Contemporary Treatment of Mandibular Edentulism
Lyndon F. Cooper, DDS, PhD, Kuang-Han Chang, DDS, and Ingeborg De Kok, DDS
Edentulism remains prevalent in the United States among individuals older than 65 years of age. It results in a wide range of local anatomical, physiological, and psychosocial changes that include continued residual ridge resorption, reduced masticatory function, altered facial esthetics associated with changes in vertical dimension and muscular function, and deterioration in self-reported social functions. It is a condition with broad physiological and psychosocial impact, which can be managed effectively using endosseous dental implants.
An obvious result of edentulation is alveolar bone loss and a reduction in mandibular function (Figure 1). A recent review of residual ridge resorption acknowledged the multifactorial etiology and suggested that combinations of anatomical, metabolic, mechanical, and yet-to-be-analyzed factors contribute to it. Denture use remains a controversial factor contributing to residual ridge resorption. Carlsson concluded that an excellent method to avoid jawbone resorption was preventive dental care to maintain dental health and avoid total extraction.1 For the hopeless dentition or the already edentulous jaws, the insertion of an implant-supported prosthesis can reduce bone loss and may even promote bone growth.
Prosthetic treatment using a complete denture is associated with additional complications, which may add to patient dissatisfaction. Commonly observed problems include denture stomatitis and denture sores as well as functional problems affecting phonetics and mastication. Conventional dentures are clearly not an ideal treatment for mandibular edentulism. When considering contemporary treatment of the edentulous patient, endosseous dental implants for the treatment of edentulism offers an alternative treatment to complete denture therapy. Key among the advantages of mandibular implants are the improvement in mandibular function, the prevention or reversal of alveolar bone loss, and the measurable improvement in self-reported satisfaction with treatment.2 Yet, complete treatment of the edentulous patient extends beyond considerations of improved prosthesis function.
Contemporary Treatment of the Edentulous Patient
There are at least six aspects of care that contribute to a contemporary approach to the treatment of the edentulous population (Table 1). Primary among these is acknowledgement of the extent of the edentulism and the importance of encouraging routine oral examination of all edentulous patients, which is is the basis for ensuring oral health and the keystone to ensuring a high-quality prosthesis. Clinicians should be motivated to prescribe endosseous dental implant-supported prostheses for every patient with an edentulous mandible.
Routine Oral Examination of the Edentulous Patient
Edentulism is more prevalent among older individuals and more common in rural communities. Other oral diseases, notably oral cancers, are also more prevalent in the older US population. The reported incidence of oral cancer is not diminishing and early diagnosis is among the most important factors affecting prognosis and treatment.3 Other oral mucosal diseases also affect the edentulous patient, including infectious diseases (eg, candidiasis) and autoimmune disorders, including mucosal disorders (eg, lichen planus). In addition, salivary diseases such as Sjögren’s syndrome have a direct impact on the ability of the edentulous patient to use dentures comfortably and effectively. The consequences of edentulism and denture use have further impact on the oral structures and merit continuous monitoring (Figure 2 ). The denture sore that is innocuous in the healthy individual may lead to osteonecrosis in the cancer survivor receiving systemic bisphosphonate chemotherapy.4 Management of the oral health needs of the edentulous patient has great relevance in the context of complex medical treatment of today’s older patient.
The edentulous oral condition is a prognostic factor that affects the difficulty of denture construction and may affect therapy outcomes. The Prosthodontic Diagnostic Index5 is an effective means of characterizing the complexity of the edentulous oral condition and offers tiered diagnostic levels that infer potential limitations of treatment and outcomes. The opportunities for patient referral to prosthodontists, oral pathologists, and oral surgeons for preprosthetic and prosthetic consultation or treatment should be pursued to maximize individual care.
Replace Dentures within 5 Years with a Renewed Focus on Esthetics
Denture satisfaction is multifactorial, and includes perceived function, fit, and appearance. Constructing new dentures or modifying existing ones by reline or rebase techniques is required to address the physical changes that occur with edentulism (residual ridge resorption, loss of vertical dimension of occlusion) as well as the physical deterioration of dentures (Figure 3 ).
Poorly fitting dentures should be directly treated. In a clinical study of 21 patients with poorly fitting dentures, Garrett and colleagues6 confirmed the general assumption that patients perceive improvements when ill-fitting dentures are relined or replaced by new dentures (Figure 4 ).
