Computer-Assisted Implant Technology—Incorporating Surgical and Restorative Implications
Louis F. Rose, DDS, MD; Howard Fraiman, DMD; and Jeffrey S. Ingber, DDS
Computed tomography (CT) technology uses computers to process 2-dimensional radiographic images, generating a 3-dimensional (3-D) image of body tissues and organs. Within the dental realm, CT scans traditionally have been used by oral and maxillofacial surgeons and periodontists. For orthognathic surgery, facial reconstruction, treatment of traumatic injuries, alveolar ridge augmentation and sinus grafting, and removal of impacted teeth, especially those adjacent to nerves, the use of a CT scan has been considered the standard of care. Having a 3-D view of the surgical site greatly enhances the surgeon’s ability to plan the case and perform expedited procedures that require less healing time, resulting in greater patient comfort and satisfaction.
The authors believe that several trends are converging to expand the routine use of CT scans to general dentists, such as:
- patients are demanding less-invasive procedures;
- patients want shortened healing times;
- patients want to experience minimal discomfort as they look to dentistry to provide them with results usually associated with plastic surgery;
- discretionary spending by patients to achieve a more youthful and esthetic appearance is increasing; and
- patients want to achieve these results with fewer appointments.
In response to these concerns, tools for facilitating implant treatment planning and surgical implementation have evolved. One such tool is the NobelGuide™ system developed by Nobel Biocare (Yorba Linda, CA). In the authors’ experience, this system allows the restorative dentist, the surgeon, and the dental laboratory to partic-ipate as equal members in the diagnosis and treatment planning of implant cases by providing each team member with an accurate 3-D rendering of the treatment site developed from CT scan data. The computer-based rendering enables the restorative dentist, surgeon, and dental technician to see the alveolar bone that is available for implant placement and its proximity to the maxillary sinus. In the authors’ experience, an optimal emergence profile, as well as adequate lip support and tongue room (for acceptable phonics), can also be assured as the implant is placed virtually.
After the optimal implant positioning is determined based on the clinician’s experience, a surgical template is produced that shows the exact position of the implants to be placed. By using special drills with depth stops that fit the surgical template and following the published protocol, the need to create a surgical flap is elim-inated. The use of a flapless surgical procedure dramatically reduces the patient’s concerns about discomfort and shortens the healing time. Once the implant(s) have been placed, a temporary or permanent prosthesis can be connected immediately, providing the patient with im-mediate restoration of dental function (referred to as Nobel Biocare Teeth-in-an-Hour™).
The NobelGuide system can be used when placing a single implant, restoring an edentulous quadrant, or reconstructing an entire jaw. Per the published protocol, NobelGuide is not currently indicated for situations where extraction is followed by immediate implant placement.
The Restorative Consultation
Successful use of the NobelGuide system begins with the restorative consultation. When failing teeth have been under joint restorative and periodontal recall for years, the decision to extract the teeth and replace them with implants is never taken lightly. Among the factors that must be considered are the:
- patient’s concerns;
- short- and long-term prognoses for the affected teeth;
- patient’s present and future esthetic appearance;
- likelihood of the need for future major bone-grafting procedures;
- present and future functional occlusion;
- opposing occlusion and biting forces;
- significant medical history and the effect of inflammation as a possible causative factor; and
- likelihood of preventing future bone loss by placement of implants.
The decision to use implants to restore an edentulous area is usually easier, particularly when the implants can be placed in a minimally invasive flapless surgery, and the patient can go home with a temporary or permanent prosthesis.
Use of the NobelGuide System
Once the decision has been made to restore lost or failing teeth with implants and the failing dentition has been extracted, successful use of the published NobelGuide protocol begins with the restorative dentist designing an ideal prototype of the final restoration. The patient should feel like a partner in this process, helping to define the final restorative outcome. The restorative components include:
- tooth exposure when smiling and talking;
- shape and size of the teeth;
- amount of facial and lip support; and
- tongue room available for adequatephonics.
The acrylic prototype enables the patient and the restorative dentist to assess all the aspects of the restoration that ultimately will be created: the appearance of the teeth, the amount of lip and face support, and the tongue space and phonics. As final ridge healing occurs, the prototype can be relined and adjusted as necessary.
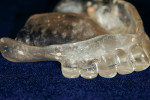
Once the patient and all members of the dental team are satisfied that an ideal prototype has been created, a bite registration is made. Six to eight gutta-percha radiographic markers are then added to the prototype prosthesis, using a #6 round bur and drilling to a depth of 1 mm (Figure 1). Placement of the radiographic markers according to the published protocol enables the prototype prosthesis to be used as a radiographic guide. Later the NobelGuide Procera® software will refer to the position of the markers to ensure that the prosthesis is properly aligned in relation to the bone.
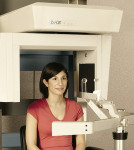
At the diagnostic imaging center, the bite registration is used to position the prosthesis properly in preparation for the CT scan. With the patient biting evenly and firmly, a scan is taken (Figure 2). This can be accomplished using either a cone-beam scanner or a multi-slice scanner.
