Provisional Cements
Howard E. Strassler, DMD
Provisional or temporary cements play an important role in restorative dentistry. They are used for the cementation of temporary indirect restorations including crowns, fixed partial dentures (FPDs), and inlays and onlays, as well as for temporary cementation of definitive restorations of the same types. Provisional cements are also recommended for the cementation of implant crowns and FPDs.
When selecting a provisional cement, there are several criteria that are important in the physical properties and handling of the restorative material, depending on the clinical use selected. The optimal properties of a provisional cement when used for temporary cementation include:
• good retention (adhesion) of the indirect restoration;
• easy to dispense, mix, and apply;
• easy removal of excess from the external surfaces of the restoration after cementation;
• adequate working and setting time;
• optimal viscosity and handling properties for ease of application;
• easy removal of the indirect restoration from the preparation when cemented without damaging the soft tissues, tooth preparation, or pulp;
• easy removal of the provisional cement from the tooth preparation, including dentin and enamel, cast core materials (cast metal, amalgam, composite resin), and implant abutment materials;
• easy removal of the provisional cement from the internal surfaces of the restoration when the restoration needs to be recemented;
• no or minimal reaction to the restorative material;
• biocompatibility to soft tissues, pulp, and tooth structure;
• will not interfere with adhesion of a final cement; and
• good shelf life.
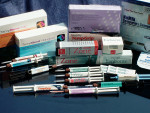
While no one provisional cement fulfills all of these properties, the choice of a provisional cement should depend on the clinical circumstance for which it is chosen. Table 1 lists andFigure 1 shows some provisional cements that a practitioner can choose. When a provisional cement is used to lute a provisional (or temporary) restoration, the ability of the cement to retain the provisional restoration helps that restoration play a significant role as part of the procedure for the fabrication of the final restoration.1
Provisional restorations for natural teeth must protect the pulp. The provisional restoration protects the tooth by minimizing extreme changes in temperature of food and beverages ingested, and the cement provides a seal against microleakage for the period of time that the provisional restoration will be in place.2,3 When the prepared tooth is impressed, the provisional restoration must provide the tooth a stable position within the arch.4,5 Positional stability refers to the provisional restoration being in occlusal function and having proximal contact with adjacent teeth. These parameters contribute not only to the function of the restoration, but also to patient comfort and periodontal health. Also, if the impression is made after the provisional restoration is removed, the provisional cement cannot interfere with the setting reaction and accuracy of the impression material.6 The margins of the provisional restoration must also be well adapted to the tooth preparation finish line without impingement of margins on the periodontium; the provisional restoration must have physiologic contours and embrasures and be highly polished so that the temporary can be cleaned to maintain periodontal health.4 For implant-supported restorations, the provisional restoration also provides a tool for the clinician in determining the new occlusal scheme and contours of the final restoration. One important aspect of provisional cements is that they allow for easy removal of the provisional restoration without harming the periodontium, tooth preparation, or pulp.
Provisional cements also play a role when luting definitive restorations. In some cases, a tooth-supported final restoration—usually all metal or porcelain-metal—is temporarily cemented to evaluate that restoration’s contours and margins as it relates to periodontal health. In the past, provisional cements were opaque in color because of the materials being used. Recently, more tooth-colored provisional cements have been introduced to not interfere with the color evaluation of translucent restoration materials. Examples of color-neutral, shaded, or translucent provisional materials include ZONE (DUX Dental, Oxnard, CA), NexTemp™ (Premier Dental Products, Plymouth Meeting, PA), TempBond® Clear (Kerr Corporation, Orange, CA), and Systemp.link (Ivoclar Vivadent, Amherst, NY). In the case of a FPD with a pontic, some clinicians prefer to first provisionally cement the restoration to assess the periodontal response of the restoration and the adaptation of the tissue-borne side of a pontic. When a FPD has been provisionally cemented, after removal and reevaluation, it is not unusual for some modifications and adjustments to be made where the pontic is contacting the ridge. In some cases, as in a patient who relates a history of dentinal hypersensitivity after tooth preparation and provisional restoration placement, the definitive restoration may be temporarily cemented to assess pulpal health. In these cases, the use of a eugenol-containing provisional cement may have a sedative effect on the pulp.7 One problem with the use of a eugenol-containing provisional cement is the negative effects the eugenol has on dental resins. These cements, if there is residual eugenol remaining after setting, can act as a plasticizer of dental resins, with their greatest effects on acrylic resins, resulting in softening of the resin with a decrease in physical properties.8,9 With the newer eugenol-containing provisional cements, the amount of unreacted eugenol can be minimized by using the correct proportions recommended by the manufacturer.4