Another aspect of denture use is denture cleanliness (Figure 5 ). One study indicated that the majority of patients were not satisfied with the cleanliness of their dentures and, importantly, older dentures were associated with a higher incidence of denture stomatitis.7
Beyond health and physiologic function, dentures also have social functions. Several investigations have underscored the social significance of denture quality to the edentulous patient,8 and the social significance of dentures requires current emphasis. Given the present focus on esthetics in dental therapy for the dentate subject, denture esthetics should be an integral part of this growth in dentistry (Figure 6 ). In fact, esthetic principles can find their roots in the classic prosthodontic literature addressing denture esthetics9 (Figure 7A and Figure 7B ).
Prescribe Mandibular Dental Implants for All Edentulous Patients
There is compelling data to support the clinical posture that mandibular implants should be prescribed for all edentulous patients. Prospective investigations of 5, 10, and 15 years demonstrate that at the patient level, implant and prosthesis survival is > 90%. The original description by Adell and coworkers10 of the Brånemark dental implant system revealed that at 15 years there was > 95% implant and prosthesis survival. Many investigators worldwide have reported that the success of dental implants for the treatment of mandibular edentulism is high (> 90% after 5 years).11 Discrepancies exist between study designs and reporting criteria;12 however, a wide body of evidence indicates that endosseous dental implants placed in the parasymphyseal mandible survive to support prosthesis function for many years (Figure 8 ).
Clinicians must also be motivated to maintain the endosseous dental implants of edentulous patients. Local peri-implant inflammation is observed when plaque and calculus form on the abutment and adjacent prostheses. Annual examinations should be performed (Figure 9A and Figure 9B). Removal of the prostheses may be required to perform peri-implant mucosal probing. Early signs of inflammation and increased peri-implant mucosal sulcus depth should be addressed by increasing hygiene through education and minor prosthesis modification. Evidencing the established criteria for success (> 0.2 mm annually) may be addressed by interceptive therapy.13
Prosthesis stability for mandibular implant-supported fixed dentures is also high.14 Yet there are complications associated with treatment. Primary among these complications are bridge screw loosening and fracture, abutment screw loosening and fracture, prosthesis fracture and prosthetic tooth wear (Figure 10 ). Tooth wear is a complication that must be addressed intermittently. The increased functional capacity imparted to the implant-supported fixed denture patient is clearly observed by prosthetic tooth wear. The biologic consequences of tooth wear include loss of vertical dimension of occlusion and the attendant sequelae. The mechanical consequences of tooth wear is the disruption of the designated occlusal scheme, typically resulting in marked vertical overjet and increased lateral tooth contacts, which may contribute to high nonaxial forces acting at the bridge screws. Although the rate of tooth wear will vary among materials and patients, experience indicates that the need for restoration of the occlusal scheme and vertical dimension of occlusion for acrylic denture teeth should be considered approximately every 3 to 5 years. These factors must be accounted for and included in the patient’s calculations of treatment cost over the long term. It is important to recognize that the majority of the complications associated with implant therapy are minor, mechanical or prosthetic in nature, and associated with little morbidity. However, they often represent unanticipated and relatively expensive interruptions in otherwise trouble-free prosthetic rehabilitation of the edentulous mandible.
A recent review of the complete denture literature suggests that many edentulous patients are satisfied with complete denture therapy and may not seek dental implant treatment.1 Every patient will not consent to receive dental implants. MacEntee and colleagues2 suggested that pain, the perception of poor chewing function and speech, and dissatisfaction with appearance motivate patients to choose dental implants. Irrespective of the status of the edentulous patient, treatment using endosseous dental implants should be discussed in terms of potential improvement of limitations in measured and self-reported outcomes.
There are few absolute contraindications for treatment of the edentulous mandible using dental implants. Because edentulism is most prevalent in the older population, the complexity of treatment because of existing medical conditions (eg, diabetes or anticoagulant therapy) must not be underestimated. Sugerman and Barber15 concluded that there was little published information regarding the long-term outcome of implants in patients with diverse systemic diseases. Weyant and Burt16 reported greater implant failure in individuals with contributory medical histories. Although there appear to be few absolute medical contraindications for dental implant therapy, occasional patient-specific limitations are encountered and a comprehensive knowledge regarding each individual patient is therefore essential.
Local factors for implant placement in the parasymphyseal are typically favorable. In a large majority of patients, this region of the mandible offers sufficient bone for treatment without prerequisite grafting. The edentulous patient may be categorized according to the anatomic representation of the mandibular and maxillary residual alveolar ridges. Earlier reports concerning the use of endosseous dental implants suggested that they would benefit the most severely resorbed mandible,17 although later investigations demonstrated that patients with both severe and moderately resorbed mandibles derived benefit from dental implant-supported protheses.18
Several classification systems are helpful in assessing the extent of alveolar resorption19 as well as residual bone volume and bone quality.20 A broader understanding of the denture patient is required and a classification system for edentulous patients can provide insight into the difficulty of denture treatment.5 Implants are not only reserved for the most severely resorbed mandibles or the most difficult denture patients. As the extent of treatment increases to meet the complexities associated with systemic disease, marked alveolar ridge resorption, neuromuscular dysfunction, local tissue factors, and patient demands, the opportunities for multi disciplinary care expand and should be explored to ensure individual patient success and satisfaction.