The protocol requires that a second CT scan of only the prototype prosthesis is then taken. This is necessary because when the Procera software adjusts the density of the first scan to make the alveolar bone visible, the plastic of the prototype will be invisible—except for the six or eight gutta-percha markers. The software adjusts the second scan so that the shape of the prosthesis is captured. Both files are saved to a CD and imported into the NobelGuide software, which then precisely aligns the image of the prosthesis with that of the surgical site, using the gutta-percha markers as reference points.
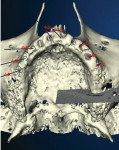
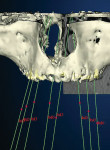
The resulting image provides a clinical view of the bone (Figure 3 and Figure 4) in relationship to the prototype prosthesis. Having such a view allows the surgeon to determine precisely where the implant(s) should be placed in order to obtain the optimal anchorage in the bone and provide the best support for the ultimate prosthesis (Figure 1). Dentists often discover that sufficient bone is available to allow for implant placement without the need for any augmentation. Alternatively, the scan may conclusively demonstrate that grafting is unavoidable. In such cases, a new prosthetic prototype can be constructed after the grafting has been carried out and healed.
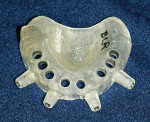
Once the ideal implant placement has been determined, a virtual rendering of the final surgical template is created by the Procera software. This template is ordered electronically and manufactured by Nobel Biocare (Figure 5). It is delivered to the dental laboratory for creation of master casts, articulation, creation of a surgical index (a special bite registration to be used during surgery), and a provisional or definitive restoration.
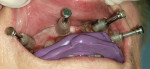
On the day of surgery, the surgical template is positioned using the surgical index and secured by means of guided anchor pins (Figure 6, Figure 7, Figure 8). Implant placement is carried out according to protocol in a completely flapless procedure, developing the osteotomy to perfectly accommodate each implant.
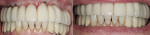
The premade restoration is placed, delivering both an esthetic and functional result (Figure 9 and Figure 10). The restoration placed at this point may be either provisional or definitive, depending upon the personal preference of both the surgeon and the patient.
Discussion
Although the NobelGuide system allows the implant team to plan treatment entirely on the computer, an alternative approach is available. When excellent bone width and height are available and conventional x-rays and mapping techniques (panoramic, bitewing, palpation, bone calipers, etc) reveal no contraindications, planning can be carried out on a stone model, from which the laboratory can create both a surgical template and a prosthetic solution. The same NobelGuide published surgical protocol and instrumentation can then be used to assure placement predictability and accuracy while carrying out a flapless surgery and delivering the prosthesis immediately.
Whether the surgery is planned conventionally or on the computer, it is not necessary to place the restoration at the time of surgery. However, a substantial body of scientific literature has demonstrated that immediate function after implant placement is a safe and predictable option.1-10
Nobel Biocare’s Teeth-in-an-Hour concept takes the approach of immediate function even further. Based on 10 years of research in cooperation with the Katholieke Universiteit Leuven, the Teeth-in-an-Hour concept received FDA clearance in 2004.11 In 2005, a 1-year report on 184 implants placed in 27 patients with totally edentulous maxillas showed a 100% implant-survival rate.12 This compares with published studies on complete maxillas using conventional early/immediate loading techniques that have shown survival rates ranging between 93.4% and 99%.13-16
Although the NobelGuide system makes implant reconstruction faster than ever, certain conditions are required to ensure that both the CT scan and the ultimate outcome are successful. These include:
- use of a multi-slice CT scanner with a 0.3-mm to 0.5-mm reconstruction interval or a cone-beam CT scanner with a 0.3-mm to 0.5-mm voxel size.17 Scans taken with a 1-mm reconstruction interval will not work properly with the software.
- proper fabrication of the radiographic guide. The gutta-percha markers should be placed 1 mm deep, and the guide should fit the soft tissue ideally. No metal component should be incorporated. Similarly, the use of any hard reline material or denture adhesive will be indistinguishable on the CT scan as gum tissue, providing a misleading image. Use of any such material should thus be avoided.
- proper positioning of the radiographic guide. Use of the bite registration should help to ensure this, though some implant teams find that having a staff member accompany the patient to the scan provides additional reassurance that both the bite registration and radiographic guide will be positioned correctly. Incorrect positioning will result in misplacement of the implants. Having an in-office CT scanner provides another approach to ensuring that the imaging personnel are properly trained in the NobelGuide scanning protocol.
- properly trained staff, including everyone from the front office personnel through the surgical assistant.
- a dental laboratory trained in NobelGuide procedures.
- NobelGuide Procera diagnostic and planning software.
- a surgeon who is proficient with the NobelGuide Procera software.
- consistent teamwork between the restorative dentist, surgeon, and laboratory.
