CAD/CAM Update: Technologies and Materials and Clinical Perspectives
Edward A. McLaren, DDS, MDC, and Lu Hyo, MDC
New CAD/CAM systems and technologies are being introduced to the dental marketplace at an ever-increasing rate. Most dental companies that are involved with restorative dentistry are already in the market or are in the process of developing a system or material for the CAD/CAM market. To give the reader an idea of how industry or business views the dental market, TDS, whose parent company makes Nike™ shoes, recently has entered the CAD/CAM market. Because of the growing confusion as to what these technologies are, what they will do, and, more importantly, what the clinical and laboratory guidelines for using these materials and techniques are, this article will address the important points of these topics.
CAD/CAM Technologies and Materials
Advances in dental ceramic materials and processing techniques, specifically CAD/CAM and milling technology, have facilitated the development and application of superior dental ceramics. CAD/CAM allows the use of materials that cannot be used by conventional dental processing techniques. Tightly controlled industrial ceramic processing can produce increased micro-structural uniformity, higher density, lower porosity, and decreased residual stresses. Such improvements have the potential to improve clinical predictability. CAD/CAM has become somewhat synonymous with zirconia, but systems are available that can machine any type of ceramics, ie, glass ceramics, interpenetrating (infiltration ceramics) materials, and solid-sintered monophase ceramics such as zirconia.
Problems and complaints with early systems focused on the machining accuracy of a particular system and not with the materials used with the system. Initial CAD/CAM systems produced restorations that had poor marginal fidelity with a general lack of internal adaption to the die as a result of low-resolution scanning devices and inadequate computing power. Technological advances in new systems and software development, coupled with specific clinical and laboratory techniques, have minimized or eliminated these problems so that marginal integrity and internal adaptation can be excellent.1
Recently, several strategies using different CAD/CAM processes and different materials that can manufacture all types of all-ceramic restorations—from inlays to onlays and from veneers to crowns to fixed partial dentures—have been developed.
CAD/CAM Technologies and Ceramic Materials
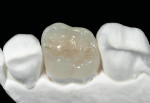
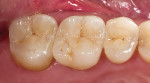
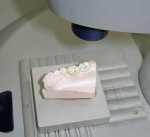
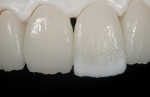
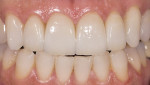
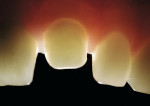
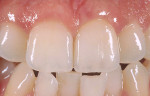
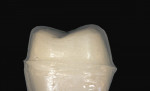
Glass ceramic materials are primarily a glass matrix material that has a fine, evenly distributed crystalline phase. These materials generally have translucency very similar to tooth structure, which makes them ideally suited for inlay and onlay applications (Figure 1 and Figure 2). They can be fabricated with a conventional power liquid technique or they can be industrially processed into a dense machineable block. Two companies fabricate materials in block form for the CEREC® inLab systems (Sirona Dental Systems, Charlotte, NC); VITA® (Vident™, Brea, CA) makes the Vitablocs® Mark II and VITA Bloc Esthetic Line materials and Ivoclar Vivadent® (Amherst, NY) makes the ProCAD and IPS e.max CAD materials. Glass ceramic materials are ideally suited for more conservative restorations (ie, inlays, onlays, and veneers). The only commercial system for generating inlays, onlays, and veneers is the CEREC inLab system (Figure 3). This system is an evolution from the dentist-based CEREC III (Sirona Dental Systems) system that is used for generating one-visit inlays and onlays. The system is a self-contained scanning and milling unit, and it is also designed to fabricate single copings and 3-unit fixed partial denture frameworks using interpenetrating phase compounds and zirconia. The dentist prepares inlays and onlays by standard techniques and sends the impression to the laboratory. The author’s experience with the system has shown that overflaring or beveling the preparation should be avoided. In the laboratory a die is generated and placed in the system and optically scanned (Figure 4). A virtual die is then displayed on the monitor and the restoration, with occlusion, is designed by the software. The die is then replaced with a glass-ceramic block of the desired material and the restoration is machined. The system will give excellent margins that are clean, confluent, noncorrugated, and nonbeveled and, ideally, a close to butt-joint margin preparation.
