Replacement Choices for the Worn-Out Amalgam Restoration
Michael A. Mcbride; James F. Simon
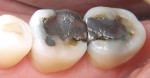
Not many years ago, the choices for replacement of a large amalgam (Figure 1) were relatively simple because the choices were limited. Now there are many more choices and the patient demand for esthetics, as well as health issues, are eliminating some former choices. Many patients today desire metal-free esthetic restorations. The dental professional desires to maintain as much healthy tooth structure as possible while maintaining the vitality of the pulp. Sometimes this can lead to a conflict in the ideal treatment for the tooth. The potential replacement choices will be discussed with the benefits and disadvantages of each highlighted.
Dental amalgam has many advantages when used as a restorative material. It has a high compressive strength, excellent wear characteristics, is easier to use than other materials, is less technique-sensitive (especially in unfavorable conditions), and has excellent long-term results. The causes of postoperative sensitivity with amalgam are well understood and usually transient in nature. Of the long-term restorative materials, dental amalgam is the least time-consuming to place and has the lowest overall cost.3
Dental amalgam is not the perfect replacement material because it has some disadvantages. Whal et al published data showing that there was no significant difference in the prevalence of cusp fracture rates in amalgam-restored teeth vs composite-restored teeth in subjects ages 18 through 54 years.4 Some of the problems with amalgam are that it is not tooth-colored (although this becomes an advantage when removal of the amalgam is necessary), it does not bond to tooth structure (but can be bonded using a separate step), and it contains mercury, which may be more of a hazard to the dental staff and to environmental concerns than to the patient. The primary problem with amalgam is that it is less conservative in its preparation requirements because of the need to remove more tooth structure during preparation for mechanical retention and resistance. The fact that it cannot be repaired easily makes it a less desirable material.
Composite
Composite is now used in more than 95% of all anterior direct restorations and in 50% of all posterior direct restorations.5 This would mean that, as the choice of composite for the replacement material for a large amalgam, a composite would often be considered. This could be problematic for the patient in the long run because of the physical characteristics of the material and difficulties in the bonding steps leading to postoperative sensitivity issues and potential for extensive recurrent decay underneath the subsequent composite restoration. Many patients are requesting—in some cases demanding—that the replacement be done with a tooth-colored material, but is this the best choice?
Composite materials should be considered as the first choice for initial, small carious lesions; however, the replacement of large amalgams can lead to problems for the patient and disappointment for the dentist. The large amalgam preparation was not designed with bonding in mind. It was designed with the need for retention and resistance. Ideally, composite should be used when all the margins are in enamel. This is not usually the case when replacing a large amalgam because the secondary decay usually extends the margins of the new preparation beyond enamel, especially interproximally.
One of the primary shortcomings of all composite materials is the characteristic of polymerization shrinkage upon curing. The larger the restoration, the greater the polymerization shrinkage of the composite (2.6% to 7.1% by volume),6 because there is a greater chance that the restoration margins will lie beyond the enamel surface, and there will be a greater potential for microleakage and recurrent decay. Shrinkage stresses negatively influence the mechanical properties and marginal integrity of the restorative material.7 There are numerous methods to attempt to control these stresses, such as layering the material, use of polymerization tips, inserts, and soft-start polymerization. Any or all of these methods should be used for these larger direct composites.
In the final analysis, the ideal indications for composite use in the posterior are limited. The criteria should include: centric stops on tooth structure rather than on composite material; patients who exhibit little signs of bruxing or clenching; the ability to isolate the area with a rubber dam; the faciolingual width should be restricted to no more than one third of the intercuspal distance;8 and all the cavosurface margins should be on enamel.9 If the base of the proximal box extends into root dentin, it is extremely difficult, if not impossible, to ensure close marginal adaptation and to obtain a perfect marginal seal, even with the use of current dentin bonding agents.10 When replacement restorations fall outside of these criteria, alternative materials and techniques should be considered.
Indirect Restorations Tooth — Colored
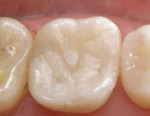
Indirect inlays or onlays made of composite or porcelain make ideal replacement restorations for these large amalgam restorations. They offer the patient the esthetics of a tooth-colored restoration while conserving tooth structure (Figure 2). The preparation for these restorations is not conservative because enough tooth structure must be removed to give strength to the material, but it is more conservative than a crown because it maintains as much healthy tooth structure as possible. Eventually, if necessary, it can always be converted to a crown in the future if further deterioration of the tooth occurs.
