New Luting Agents Offer New Clinical Advantages
Karl F. Leinfelder, DDS, MS; Douglas A. Terry, DDS; Chuck Maragos, CDT
A new class of luting agents has recently been added to the profession. Identified as "self-etching" or "self-adhesive" cements, these materials offer a number of clinical advantages over their predecessors. It is the purpose of this article to describe the treatment of a patient by fabricating and placing a ceramic restoration. The luting system used in this case was a relatively new product identified as Breeze™ Self-Adhesive Resin Cement by Pentron Clinical Technologies, LLC (Wallingford, CT).
Clinical Procedure
A 42-year-old female patient presented with sensitivity on the maxillary right first molar. After thorough examination and a self-assessment, the patient requested the replacement of the existing ceramo-metallic crown with a restoration that provided a natural appearance. Before initiating the restorative procedure, preoperative considerations included: radiographic review, occlusal analysis, a diagnostic wax-up, restorative material selection, a custom shade selection, and shade diagram. Shade selection and a photographic comparison were performed before initiation of treatment to prevent an improper shade assessment from tooth dehydration. Upon removal of the existing crown, caries was removed, a composite buildup was placed, and the preparation was modified. After tooth preparation, a photographic shade comparison of the underlying dentin substrate was performed before provisionalization. The specific shade tabs, comparative photographs, and diagrams were provided to the technician so that an exact reference could be used during the fabrication of the restoration. The restorative material selection by the clinician and ceramist was based upon a review of these photographs. The decision was made to use a zirconium CAD/CAM generated substructure (ie, Procera®, Nobel Biocare USA Inc, Yorba Linda, CA) to disguise the discoloration of the underlying dentin substrate.
A provisional restoration was fabricated from the diagnostic wax-up using a custom acrylic matrix technique with an auto-curing acrylic resin. This interim restoration not only provided protection and support to the prepared tooth, but preserved the position, form, and color of the gingiva, maintaining periodontal health while the definitive restoration was being fabricated.
Adhesive cementation of an indirect restoration is the final process in a sequence of precisely orchestrated and repeated manipulations of instruments and restorative materials.1 This is the most complex, multifaceted procedure in dentistry because of the number of variables that can affect the success and long-term outcome of the restoration. The selection of luting cement is an essential part of this procedure and requires a material that provides optimal retention during function, favorable esthetics, adequate working time, ease of removal and cleanup, and a durable bond with good marginal adaptation of the luting material to the restoration and the tooth. Furthermore, in creating optimal esthetic harmony with the surrounding dentition, the color of the underlying substrate and restorative cement can directly influence the appearance of the final restoration.
The degree of translucency/opacity and the thickness of the ceramic material can also influence final esthetics. When the ceramic material is translucent and/or has a thin dimension, an opaque cement can have a negative influence on the value. Using a translucent cement with a high chromatic substrate and/or a ceramic material that is translucent or thin in dimension can have the same negative effect on esthetics. In this case, the selection of the zirconia substrate negates the esthetic consideration for the color of the substrate and cement because of the inherent opacity of the restorative material. However, other factors that should be considered include retention, durability, and longevity, which can all be influenced by preparation design, cement type, and surface preparation of the tooth and restoration.
A principal determinate in the long-term success of adhesive restorations relies on the strength and durability of the interface between the resin cement and the bondable surface of the restoration.2 Thus, it relies not only on an adequate preparation, but on the conditioning of the bonding surfaces involved.