When using a provisional cement with natural teeth, the teeth should be evaluated after the removal of the cement on a provisional restoration or final restoration and before the final cementation. Currently, adhesive cements are the most commonly used luting agents for definitive cementation. The tooth surfaces of the preparation must be adequately cleaned to remove the residual provisional cement. A number of studies have investigated the effects of provisional cements on the adhesion of final cements. Both eugenol and eugenol-free provisional cements have been shown to decrease the bond strength of resin-modified glass ionomers, zinc polycarboxylate, and composite-resin bonded cements.10-15 Techniques to remove residual provisional cements from tooth preparations have been evaluated with both eugenol-containing and eugenol-free provisional cements, and include scraping the tooth with a hand instrument, usually a scaler or curet; cleaning the tooth preparation with a prophylaxis cup with a water-pumice paste slurry; and the use of an intraoral sandblaster.16,17 Of the three methods, the intraoral sandblaster method was the most reliable, followed by a prophylaxis cup with a water-pumice paste slurry. If using the water-pumice slurry-polish technique, it is important that all surfaces of the tooth preparation be cleaned, especially the margins, and the tooth be kept clean during final cementation.18 Also, it is important that all residual cement be removed from the final restoration that has been provisionally cemented. This can be accomplished with sandblasting, rotary cleaning on the restoration intaglio surface, ultrasonic cleaning of the restoration, or wiping the surfaces with ethyl alcohol.18,19
When placing final restorations for implant-supported prostheses, some practitioners place the final restoration with provisional cement so it can be more easily removed on a regular basis, or if one or more of the abutments of a FPD come loose, the prosthesis can be removed and recemented. The ability to retrieve cemented implant-supported FPDs using different provisional cements has been evaluated.20-23 These studies found that provisional cements allow for the retrieval of an implant restoration but that cements were different in their retentive ability. When comparing provisional cements to final cements it was found that the more rigid the cement, the greater the difficulty in retrieving the implant restoration from the abutments.23,24 Provisional cements make the removal and retrieval of implant restorations more predictable. The clinician’s judgment to use a certain type of cement for an implant-retained restoration should be based on the circumstance at hand.25
Classes of Provisional Cements
The earliest provisional cements were made from zinc-oxide powder and eugenol liquid (ZOE). These two materials were mixed as a powder-liquid into a paste-like consistency. The ratio of powder to liquid varied from mix to mix, as did the consistency. Wallace described a formula for a predictable ZOE temporary cement in 1933.26 The setting reaction of ZOE cements is a chelation reaction where an amorphous, zinc eugenolate is formed.26 The use of a eugenol-containing provisional cement was recommended for luting provisional restorations for crowns and inlay and onlay preparations to help the pulp “settle down” after the trauma of tooth preparation. Eugenol is known to have an obtundent (sedative) effect on the pulp.7,26 For many years ZOE continued to be the cement of choice for provisional restorations.5 As previously stated, one problem with eugenol-containing temporary cement has been the effect of eugenol on dental resins used in provisional restoration fabrication. Eugenol inhibits the setting reaction of acrylic resins by inhibiting free radical polymerization in the resins used for provisional restorations and softens acrylic resins.8,26 This is problematic if a tooth needs a preparation refined and the resin temporary must be relined to adjust its fit to the tooth. The residual eugenol does not allow new acrylic to be added in a reline of the provisional restoration. A resin-based provisional restoration that is softened when subjected to the forces of occlusion can fracture.8,27 Replacement of a provisional restoration is usually an urgent need and the patient would need to return to the dental office for the fabrication of a new temporary restoration.
To address this problem, a number of manufacturers introduced provisional cements that are eugenol-free.26,28,29 Besides the problems of relining and reusing existing provisional restorations, these cements were also introduced because some patients are hypersensitive to eugenol.30 One problem with the earliest zinc-oxide/non-eugenol provisional cements was their poor physical properties.26 The earliest introduced zinc-oxide/non-eugenol cements did not set as rigidly as ZOE cements and were not as retentive with temporary restorations.31,32 The variety in different compositions of provisional cements and their many applied uses makes it difficult to describe the desired physical properties necessary for their use. Standards for dental ZOE cements and zinc-oxide/non-eugenol cements have been described in ANSI/ADA Specification No. 30 (ISO 3107).26 The limiting values for these physical properties are described and many of the provisional cements meet these specifications. These physical properties include setting time, compressive strength, disintegration, and film thickness.
