A Primer on Cone Beam CT
Allan G. Farman; Claudio M. Levato; William C. Scarfe
Cone Beam Computerized Tomography (CBCT) is an application that is taking dentistry by storm. In a single rotation, CBCT provides precise, essentially immediate, and accurate three-dimensional (3-D) radiographic images. The data acquired by the scan can also be used for image guidance and to create 3-D epoxy models used for treatment applications. The significant advancements and applications provided by this technology do not compete with standard digital radiographic applications. Rather, CBCT is a complementary modality for specific applications.
CBCT IMAGE ACQUISITION
Cone-beam techniques use a single rotation in which the x-ray source and a reciprocating x-ray detector are attached by an arm and rotate around the patient’s head acquiring multiple basis projection images. It is also possible to fuse scans from more than one rotation in some cases. The field of view (FOV) determined by the area of interest is primarily dependent on the detector size and beam projection geometry. While FOV can be varied by the application of zoomed image reconstruction, this can reduce image resolution.
The number of projection images comprising the data set varies, depending on the system, and this number is determined both by the frame rate and the exposure cycle. The higher the frame rate, the more information that is available to construct the image; however, the signal-to-noise ratio of individual slices is also decreased. A number of units have variable exposure sequences and numbers of frames (Table 1).
CBCT ADVANTAGES
Because CBCT provides images of high contrasting structures well, it is highly suited for evaluating bone and teeth. Combined with the limitation of FOV, CBCT is almost perfectly positioned for dentistry. CBCT use in clinical practice provides a number of advantages compared to conventional CT. These advantages include beam limitation, reduced scan time, and rapid image display. Other advantages are discussed below.
Variable FOV
Collimation of the CBCT primary x-ray beam enables limitation of exposure to the region of interest. An optimal FOV can be selected for each patient based on disease presentation and the region designated to be imaged.
Submillimeter Resolution
CBCT units use megapixel solid state devices for x-ray detection providing a minimal voxel resolution between 0.09 mm and 0.25 mm isotropically, exceeding the highest grade multislice CT in terms of spatial resolution.
High-Speed Scanning
CBCT generally acquires all basis projection images in a single rotation, so scan time can be minimized. While faster scanning times usually mean less basis projections from which to reconstruct the MPR (multiplanar reformatting) images, motion artifact because of subject movement is reduced. Reconstruction times vary depending on FOV and scanning speed.
Dose Reduction
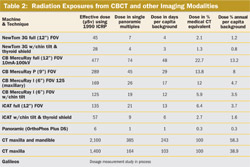
Reports indicate that the CBCT patient-absorbed dose is significantly reduced when compared to conventional CT (Table 2).1-3 The NewTom 3G system also has an automatic exposure control device which selects the starting intensity of the x-ray beam, depending on the size of the patient, and modifies the anodic current according to the density of the transversed tissues (maximum value, 15 mA). This reduces the patient-absorbed dose to approximately that of a film-based periapical survey of the dentition or 1 to 7 times that of a single panoramic image. Depending on bone density, a hospital fan-beam CT exposes the patient to 6- to 8-times CBCT exposure for one jaw and 15-times CBCT exposure when imaging both jaws.
Voxel Isotropy
Voxels are the smallest element of the 3-D x-ray image. They have a dimension of thickness as well as the height and width of two-dimensional (2-D) pixels. Voxel representation and, therefore, resolution are dependent on lateral slice thickness, determined principally by the matrix size of the detector and longitudinal slice thickness (body axis). CBCT uses a 2-D detector and the same high resolution is obtained in the longitudinal slice (body axis direction) and lateral slice (transverse direction). This voxel representation is known as “isotropic.” Because of this characteristic, coronal multiplanar reformatting (MPR) of CBCT data has the same resolution as axial data.
Real-Time Analysis and Enhancement
Reconstruction of CBCT data is performed natively using a personal computer. In addition, availability of software to the user is via direct purchase or “per use” license from the various vendors. As the original data is isotropic, it can be reorientated such that the patient’s anatomic features are realigned. Finally, the availability of cursor-driven measurement algorithms provides the clinician with an interactive capability for real-time dimensional assessment.