There are risks specifically associated with dental implant treatment of the parasymphyseal mandible. These are less commonly reported risks of treatment and include placement of an implant near the inferior alveolar nerve or severing of the inferior alveolar nerve leading to dysesthesia or paresthesia, mandibular fracture after implant placement, or life-threatening bleeding from the lingual artery. These risks can be reduced by careful planning as well as the rare exclusion of select patients based on current illness or past medical history. Guided surgeries using computed tomography analyses (Figure 11 ) and more recent innovations using CAD/CAM surgical guides offer additional potential benefit in careful implant placement.21
The most common risk facing the patient who receives careful treatment planning and prosthesis evaluation before implant placement is the risk of early implant failure (before loading). Delayed failures are reported to be less common. Implant fracture is reported to occur infrequently (approximately 1% of all failures).22
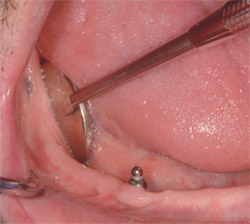
A spectrum of treatment modalities and protocols ranging from overdenture therapy using a two-stage procedure to implant-supported fixed denture therapy provided by immediate loading are available to the vast majority of edentulous patients. A simple designation of treatment options for the edentulous mandible is to consider the majority of patients for treatment using either two implants with ball abutments for overdentures (Figure 12A and Figure 12B ) or four implants supporting a fixed denture constructed using a metallic bar veneered with resin or porcelain (Figure 13 ).
Additionally, six to eight implants can be used to support porcelain-fused-to-metal (PFM) fixed partial dentures. There are advantages and disadvantages for each treatment opportunity and the cost of treatment represents a major distinguishing characteristic among these three different approaches to therapy.
Overdentures Using Two Implants without Prosthetic Bars or Superstructures
Implant-retained overdentures have been reported to be the minimal standard of care for the treatment of mandibular edentulism.23 There are excellent reviews that discuss the advantages and disadvantages of this treatment24 and most succinctly, the implant-retained mandibular overdenture using ball abutments as retentive elements represents a cost-efficient prosthesis that offers physiological advantages of maintained alveolar bone mass and improved masticatory function, psychosocial advantages of improved self-image and social function, and benefits of access for oral hygiene. The controversy regarding the use of gold bars and clips vs ball abutments with retainers as retentive elements for the overdenture can be summarized by recognizing that there is a lack of evidence that splinting of implants improves osseointegration outcomes or that the bar offers better retention of the overdenture. The presence of the bar can result in increased plaque retention and peri-implant inflammation. Both bar-retained and ball-retained prostheses require regular maintenance and the expense of this maintenance should be explained to patients at the consultation visit.
The presently stated preference for simplicity using two-implant?retained overdentures may involve the use of ball attachments or the recently introduced Locator™ (Zest Anchors, Inc, Escondido, CA) attachment system. Like the Locator abutment, ball abutments should be used with resilient attachments (eg, Preci-Clix™ attachments, Preat Corporation, Santa Ynez, CA) that preclude abutment wear during function. The stated advantages of the Locator system include reduced vertical dimension of the components, adaptation of divergent implants, and simple modification of retention by selection of resilient attachments. These advantages should not serve as excuses for poor treatment planning. When compared to more complex prosthetic reconstruction for overdentures such as three- or four-implant?supported bar overdentures, Van Kampen et al25 measured retention of ball vs bar attachments for 18 overdenture patients and found little difference, thereby confirming the laboratory result of Petropoulos et al.26
The two-implant?supported overdenture can be used for a wide range of mandibular edentulous patients. A minimum residual ridge height of 10 mm is recommended. The presence of the inferior alveolar nerve at the ridge crest of markedly resorbed ridges should be acknowledged and addressed by denture relief, but should not preclude the provisional prescription of a two-implant overdenture.