Recently, a number of improved eugenol-free cements have been introduced. While in the past eugenol-free cements meant the cements still had zinc oxide, there are eugenol-free cements that are not based on the original formulations. Some provisional cements have added ingredients for additional benefits of their material, eg, Temp Advantage™ (GC America, Inc, Alsip, IL) and TempSpan® CMT (Pentron Clinical Technologies, LLC, Wallingford, CT). They contain additives of fluoride and potassium nitrate for desensitization of the preparation. TempSpan CMT also contains calcium phosphate, and Temp Advantage contains chlorhexidine for preparation disinfection.
Some eugenol-free provisional cements have been formulated to address problems identified with past cements. These included the need for a more rigid provisional cement to improve the retention of the restoration and easier clean-up of the provisional cement from the preparation and restoration. A clinician may use different provisional cements for different circumstances. For example, achieving easier removal of the restoration at a later time will indicate one cement, while the need for better retention on a crown preparation that is not well retentive because of its occlusal-gingival height or because of the presence of excess taper to the axial walls of the crown preparation will indicate a more rigid provisional cement. TempoSIL® (Coltène/Whaledent Inc, Cuyahoga Falls, OH) achieves both goals. It is an addition-cured, silicone-based zinc-oxide temporary cement with a silane agent for improved adhesion and marginal integrity. This formula produces a firm, yet elastic temporary cement that can be easily peeled off the tooth preparation (either natural tooth, core of restorative material, or implant abutment) and easily removed from the internal surfaces of both provisional and final restorations. Other provisional cements, such as UltraTemp® (Ultradent Products, Inc, South Jordan, UT) and HY-Bond Polycarboxylate Temporary Cement (Shofu Dental Company, San Marcos, CA) use a polycarboxylate formulation to make them eugenol-free. UltraTemp addresses the need for greater rigidity for restoration retention; it is available in two different formulas—regular and rigid set. HY-Bond has one formula for a more rigid set. TempSpan CMT is a resin-based formulation that provides for a translucent color, greater rigidity, and a two-stage gel-setting reaction for easy removal of excess. TempSpan CMT also has sodium fluoride, potassium nitrate, and calcium phosphate for decreased sensitivity.
Convenience Packaging with Provisional Cements
In the past, many temporary cements were packaged in paste-squeeze tubes. There are problems associated with dispensing and maintaining these tubes. It would not be unusual to have excess cement extruding from the tube, making the tube sticky and difficult to clean because of the oily consistency of the pastes. Convenience packaging has made the use of provisional cements easier with more consistent dispensing. When ZOE provisional cement is desired, Embonte2 (Dux Dental) affords convenient and easy-to-use packaging. Embonte2 is provided in unit-dose packaging, which allows it to be dispensed in the right amount of both base and catalyst paste for a single-unit provisional crown cementation. Embonte2 has the same ZOE formulation and is dispensed in a dual-cartridge auto-aspirating syringe that eliminates the waste of conventional squeeze tubes with its patented auto-aspirating feature.
If convenience packaging is desired with a eugenol-free provisional cement there are a number of good choices. Some paste is moisture-sensitive and self-setting, and is available in a unit-dose. Eugenol-free NoMix® Temporary Cement (Centrix Dental, Shelton, CT) is a single-paste, no-mix, moisture-activated temporary cement. The interior of the restoration can be wetted with water before the cement is dispensed into the restoration. Initial set for clean-up is 5 minutes, with complete setting in 15 minutes. This extended working time allows for its use with single units and multiple units. Also, this temporary cement is packaged in a unit-dose so the patient can take it home to re-cement his or her own provisional restoration.
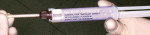
Many of the newest provisional cements are available in a double-barreled automixing syringe. In the case of TempoCem® NE (Zenith Dental, Englewood, NJ) a double-barreled cartridge is dispensed using a gun-type applicator similar to those used with bis-Acryl provisional composite resins. Automixing a dual-tube provisional cement allows the chairside assistant to dispense the right amount for a single unit or multiple units directly into the provisional restoration Figure 2). It also means that each mix is consistent because the catalyst and base paste will always be dispensed through the mixing tip in the optimal volume ratio and mixed in a consistent fashion through the automix tip. It also minimizes waste and eliminates the clean-up of a cement spatula and mixing pad.32 Some of the products that are available in this automix, double-barreled syringe are Temp Advantage, TempSpan CMT, ZONE, Systemp.cem, and TempoSil.