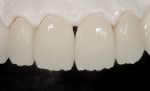
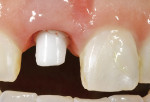
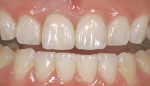
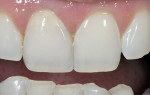
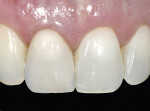
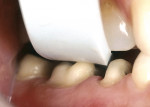
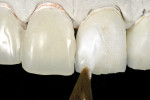
For veneers, the same glass ceramic materials are used. Dies are generated and scanned as in inlay/onlay applications. The veneers are machined from the appropriate shade and translucent material. For the best esthetics, the machined veneer is cut back in the laboratory in the incisal one third to one half and enamel or translucent porcelain is built up (or stacked) and then fired (Figure 5 and Figure 6). The benefit of veneers fabricated by this technique is that it is much safer to try them in intraorally because the ceramic is much tougher than veneers fabricated by conventional porcelain techniques. Also, if necessary, the restorations can be easily re-fired just like a conventional porcelain-fused-to-metal (PFM) or high-strength all-ceramic crown. The disadvantage of this technique is that the veneers need to be about 0.9 mm or thicker for optimal esthetics. The author uses veneers with this technique; the veneer thicknesses are about 0.9 mm or more. The author uses conventional veneers for veneers thinner than 0.9 mm (Figure 7). It is important to note that the clinical situation should dictate the material and technique selected (ie, if thinner, more conservative veneers are the desired clinical result, then teeth should not be over-prepared to use machined or pressed glass ceramic materials). The system does not lend itself to knife-edge or no-preparation margin techniques. The best results for these situations are obtained with a medium chamfer preparation.
CAD/CAM Technologies and Interpenetrating (Infiltration Ceramics) Phase Materials
This class of materials uses a partially sintered crystalline matrix of a high modulus (stiff) material, in which there is a junction of the particles in the crystalline phase (Figure 8). The crystalline phase consists of alumina, an alumina/magnesia mixture, or an alumina/zirconia mixture. The material is supplied in block form (Figure 9) and only supplied for the CEREC inLab system. The framework made from any of the three materials is then infiltrated with a low-viscosity lanthanum glass at high temperature (Figure 10). The ceramic phase and the glassy phase form a continuous interconnecting meshwork. The final structure is about 85% crystalline and 15% glass. The materials are virtually the same as the VITA In-Ceram® (Vident) material. The big difference is the material is machined from a block rather than a slurry mixture of powder and liquid being built up with a brush. The alumina/magnesia mixture is a very translucent core material and, in the author’s opinion, is ideal for when anterior crowns are indicated and maximum translucency is desired (Figure 11 and Figure 12). The material has shown excellent clinical results for single posterior crowns of either the alumina or zirconia-infiltrated core; thus, it can be recommended for single posterior crowns. Because of the better physical properties of the solid sintered zirconia, the author uses cores from this material for all-ceramic posterior crowns. There are a couple of systems on the market that use electroplating technology (one example is WolCeram, MicroDental Laboratories, Dublin, CA) to “plate” the alumina material to a master die. It is then infiltrated with the same glass as in the conventional In-Ceram technique or the CAD/CAM technique. These systems should perform as well as the conventional In-Ceram material because it has very similar physical properties; thus, it can be recommended for single posterior crowns. The system has been recommended by some for posterior bridge applications, but there are no published clinical studies supporting these plating systems for use in posterior bridges. The In-Ceram alumina material is not recommended for posterior fixed partial dentures (bridges) by the manufacturer. The author’s personal experience would agree with that, as over 30% of the posterior bridges fabricated with the alumina material failed by 7 years. The system has proved to be safe and effective for 3-unit anterior bridges.2
Preparations ideally should be a 360° heavy chamfer to shoulder. Sharp line angles need to be rounded as none of the CAD/CAM systems machine well into sharp line angles. Sharp line angles can also concentrate stress and lead to earlier than normal fracture. Preparations for Spinell anterior restorations should allow for 1.2 mm of crown thickness for ideal esthetics. Because of the greater opacity of the alumina or the zirconia material, 1.5 mm of space is necessary for ideal esthetics, which is the same as a PFM.3
Solid Sintered Monophase Ceramics
Solid sintered ceramics have the highest potential for strength and toughness but, because of high firing temperatures and sintering shrinkage techniques, they were not available to use as high-strength frameworks for crowns and fixed partial dentures until recently. Solid sintered monophase ceramics are materials that are formed by directly sintering crystals together without any intervening matrix to form a dense, air-free, glass-free, polycrystalline structure (Figure 13). There are several different processing techniques that allow the fabrication of either solid sintered aluminous oxide or zirconia oxide frameworks.
