CAD/CAM Dentistry: A New Forum for Dentist-Technician Teamwork
Lee Culp, CDT; Alex Touchstone, DDS
The laboratory technician’s primary role in restorative dentistry is to perfectly copy all of the functional and esthetic parameters that have been defined by the dentist into a restorative solution. It is an architect/builder relationship. Throughout the entire restorative process, from the initial consultation through treatment planning, provisionalization, and final placement, the communication routes between the dentist and the laboratory technician require a complete transfer of information pertaining to existing, desired, and realistic situations and expectations to and from the clinical environment. Functional components, occlusal parameters, phonetics, and esthetic requirements are just some of the essential types of information that are necessary for the technician to complete the fabrication of successful, functional, and esthetic restorations.
Today, as in the past, the communication tools between the dentist and the technician are photography, written documentation, and impressions of the patient’s existing dentition. The clinical prep-arations and the opposing dentition from these impressions/models are created and mounted on an articulator, which simulates the jaw movements of the mandible.
As restorative dentistry evolves into the digital world of image capture, computer design, and the creation of dental restorations through robotics, the dental laboratory must evolve as well. To fully understand this concept, a laboratory must be clearly defined. At first thought, it may seem that a laboratory is the place where a dentist sends his or her patient’s impressions to be processed into restorations, which are sent back to the dentist for adjustment and delivery (Figure 1). This definition fits well with the traditional concept of a laboratory–dentist workflow. However, the possibility to transfer computer-aided design/computer-aided manufacturing (CAD/CAM) restoration files electronically has provided the catalyst for a significant change in the dentist–laboratory relationship (Figure 2).
The Virtual Laboratory
Imagine that the laboratory is not a physical place, but exists only in the talents of those performing the restorative process: the dentist, auxiliaries, and technician(s). The equipment used to create the restoration may be located centrally, remotely, or both. The laboratory is essentially a workflow, which is as flexible as the abilities of the dentist, the technician, and the equipment will allow. The primary decision becomes where the hand off from one partner to another should occur. The dentist who has the ability to optically scan teeth for impression-making and who often chooses CAD/CAM restorations as the best treatment option for their patients has enhanced freedom as to where the hand off to the technician should occur. The laboratory is no longer a place, it is instead to a large degree, virtual.
In some instances, it may make sense for the dentist to work independently and finish the restoration chairside in a single visit with the obvious advantages a clinical CAD/CAM system has to offer (Figure 3). These cases might include less complex restorations or fewer numbers of restorations for the same patient that do not require any special characterization other than perhaps stain and glaze or polish. Other times, it may be advantageous to engage the services of a technician because he or she possesses the skill and, perhaps more importantly, the time to create restorations that either demand more complex characterization or can be more efficiently created in an indirect manner.
Computer-aided Dentistry
The first successful introduction of CAD/CAM into dentistry was the chairside CEREC® 1 system (Sirona Dental Systems, Charlotte, NC) in 1982. The fundamental principle of this concept was to electronically capture a preparation’s image and then use software to interpolate the information and create a digital model. A virtual restoration design was then suggested and, after user-defined parameters were set, the restoration design was milled from a ceramic block and seated, all in one appointment. With the introduction of the CEREC 2 and CEREC 3 systems (Sirona Dental Systems), subsequent software and hardware upgrades primarily focused on improvements in user-friendliness, accuracy, and material milling options. The current generation, CEREC 3D (Sirona Dental Systems), is still the only chairside CAD/CAM system available to dentists, although other systems are in development for future release.
The introduction of CEREC® inLab (Sirona Dental Systems) in 2004 (Figure 4), along with its accompanying software upgrades and libraries, became one of the first computerization model to accurately present a virtual model and take into consideration the occlusal affect of the opposing (antagonistic) dentition. It essentially takes a complex occulsal scheme and its parameters, condenses the information, displays it in an intuitive format (which allows anyone with basic knowledge of dental anatomy and occlusion to make modifications to the design), and then sends it through to the automated milling unit. For dental laboratories, the introduction of the inLab system effectively automated some of the more mechanical and labor-intensive procedures (eg, waxing, investing, burnout, casting, and/or pressing) involved in the conventional fabrication of a dental restoration, allowing the laboratory technician to create functional dental restorations with a consistent, precise method (Figure 5, Figure 6, Figure 7).