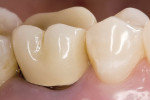
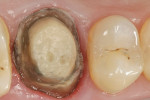
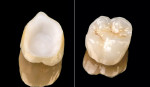
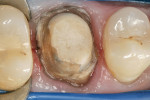
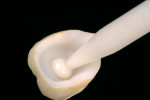
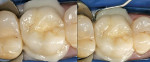
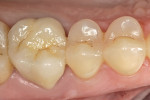
There are various pre-cementation protocols recommended by the manufacturers of different ceramic systems. The author’s standard cementation protocol for zirconium includes microetching the inner surface of the restoration with CoJet™ sand (3M ESPE, St. Paul, MN) followed by a silane application. The microetching of highly crystalline ceramics such as zirconium with a tribochemical silica coating creates binding sites for the silane molecules, while the silane provides wettability and a chemical coupling with the methacrylate-based cements. The clinical procedure presented here illustrates this cementation protocol using a self-adhesive resin cement system (Breeze) (Figure 1; Figure 2; Figure 3; Figure 4; Figure 5; Figure 6; Figure 7; Figure 8).
Discussion
The growing interest in "self-etching" or "self-adhesive" luting agents as the material of choice for many clinicians is based in part on simplicity. In essence, the mixed cement is injected onto the internal surfaces of the restoration as well as onto the preparation itself. Other than washing and air dispersing the prepared surfaces, no other treatment, including acid-etching or use of a dentin bonding agent, is required. Even though the procedure is simple, moderately high bond strengths are attained with no postoperative sensitivity.
The latest self-adhesive cement has just been marketed. Identified as Breeze Self-Adhesive Resin Cement, this luting agent is characterized by a number of interesting properties and composition. Unlike many of its predecessors, its composition is a bit more complex. In essence it consists of bis-GMA, UDMA, HEMA, and 4-META. It also contains carboxylated methacrylates. The filler is tri-modal, consisting of silane-treated bariumborosilicate glass, glass ionomer, and colloidal silica. The filler loading is 65% by weight and 40% by volume. The combination of this material’s resin chemistry and particle content imparts a number of important properties.
First of all, the shear bonding strength of Breeze to dentin is 18.2 MPa, whereas to enamel it is 10.9 MPa. In addition, the bond strength to zirconium is 11.3 MPa and 19.8 MPa to gold-based alloys. Finally, the shear bond strength to Rexillium III base-metal alloy is 19.4 MPa. Bonding to the various substrates can be attributed to the 4-META and the carboxylated methacrylates.
The radiopacity is quite high at 300%, that of a 1-mm thick aluminum standard. This value permits ready detection of the cementing medium radiographically. The mean particle size is 1.2 µm while the film thickness is 25 µm. Finally, the flexural strength is 94 MPa, whereas the flexural modulus is 6.1 MPa.
The delivery system for Breeze consists of a 1:1 dual syringe with an auto-mix tip. The material may also be hand mixed, but setting time will be extended. The available shades consist of the following: A2, Translucent, and Opaceous White. Breeze exhibits a gelation time of 1.5 to 3 minutes and a setting time of 3.5 to 4 minutes when the auto-mix tips are used. Indications for use of this self-adhesive agent include metal and ceramic, cementable all-ceramic and metallic crowns, bridges, inlay/onlays, posts, and indirect composite resin restorations.
Disclosure
Dr. Leinfelder is a consultant for Pentron Clinical Technologies.
References
1. Donovan TE, Cho GC. Contemporary evaluation of dental cements. Compend Contin Educ Dent. 1999;20(3):197-220.
2. Hilton TJ. Posterior inlays and onlays. In: Schwartz JS, Summitt JB, Robbins JW. Fundamentals of Operative Dentistry: A Contemporary Approach. Carol Stream, Illinois: Quintessence Publishing; 1996:229-249.
About the Authors
Karl F. Leinfelder, DDS, MS
Adjunct Professor, Biomaterials Clinical Research
University of North Carolina
Chapel Hill, North Carolina
Professor Emeritus
University of Alabama School of Dentistry
Birmingham, Alabama
Douglas A. Terry, DDS
Adjunct Assistant Professor
Department of RestorativeDentistry and Biomaterial
University of Texas Health Science Center at Houston
Private Practice
Houston, Texas
Chuck Maragos, CDT
Laboratory Technician and Owner
Valley Dental Arts
Stillwater, Minnesota