Planning for parallel implants facilitates restoration and the use of ball abutments. Planning must also include the provision for sufficient occlusogingival dimension measured from the plane of occlusion (or the incisal edge) to the residual ridge crest. This dimension represents the space that will be filled by the prosthetic teeth, the denture acrylic, the ball housing, and the abutment. A minimum of 10 mm is recommended to accommodate 4 mm of incisor length above the denture resin, 2 mm of acrylic resin to support the retainer, 1 mm for the thickness of the retainer above the ball abutment, and a minimum of 3 mm for a ball abutment beyond the crest of bone. Therefore, when a panoramic radiograph and clinical examination reveal that the residual anterior mandible is > 15 mm to 18 mm in height, encroachment on this restorative space may occur and should be compensated for by an alveolectomy preceding implant placement. This aspect of treatment planning allows an esthetic and robust denture to be made that will avoid many of the complications commonly encountered with mandibular overdentures.
It is possible to place two implants in the parasymphyseal mandible using tomography to guide a flapless surgical procedure. When this is possible, the implants and two ball abutments may be placed and a denture can be inserted at the time of surgery (immediate provisionalization). To permit osseointegration to occur without excessive loading of the implants, the intaglio surface of the denture must be relieved circumferentially around the abutments and relined in this relieved region using a soft, resilient liner. After 6 to 8 weeks of healing, the retainers can be connected by a reline procedure or direct pick-up method using autopolymerizing denture repair resin. After the connection procedure, it is prudent to perform a remount procedure to refine the denture occlusion. The ultimate success for the overdenture therapy is reliant upon osseointegration success of the implants as well as the overall clinical success of conventional denture therapy. Long-term success is critically dependent on recall evaluation, patient compliance with oral and denture hygiene, and consideration of reline therapy throughout the lifetime of the overdenture prosthesis.
Four Implants and an Implant-Supported Fixed Denture
The implant-supported fixed denture revolutionized the treatment of mandibular edentulism.10 There are also excellent reviews that discuss the advantages and disadvantages of this treatment.27 The biological capacity of the parasymphyseal mandible to support implant function is great. Simplification using fewer implants (four vs five or six) and immediate loading protocols have emerged.28 The potential advantages for this simplification are reduced component costs, prosthetic construction simplification, and improved access for hygiene. When there is elevated concern for osseous support using only four implants (eg, residual mandible height of 8 mm to 9 mm) or there is concern for marked function (eg, in a well-known bruxer), an additional implant can be provided.
A minimum residual ridge height of 8 mm is recommended. When dysesthesia is marked as a result of the presence of the inferior alveolar nerve at the ridge crest, this treatment approach may be preferred when compared to the overdenture. When oral hygiene may be questioned or restricted for physical reasons, the implant-supported fixed denture may be dissuaded in favor of an overdenture prosthesis.
Planning for implant placement for an implant-supported fixed denture also requires concern for occlusogingival dimension. To ensure an esthetic, phonetic, hygienic, and mechanically robust prosthesis, an absolute minimum of 10 mm of occlusogingival dimension is recommended to accommodate 4 mm of incisor length above the metallic bar, 4 mm for the prosthetic cylinders, metallic bar and retaining screws, and 2 mm to account for the transmucosal dimension of the abutment beyond the crest of bone. After examining mandibular casts mounted to oppose the established maxillary dentition at the correct vertical dimension of occlusion, any occlusogingival dimensional discrepancies should be addressed by consideration of an alveolectomy at the time of implant placement.
To further ensure the mechanical integrity of the final prosthesis, the distance between the most anterior and most posterior implants (ie, the A-P spread) must also be defined and maximized (Figure 14A and Figure 14B ). In simple terms, the A-P spread must be > 10 mm to accommodate a prosthetic cantilever of 15 mm (the dimension of two mandibular bicuspids). A recent development involves axial displacement of terminal implants in the “all-on-four” concept29 and is now widely advocated using several different implant systems.
The construction of the implant-supported fixed denture requires great attention to detail. The fabrication of the metallic framework of the prosthesis must be achieved with precision to ensure passive fitting at all four of the abutment/prosthesis interfaces. This ensures proper bridge screw mechanics that will preclude the majority of screw loosening and screw fracture incidents. Several new technologies including CAD/CAM machining (Procera®, Nobel Biocare, Yorba Linda, CA) and laser welding adaptation (Cresco™, Astra Tech, Inc, Waltham MA), offer direct solutions to precision of fit. The veneering of prosthetic teeth can be planned as a PFM prosthesis or as an acrylic-wrapped denture tooth prosthesis. Although there may be advantages of esthetics and wear resistance to the PFM prosthesis, the initial cost and potential cost of repairs must be considered. Acrylic denture teeth processed to the metal framework has the disadvantage of wear and delamination or tooth fracture, but the advantages of initial cost and planned tooth replacement have been acknowledged.