There are three basic techniques for fabricating solid sintered monophase ceramic frameworks for porcelain application. One system, DCS Preciscan (marketed in the United States by Dentsply Austenal) machines from a solid sintered block of material the final desired framework shape. This system is expensive and has not proven cost effective as a result of the excessive machining time and manual labor necessary to adjust and fit the coping. Secondly, the Procera® system (Nobel Biocare, Yorba Linda, CA) employs an oversized die where slurry of either aluminous oxide or zirconia oxide is applied to the die, subsequently fired, fully sintered, and shrunk to fit the scanned die. The Procera system also has the ability to fabricate custom abutments for regular platform Brånemark implants (Figure 14 and Figure 15). The third method machines an oversized coping from a partially sintered block of zirconia oxide material, which is then fired to full sintering temperature and then shrunk to fit the die. Most of the systems on the market today use some variation of this type of technology. Examples of these systems are the CEREC InLab (which uses VITA YZ [Vident] and Ivoclar e.max materials), Lava™ (3M™ESPE™, St. Paul, MN) Cercon (Dentsply, York, PA), Everest (KaVo, Lake Zurich, IL), and TDS systems (Figure 16). These systems scan the prepared die, and then the software creates virtual dies and frameworks. An oversized framework is created through a CAM process, which is then fully sintered in a special oven. The VITA YZ and the Lava™ systems also allow for internal shading of the core material. In the author’s experience, the white zirconia is too reflective and thus the final result is too opaque. The recommendation is to use a system that allows internally colored cores. The two systems that allow internally colored zirconia cores of different shades are the VITA YZ system machined on the CEREC inLab; this system is marketed as inVizion™ (Vident), and the Lava™ system (Figure 17 and Figure 18). Some systems allow the external application of color on the surface of the white core but this also has the potential of being too opaque.
Zirconia oxide, sometimes called zircon, has unique physical characteristics that make it twice as strong and twice as tough as alumina-based ceramics. While the reported values for flexural strength of this new material range from over 900 MPa to 1,100 MPa,4 it is important to note there is no direct correlation between flexural strength (modulus of rupture) and clinical performance. Generally, stronger materials have performed better but there are many factors that contribute to a material’s clinical success along with the flexural strength of the material. A more important physical property is fracture toughness, which has been reported to be between 8 MPa m1/2 and 10 MPa m1/2 for zirconia.3 This is significantly higher than any previously reported ceramic, and roughly twice the amount reported for the alumina materials. Fracture toughness is a measure of a material’s ability to resist crack growth (ie, a measure of the amount of energy necessary to cause crack growth). Clinically, restorations are not loaded to failure as is done in a flexural strength test; instead, millions of subcritical loads (chewing) are applied. Materials ultimately fail because of this cyclic fatigue by crack propagation. Thus, materials with higher fracture toughness are more ideal clinically as it takes more energy to cause crack growth. Other factors such as stress corrosion (chemically assisted crack growth) and residual flaws in the material greatly affect the final strength of a finished material and are discussed elsewhere.5
Clinical Indications
There have been relatively few clinical studies reporting on CAD/CAM-generated, all-ceramic, zirconia-core–based crowns that have included large sample sizes or long follow-up periods. Ideally, follow-up periods would be at least 5 years with sample sizes of several hundred units. Long follow-up periods are necessary because it takes several years for fatigue to cause failure. The author has placed over 300 VITA YZ and Lava™ restorations over the last 36 months with excellent success. To date there have been no zirconia core fractures observed; there have been a few cases of porcelain delaminated from some of the early crowns. It was determined that inappropriate firing of the porcelain to the core was the cause. Proper firing of a bonding layer of porcelain to the core is necessary to create a stable porcelain/zirconia core interface. The laboratory technique for doing this is covered elsewhere by the author.3 Thus, based on this early success, zirconia core restorations can be recommended for single units anywhere in the mouth.