Techniques For Easy Intraoral Clean-up and Removal
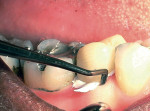
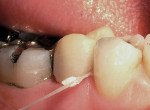
Once the provisional restoration has been adapted, finished, and polished, it is ready for cementation. To avoid leaving a white streak of provisional cement around the margins of the restoration and to facilitate the removal of excess provisional cement, the polished surfaces of the provisional restoration can be lightly painted using a disposable brush with a petroleum gel Figure 3). Using petroleum gel on the tissue-surface side of a pontic and cervical to the connector of a FPD provisional also makes set temporary cement easier to remove. A problem area when removing provisional cement is the gingival embrasure below the contact area. Just flossing the contact will often not allow for cement removal. Gross cement can be easily removed after the complete set of the cement with a scaler Figure 4). For teeth with large gingival embrasures, there are times when the cement is more difficult to remove from the embrasure spaces. For these cases, tying two to three knots into the end of dental floss will allow the larger knotted area to pull out the set cement Figure 5). It is critical that all residual temporary cement be removed. Excess cement remaining in the sulcus can result in irritation of the periodontium and, in the most extreme cases, result in severe periodontal inflammation with the potential for bone loss.1,4
Conclusion
While there is no one provisional cement that meets all of the requirements of an ideal temporary cement, the current generation of provisional cements offers a number of advantages over what has been used in the past. If you are having success with the provisional cement you are currently using, there is no reason to make a change. If you have expanded the types of restorations you are placing to include all-ceramic and implants, there may be a need for more than one brand of provisional cement. The advantages of a more rigid-setting provisional cement may be necessary for a number of clinical situations, including a crown with compromised retention or a patient who has parafunctional habits that will dislodge the restoration. If you are having problems with postoperative sensitivity during provisional cementation, either a eugenol-containing provisional cement or a eugenol-free formulation with additives for desensitizing may solve these problems. It may be necessary to have at least two different provisional cements to accommodate your practice. Of importance with the use of any cement, the provisional cement must be cleaned thoroughly from the tooth before definitive cementation.
Disclosure
The author has received grant and research support from Centrix Dental, DENTSPLY Caulk, and Ultradent Products, Inc.
References
1. Bral M. Periodontal considerations for provisional restorations. Dent Clin North Am. 1989;33(3):457-477.
2. Mash LK, Beninger CK, Bullard JT, Staffanou RS. Leakage of various types of luting agents. J Prosthet Dent. 1991;66(6): 763-766.
3. Pan YH, Ramp LC, Lin CK, Liu PR. Comparison of 7 luting protocols and their effect on the retention and marginal leakage of a cement-retained dental implant restoration. Int J Oral Maxillofac Implants. 2006;21(4):587-592.
4. Geganuff AG, Holloway JA. Provisional restorations. In: Rosensteil SF, Land MF, Fujimoto J. Contemporary Fixed Prosthodontics. 4th ed. Mosby Elsevier. St. Louis; 2006:466-504.
5. Shillingburg HT Jr. Provisional restorations. In: Shillingburg HT, Hobo S, Whitsett LD, et al. Fundamentals of Fixed Prosthodontics. 3rd ed. Quintessence Publishing: Chicago; 1997:225-256.
6. Jones RH, Cook GS, Moon MG. Effect of provisional luting agents on polyvinyl siloxane impression material. J Prosthet Dent. 1996;75(4):360-363.
7. Pashley EL, Tao L, Pashley DH. Sealing properties of temporary filling materials. J Prosthet Dent. 1988;60(3):292-297.
8. Gegauff AG, Rosensteil SF. Effect of provisional luting agents on provisional resin additions. Quintessence Int. 1987;18(12):841-845.
9. Millstein PL, Nathanson D. Effect of eugenol on cured composite resin. J Prosthet Dent. 1983;50(2):211-215.
10. Terata R, Nakashima K, Kubota M. Effect of temporary materials on bond strength of resin-modified glass-ionomer luting cements to teeth. Am J Dent. 2000;13(4):209-211.
