Palatal Lesions
Ines Velez, DDS; and Michael A. Siegel, DDS
The keratinized, stratified, squamous mucosal lining covering the hard palate is bordered laterally and ventrally within the upper alveolar ridge mucosa. Dorsally, this lining epithelium is bordered by the oropharyngeal soft palatal mucosa. Several types of oral and oropharyngeal pathologic lesions may appear in this area. There are a number of conditions that have special predilection for this site.
Torus palatinus, probably the most common palatal entity,1 presents as an osseous, exophytic, centrally located, midline, usually symmetric asymptomatic lesion of the hard palate. The epithelial tissues over tori are attenuated (stretched) due to the underlying bony prominence, subjecting this site to ulcerations of traumatic origin. Inflammatory lesions of dental origin are also common conditions present in the hard palate.1
Malignant squamous epithelial neoplasms—such as squamous cell carcinoma, verrucous carcinoma, and carcinoma of the maxillary sinus—may also appear in this area. Carcinoma of the maxillary sinus usually remains asymptomatic for a long period of time.1 Eventually, the tumor grows to fill the sinus and the diagnosis is made because the lesion has produced a bulge of the palatal or alveolar ridge area. This is a tumor usually associated with elderly patients.1
Squamous cell carcinoma from the soft palate is often painful, may cause dysphagia, and offers a worse prognosis than tumors located in more anterior locations. Squamous cell carcinomas extending from the maxillary alveolar ridge onto the hard palate may present a diagnostic challenge as they mimic periodontal disease or pyogenic granulomata. Alveolar and palatal carcinomas are usually painless. Verrucous carcinoma is a type of squamous cell carcinoma that exhibits a papillary, white clinical appearance, behaves indolently, and rarely metastasizes. The most common locations for this condition are the hard palate and the alveolar ridge, and they are often associated with elderly patients wearing complete denture prostheses.1
The numerous small minor salivary glands located within the submucosa of the palate are capable of developing a wide range of conditions.2 For example, necrotizing sialometaplasia is a salivary gland condition that usually appears as a crater-like defect of the posterior palate, may be associated with pregnancy, and, while ominous in appearance, will usually resolve spontaneously after biopsy confirmation of the diagnosis.1
Salivary gland tumors represent a diverse group of neoplasms. The majority of these tumors are of ductal or acinic epithelial derivation. Although tumors of salivary glands are not common, they are also not rare in occurrence.3 The biologic behavior of salivary gland tumors is paradoxical. A benign tumor of salivary glands tends to exhibit a more aggressive behavior pattern than the usual benign tumor, while a malignant tumor of salivary glands is less aggressive than the usual malignant tumor.3
Minor salivary gland tumors have an affinity for the posterior hard palate and the soft palate, and virtually never arise in the midline; this is probably due to the natural distribution of salivary tissues of the palate.3 Both benign and malignant salivary gland neoplasms of the palate appear as well-circumscribed, dome-shaped, smooth-surfaced, non-movable swellings that exhibit a very slow growth pattern. Pain and ulceration are occasionally seen in adeno-carcinomas at this site.
The most common benign salivary gland tumor of the palate is the pleomorphic adenoma.4,5 The most common malignant tumors of the palate are adenoid cystic carcinoma (cylindroma), followed by polymorphous low-grade adenocarcinoma and then mucoepidermoid carcinoma.5 Most of these tumors, both benign and malignant, are asymptomatic masses or are associated with a low level of discomfort. As previously mentioned, constant pain in the palate associated with a gradual increase in intensity, and usually present before any noticeable swelling, is a common and important finding of adenocystic carcinoma. Malignant tumors of the palate may show radiographic evidence of bone destruction and sometimes a radiopacity produced by the neoplastic mass. Intraosseous salivary gland tumors also may develop within the jaws.3
Melanoma is a malignant tumor of melanocytic origin. Although the vast majority of them occur on the skin,4 they may develop in any site, such as the oral cavity, where melanocytes exist. Oral melanoma appears predominantly on the hard palate or maxillary alveolus and tends to be much more aggressive than its cutaneous counterpart. Early lesions are usually flat and later become nodular and fixed. Most melanomas appear as dark/light brown lesions.2,6-8 The prognosis of non-skin melanoma is very poor and is primarily dependent on its depth. As a general rule, the “3-D” rule can be applied to a melanoma’s prognosis.9 The darker the melanoma appears clinically, the deeper it is within the epithelium and, therefore, the deadlier will be the result of this tumor. It is usually the most aggressive malignant neoplasm of the human body.3
To clinically differentiate a melanoma from a nevus, another pneumonic is used: the “ABCD” system. The “ABCD” system is widely used by dermatologists and stands for:
• Asymmetry of the lesion;
• Border irregularity;
• Color variation; and
• Diameter greater than 0.6 cm.9
Lymphoma (lymphosarcoma) constitutes a diverse and complex group of malignancies of lymphoid histogenesis.10,11 The most frequent locations of extra nodal lymphoma in the head and neck are the posterior hard and the soft palate. Lymphomas usually appear as a non-tender diffuse mass and are rarely ulcerated. Many salivary gland lymphocytic infiltrates of the palate are actually non-Hodgkin’s B-cell lymphomas of the mucosa-associated lymphoid tissue (MALT).11 Sarcomas—malignant tumors of nonepithelial-tissue origin—may arise in any location of the human body and they usually appear as ulcerated masses in young or middle-aged people.
