A Relatively “Painless” Way to Avoid Pain
Nancy Andrews
Most dentists will agree that of all the services that can be performed for patients, eliminating the fear and pain associated with anesthesia would perhaps be at the top of the list, while also removing significant stress from clinical practice. Some clinicians, however, honestly think their injections are painless, explaining that patients never complain. Patients may not complain, but that may be because they do not expect a truly “painless” injection. The question is, can they learn to expect painless injections? A small percentage of patients do not consider injections painful irrespective of the technique used. A similarly small percentage of patients interpret all injections performed—regardless of the technique used—as excruciating. Most patients, however, fall somewhere in between, ranging from those who feel pain and hate or fear injections but tolerate them, to those who rarely feel pain and are generally relaxed and comfortable with injections. The purpose of this article is to present methods to move patients into the latter category.
THE IMPORTANCE OF PAINFUL INJECTIONS
Most undesirable reactions to injectable local anesthetics are a response to the act of injecting the drug, not the drug itself.1 Syncope and hyperventilation, possibly resulting in medical emergencies, are the most common psychogenic reactions.2 Pain associated with injections is attributed to needle insertion/manipulation and drug delivery/deposition in tissue.3 Dealing with fearful, anxious patients is the most commonly reported challenge in controlling pain.4
Fear of dental injections contributes to postponement of dental treatment. About half of patients questioned consider injections painful and are fearful of them. More than 50% of non-attending public have phobia of dental pain associated with dental injections, and 90% have at least mild anxiety about receiving an injection. Other factors that reduce patient acceptance of dental treatment are a dislike of prolonged numbness after treatment and uncomfortable numbness of patients’ lips and tongue.2
STRATEGIES TO REDUCE, BLOCK, OR MASK INJECTION PAIN
There are three aspects of injections that elicit pain: initial needle penetration, advancement of the needle to the injection site, and injecting the drug. There is also one “wild card”: fear, or preconceived beliefs about pain and/or risk of injections.
Applying a topical anesthetic before injection is the most popular way to control initial needle penetration pain. Conflicting study conclusions and anecdotal information on the effectiveness of topical gel in preventing needle insertion and manipulation pain suggests that topical gels can be effective, but the duration of action may vary from 5 to 40 minutes.5 Patient reactions to taste and the time spent waiting for the topical to take effect may be negative outcomes. Concerns about toxic sequelae and adverse effects related to the amounts of drug absorbed through the mucosa suggest that alternative means of injection pain control are desirable.
Transcutaneous Electrical Nerve Stimulation (TENS) devices are reportedly well accepted by some patients in lieu of topical anesthetics in clinical studies, but require additional time, may not be effective on phobic patients, and are less commonly used.3 Sharp needles have been shown to cause less pain and trauma than dull needles. Because it is common to give at least several successive injections, the very simple technique of changing the needle after two or three injections will reduce immediate and/or recovery pain.
Visual, auditory, and tactile stimulation is another technique for distracting the patient’s attention. Manually shaking the patient’s cheek is a crude method of creating such a pain-masking sensation and can be effective, but may be inconsistently so. While cheek shaking may effectively distract the patient’s attention, aggressive cheek shaking may leave the cheek sore or bruised.
Giving “slow” injections allows time for the anesthetic to precede the advancement of the needle and for more passive flow of the anesthetic through tissue, thereby reducing tissue tearing and associated pain. This technique is a pillar of virtually all clinical instruction strategies for manual anesthetic injections, but a slow injection may vary significantly between clinicians as well as in each clinician’s hands from one time to the next. Demanding schedules may also not always allow injections to be given slowly enough to completely avoid pain.
Electronically controlled devices meter out the anesthetic slowly, overcoming inconsistent hand pressure and variations in perception of time or pressure-resistance. If time allows, these devices have been shown to be consistently effective and increasingly popular. According to Dr. Stanley F. Malamed, professor of anesthesia and medicine at the University of Southern California School of Dentistry, “Any intraoral injection that a dentist finds uncomfortable for a majority of patients can be administered more comfortably using a computer controlled system.” 4 Patient perception of alternative technology designed specifically to reduce pain may also add a placebo effect with some benefit.
There are several electronic devices that employ microprocessors to control the volume and pressure of local anesthetic delivery. The Comfort Control™ Syringe (CCS) (Dentsply/Professional, York, PA; Figure 1) and the CompuDent™ (formerly the Wand™, Milestone Scientific, Livingston, NJ), both rely on slow anesthetic delivery to reduce pain.
CompuDent uses a floor foot pedal to initiate the flow of anesthetic through long tubing to the handpiece at a rate and pressure designed to be below the patient’s pain threshold. The handpiece is held in a pen grasp designed to facilitate greater tactile sense and control and easier rotation than the traditional syringe grasp. The pre-puncture technique incorporates the bevel of the needle on the tissue, the pressure of a cotton-tipped applicator applied to the end of the needle forcing anesthetic into the tissue, and then the slight rotation of the needle to pierce the tissue. The anesthetic pathway is developed by penetration and slight rotation of the needle through previously anesthetized tissue. Once the needle arrives at the injection site, the delivery of the anesthetic is below the patient’s pain threshold (Figure 2).