Conclusion
NobelGuide is a treatment planning and surgical implementation system that en-ables the implant team to transfer extraoral planning into the mouth with accuracy and ease. The system shows the team the exact position and depth of the implants before surgery. At the time of surgery, placement of the implant, abutment, and restorative crown or bridge all occur during the same procedure.
The ease, safety, predictability, convenience, and superior esthetic results provided by this approach are highly appealing to patients. Other benefits include the lack of any healing time required prior to functioning and the ability to intimately experience what the end result will look like long before surgery, and to refine that result if necessary. Avoidance of long, uncomfortable, and costly bone-grafting procedures is another factor involved in positively influencing treatment acceptance.
Acknowledgment
The restorative dentistry presented in this article was performed by Dr. Jeffrey S. Ingber. Photography by Roman Drapatsky: Web design, Photography.
References
1. Scortecci G. Immediate function of cortically anchored disk-design implants without bone augmentation in moderately to severely resorbed completely edentulous maxillae. J Oral Implantol. 1999;25(2): 70-79.
2. Babbush CA. Provisional implants: surgical and prosthetic aspects. Implant Dent. 2001;10(2): 113-120.
3. Glauser R, Ree A, Lundgren A, et al. Immediate occlusal loading of Branemark implants applied in various jawbone regions: a prospective 1-year clinical study. Clin Implant Dent Relat Res. 2001;3(4): 204-213.
4. Lozada JL, Ardah AJ, Rungcharassaeng K, et al. Immediate functional load of mandibular implant overdentures: a surgical and prosthodontic rationale of 2 implant modalities. J Oral Implantol. 2004;30(5): 297-306.
5. Locante WM. Single-tooth replacements in the esthetic zone with an immediate function implant: a preliminary report. J Oral Implantol. 2004;30(6):369-375.
6. Ganeles J, Wismeijer D. Early and immediately restored and loaded dental implants for single-tooth and partial-arch applications. Int J Oral Maxillofac Implants. 2004;19(Suppl):92-102.
7. Degidi M, Piatelli A. Comparative analysis study of 702 dental implants subjected to immediate functional loading and immediate nonfunctional loading to traditional healing periods with a follow-up of up to 24 months. Int J Oral Maxillofac Implants. 2005;20 (1):99-107.
8. Villa R, Rangert B. Early loading of interforaminal implants immediately installed after extraction of teeth presenting endodontic and periodontal lesions. Clin Implant Dent Relat Res. 2005;7(Suppl 1): S28-S35.
9. Becker W, Wong J. Early functional loading in the fully edentulous mandible after mandibular resection and reconstruction due to an ameloblastoma: case report. Clin Implant Dental Relat Res. 2003:5(1):47-51.
10. Lee CYS. Immediate load protocol for anterior maxilla with cortical bone from mandibular ramus. Implant Dent. 2006;15(2):153-159.
11. Data on file. Nobel Biocare. Yorba Linda, CA.
12. van Steenberghe D, Glauser R, Blomback U, et al. A computed tomographic scan-derived customized surgical template and fixed prosthesis for flapless surgery and immediate loading of implants in fully edentulous maxillae: a prospective multicenter study. Clin Implant Dent Relat Res. 2005;7(Suppl 1): 111-120.
13. Balshi SF, Wolfinger GJ, Balshi TJ. A prospective study of immediate functional loading following the Teeth in a Day protocol: A case series of 55 consecutive edentulous maxillas. Clin Implant Dent Relat Res. 2005;7:24-31.
14. Malo P, Rangert B, Nobre M. All-on-Four immediate-function concept with Branemark System R implants for completely edentulous maxillae: a 1 year retrospective clinical study. Clin Implant Dent Relat Res. 2005;7(Suppl 1):S88-S94.
15. Olsson M, Urde G, Andersen JB, et al. Early loading of maxillary fixed cross-arch dental prostheses supported by six or eight oxidized titanium implants: Results after 1 year of loading, case series. Clin Implant Dent Relat Res 2003;5(Suppl 1):81-87.
16. Ostman PO, Hellman M, Sennerby L. Direct implant loading in the edentulous maxilla using a bone density-adapted surgical protocol and primary implant stability criteria for inclusion. Clin Impl Dent Relat Res 2005;7(Suppl 1):S60-S69.
17. NobelGuide™ Procedures and Products Concept Manual #16161. Data on file. Nobel Biocare, Yorba Linda, CA.
About the Authors
Louis Rose, DDS, MD
Clinical Professor of Periodontics
University of Pennsylvania School of Dental Medicine
Philadelphia, Pennsylvania
Private Practice
Philadelphia, Pennsylvania
Howard Fraiman, DMD
Assistant Clinical Professor of Preventive and Restorative Sciences
University of Pennsylvania School of Dental Medicine
Philadelphia, Pennsylvania
Private Practice
Philadelphia, Pennsylvania
Jeffrey S. Ingber, DDS
Private Practice
Philadelphia, Pennsylvania