CASE PRESENTATION 1
A 19-year-old Caucasian man presented to Nova Southeastern University’s Oral and Maxillofacial Surgery Department complaining about a “painful eruption of the wisdom tooth.” The patient was unaware of any history of present illness until the acute onset of the painful eruption approximately 2 months earlier. Medical history, dental history, social history, and family history were unremarkable. There were no extraoral signs of disease present. Intraoral examination showed an exophytic, crater-form, ulcerated, macerated, well-circumscribed lesion measuring approximately 2.5 cm in diameter and covered by a fibrino-purulent membrane. The lesion was located palatal to the alveolar ridge and extended to the midline of the palate (Figure 1). No radiographic manifestations were seen in panoramic, periapical, and occlusal radiographs. All teeth in the maxillary left quadrant were vital.
Palatal torus and odontogenic infection were easily ruled out of the differential diagnosis by reviewing the clinical and radiographic manifestations. This lesion appeared as an ulcerated, fast-growing mass in the area where salivary gland tumors are usually located. A malignant salivary gland tumor was the first clinical consideration because of the lesion’s location, aggressive nature, and rapid growth rate. Necrotizing sialometaplasia, a crater-like ulcer, does not exhibit a large nodular growth similar to the case presented here; therefore, it was not considered into the differential diagnosis. Conventional squamous cell carcinoma, verrucous carcinoma, and carcinoma of the maxillary sinus were ruled out due to the patient’s young age.
Sarcomas may be present in young people with the clinical characteristics seen in this case. Approximately 40% of rhabdomyosarcomas and 14% of neurogenic sarcomas occur in the head and neck area.4 They were included in the differential di-agnosis. Liposarcoma, fibrosarcoma, and chondrosarcoma are rare in the oral cavity; osteosarcoma generally will show radiographic changes; and angiosarcoma exhibits a purple, reddish discoloration of the mucosa.1
Melanoma is commonly a dark-colored lesion that usually begins as a brown to black macule with irregular borders, but then a lobulated, painless mass develops. Satellite lesions are commonly seen. However, amelanotic melanomas occur. About 20% of oral melanomas contain so little pigment that they have a normal mucosal color.1 For this reason, melanoma is often included in a differential diagnosis of an aggressive lesion, because it has a reputation for mimicking other pathologic entities. MALT lymphoma was not considered into the differential diagnosis of this case. Usually a low-grade non-Hodgkin’s lymphoma, MALT lymphoma may develop into a high-grade tumor with aggressive behavior, which may appear as a palatal ulcerated mass, but it appears diffuse and its borders are not clearly delineated.10
The final differential diagnosis included: malignant salivary gland tumor, sarcoma, and melanoma. An incisional biopsy was performed using local anesthesia. Microscopic histopathologic examination revealed infiltrating carcinoma showing a uniform pattern, with duct and gland-like structures, which was not reminiscent of any other malignant neoplasm of salivary glands. Perineural invasion of the nerve sheath was present. The diagnosis was adenocarcinoma NOS (not otherwise specified). The patient was treated with a wide surgical excision and adjuvant radiation therapy. The prognosis for this tumor is poor, with a 5-year survival rate of 56%.5
CASE PRESENTATION 2
A 38-year-old South American patient was referred to Nova Southeastern University for the diagnosis of a mass in the left lateral palate. The patient noticed the lesion and a slight swelling of the left side of the face approximately 1 month prior to the consultation. No significant medical, dental, family, or social history was presented. Physical examination showed a well-developed, well-nourished man with a small swelling of the left maxillary face (Figure 2). No fever, pain, bleeding, or paresthesias were identified. During intraoral examination a large, firm mass covered by normal mucosa, completely occupying the left palate, was noted (Figure 3).
The lesion extended from the palatal midline medially into the fornix of the vestibule laterally and covered the alveolar ridge in an edentulous area. The borders of this mass were fixed to the surrounding tissues. The remaining teeth in this quadrant were vital. No radiographic changes were found in the panoramic, occlusal, or periapical films. The differential diagnosis included: sarcoma, salivary gland tumor, and MALT lymphoma. An incisional biopsy was performed on an outpatient basis under local anesthesia. The histopathologic examination revealed nests of atypical melanocytic cells with high mitotic activity and pleomorphic nuclei. A working diagnosis of melanoma was rendered and the patient was re-ferred for positron emission tomography (PET) studies. After medical consultation, PET scanning, and medical laboratory testing, a definitive diagnosis of primary melanoma of the liver was confirmed. The patient refused treatment and returned to his country of origin.