Evaluate for Biologic and Prosthetic Complications on a Regular Basis
The recall of patients and maintenance of implant-supported fixed dentures is required. Biological consequences of implant placement in the parasymphyseal mandible include bone accrual in the mandible. This is considered to be a clinical manifestation of Wolff’s Law (the bone’s response to physical loading). Bone responses adjacent to the implant are controlled by mechanical as well as biological effectors. Local inflammation at the implant abutment resulting from biofilm accumulation should be monitored and addressed. Periodontal probing at the recall appointment of the dental implant abutments will reveal changes in tissue dimensions and show inflammation by bleeding. It may be necessary to remove the prosthesis annually to accurately perform probing measurements and thoroughly clean the prosthesis. Reversing local peri-implant mucosal inflammation is possible by the removal of plaque and the reinforcement of hygiene measures by instruction or modification of the prosthesis to permit greater access. Periodic recall should include radiographic assessment of the implant?bone interface with particular emphasis of the marginal bone response. Albrektsson and Zarb30 suggested that marginal bone loss should not exceed 0.2 mm annually after the first year of bone adaptation. Bone loss of 1 mm in a year indicates an inflammatory process that should be intercepted. Lang and colleagues suggested a protocol for intervention.13 Cupping bone loss around an implant has been reported to suggest mechanical overloading31 and intervention may include alteration of the prosthesis, perhaps by first evaluating the bilateral symmetry of centric occlusal contacts, second by identifying marked excursive contacts, and third by considering the cantilever length of the prosthesis. Intervention at the prosthesis level should accompany any attempt to recover from cupping bone loss.
Screw loosening or screw fracture is the most common prosthetic complication associated with the implant-supported fixed denture. Mechanical loading is suggested to be the cause of this problem and may be due to bending moments experienced by the bridge screw or the abutment screw. The rate of such complications has been suggested to be high. For example, early investigations reported greater than 20% incidence of screw complications.32 However, there may be advantages to contemporary implant designs that involve interference fits and internal tapered connections. As an example, treatment of 109 patients with implant-supported fixed dentures resulted in no screw loosening or fracture during a 5-year prospective investigation.33 Component systems that protect the assembly screw(s) from functional overloading contribute to improved therapeutic outcomes.
Six to Eight Implants and an Implant-Supported Fixed Partial Denture
This treatment alternative is reserved for individuals with little residual ridge resorption or the desire for toothlike restorations, which are supported by the patience and financial means to achieve this result. Implant-supported fixed dentures fabricated using either porcelain or acrylic veneers, alternatively, can be provided. The promise of toothlike restorations should not be taken lightly by the clinician. Therefore, it is suggested that this treatment be reserved for individuals with ideal residual ridge morphology or those who are willing to undergo bone grafting procedures and accept the risks and potential limitations of vertical and/or horizontal ridge augmentation procedures.
The key limitation to this treatment is ideal implant placement. Toothlike restorations require ideal implant placement, which is wholly dependent on presurgical prosthetic planning using fully waxed diagnostic casts and well-formed surgical guides. Subsequent peri-implant tissue morphology may be limited, but the lower lip typically shelters this limitation and its impact is not a key factor in treatment acceptance as it often is for the edentulous maxilla.
When this treatment is performed using segmented fixed partial dentures, the opportunities for long-term maintenance appear good. The potential for prosthetic failure can be isolated to only a few implants and a relatively small prosthesis, which simplifies possible repair or replacement. The same is true for implant failure with segmented fixed partial dentures. If an early or late implant failure is encountered, there is an opportunity for provisionalization during the period of time that implant placement is repeated.
CONCLUSION
Edentulism remains prevalent in the United States and a renewed focus on the edentulous patient is indicated by demographics. Dental implant therapy is effective and successful. The associated complications require a lifetime of recall evaluation for prevention and dutiful maintenance. Clinicians should actively encourage edentulous patients to attend annual recall evaluations, to consider denture replacement in a timely manner, and to consider the potential use of endosseous dental implants as an effective means of improving their own perceptions of function, appearance, and image.
References
1. Carlsson GE. Responses of jawbone to pressure. Gerodontology. 2004;21(2):65-70.
2. MacEntee MI, Walton JN, Glick N. A clinical trial of patient satisfaction and prosthodontic needs with ball and bar attachments for implant-retained complete overdentures: three-year results. J Prosthet Dent. 2005;93(1):28-37.
3. Morse DE, Kerr AR. Disparities in oral and pharyngeal cancer incidence, mortality and survival among black and white Americans. J Am Dent Assoc. 2006;137(2):203-212.