Display Modes Unique to Maxillofacial Imaging
CBCT units reconstruct the projection data to provide multiple coronal, sagittal, and axial MPR frames. Common to all standard viewing layouts are preset options providing display of coronal, sagittal, and axial MPR frames. Basic enhancements include zoom or magnification, window/ level, the capability to add annotation, and measurement algorithms. Some proprietary software is capable of advanced imaging processing functions such as:
- Selected MPR, such as linear oblique, useful for TMJ assessment, or curved oblique, providing a panoramic image.
- Transaxial/slice MPR including cross-sectional imaging provides sequential multislice images usually orthogonal to the panoramic MPR, which is useful in implant site assessment.
- Variable slice thickness adjustments for oblique MPR images permit production of undistorted plain radiograph projection-like images. One example is the creation of a cephalometric projection, either sagittally or coronally. This is developed by increasing the slice thickness of a mid-sagittal MPR plane to the width of the head (130 mm to 150 mm) to produce an image composed of the summated voxels. This functionality may potentially reduce the need for additional radiographic exposure. Oblique MPR images along the curve of the dental arch with slice thickness comparable to the in-focus image layer of panoramic radiographs (25 mm to 35 mm) can also be created individually to provide a panoramic radiograph customized for each patient. However, unlike conventional panoramic radiographs, these MPR images are undistorted and are free from projection artifacts. Panoramic images of layer thickness as narrow as 1 voxel measurement can also be produced using CBCT.
- The maximum intensity projection is a 3-D volume-rendering technique which is used to demonstrate high-intensity structures within volumetric data. At each pixel, the highest data value encountered along a corresponding viewing ray is depicted. In combination with oblique MPR and selection of wide slice thickness, this technique is capable of providing 3-D surface-rendered images.
- Surface- and volume-rendering algorithms are available to provide 3-D reconstruction and interactive presentation of data.
- Previously unavailable with analog film, image-enhancement algorithms are now able to optimize image appearance. While the diagnostic efficacy of the application of such algorithms is yet to be studied, preliminary investigations indicate that sharpening and edge filters show the greatest potential in refining anatomic structures for interpretation.
Reduced Image Artifact
CBCT projection geometry, together with fast acquisition time, results in a low level of metal artifact in primary and secondary reconstructions.
Variable Acquisition Modes
Many CBCT units are capable of variable-scanning FOVs capable of imaging the entire craniofacial complex or limiting FOV for specific diagnostic tasks (Table 1).
ORAL AND MAXILLOFACIAL IMAGING
CBCT technology has paved the way for the development of relatively small and inexpensive CT scanners dedicated for use in oral and maxillofacial imaging. The first commercial CBCT system for oral and maxillofacial imaging was the NewTom (Dent-X® Visionary Imaging, Elmsford, NY) that was approved by the Food and Drug Administration in April 2001 and is currently in its third generation as the NewTom 3G. Since that time, four additional systems have been approved (Figure 1; Table 1). Manufacturers’ Web sites (Table 1) provide numerous examples illustrating the value of CBCT in evaluating the position of impacted teeth, supernumerary teeth, maxillary sinus position (in reference to maxillary molars), mandibular canals, and lingual nerves. Other examples of this modality’s uses include implant planning, surgical assessment of pathology, and preoperative/postoperative assessment of craniofacial fractures. Diagnostic examples are illustrated in Figure 2 and Figure 3.
LASER MODELING
An important clinical application of CT and CBCT in the maxillofacial region is the production of laser-generated models. These are produced using a computer-driven process that creates precise 1:1 models using laser-polymerization of epoxy resin. A computer-controlled laser generates an ultraviolet beam, which travels across the surface of a vat of a photocurable liquid polymer. The laser draws each axial cross-section of the anatomy one layer at a time. The photovoltaic energy from the laser polymerizes the epoxy instantaneously. The cured cross-sectional layer is lowered into the vat of resin and the next layer is processed. Successive layers of the anatomy are built in increments until the model is completed. The models produced are used for presurgical planning of a number of complex maxillofacial surgical cases, including craniofacial reconstruction due to trauma, tumor resection, or syndrome deficiency, as well as for distraction osteogenesis and more widely for dental implants. The models provide the practitioner with a high level of confidence before he or she ever performs a surgical procedure and can reduce surgical and anesthetic time dramatically.
