Using Diagnostic Wax-Ups and Provisional Restorations When Re-Establishing Canine Function
Frank J. Milnar, DDS, AAACD
Important to the success of indirect restorative treatments is the clinician’s ability to realize both the patient’s expectations and the clinical requirements that will ensure long-term function. However, accomplishing this objective, while at the same time carrying out the minimal intervention and conservative techniques that are increasingly demanded by patients today, can be challenging.
For this reason, one of the most important factors in restorative success is pretreatment case planning.1 This involves fabrication of a wax-up and use of provisional restorations.1 These tools can help the clinician identify and understand any potential problems with the case before the final restorations are made and helps to ensure a higher likelihood of clinical success.1
In this regard, provisionalization has become critical to the esthetic restorative treatment process.2,3 This is particularly true in terms of evaluating and sharing information about how proposed restoration designs will function, affect occlusion and phonetics, and meet a patient’s esthetic desires.2,4 A patient can determine his or her comfort level with the proposed new smile and/or restorations while wearing temporary restorations (eg, evaluate speech and function as well as the relationship of their upper and lower arches).4
However, in addition to protecting the prepared tooth structure during the period between tooth preparation and placement of the final restorations,4 provisional restorations must preserve occlusal function.5 Therefore, the provisional restorations must maintain and/or re-establish the appropriate protrusive and lateral guidance.5 This means that they should be sufficiently strong so that they resist the forces of occlusion. Furthermore, the provisional restorations should be cemented with a luting agent that will resist the forces of removal.5
CASE PRESENTATION
A 41-year-old woman presented for a consultation because she was dissatisfied with the appearance of her smile (Figure 1). She wanted an esthetic restorative treatment that would look natural, and she was particularly interested in conservative procedures.
A thorough examination was performed that included radiographs, photographs, and periodontal probings. Additionally, the patient was carefully evaluated in terms of her occlusion and the morphologic, histologic, and optical characteristics of her teeth.
Teeth Nos. 8 and 9 had been restored previously with composite restorations. Overall, her maxillary anterior teeth demonstrated obvious incisal wear. The examination revealed the cause of this wear to be a loss of canine function. Therefore, the treatment plan would need to re-establish the appropriate occlusal relationship for the patient to help ensure the long-term success of any restorations that would be placed.6
Treatment Planning
Preoperative impressions were taken to fabricate study models, as well as for use by the laboratory in making an enhanced wax-up. This wax-up would demonstrate for the patient the manner in which the proposed restorations would improve her smile in a conservative manner, as well as re-establish proper occlusion.
A custom shade of the patient’s teeth was taken using conventional shade mapping and a spectrophotometer (Vita Easyshade®, Vident, Brea, CA). These recorded shades facilitated communication between the dentist and the laboratory ceramist for the purpose of creating the wax-up. Ultimately, any proposed and accepted restorations would then be able to reflect the patient’s desired tooth shade in terms of value (ie, brightness), chroma (ie, color intensity), and hue (ie, basic color based on wavelength of visible light).7
At a subsequent appointment, the patient approved the esthetic, anatomically enhanced wax-up (Master Diagnostic Model™, Valley Dental Arts, Stillwater, MN) that demonstrated the manner in which the appearance of her maxillary teeth and her overall smile could be improved. It specifically showed the proposed placement of all-ceramic veneers on teeth Nos. 6 and 11 and a combination of full-coverage crowns and/or modified veneers on teeth Nos. 7 through 10 (Figure 2). Because the patient was interested in natural-looking restorations (ie, fluorescent, opale-scent, multidimensional), the treatment plan called for the use of a pressed ceramic material (Authentic® Pressable Ceramics, Jensen Dental Solutions, North Haven, CT) that would enable the restorations’ colors to be built up internally.
The patient accepted the treatment plan, and a polyvinyl siloxane impression of the wax-up was then made for use in fabricating provisional restorations.