11. Erkut S, Kücükesmen HC, Eminkahvagil N, et al. Influence of previous provisional cementation on the bond strength between two definitive resin-based luting and dentin bonding agents and human dentin. Oper Dent. 2007;32(1):84-93.
12. Paul SJ, Schärer P. Effect of provisional cements on the bond strength of various adhesive bonding systems on dentine. J Oral Rehabil. 1997;24(1):8-14.
13. Carvalho CN, de Oliveira Bauer JR, Loguercio AD, Reis A. Effect of ZOE temporary restoration on resin-dentin bond strength using different adhesive strategies. J Esthet Restor Dent. 2007;19(3):144-152.
14. Dilts WE, Miller RC, Miranda FJ, Duncanson MG Jr. Effect of zinc oxide-eugenol on shear bond strengths of selected core/cement combinations. J Prosthet Dent. 1986;55(2): 206-208.
15. Tjan AHL, Nemetz H. Effect of eugenol-containing endodontic sealer on retention of prefabricated posts luted with an adhesive composite resin cement. Quintessence Int. 1992;23(12):839-844.
16. Fonseca RB, Martins LR, Quagliatto PS, Soares CJ. Influence of provisional cements on ultimate bond strength of indirect composite restorations to dentin. J Adhes Dent. 2005;7(3):225-230.
17. Grasso CA, Caluori DM, Goldstein GR, Hittelman E. In vivo evaluation of three cleansing techniques for prepared abutment teeth. J Prosthet Dent. 2002;88(4):437-441.
18. Rosensteil SF. Luting agents and cementation procedures. In: Rosensteil SF, Land MF, Fujimoto J. Contemporary Fixed Prosthodontics. 4th ed. Mosby Elsevier. St. Louis; 2006:909-927.
19. Mosharraf R. A simple method for cleaning zinc oxide-eugenol provisional cement residues from the intaglio surface of casting restorations. J Prosthet Dent. 2004;91(2):200.
20. Ramp MH, Dixon DL, Ramp LC, et al. Tensile bond strengths of provisional luting agents used with an implant system. J Prosthet Dent. 1999;81(5):510-514.
21. Lepe X, Bales DJ, Johnson GH. Retention of provisional crowns fabricated from two materials with the use of four temporary cements. J Prosthet Dent. 1999;81(4):469-475.
22. Michalakis KX, Pissiotis AL, Hirayama H. Cement failure loads of 4 provisional luting agents used for cementation of implant-supported fixed partial dentures. Int J Oral Maxillofac Implants. 2000;15(4): 545-549.
23. Akca K, Iplikcio€lu H, Cehreli MC. Comparison of uniaxial resistance forces of cements used with implant-supported crowns. Int J Oral Maxillofac Implants. 2002;17(4): 536-542.
24. Pan YH, Lin CK. The effect of luting agents on the retention of dental implant-supported crowns. Chang Gung Med J. 2005;28:403-410.
25. Mansour A, Ercoli C, Graser G, et al. Comparative evaluation of casting retention using the ITI solid abutment with six cements. Clin Oral Implants Res. 2002;13(4): 343-348.
26. Powers JM. Cements. In: Craig RG, Powers JM. Restorative Dental Materials. 11th edition. Mosby, St. Louis, 2001:593-634.
27. Rosensteil SF, Gegauff AG. Effect of provisional cementing agents on provisional resins. J Prosthet Dent. 1988;59(1):29-33.
28. Sadan A. Clinical considerations in cement selection for provisional restorations—Part I. Pract Periodontics Aesthet Dent. 2000;12(7): 638.
29. Sadan A. Clinical considerations in cement selection for provisional restorations—Part 2. Pract Periodontics Aesthet Dent. 2001;13(1):16.
30. Sarrami N, Pemberton MN, Thornhill MH, Theaker ED. Adverse reactions associated with the use of eugenol in dentistry. Br Dent J. 2002;193(5): 257-259.
31. Strassler HE, Gonzales R. Unique delivery systems for temporary cements for provisional restorations. Contemporary Esthetics and Restorative Practice. 2005;9(3): 70-72.
32. Strassler HE, Tomona N, Serio CL. Anterior provisional restorations with a translucent prefabricated crown form. Contemporary Esthetics and Restorative Practice. 2004;8(9):44-48.
About the Author
Howard E. Strassler, DMD
Professor and Director of Operative Dentistry
Department of Endodontics
Prosthodontics, and Operative Dentistry
University of Maryland Dental School
Baltimore,Maryland