CONCLUSION
CBCT provides 3-D images that facilitate the transition of dental imaging from initial diagnosis to image guidance throughout the treatment phase. This technology provides increased precision, lower doses, and lower costs when compared to medical fan-beam CT. It provides the third dimension on dental imaging and is extending dental imaging from diagnosis to image guidance of operative and surgical procedures.
Systems average around $200,000. This is affordable for busy implant, oral surgery, or orthodontic offices, but access for other practitioners is possible through imaging centers and university-based maxillofacial radiology clinics. It is possible for the referring practitioner to interact with the images on her/his personal computer given appropriate software. As image sets are digital, it is possible to refer cases to specialist services for the tissue volumes to be studied for unsuspected—or suspected—pathology.
This is a blossoming field which provides an ongoing income potential for a dentist who combines CBCT image-guidance with treatment. Image-guidance is an exciting advance that is already having substantial impact on the practice of dentistry.
DISCLAIMER
None of the authors have conflicts of interest related to the subject matter of this article.
REFERENCES
1. Ludlow JB, Davies-Ludlow LE, Brooks SL. Dosimetry of two extraoral direct digital imaging devices: NewTom cone beam CT and Orthophos Plus DS panoramic unit. Dentomaxillofac Radiol. 2003;32(4): 229-234.
2. Ludlow JB, Davies-Ludlow LE, Brooks SL, Howerton B. Dosimetry of 3 BCT units for oral and maxillofacial radiology. Paper presented at 15th International Congress of the International Association of Dento-Maxillo-Facial Radiology, Cape Town, South Africa, June 2005.
3. Ngan DC, Kharbanda OP, Geenty JP, Darendeliler MA. Comparison of radiation levels from computed tomography and conventional dental radiographs. Aust Orthod J. 2003;19(2): 67-75.
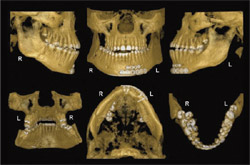 Figure 1 3-D reconstructed iCAT CBCT views of repaired fractured mandible with resulting malocclusion. Note the lack of scatter artifact form the surgical metallic support structures. 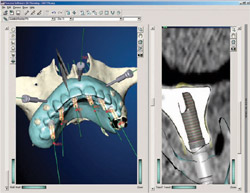 Figure 3 CBCT DICOM file data set used for image-guided implantology after being imported to Procera software. (Image courtesy of Nobel Biocare, USA, Yorba Linda, CA.) | 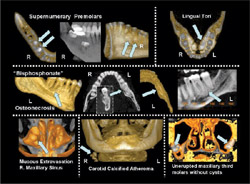 | ||||||
| Figure 2 Various conditions displayed by 3-D reconstructed iCAT CBCT reconstructed images. Top row left and center shows localization of mandibular supernumerary premolars (arrowed) lingual to the regular dentition; top right demonstrates sectional 3-D view of large mandibular tori (left side arrowed); center row demonstrates osteonecrosis with loss of left lingual cortical plate in molar region (arrowed) through osteonecrosis (3 years post-chemotherapy and bisphosphonate treatment for metastatic breast cancer); lower right demonstrates dome-shaped mucous extravasation phenomenon in right maxillary sinus; lower center shows carotid calcified atherosclerotic plaque (arrowed) as incidental finding in patient referred for implant planning (on questioning patient had prior history of left carotid endarterectomy); lower right demonstrates bilateral unerupted maxillary third molars without cystic involvement as proven by air-tissue boundary (arrowed). | |||||||
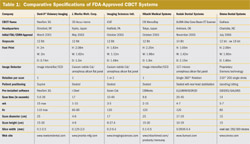 |  | ||||||
| Table 1 | Table 2 | ||||||
| |||||||