The CCS has a two-stage delivery, beginning at a slow rate, automatically increasing to a preselected rate after 10 seconds. Five injection rates are available.
Both electronically controlled devices are usually used with topical anesthetics. They both require less force, resulting in less needle deflection and easier needle rotation. Both devices require electrical outlets, and room for the control units. Methods that rely on slow anesthetic delivery are technique-sensitive, require more chairtime per patient, and therefore increase the cost of treatment. Despite the cost of these devices and time pressures many busy practitioners face, the value of removing or significantly reducing injection pain is worth the investment for many devoted customers.
THE GATE CONTROL THEORY
The brain’s ability to perceive only one sensation at a time gives rise to the strategy of causing a sensation other than pain that supersedes the sensations generated by the injection. Techniques or devices that create pressure or vibration have been shown to inhibit painful sensations if they stimulate the appropriate nerves prior to or at the same time as painful stimuli. The patient perceives only pressure or vibration because those sensations block the pain signal. The gate control theory refers to a physiologic phenomenon rather than a simple distraction, but the two may exist at the same time.
A mechanical device is available that performs this vibratory action very effectively and consistently. VibraJect® (ITL Dental, Irvine, CA) is a small battery-driven motor that vibrates at 10,000 cycles per minute and attaches to standard syringes with autoclavable clip-on motor brackets (Figure 3). The vibration feels slight to the operator, but is precisely designed to stimulate nerves so that the pain threshold is raised and the injection is imperceptible to most people. It snaps onto most syringes and requires virtually no extra time or space. Some clinicians hesitate to use such a device, because they consider the gate control theory an unproven idea, and view the technology as a simple distraction that might get in their way. Other concerns are that the vibration might affect the operator’s tactile feel or alarm the patient; however, motivated clinicians report overcoming these concerns quickly. When the VibraJect is used on traditional syringes the speed of the injection is controlled manually and slow injections are recommended. The VibraJect may also be used with the CompuDent for virtually undetectable injections, according to the manufacturer’s literature.6
The two sensory cells in the oral cavity most likely associated with the pain reduction phenomenon created by vibration like that generated by the VibraJect include free nerve endings and mechanoreceptors, or tactile nerves. Free nerve endings, which perceive temperature and pain, have no myelin sheath and respond with relatively low intensity and speed. Tactile nerves are larger, insulated with myelin sheaths, and respond with higher speed and intensity. These nerves transmit tactile sensations of pressure and vibration. The rapidly transmitted pressure and/or vibration messages reach the brain first, thereby preventing pain signals from being perceived.
CONCLUSION
Eliminating painful injections is worth considering—even if patients rarely complain. Fear of painful injections contributes to postponement of, and may reduce patient acceptance of, dental treatment as well as contributing to the stress of practicing dentistry. Giving comfortable injections is unquestionably a skill and a source of pride for those who have mastered it. Being able to depend on painless injections is appealing for obvious reasons, including the probability of attracting more patients.
DISCLOSURE
The author received grant and research support from VibraJect, LLC.
REFERENCES
1. Daublander M, Muller R, Lipp MD. The incidence of complications associated with local anesthesia in dentistry. Anesth Prog. 1997;44(4):132-141.
2. George M, Niessen L. Stop the pain—assessing patients’ anesthetic options for nonsurgical periodontal therapy. Woman Dentist Journal. 2005;3(5): 24-30.
3. Quarnstrom F, Bang-Pastore SH, Woldemicael R, Chen D. VibraJect VS. The Wand for the control of injection pain. Available at: https://www.itldental.com/Vibraject_vs_wand.php. Accessed September 26, 2006.
4. Goff S. Care with Comfort: DPR Exclusive Anesthesia/Sedation Survey. Dental Products Report. October, 2006:34-44.
5. Yagiela J. Safely easing the pain for your patients. Dimensions of Dental Hygiene. 2005;3(5):20-22.
6. VibraJect Web site: https://www.itldental.com. Accessed September 26, 2006.
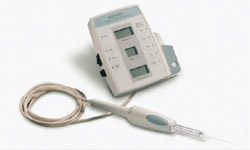 Figure 1 The Comfort Control Syringe (CCS). | 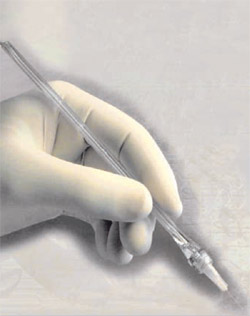 Figure 2 The Compudent System (Image courtesy of Milestone Scientific). | ||||||
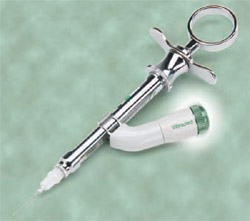 Figure 3 The VibraJect device. (Image courtesy of ITL Dental) | |||||||
| |||||||




