Novel Materials Work Best with Proper Preparations
Robert B. Mongrain, DMD
The variety of materials coming to the dental market today continues to provide new and exciting ways to restore teeth that that have been damaged by dental disease. As material choices increase, the clinician’s responsibility to continue to learn and strive to understand the materials he or she chooses to work with also increases.
Many resources are available to provide the information necessary to incorporate these new materials into the dental practice. The focus is primarily on the strength characteristics and esthetics of these materials. As a result, the most active area of education is training in the proper adhesion of the restoration to the tooth. Certainly adhesive bonding is the most technique-sensitive and failure-prone link in the chain. Improper adhesion may cause sensitivity, pulpal death, recurrent decay, or fracture of the restoration.1 This is not conducive to raising the level of quality in dental practices.
With all of the attention given to these topics, one key issue is often overlooked—the importance of the preparation in concert with the type of material being used in the particular restoration being placed. Very often clinicians develop an idea of what full- and partial-coverage restorations should look like during their dental education. While they may perform these preparations well, the assumption is often made that the same preparation techniques learned for one type of material, such as the common porcelain-fused-to-metal restoration, can be directly transferred to other types of materials. Actually, the reverse is true. When first making the transition to all-ceramic materials, the con-cepts of preparation that are useful in metal can be detrimental to non-metallic materials.2
In this article the author will examine the importance of executing the preparation in such a way as to enhance the success of the clinical restoration. No matter how much education and knowledge is gained concerning the characteristics of the materials and the proper adhesive techniques, an improperly prepared tooth cannot be overcome. Proper shaping at the margin, the correct contours, and adequate interocclusal reduction must all be carefully performed to achieve clinical success.
After the introduction of the Empress® system by Ivoclar Vivadent (Amherst, NY),3 more and more dentists have become comfortable in providing all-ceramic options for their patients. Another milestone was the introduction of the “chairside” CEREC® 3D system, by Sirona Dental Systems, Inc (Charlotte, NC), which for the first time allowed the clinician to prepare and seat an all-ceramic restoration in the same visit. Today the technology is well established both by academic research and clinician acceptance.4 Another chairside system will be coming to the United States very soon. The E4D system, manufactured by D4D Technologies LLC (Richardson, TX), is currently in the latter stages of clinical testing and development. Perhaps a more significant development is the recent introduction of a number of new CAD/CAM in-lab systems, such as the Lava™ All-Ceramic System, by 3M ESPE (St. Paul, MN), and the Cercon® Zirconia System from DENTSPLY International (York, PA).
Some current materials available for the CEREC system for chairside use are of similar strength to the IPS Empress® system.5 These materials have a proven track record of clinical success but all require adhesive cementation, which is a technique-sensitive process.6 As previously mentioned, most dentists would like to reduce their dependence on adhesive bonding. A new material that has been released for the CEREC system is the IPS e.max CAD LT by Ivoclar Vivadent. This material is made up in part of lithium disilicate glass. When fully crystallized, it has a biaxial fracture strength of 360 MPa, according to the manufacturer.7 This compares to values commonly reported for previously available chairside materials of 150 MPa to 180 MPa.6 The lithium disilicate glass system has been available for some time in the form of IPS Empress® 2 and, more recently, the IPS e.max CAD HT block used with the inLab® system by Sirona Dental Systems, Inc for framework fabrication of laboratory restorations. The esthetics of the blocks have been enhanced to allow for chairside use with simple staining and glazing for single-visit placement. To achieve maximum strength with this system, a 25-minute crystallization firing is required after milling and fitting the restoration.8 Once this has been done, the restoration can be prepared and either cemented or bonded depending on the clinical situation. This provides greater flexibility in clinical applications for chairside-fabricated restorations, with the ability to use conventional cementation in cer-tain situations and to rely less on adhesive bonding and more on the strength of the material itself for the success of the restoration.
CASE PRESENTATION
A 39-year-old woman presented with a deep carious lesion in the lower left first premolar that required endodontic therapy. After endodontic therapy was completed, it was decided to restore the tooth in a single visit. Because the tooth had significant loss of structure and molars had been lost to previous decay, there was a desire to complete the restoration with the highest-strength material possible. With the advent of IPS e.max CAD LT blocks for the CEREC system, it was possible to restore the tooth with a material more fracture resistant than other chairside CAD/CAM materials, with good esthetics, in a single visit.
Figure 1shows the tooth before restoration. After the endodontic procedure was completed, a post was placed using a RelyX™ Fiber Post (3M ESPE) cemented with RelyX™ Unicem self-adhesive cement. The core was built up with FluoroCore® from DENTSPLY Caulk (Milford, DE).
The preparation was begun after the build-up was completed. As noted earlier, a planned, sequential approach to preparation combined with a clear understanding of the preparation requirements is critical to optimize success with new materials. The manufacturer’s recommendation for tooth reduction for the IPS e.max CAD LT is as follows: a minimum 1.5 mm of occlusal reduction, 1.5 mm of axial reduction, and a 1-mm shoulder at the gingival margin.