Tooth Preparation
The patient was anesthetized, and a series of burs (Brasseler USA, Savannah, GA) was used to prepare the teeth for the all-ceramic crown restorations. When all-ceramic restorations are planned, the teeth will typically be prepared with a 90° full shoulder with a rounded gingival-axial line angle or deep chamfer, as well as axial surface reduction of 1 mm to 1.5 mm, to ensure predictable function and strength. Additionally, the occlusal aspect or incisal edge should be reduced by 1.5 mm to 2 mm; specific margin designs are dependent upon the specific restorative material being used.8
The preparations were thoroughly cleaned of any residue, and retraction cord was placed into the gingival sulcus for hemostasis. The retraction cord was removed, and a polyvinyl siloxane impression was taken of the final preparations. The bite was also recorded using a fast-setting, addition-silicone bite registration material (Registrado X-tra, VOCO America, Inc, Sunnyside, NY) (Figure 3). Additionally, a stumpf shade was taken and found to be ST8, which was ideal for the proposed pressed ceramic restorations because it would enable the use of an optimized dentin shade.
Provisionalization
To create the direct provisional restorations, shade B1 of the temporary material (StructurPremium, VOCO America, Inc) was injected into a matrix that was made from the wax-up (Figure 4). As previously noted, provisional restorations must be sufficiently strong to resist occlusal forces. According to the manufacturer, the selected material demonstrates high fracture resistance, as well as compressive and tensile strengths.
Once loaded with temporary material, the matrix was loaded into the patient’s mouth and the material was allowed to set for 1.5 minutes. The matrix was then removed, after which the provisionals were removed from the matrix. All margins were sanded and polished interproximally, which was easily accomplished as a result of the provisional material’s characteristics. Although the provisional material demonstrates a natural fluorescence and brilliant gloss, the temporaries were glazed using a denture sealant (Palaseal, Heraeus Kulzer, Armonk, NY) (Figure 5) that was then cured according to the manufacturer’s instructions.
A non-eugenol temporary luting cement was selected for this case (Provicol WM, VOCO America, Inc) and loaded into the provisionals using a direct-dosing syringe (Figure 6). This cement was selected because the author has found it to provide excellent adhesion to temporaries, but also because it demonstrates a desensitizing effect as a result of the calcium hydroxide it contains.9,10 The provisionals were then seated onto the prepared teeth, and excess cement was released from the margins (Figure 7).
Excess cement was removed from the margins and from the surface of the provisionals. Occlusion and phonetics were verified, and the patient was dismissed (Figure 8 and 9).
Restoration Fabrication
The laboratory was provided with the final impressions and bite registration, enhanced wax-up, and preoperative photographs and shade maps. Using these materials, the laboratory ceramist pressed the appropriate low-fusing, leucite-reinforced ceramic ingots so that the restorations for teeth Nos. 6 through 11 could be built up using a layering and custom staining technique.
Final Cementation
At the final cementation appointment, the provisional restorations were removed, and the preparations were cleaned with an antimicrobial scrub (Consepsis Scrub, Ultradent Products, Inc, South Jordan, UT). A hemostatic gel (ViscoStat Clear, Ultradent Products, Inc) was placed along the gingival margins to prevent hemorrhage, and suitable isolation was achieved.
The all-ceramic crowns were tried in to verify the interproximal and centric contacts, as well as marginal adaptation, and then removed. The tooth preparations were etched for 15 seconds, rinsed, and dried. The internal aspects of the crowns were etched for 1 minute, rinsed, and dried, after which they were silanated for 1 minute and lightly air-dried. An adhesive primer was applied to the preparations and cured according to the manufacturer’s instructions.
Then, the selected dual-cure resin cement was loaded into the restorations and they were seated. After the release of excess resin cement, a glycerin gel (De-Ox®, Ultradent Products, Inc) was placed along the gingival margins to prevent the formation of an oxygen-inhibiting layer.
Once the restorations were definitively cured into place, excess cement was cleaned from around the margins and the patient was given the opportunity to evaluate her new smile. The final esthetic restorative outcome—which was based on the wax-up and the provisional restorations—completely satisfied her expectations (Figure 10).