The indirect restoration allows for improved marginal fit and strengthening of tooth structure because the restoration is bonded into place. Other advantages include: better control of contacts, contours, anatomic form, color matching, wear resistance, and, because the polymerization shrinkage takes place outside the mouth, less stress on the bond to tooth structure. The preparation is less traumatic to the tooth and the surrounding tissue because it is more conservative and the margins can be kept supragingival in many instances.
The indirect restoration does have some disadvantages. It usually takes longer to complete because it may mean an impression, a temporary, and two appointments if it is fabricated by the laboratory. Thus the cost to the patient is increased because of the additional time and the laboratory bill. It is a technique-sensitive restoration because it is bonded to place and all the steps for proper bonding must be followed. The porcelain restoration does not allow for the possibility of intraoral repair. If some part were to fracture, the entire restoration would need to be removed and replaced with another restoration.
This problem has been somewhat addressed with the chairside computer-assisted design/computer-assisted manu-facturing (CAD/CAM) unit from Sirona Dental (CEREC® 3D, Sirona Dental Systems, Charlotte, NC) and the newly introduced unit from D4D Technologies (E4D Chairside CAD/CAM System, D4D Tech-nologies, Richardson, TX). The CEREC unit has been in service for over 20 years and has many long-term studies to support its use.11 The survival probability of a CEREC-generated restoration has been reported to be approximately 97% for 5 years and 90% for 10 years.11 The disadvantage of this type of restoration is the large initial investment for the equipment and the initial learning curve for the use of the computer program and the demands for specific preparation criteria. Once the criteria and the computer program have been mastered, a very well-fitting, long-lasting restoration can be delivered to the patient in one appointment that is both conservative and esthetic.
Partial Coverage Indirect Restorations — Gold
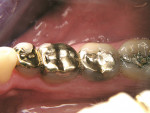
For centuries, an alternative to complete-coverage restorations has been the partial gold coverage restoration. This type of restoration was the standard of care for conservative, high-quality, long-term restorations12 (Figure 3). These would include gold inlays, onlays, and partial veneer crowns. Gold restorations have excellent mechanical and biocompatibility properties and do not deteriorate over time. The mechanical properties of gold include proper stiffness, strength, ductility, hardness, and coefficient of expansion for a long-term dental restoration.13 Some of the properties of gold described in one article12 include: gold does not corrode, leaving the tooth discolored as amalgam often does; it has nearly an identical wear factor as a natural tooth; it protects and supports the remaining tooth structure even when placed in a thin layer; if properly placed, the margins are almost imperceptible; the restoration exhibits a high degree of polishing and finishing, which results in less plaque retention; and it enables the reproduction of normal tooth anatomy and esthetics.
Although there are a few articles in the literature that do not show support for the longevity of gold inlays and onlays,14,15 the literature for the most part has supported the longevity of intra- and extra-coronal gold restorations.16-19 A more recent article20 reported the longevity results of 1,314 cast-gold restorations placed in 114 patients by one practitioner. All restorations were cemented with zinc phosphate cement. The survival rate ranged from 97% at 9 years to 94.1% in place for more than 40 years. There was an overall failure rate of 4.6%.
Gold inlay indications are basically the same as those of medium-sized amalgam restorations. They are not indicated for restoration of small carious lesions. Amalgam or composite are better suited in these instances. Because gold inlays are more expensive than amalgam or composite restorations, they need to be placed in patients who have better oral hygiene. The teeth restored with this type of restoration should have sufficient bulk to provide adequate resistance and retention form. They are not for use where the missing tooth structure is greater than one third of the buccal-lingual cusp tip distance. Nor are they generally indicated in mesial-occlusal-distal situations because of in increased risk of cuspal fracture.
Gold onlays have the same mechanical and biologic benefits of gold inlays plus the added advantage of providing cuspal coverage for teeth that have a more extensive loss of tooth structure. Before bonded ceramic restorations became widely available they were seen as one of the most conservative treatment options available to dentists.
Many dentists would agree that if it were not for esthetic considerations, gold restorations would still be the treatment option of choice. If a tooth to be restored meets the indications for a gold restoration, oftentimes it can still be prepared in a manner so that the restoration is not visible. This is especially true in the maxillary posterior region.
Patients who desire long-term and esthetic restorations should still consider gold inlays and onlays when the display of the gold can be minimized. Gold restorations have the potential to provide unparalleled long-term function and tissue compatibility.
