Using Biophysical Principles to Reduce Restorative Failures
Raymond J. Voller, DMD
Many challenges presented to clinicians during the course of their daily practice encompass biologic and physiologic principles cleverly disguised as dental procedures and techniques. Common sense prevails in the application of these principles and when the best course of treatment is carefully and methodically planned out and completed, the long-term benefits make the work involved worth the time.
Most seasoned dentists have witnessed their fair share of successes and failures of restorative and esthetic dentistry. The failures seem to occur mostly because of variance from a strict protocol that adheres to these sound biologic and physiologic principles, and of course, because of negligence on the part of the patient. Occasionally, however, the restorative dentistry or carious event does not cause an immediate failure; over time, attachment loss occurs chronically and can subsequently cause the eventual loss of the natural abutments.1
Dental treatment that is designed to be more simplified and supragingival is more desirable. When the envelope of function is taken into consideration and the correct placement of occlusal forces is distributed over as wide a surface area as possible, most preferably down the long axis of the remaining natural or artificial dentition, long-term success is imminent.2 If a proposed tooth is biocompromised and it takes more than a few minutes to decide if salvagability is viable or not, then in the author’s opinion, the tooth most likely is not a good candidate to retain.
With the advent of implant dentistry we have an extremely predictable alternative to natural dentition, particularly if the remaining osseous architecture lends itself to an ideal positioning. However, as with the natural dentition, a poorly designed prosthesis attached to a well-integrated implant can have deleterious effects on the long-term retention of the implant.3
Many of the patients seen by the author are partially edentulous, and many already possess an upper denture. As one studies the treatment plan, the question that should arise is, what was the original etiology of their current condition? These issues should be expounded on with the initial interview and a comprehensive examination so as to prevent a relapse. Additionally, the author has noted that many patients also have difficulty wearing a lower prosthesis. Several reasons for this exist; poor residual ridges, poorly contoured abutment candidates, the presence of the tongue, and impingement of the prosthesis into the purported freeway space are among the most common issues.
In the author’s experience, poorly constructed, uncomfortable removable prostheses tend to cloud patients’ judgment and sway them from reinvesting in something that may fail. One element that the author has found to increase the success of removable prostheses is the custom attachment.
There are several strategies to replace the conventional clasping of abutment teeth for removable partial dentures using attachments on full-coverage restorations.4 An application of simple physics should help determine which attachment most efficiently helps direct the vectors of forces in the most efficable manner possible. The closer the forces can be directed down the long axis, with the minimization of torque and/or lateral forces, the better chance of the success of the restoration.
The patient also must be able to maintain the attachments with regard to oral hygiene, and the prosthesis must fit in that "gray area" of having just enough retention to resist dislodgement, yet not so much that the patient cannot effortlessly remove the prosthesis as needed.
In addition, esthetically pleasing alternatives to fixed prosthetics are driving the market toward more camouflaged types of attachments.5 Patients seen by the cosmetically oriented dentist already have in their minds that their restorations must mimic the natural contours and shades of their existing dentition and must blend into the natural abutments that are to be restored. This is most easily accomplished by the use of attachments that are actually covered and held fast to the abutment teeth. With attachments, not only can the restorative dentist improve esthetics, but also the functionality of the entire treatment.6
Attachments such as the Bredent attachment (XPDent Corp, Miami, FL), serve the patient extremely well as a treatment modality option with removable partial dentures for several reasons.7 Primarily, they are designed very close to the abutment tooth center, allowing the direction of the force vectors straight down along the long axis of the tooth. With a properly designed rest seat, it simulates the traditional RPI (rest, proximal plate, I-bar) clasp. The distal proximal plate allows for some frictional retention, but the ball-and-socket snap fit of the attachment itself is what offers the primary retention for the prosthesis.
Because of the "trailer ball" type of design, there is less accuracy required to actually seat the prosthesis. Many of the patients the author sees do not always have the manual dexterity required to repeatedly and accurately seat a prosthesis, so the "give" of the Bredent attachment lends itself extremely well to allowing the patient to reproducibly seat the denture without "perfect positioning," as is required by several of the other types of attachments.
The ball is placed 0.5 mm above the residual ridge to maximize interocclusal space and keep loading forces as low as possible. The additional benefit of improved oral hygiene that this offers also helps prevent decay at the margins in the attachment areas.