For fixed partial dentures, reported clinical data has been short term but promising. This and many anecdotal reports of success would indicate that high-strength ceramic frameworks subsequently veneered with porcelain should perform to clinically acceptable standards for 3-unit anterior and posterior fixed partial dentures as long as accepted guidelines are maintained. It is important to note that while several studies are being initiated or are already ongoing (including here at UCLA) using CAD/CAM technology for the fabrication of posterior fixed partial dentures, no large-sample, long-term data yet exists to justify their ubiquitous use. Early results look extremely promising but the effects of fatigue and chemical corrosion take time to manifest their effects. Clinical use of these materials for posterior fixed partial dentures should still be considered experimental at this point and patients should be fully informed of possible effects.
Clinical Guidelines
The correct reduction for the room necessary for the esthetic fabrication of a zirconia all-ceramic crown is the same as for esthetic PFM restorations. Evaluation of restorations in which the author performed all clinical and ceramic procedures has led to the determination that 1.5 mm of labial overall crown thickness was the minimum ideal dimension for predictable esthetics and shade reproduction. The core can be thinned to 0.3 mm on the facial, which leaves room for 1.2 mm of porcelain. A minimum of 1 mm of crown thickness is required for the lingual walls. Incisal edge thickness can be as little as 1.5 mm, but 2 mm is ideal esthetically. Posteriorly, it is necessary to have 2.5 mm of occlusal reduction for both esthetic all-ceramic and metal-ceramic restorations, especially if natural, unworn occlusal anatomy is desired in the final restoration. The best aid the author has found to accomplish this reduction is the 2-mm Reduction Guide from Kerr Corporation (Orange, CA); if the 2-mm guide passes with only slight binding through the occluded opposing arches then there is close to 2.5 mm of interocclusal space (Figure 19). As with the previously mentioned machinable materials, ideally preparations should be a 360° heavy chamfer to shoulder and sharp line angles should be avoided. Preparation line angles need to be rounded as sharper line angles are not easily milled (Figure 20).
Lab Considerations
One of the main benefits of zirconia is using the same ceramic or veneer material for all clinical situations. Porcelains for zirconia frameworks can be used for porcelain veneers (Figure 21 and Figure 22), crowns, and fixed partial dentures. The only other porcelain a laboratory would need is a metal-ceramic material.
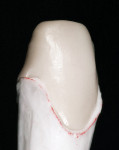
There are some tricks to working with the zirconia cores to get the best esthetic results. Zirconia cores are slightly more opaque than dentin, so it is ideal to design the framework to allow for a more translucent porcelain margin material to be placed. There is a misconception that the margin material should have the same translucency as dentin. If the marginal area were at all visible it would not be noticeable unless the margin material also had the exact same chroma and hue as the surrounding tooth structure. It is actually ideal to have the marginal material to be slightly more translucent than the surrounding tooth structure so that it blends in by picking up some color from the tooth—the so-called contact lens or chameleon effect. So, just as with metal or more opacious ceramic cores, a porcelain margin is mandatory for ideal esthetics. The benefit over metal–ceramics is that the framework only needs to be shortened slightly to allow enough light through to illuminate the gingival area to create a natural effect (Figure 23).
References
1. McLaren EA, Terry DA. CAD/CAM systems, materials, and clinical guidelines for all-ceramic crowns and fixed partial dentures. Compend Contin Educ Dent. 2002;23(7):637-654.
2. Sorensen JA, Kang SK, Torres TJ, Knode H. In-Ceram fixed partial dentures: three-year clinical trial results. J Calif Dent Assoc. 1998;26(3):207-214.
3. McLaren EA, Giordano RA. Zirconia based ceramics:material properties, esthetics, and layering techniques of a new porcelain, VM9. Quintessence Dental Technol. 2005;28:99-111.
4. White SN, Miklus VG, McLaren EA, et al. Flexural strength of a layered zirconia and porcelain dental all-ceramic system. J Prosthet Dent. 2005;94(2):125-131.
5. Sorensen JA, Berge HX, Edelhoff D. Effect of storage media and fatigue loading on ceramic strength [abstract]. J Dent Res. 2000;79:271. Abstract 1017.
About the Authors
Edward A. McLaren, DDS, MDC
Adjunct Associate Professor
Director, UCLA Center for Esthetic Dentistry
Los Angeles, California
Private Practice, Limited to Prosthodontics and Esthetic Dentistry
Los Angeles, California
Lu Hyo
Master Dental Ceramist
Assistant Director, UCLA Master Dental Ceramist Program
UCLA School of Dentistry
Los Angeles, California