CONCLUSION
To meet the demands of patients today, manufacturers have introduced new developments in provisional materials and cements.3 This has perhaps occurred as a result of the profession’s recognition of the integral role that provisional restorations play in the development and management of the design of final restorations.3
In that regard, this case has demonstrated the manner in which provisional restorations can function as more than just an intermediate covering of tooth preparations.11 Rather, the well-planned provisional restoration enables clinicians to assist patients in becoming accustomed to what is ideal for them occlusally, phonetically, and esthetically.11 In this case, the patient was able to adjust to alterations in her canine function while wearing the provisional restorations.
ACKNOWLEDGMENT
The pressed ceramic restorations (Authentic®) featured in this case were fabricated by Denise Quitter, CDT, of Valley Dental Arts, Stillwater, MN.
DISCLOSURE
Dr. Milnar has received product support from VOCO America, Inc, and Ultradent Products, Inc.
References
1. Small BW. Pretreatment wax-ups and provisionals for restorative dentistry. Gen Dent. 2005;53(2):98-100.2. Spoor R. Predictable provisionalization: achieving psychological satisfaction, form, and function. Pract Proced Aesthet Dent. 2004;16(6): 433-440.
3. Terry DA. Achieving clinical success with provisionals. Inside Dentistry. 2005; 1(1):78-80.
4. Schwedhelm ER. Direct technique for the fabrication of acrylic provisional restorations. J Contemp Dent Pract. 2006;7(1): 157-173.
5. Burke FJ, Murray MC, Shortall AC. Trends in indirect dentistry: 6. Provisional restorations, more than just a temporary. Dent Update. 2005;32(8):443-452.
6. Wynne WP. Considerations for establishing and maintaining proper occlusion in the aesthetic zone. Dent Today. 2004;23(4):112-119.
7. Baltzer A, Kaufmann-Jinoian V. Shading of ceramic crowns using digital tooth shade matching devices. Int J Comput Dent. 2005;8(2):129-152.
8. American Dental Association Council on Dental Materials, Instruments, and Equipment. Recent developments in materials and processes for ceramic crowns. J Am Dent Assoc. 1985;110(4):548-549.
9. Horsted-Bindslev P, Vilkinis V, Sidlauskas A. Direct capping of human pulps with a dentin bonding system or with calcium hydroxide cement. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2003;96(5):591-600.
10. Unemori M, Matsuya Y, Akashi A, et al. Composite resin restoration and postoperative sensitivity: clinical follow-up in an undergraduate program. J Dent. 2001;29(1):7-13.
11. Fondriest JF. Using provisional restorations to improve results in complex aesthetic restorative cases. Pract Proced Aesthet Dent. 2006;18(4):217-223.
 |  | |
| Figure 1 Preoperative view of the patient in natural smile. | Figure 2 View of the enhanced wax-up that was fabricated for the patient's review. | |
 |  | |
| Figure 3 A bite registration was obtained using a fast-setting material. | Figure 4 The polyvinyl stent was filled with the highly esthetic syringable provisional material in shade B1. | |
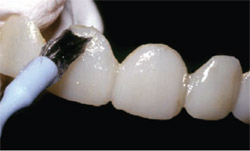 |  | |
| Figure 5 The provisional restoration was glazed using a denture sealant and then lightcured according to the manufacturer's instructions. | Figure 6 A non-eugenol temporary luting cement was loaded into the provisional restorations. | |
 |  | |
| Figure 7 The provisional restoration was completely seated, at which point excess cement was released from the margins. | Figure 8 Close-up view of the patient in natural smile with the polished and sealed provisional restorations in place. | |
 |  | |
| Figure 10 Postoperative 1:1 retracted view of the definitive all-ceramic restorations after cementation. | ||
| Figure 9 Full-facial view of the patient in natural smile with the provisional restorations in place. | ||
| About the Author | ||
 Frank J. Milnar, DDS, AAACD Frank J. Milnar, DDS, AAACDFamily, Cosmetic, and Restorative Dentistry Saint Paul, Minnesota | ||