CASE PRESENTATION
This case presented to the author’s office with several problems, including severe wear, decay, and some localized periodontal issues (Figure 1; Figure 2; Figure 3; Figure 4). After reviewing the patient’s medical and dental history, and ensuring that the patient was able to undergo dental treatment, it was decided to retain five of the best distal mandibular teeth. Cosmetic imaging was performed to help educate the patient on the desirable changes. Preliminary study models were taken, along with a panoramic radiograph (Figure 5).
After debridement, scaling, and root planing, the periodontal condition was re-evaluated and stabilized. Tooth No. 9 was acutely abscessed and was extracted. A maxillary and mandibular temporary acrylic overlay was constructed over the existing natural dentition to test a new vertical dimension and the patient was instructed to wear these for 2 months (Figure 6).
After the patient was comfortable with the proposed vertical dimension, bite registrations were obtained for the construction of a temporary immediate maxillary full denture and a temporary partial mandibular clasp-retained denture. All of the upper teeth and lower incisors were extracted and the temporary prostheses were seated and adjusted accordingly (Figure 7 and Figure 8).
After several weeks of healing, the patient was prepared for full-coverage crowns on teeth Nos. 21, 22, 27, 28, and 29 (Figure 9). Temporary crowns were constructed from a previously fabricated wax-up at the new vertical dimension afforded by the temporary prostheses (Figure 10).
The impressions and opposing model of the temporary upper denture were sent to the laboratory for construction of splinted crowns for teeth numbers 21, 22, 27, 28, and 29, and the Bredent attachment was prescribed for the distals of each corresponding set of splinted crowns. These were subsequently tried in, and once marginal integrity was confirmed, they were pulled in an impression and sent to the laboratory for construction of the lower partial denture. It is highly recommended that the splinted crowns and attachments be sent to the laboratory in an impression such as this so that the partial denture can be constructed directly on the crowns and Bredent attachments.
After construction, the lower partial denture was returned and the splinted crowns and attachments with the lower partial were all tried in to confirm proper fit and retention. Once all the parameters were satisfactory, the crowns were bonded to the teeth (Figure 11 and Figure 12). A bite-check was obtained and the lower partial was fit to an upper base plate for the construction of a final upper complete denture.
The lower partial was then pulled in an impression to construct a new lower model without the attachments and crowns. After tooth selection, this was sent to the laboratory for the final try-in of the proposed wax-up. After approval of the set-up by the patient and confirmation of a reproducible occlusion, the patient was reappointed and the completed trial maxillary and lower partial dentures were subsequently inserted. Approximately 2 mm of space was left under the prostheses for the use of Hydrocast (Kay-See Dental Co, Kansas City, MO) as a final, functionally generated impression to accurately register the soft tissues and obtain maximum adaptation to the supporting residual ridges. Generally, tissue stops are used to help obtain a reproducible vertical dimension.
After a few days, and after the patient approved the fit and function of both trial prostheses, a final bite-check was obtained. The lower partial denture was pulled in an impression and both the maxillary and mandibular dentures were poured in die stone for the final models. These were sent to the laboratory for the construction of the final upper complete denture, and the finishing of the lower partial denture (Figure 13; Figure 14; Figure 15; Figure 16).
CONCLUSION
The esthetics and functional demands placed on dentists by the discerning patient can easily be satisfied by the proper selection of materials, the correct application of the procedures necessary to place and construct these materials, and strict adherence to biophysical principles. The attachments illustrated in this case report clearly fit into the armamentarium of the restorative, cosmetically oriented dentist and should be used to help prevent the deleterious effects of improperly directed force vectors so often found in failing restorations.
The Bredent attachment is, in the author’s opinion, one of the most underused and unheralded breakthroughs in dentistry to help prevent tooth and subsequent attachment and bone loss. As with almost all successful long-term dentistry, properly designed, esthetically pleasing, and functional restorations are possible with minimal effort and careful preoperative planning to provide patients with the best dentistry has to offer.
References
1. Broadbent JM, Williams KB, Thomson WM, Williams SM. Dental restorations: a risk factor for periodontal attachment loss? J Clin Periodontol. 2006;33(11): 803-810.2. Dawson PE. Evaluation, Diagnosis, and Treatment of Occlusal Problems. 2nd Ed; St. Louis, Mo: CV Mosby Co; 1989: 470-471.
3. Porter JA, von Fraunhofer JA. Success or failure of dental implants? A literature review with treatment considerations. Gen Dent. 2005;53(6): 423-432.