Indirect Crown Restorations
If a tooth has had extensive proximal and facial-lingual caries, a conservative restoration may not be indicated. In these cases a complete crown may be indicated. The crown may be metal-ceramic, all-ceramic, or full cast, depending on esthetic considerations. The tooth should be relatively intact with sufficient coronal structure to support the restoration. This is particularly important in the incisal and occlusal areas where the porcelain thickness should not exceed 2 mm.21 Full-coverage restorations have better retention than partial coverage cast restorations, and they are generally required to serve as a retainer for a fixed partial denture. Although full-coverage restorations will always be the treatment of choice for extensively damaged teeth, they should not be routinely used in place of a more conservative treatment option simply because they are easier to place than partial coverage restorations.
Conclusion
The dentist and the patient have many choices for the replacement of an old, defective amalgam restoration. The cost/benefit ratio of each choice must be weighed against the desires of the patient and the correct treatment for the tooth. Sometimes, compromises must be made to satisfy these desires; however, the choice must be made after having considered the advantages and disadvantages of each material and based on sound clinical judgment. Maximum retention of healthy tooth structure with the most conservative restoration possible should be the primary concern in any decision.
Disclosure
The author is a consultant for Sirona Dental Systems.
References
1. Yip HK, Li DK, Yau DC. Dental amalgam and human health. Int Dent J. 2003;53(6):464-468.
2. Joshi A, Douglass CW, Kim HD, et al. The relationship between amalgam restorations and mercury levels in male dentists and nondental health professionals. J Public Health Dent. 2003;63(1): 52-60.
3. Roberson TM, Heymann HO, Swift EJ. Art and Science of Operative Dentistry. 5th ed. Philadelphia, PA: Mosby; 2006:341.
4. Wahl MJ, Schmitt MM, Overton DA, et al. Prevalence of cusp fractures in teeth restored with amalgam and with resin-based composite. J Am Dent Assoc. 2004;135(8): 1127-1132.
5. Stein PS, Sullivan J, Haubenreich JE, et al. Composite resin in medicine and dentistry. J Long Term Eff Med Implants. 2005;15(6):641-654.
6. Feilzer AJ, De Gee AJ, Davidson CL. Curing contraction of composites and glassionomer cements. J Prosthet Dent. 1988;59(3): 297-300.
7. Choi KK, Ryu GJ, Choi, SM, et al. Effects of cavity configuration on composite restoration. Oper Dent. 2004;29(4): 462-469.
8. Ferracane JL. Using posterior composites appropriately. J Am Dent Assoc. 1992;123(7):53-58.
9. Summitt JB, Robbins JW, Hilton TJ, et al. Fundamentals of Operative Dentistry. 3rd ed. Chicago, IL: Quintessence Books; 2006:289-339.
10. Van Noort R. Introduction to Dental Materials. 2nd ed. Philadelphia, PA: Mosby; 2002:118.
11. Fasbinder DJ. Clinical performance of chairside CAD/CAM restorations. J Am Dent Assoc. 2006;137: 22S-30S.
12. Gusa R, Voda A, Fichtner G. Cast gold restorations for predictable clinical longevity. Signature. 8(2).
13. Van Noort R. Introduction to Dental Materials. 2nd ed. Philadelphia, PA: Mosby; 2002:222.
14. Allan DN. The durability of conservative restorations. Br Dent J. 1969;126(4):172-177.
15. Crabb HS. The survival of dental restorations in a teaching hospital. Br Dent J. 1981;150:315-318.
16. Bentley C, Drake CW. Longevity of restorations in a dental school clinic. J Dent Educ. 1986;50(10):594-600.
17. Mjor IA, Medina JE. Reasons for placement, replacement, and age of gold restorations in selected practices. Oper Dent. 1993;18(3):82.
18. Stoll R, Sieweke M, Pieper K, et al. Longevity of cast gold inlays and partial crowns—a retrospective study at a dental school clinic. Clin Oral Investig. 1999;3(2):100-104.
19. Studer SP, Wettstein F, Lehnar C, et al. Long-term survival estimates of cast gold inlays and onlays with their analysis of failures. J Oral Rehabil. 2000;27:461-472.
20. Donovan T, Simonsen RJ, Guertin G, et al. Retrospective clinical evaluation of 1,314 cast gold restorations in service from 1 to 52 years. J Esthet Restor Dent. 16(3):194-204.
21. Rosenstiel SF, Land Fujimoto J. Contemporary Fixed Prosthodontics. 4th ed. Philadelphia, PA; Mosby Elsevier; 2006:269.
About the Authors
Michael A. McBride, DDS
Associate Professor
Department of Restorative Dentistry
University of Tennessee
College of Dentistry
Memphis, Tennessee
James F. Simon, DDS, MEd
Professor
Department of Restorative Dentistry
University of Tennessee
College of Dentistry
Memphis, Tennessee