seconds. Note that using the stent and carefully controlling the application of the composite helped to ensure accurate and precise placement, which later simplified the finishing and polishing steps.12
The putty stent was removed to preview the lingual enamel layer and assess opacity. It was returned to the patient’s mouth for the placement of the bulk of the artificial dentin layer. Shade B1 composite was placed in a 2-mm-thick increment on each tooth to form the body and mammelons of the restorations on teeth Nos. 8 and 9. Before being light-cured for 20 seconds, this layer was sculpted onto the long bevel to mask the fracture line, but left just shy of the proximal and incisal edges, leaving sufficient room for the application of the final enamel layer. To create natural-looking variations in shade and chroma, an Extra Bright White (XBW) shade composite was placed along the incisal third of the teeth (Figure 9), sculpted into place, and light-cured for 20 seconds after the putty stent was removed.
A thick final enamel layer of BW (Bleaching White) composite was placed on the central incisors with the putty stent removed (Figure 10), then sculpted and light-cured for 20 seconds. Before the creation of surface texture and tertiary characterizations, the enamel layer and overall appearance of the restorations was critiqued with the putty stent in place (Figure 11). To ensure a complete depth of cure, trans-enamel light-curing was performed from multiple aspects.
Finishing and Polishing
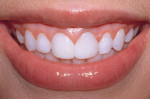
When contouring and/or gross reduction of composite resin restorations is performed during the finishing stages, this author has found it beneficial to use a variety of burs and diamonds (Figure 12).12 To create the final form of the incisal edges and finish the embrasure between teeth Nos. 8 and 9, a proprietary composite finishing system (New Horizon Composite Finishing System, Frank J. Milnar, DDS; #K0097, Brasseler USA, Savannah, GA) was used. The surface of the restorations was refined (Figure 13 and Figure 14), and micromorphology was also created (Figure 15 and Figure 16).12 To achieve a life-like final luster, polishing points and brushes were used (Groovy, Clinician’s Choice, New Milford, CT) (Figure 17 and Figure 18). Upon completion, the final restorations blended seamlessly with the patient’s natural smile (Figure 19 ; Figure 20 ; Figure 21).
Conclusion
Undertaking minimally invasive composite layering techniques requires a heightened sense of observation so that the nat-ural tooth structure can be meticulously reproduced through the placement of biomimetic materials. Of course, the clinician’s primary responsibility is to do no further harm while executing the treatment; those restoratives that enable conservative protocol should be considered first. Also, when contemplating the manner in which to use these technical skills and selected composite materials, adhering to visual ergonomic principles may be beneficial to the reproduction of a restoration that truly imitates the form and function of natural teeth.
Disclosure
Dr. Milnar has received financial and material/product support from GC America, Inc.
Acknowledgment
The author would like to acknowledge Dr. Dean Lodding, his American Academy of Cosmetic Dentistry Accreditation Advisor, who encouraged the author to improve his clinical skills and remain focused on “the zone of excellence,” which is the gold standard in the accreditation process. Without his mentoring, accreditation for this author would not have been attainable.
References
1. Donly KJ, Brown DJ. Identify, protect, restore: emerging issues in approaching children’s oral health. Gen Dent. 2005;53(2):106-110.
2. Terry DA. A biomodification of tooth discoloration. Pract Proced Aesthet Dent. 2006;18(4):226,228-229.
3. Allen KL, McAndrew M. Integrating dental anatomy and biomaterials: an innovative use of composite resin. Gen Dent. 2004;52(2):132-133.
4. Tay FR, Pashley DH. Dental adhesives of the future. J Adhes Dent. 2002;4(2):91-103.
5. White JM, Eakle WS. Rationale and treatment approach in minimally invasive dentistry. J Am Dent Assoc. 2000;131(suppl): 13S-19S.
6. Mount GJ, Ngo H. Minimal intervention: a new concept for operative dentistry. Quintessence Int. 2000;31(8):527-533.
7. Peters MC, McLean ME. Minimally invasive operative care. I. Minimal intervention and concepts for minimally invasive cavity preparations. J Adhes Dent. 2001;3(1):7-16.
8. Terry DA, Geller W, Tric O, Anderson MJ, Tourville M, Kabashigawa A. Anatomical form defines color: function, form, and aesthetics. Pract Proced Aesthet Dent. 2002;14:59-67.
9. Terry DA, Leinfelder KF. An integration of composite resin with natural tooth structure: the Class IV restoration. Pract Proced Aesthet Dent. 2004;16(3): 235-242.
10. Behle C. Placement of direct composite veneers utilizing a silicone buildup guide and intraoral mock-up. Pract Periodontics Aesthet Dent. 2000;12(3): 259-266.
11. Bichacho N. Direct composite resin restoration of the single anterior tooth: clinical implications and practical applications. Compend Contin Educ Dent. 1996;17(8): 796-802.
12. Peyton JH. Finishing and polishing techniques: direct composite resin restorations. Pract Proced Aesthet Dent. 2004;16(4): 293-298.
About the Authors
Frank J. Milnar, DDS, AAACD
Private Practice
Family, Cosmetic and Restorative Dentistry
Saint Paul,Minnesota