4. Bambara GE. Attachment dentistry. A rationale for reflection and treatment planning. N Y State Dent J. 2003;69(1):28-30.
5. Donovan TE, Derbabian K, Kaneko L, Wright R. Esthetic considerations in removable prosthodontics. J Esthet Restor Dent. 2001;13(4):241-253.
6. Ku YC, Shen YF, Chan CP. Extracoronal resilient attachments in distal-extension removable partial dentures. Quintessence Int. 2000;31(5): 311-317.
7. Donovan TE, Cho GC. Esthetic considerations with removable partial dentures. J Calif Dent Assoc. 2003;31(7):551-557.
 | 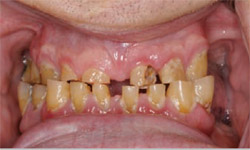 | |
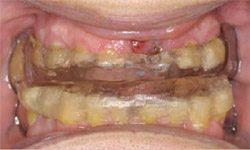
| Figure 2 Close-up retracted preoperative photograph illustrating severely worn, decayed dentition and lack of posterior support. | ||
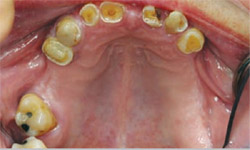 | ||
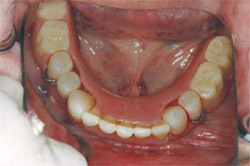
| Figure 3 Preoperative retracted view of maxillary teeth. | ||
| Figure 1 Preoperative, full-face photograph illustrating lack of vertical support and averted smile. | ||
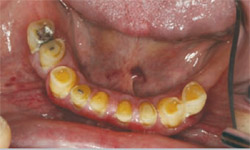 | 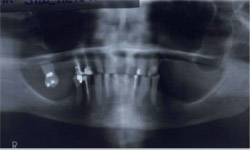 | |
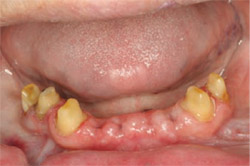
| Figure 4 Preoperative retracted view of mandibular teeth. | Figure 5 Preoperative panoramic radiograph. | |
 | 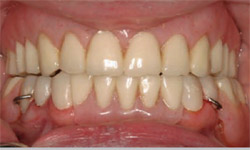 | |
| Figure 6 Retracted view of maxillary and mandibular acrylic overlays in occlusion at proposed vertical dimension. | Figure 7 Retracted view of temporary immediate maxillary full denture and mandibular partial denture attached to provisional splinted crowns. | |
 |  | |
| Figure 8 Retracted occlusal view of the temporary immediate mandibular partial denture retained by temporary crowns. | Figure 9 Retracted view of mandibular preparations for full-coverage splinted crowns. | |
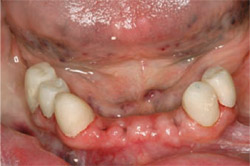 | 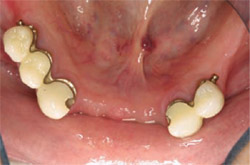 | |
| Figure 10 Retracted view of mandibular provisional splinted crowns. | Figure 11 Retracted occlusal view of final splinted crowns restorations illustrating Bredent attachments on the distals of the abutments. | |
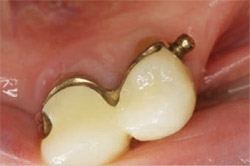 | 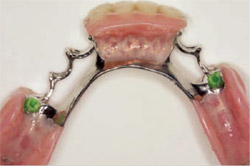 | |
| Figure 12 Close-up occlusal view of mandibular left splinted crowns and Bredent attachment. | Figure 13 Tissue-side view of completed mandibular partial denture prosthesis illustrating female portion of the Bredent attachments. | |
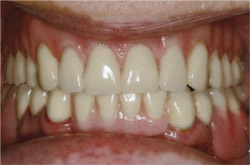 | 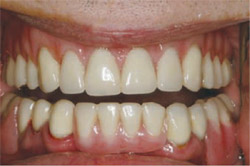 | |
| Figure 14 Retracted anterior postoperative view of final restoration in maximum intercuspation. | Figure 15 Retracted anterior postoperative view of final restoration slightly open. | |
 | ||
| Figure 16 Final full-face portrait of postoperative results. | ||
| About the Author | ||
 Raymond J. Voller, DMD Raymond J. Voller, DMDPrivate Practice Kittanning, Pennsylvania | ||