4. Woo SB, Hellstein JW, Kalmar JR. Systematic review: bisphosphonates and osteonecrosis of the jaws. Ann Intern Med. 2006;144(10):753-761.
5. McGarry TJ, Nimmo A, Skiba JF, et al. Classification system for complete edentulism. The American College of Prosthodontics. J Prosthodont. 1999;8(1):27-39.
6. Garrett NR, Kapur KK, Perez P. Effects of improvements of poorly fitting dentures and new dentures on patient satisfaction. J Prosthet Dent. 1996;76(4):403-413.
7. Dikbas I, Koksal T, Calikkocaoglu S. Investigation of the cleanliness of dentures in a university hospital. Int J Prosthodont. 2006;19(3):294-298.
8. Nitschke I, Muller F. The impact of oral health on the quality of life in the elderly. Oral Health Prev Dent. 2004;2(suppl 1):271-275.
9. Frush JP, Fisher RD. Introduction to dentogenics restorations. J Prosthet Dent. 1955;5:586-595
10. Adell R, Lekholm U, Rockler B, et al. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg. 1981;10(6): 387-416.
11. Rasmusson L, Roos J, Bystedt H. A 10-year follow-up study of titanium dioxide-blasted implants. Clin Implant Dent Relat Res. 2005;7(1):36-42.
12. Esposito M, Coulthard P, Thomsen P, et al. Interventions for replacing missing teeth: different types of dental implants. Cochrane Database Syst Rev. 2005;1: CD003815. Review.
13. Lang NP, Berglundh T, Heitz-Mayfield LJ, et al. Consensus statements and recommended clinical procedures regarding implant survival and complications. Int J Oral Maxillofac Implants. 2004;19(suppl):150-154.
14. Ganeles J, Rosenberg MM, Holt RL, et al. Immediate loading of implants with fixed restorations in the completely edentulous mandible: report of 27 patients from a private practice. Int J Oral Maxillofac Implants. 2001;16(3):418-426.
15. Sugerman PB, Barber MT. Patient selection for endosseous dental implants: oral and systemic considerations. Int J Oral Maxillofac Implants. 2002;17(2): 191-201.
16. Weyant RJ, Burt BA. An assessment of survival rates and within-patient clustering of failures for endosseous oral implants. J Dent Res. 1993;72(1):2-8.
17. Mericske-Stern R. Clinical evaluation of overdenture restorations supported by osseointegrated titanium implants: a retrospective study. Int J Oral Maxillofac Implants. 1990;5(4):375-383.
18. Raghoebar GM, Meijer HJ, van ‘t Hof M, et al. A randomized prospective clinical trial on the effectiveness of three treatment modalities for patients with lower denture problems. A 10 year follow-up study on patient satisfaction. Int J Oral Maxillofac Surg. 2003;32(5):498-503.
19. Cawood JI, Howell RA. A classification of the edentulous jaws. Int J Oral Maxillofac Surg. 1988;17(4):232-236.
20. Lekholm U, Zarb G. Patient selection and preparation. In: Brånemark PI, Zarb G, Albrektsson T, eds. Tissue-Integrated Prostheses: Osseointegration in Clinical Dentistry. 1st ed. Chicago, IL: Quintessence. 1985:195-205.
21. Sarment DP, Sukovic P, Clinthorne N. Accuracy of implant placement with a stereolithographic surgical guide. Int J Oral Maxillofac Implants. 2003;18(4):571-577.
22. Eckert SE, Meraw SJ, Cal E, Ow RK. Analysis of incidence and associated factors with fractured implants: a retrospective study. Int J Oral Maxillofac Implants. 2000;15(5):662-667.
23. Feine JS, Carlsson GE, Awad MA, et al. The McGill consensus statement on overdentures. Montreal, Quebec, Canada. May 24-25, 2002. Int J Prosthodont. 2002;15(4):413-414.
24. Sadowsky SJ. Mandibular implant-retained overdentures: a literature review. J Prosthet Dent. 2001;86(5):468-473.
25. van Kampen FMC, Cune MS, van der Bilt A, Bosman F. Retention and postinsertion maintenance of bar-clip, ball and magnet attachments in mandibular overdenture treatment: an in vivo comparison after 3 months of function. Clin Oral Implants Res. 2003;14(6):720-726.
26. Petropoulos VC, Smith W, Kousvelari E. Comparison of retention and release periods for implant overdenture attachments. Int J Oral Maxillofac Implants. 1997;12(2):176-185.