DISCUSSION
The diagnosis of palatal lesions constitutes a challenge for the clinician. The palate is a complex area of the mouth with a variety of native tissue types that give rise to a plethora of different pathologies. Understanding the lesions of the palate requires appreciation of the different tissues native to the region and the complexity of the salivary glands and their structural components. Salivary gland tumors are set apart from the rest of the palatal pathologies due to the extensive number of these lesions that had been identified. The United States Armed Forces Institute of Pathology (AFIP) has classified salivary gland tumors into these categories: 13 benign tumors; six malignant, low-grade tumors; 10 malignant, intermediate-grade tumors; and 13 malignant, high-grade neoplasms.12 The posterior palate is also a part of the Waldeyer’s ring and presents numerous aggregates of normal, protective lymphoid tissue that may give origin to lymphoma.11-14 Significant numbers of melanocytes are normally found in the palatal mucosa; in fact, the most common place for a melanocytic nevus and melanomas of the oral cavity is the palate.7 Approximately 30% of melanomas arise from previously existing pigmented lesions.1,4 Respiratory epithelium, native to the maxillary sinus, may be the source of lesions appearing in the palate, especially in the presence of an oral-antral communication.3,15 Squamous epithelium, fibrous tissue, periosteum, skeletal muscle, smooth muscle, nerve fibers, endothelium, bone, and fat tissue are present throughout the area. The key to success in the diagnosis and treatment of any of these lesions is knowledge of the anatomy of the palatal structures and a high index of clinical suspicion. The astute clinician will remember that early diagnosis often leads to the best prognosis for the patient. It is, therefore, imperative for all dentists to be vigilant in performing a careful head-and-neck cancer examination for each and every one of their patients.
References
1. Neville BW, Damm DD, Allen CM, et al. Oral and Maxillofacial Pathology. 2nd ed. Philadelphia, PA; WB Saunders: 2001:400.2. Dardick I, Van Nostrand AW. Morphogenesis of salivary gland tumors. A prerequisite to improving classification. Pathol Annu. 1987;22:1-53.
3. Batsakis JG. Tumors of the head and neck. 2nd ed. Baltimore, MD: Williams & Wilkins; 1979:1-99.
4. Pilch BZ. Head and Neck Surgical Pathology. 1st ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2000:389-420.
5. Ellis GL, Auclair PL, Atlas of Tumor Pathology: Tumors of the Salivary Glands. Washington DC Armed Forces Institute of Pathology, 1996:300-373.
6. Rintala AE. Solitary metastatic melanoma of the soft palate. Am Path Surg. 1987;5:463-465.
7. Bongiorno MR, Arico M. Primary malignant melanoma of the oral cavity: A case report. Int J Dermatol. 2002;41:178-181.
8. Owens JM, Gomez JA, Byers RM. Malignant melanoma of the palate of a 3-month old child. Head Neck. 2000;24(1):91-94.
9. Abbasi NR, Shaw HM, Rigel DS, et al. Early diagnosis of cutaneous melanoma. Revisiting the ABCD criteria. J Am Dent Assoc. 2004;292(22):2771-2776.
10. Tan LH. Lymphomas involving Waldeyer’s ring: placement, paradigms, peculiarities, pitfalls, patterns and postulates. Ann Acad Med Singapore. 2004;33(Suppl):S15-S26.
11. Makepeace AR, Fermont DC, Bennett MH. Non-Hodgkin’s lymphoma of the nasopharynx, para-nasal sinus and palate. Clin Radiol. 1989;40(2):144-146.
12. King AD, Kik L, Ahuja AT. MRI of primary non-Hodgkin’s lymphoma of the palatine tonsil. Br J Radiol. 2001;74:226-229.
13. Bertoni F, Sauna P, Tinquely M, et al. Association of gastric and Waldeyer’s ring lymphoma. Hematol Oncol. 2000;18(1): 15-19.
14. Saul SH, Kapadia SB. Secondary lymphoma of Waldeyer’s ring: natural history and association with prior extranodal disease. Am J Otolaryngol. 1986;7(1):34-41.
15. Marx RE, Stern D. Oral and Maxillofacial Pathology: A Rationale for Diagnosis and Treatment. 2nd ed. Quintessence Publishing. 2003;725, 736, 833.
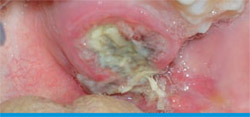 | 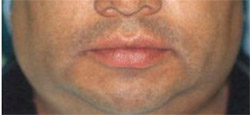 | |
| Figure 1 Palatal lesion covered by a fibrinopurulent membrane. | Figure 2 Case presentation 2. Note the small swelling visible in the left maxillary face. | |
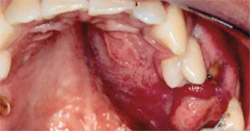 | ||
| Figure 3 Lesion discovered on intraoral examination. Described as a large, firm mass covered by the normal mucosa and completely occupying the left palate. | ||
| About the Authors | ||
 Ines Velez, DDS Ines Velez, DDSAssociate Professor and Director Oral and Maxillofacial Pathology Service Nova Southeastern University College of Dental Medicine Fort Lauderdale, Florida | ||
| Michael A. Siegel, DDS Professor and Chairman Department of Diagnostic Sciences Nova Southeastern University College of Dental Medicine Fort Lauderdale, Florida | ||