Logical diamond-bur shape selection with the final preparation design in mind will help ensure adequate and appropriate reduction. In this case, the occlusal reduction was begun with a larger diamond. Figure 2 shows the Two Striper® 364.5C (Premier Dental Products Company, Plymouth Meeting, PA) pear-shaped diamond cutting at an angle to the long axis of the tooth. Cutting grooves just past the depth of the end of the diamond will provide the minimum 1.5-mm reduction. Finishing the occlusal reduction can be accomplished with a football-shaped bur, such as a Two Striper 285.5, while following the contours of the occlusal anatomy.
Next, using a thin tapered diamond (Two Striper 781.1C), the contacts were carefully opened (Figure 3). To quickly accomplish the bulk axial reduction, a tapered cylinder with rounded corners with at least a 1-mm tip is required. The author suggests at least a 1.2-mm tip to ensure adequate reduction. Figure 4 shows a Two Striper 2001.8 KR performing bulk reduction. This turbo diamond in a KR style ensures maximum cutting efficiency, and the rounded edges of the tip eliminate sharp angles in the margin. Final smoothing of the margins was accomplished with a fine-grit diamond of the same shape (Figure 5).
After the preparation, a diode laser was used to control bleeding and to expose subgingival margins. The completed preparation is shown in Figure 6. The preparation was then powdered for imaging with the CEREC 3D system. Using a bite registration in CEREC antagonist mode, the occlusion and contours were established and a shade A2 IPS e.max CAD LT block was milled. Figure 7 shows the restoration tried in the mouth before final crystallization.
Crystallization according to the manufacturer’s recommended cycle was performed next. Glaze and stain designed specifically for the IPS e.max CAD LT material were applied before crystallization to accomplish all of the firing tasks in one step, minimizing necessary chair time. The restoration was cemented with Multilink® Automix (Ivoclar Vivadent) translucent. After removal of excess cement, the restoration was light-cured for maximum bonding, finished, and polished. After seating, final adjustments to the occlusion were made with a finishing diamond and copious water spray. The Diamond Twist SCL™ and Diamond Twist SCO™ (Premier Dental Products Company) polishing systems are especially effective on the ceramic, creating minimal heat rise and providing a high-gloss shine similar to glazing. The final result has excellent esthetics and strength in a single clinical visit (Figure 8).
CONCLUSION
New technologies offer new opportunities. When using these advances it is necessary to learn all aspects of the materials, including preparation requirements, to ensure excellent clinical results.
References
1. Perdigao J, Geraldeli S, Hodges JS. Total etch versus self-etch adhesive: effect on postoperative sensitivity. J Am Dent Assoc. 2003;134(12):1621-1629.2. Preparation guidelines. Ivoclar Vivadent®. December 2006.
3. Lehner C, Studer S, Brodbeck U, et al. Short-term results of IPS-Empress full-porcelain crowns. J Prosthodont. 1997;6(1):20-30.
4. Dunn M. Biogeneric and user-friendly: The Cerec 3D software upgrade V3.00. Int J Comput Dent. 2007;10(1):109-117.
5. Wassell RW, Walls AW, Steele JG. Crowns and extra-coronal restorations: materials selection. Br Dent J. 2002;192(4):205-211.
6. Attia A, Abdelaziz KM, Freitag S, Kern M. Fracture load of composite resin and feldspathic all-ceramic CAD/CAM crowns. J Prosthet Dent. 2006;95(2):117-123.
7. Data on file. IPS e.max CAD Scientific Documentation, Ivoclar Vivadent®.
8. Directions for use, E-Max CAD. Ivoclar Vivadent®. December 2006.
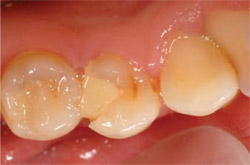 | 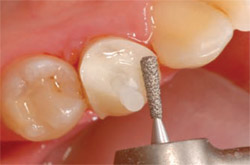 | |
| Figure 1 Preoperative photograph. | Figure 2 The Two Striper 364.5C. | |
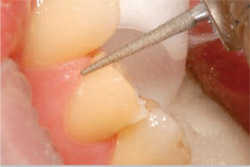 | 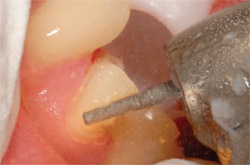 | |
| Figure 3 Open contact with the 781.10C. | Figure 4 Bulk reduction with the 2001.8C KR. | |
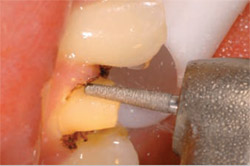 | 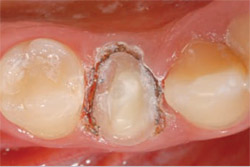 | |
| Figure 5 Refining the margin with the 703.8F KR. | Figure 6 The finished preparation. | |
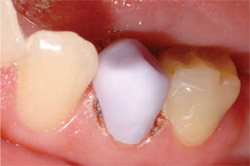 | 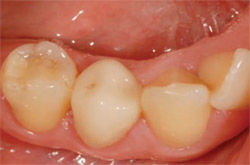 | |
| Figure 7 Restoration try-in. | Figure 8 Postoperative photograph. | |
| About the Author | ||
 Robert B. Mongrain, DMD Robert B. Mongrain, DMDPrivate Practice Tulsa, Oklahoma | ||