27. Zitzmann NU, Marinello CP. Related Articles, Links A review of clinical and technical considerations for fixed and removable implant prostheses in the edentulous mandible. Int J Prosthodont. 2002;15(1): 65-72. Review.
28. Brånemark PI, Engstrand P, Ohrnell LO, et al. Branemark Novum: a new treatment concept for rehabilitation of the edentulous mandible. Preliminary results from a prospective clinical follow-up study. Clin Implant Dent Relat Res. 1999;1(1):2-16.
29. Malo P, Rangert B, Nobre M. “All-on-Four” immediate-function concept with Brånemark System implants for completely edentulous mandibles: a retrospective clinical study. Clin Implant Dent Relat Res. 2003;5(suppl 1):2-9.
30. Albrektsson T, Zarb GA. Current interpretations of the osseointegrated response: clinical significance. Int J Prosthodont. 1993;6(2):95-105.
31. Rangert B, Krogh PH, Langer B, et al. Bending overload and implant fracture: a retrospective clinical analysis. Int J Oral Maxillofac Implants. 1995;10(3):326-334. Erratum in: Int J Oral Maxillofac Implants. 1996;11(5):575.
32. Zarb GA, Schmitt A. The longitudinal clinical effectiveness of osseointegrated dental implants: the Toronto study. Part III: Problems and complications encountered. J Prosthet Dent. 1990;64(2):185-194.
33. Arvidson K, Bystedt H, Frykholm A, et al. Five-year prospective follow-up report of the Astra Tech Dental Implant System in the treatment of edentulous mandibles. Clin Oral Implants Res. 1998;9(4):225-234.
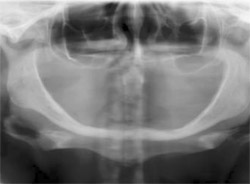 | 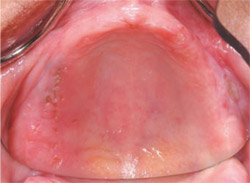 | |
| Figure 1 Residual ridge resorption is often severe. This panoramic radiograph illustrates complete resorption of alveolar bone with a residual mandible that is just 6 mm to 8 mm high. Although the prognosis for denture use is poor, dental implant treatment is possible and the resulting prosthesis prognosis would be enhanced. | Figure 2 Denture use is associated with many common sequelae, including denture stomatitis and denture-related ulceration of the mucosa. These ulcerations are often self-limiting after adjustment of denture occlusion or denture flange impingement. | |
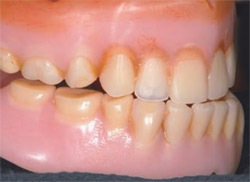 | 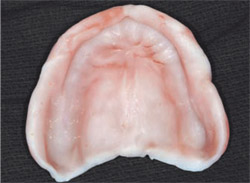 | |
| Figure 3 Dentures are often used without timely replacement. Although the period of usefulness of complete dentures is not fully defined, esthetic deficiencies because of wear, whitening, staining, or repair (shown) as well as tooth wear (shown) and ill-fitting intaglio surfaces are all reasons for denture replacement. | Figure 4 Denture reline procedures can be useful for diagnostic, therapeutic or impression-making purposes. A number of soft reline materials provide a rapid way to interrogate tissue responses to new denture bases and improve denture base/ tissue relationships. The reline procedure can be integrated into the earliest stages of denture and implant-retained overdenture therapies. | |
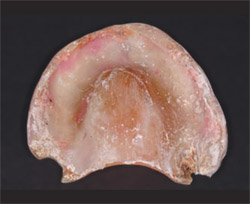 | 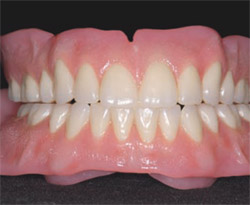 | |
| Figure 5 The quality of existing dentures is often related to denture hygiene. This denture illustrates a 20-year-old denture displaying complete wear of the occlusal surface of the molar through the denture base and extreme biofilm accumulation. Patient education is key to prevention. | Figure 6 The quality of new dentures should reflect contemporary interest in dental esthetics. Tooth shades and gingival morphologies can be arranged and processed to model ideal dentitions. (Shown here are BlueLine™ teeth, Ivoclar Vivadent, Amherst, NY, which were processed using custom- stained acrylic resin. Dentures processed by Donald J. Yancey.) | |
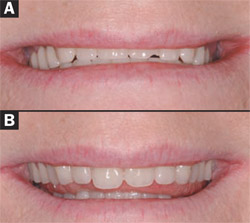 |  | |
| Figure 7A and Figure 7B Denture esthetic determinants are part of facial esthetics and should be organized around general defined principles. (A)The preoperative, existing denture is associated with reduced vertical dimension of occlusion and poor lip support. There is limited incisal display and an inverted smile line because of tooth attrition and fracture. (B) At denture try-in, the possible tooth arrangement is considered in terms of facial esthetics and dental esthetics. | Figure 8 Routine oral examination of the edentulous patient should be scheduled every 6 to 12 months and include a comprehensive oral examination of all of the oral soft tissues. The implants should be probed and the local tissues carefully interrogated. Intervention when peri-implant inflammation is observed should be provided and referral to a periodontist may be indicated. It is equally important to evaluate the overall health of the denture-supporting tissues and adjacent oral mucosa, tongue, and pharyngeal region. | |
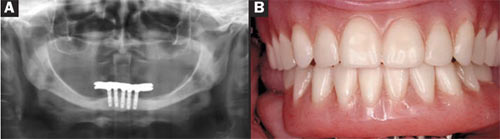 | ||
| Figure 9A and Figure 9B Implant-supported fixed dentures are associated with long-term function and implant success. (A) A 9-year postoperative radiograph illustrates the peri-implant bone levels at five 8-mm x 3.5-mm dental implants supporting an implant-supported fixed denture. (B) At 9 years, new acrylic denture teeth were processed on the original cast gold bar and the maxillary denture was replaced to restore the worn prosthesis and revitalize the esthetic appearance of the existing prosthesis. | ||
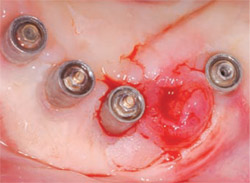 | 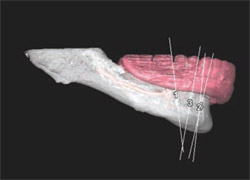 | |
| Figure 10 Prosthetic complications occur and are often complex in nature. Broken abutment and bridge screws (shown) create soft tissue complications and prosthetic complications that often require surgical intervention, identification, purchase and acquisition of appropriate components, and prosthetic repair. Patients must be informed of the potential cost and limitations of repair. | Figure 11 In many situations, a computed tomographic image of the bone and prosthesis offers the advantage of defining the relationship of vital structures (such as the inferior alveolar nerve) to the designated dental implant position Additional treatment information is available when the location of the prosthesis can be simultaneously observed. | |
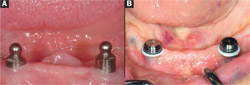 | 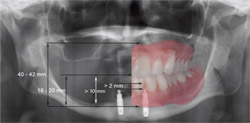 | |
| Figure 12A and Figure 12B Two implants offer a simple solution to mandibular overdenture function. (A) Two ball abutments 5 years after placement and loading with a mandibular overdenture. This status typifies the successful outcome reported in many clinical studies. (B) Newer abutments such as the Locator (shown with housing and spacer before chairside pickup) and new ball attachments such as Preci-Clix offer improved clinical management of the two-implant overdenture patient. | Figure 13 When the image of a complete mandibular denture is superimposed over the panoramic radiograph of two implants and ball abutments, the dimensional requirements for successful denture construction are clearly illustrated. When there is < 10 mm between the alveolar crest (the implant/abutment interface) and the planned occlusal plane, there is often insufficient space to house the implant abutment and the attachment housing in a sufficient thickness of acrylic resin (> 2 mm as shown) to preclude complications. | |
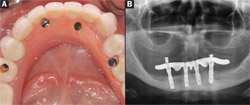 | ||
| Figure 14A and Figure 14B Contemporary concepts for implant-supported fixed dentures include the routine use of four implants to support the prosthesis. (A) As shown in this occlusal view, the axial displacement of implants enables greater anterior-posterior spread and enhanced biomechanical stability of the prosthesis at the abutment screw and bridge screw level. (B) Panoramic radiographic representation of treatment reveals the strategic distribution of the four implants medial to the mental foramen. | ||
| About the Authors | ||
 Lyndon F. Cooper, DDS, PhD Lyndon F. Cooper, DDS, PhDStallings Distinguished Professor Director of Graduate Prosthodontics School of Dentistry University of North Carolina at Chapel Hill Chapel Hill, North Carolina | ||
 Kuang-Han Chang, DDS Kuang-Han Chang, DDS Resident Graduate Prosthodontics School of Dentistry University of North Carolina at Chapel Hill Chapel Hill, North Carolina | ||
 Ingeborg De Kok, DDS Ingeborg De Kok, DDS Assistant Professor Department of Prosthodontics School of Dentistry University of North Carolina at Chapel Hill Chapel Hill, North Carolina | ||