As with any conventional laboratory-prescribed restorative process, the CAD/CAM procedure begins with the usual steps: the clinician prepares the case according to the appropriate preparation guidelines, takes impressions of the case, and sends these and other critical communication aspects to the laboratory. After the laboratory receives all of the materials from the dentist, the impression is poured, the models mounted, and the dies are trimmed. A bite registration is taken using the mounted models and will be used in a subsequent step. At this time, the procedure moves into the realm of computerized technology for scanning and fabrication (Figure 8, Figure 9, Figure 10).
Although this application offers many advantages to the dentist–technician team, it still requires the making of an intraoral impression using conventional techniques and sending these impressions to the laboratory for the creation of a preparation and the opposing models.
Case Study
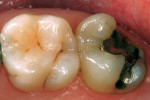
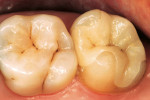
A 45-year-old woman presented with the distolingual cusp missing from her maxillary second molar (tooth No. 15) (Figure 11). She possessed a negative medical history and good oral hygiene with resultant periodontal health. The tooth had been previously restored with an amalgam restoration, and new decay undermining the mesial marginal ridge was diagnosed with digital radiography. Treatment options of a gold onlay, a porcelain-fused-to-metal crown, or a CAD/CAM ceramic onlay were considered and discussed with the patient. Although a gold onlay is an excellent, prudent choice, properly placed CEREC onlays have been demonstrated in many clinical studies to meet the clinical demand of ceramic inlays.1,2
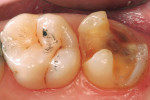
The patient was scheduled for a 45-minute appointment. On arrival, her maxillary left posterior sextant was anesthetized. The decay and old amalgam were removed and the tooth was prepared for the CEREC onlay, following accepted CAD/CAM glass-ceramic preparation guidelines (Figure 12).
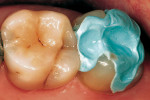
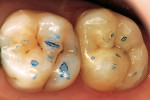
A static bite registration was then created by injecting a blue resilient bite registration material (Patterson Dental, St. Paul, MN) into the preparation only and having the patient occlude (Figure 13). The bite registration, first molar, and surrounding structures were then coated lightly with titanium dioxide contrast powder. Using the CEREC 3D acquisition unit and associated software, optical impression images were made of the bite registration and of the first molar. The bite registration was removed, the preparation was coated, and duplicate images of the preparation and the first molar were acquired. The images were stored in their appropriate image catalogs. The entire restoration file was saved and exported into a separate folder. Clinical photographs were taken using a Canon 10D camera body equipped with a 100-mm macro lens and ring flash (Canon USA, Inc, Lake Success, NY). The patient’s tooth was provisionalized with resilient intermediate composite resin (Fermit-N, Ivoclar Vivadent, Amherst, NY) and the patient was scheduled for a 30-minute appointment 2 days later.
The actual design of the restoration was not started at this point. The restoration file and clinical images were downloaded to a universal serial bus memory stick. The memory stick was then transferred to another computer that had Internet capability. The restoration file and clinical images were attached to an electronic mail (e-mail) message addressed to the laboratory along with information related to the prepared tooth and desired final shades.
Laboratory Procedures
After the data file was received through e-mail from the dental office, it was uploaded into the inLab system and the design procedure was initiated. A file must be created within the software for each individual case. The operator input the patient’s name, case number, dentist’s name, the date, the tooth number(s), and type of restoration desired (eg, full crown, veneer, inlay/onlay, or framework [coping]). Additional preferences (including material choices) can be set either globally for all cases from an individual dentist or based on the individual case. These options include preferred contact tightness, occlusal contact intensity, and the virtual die space, which defines the internal fit of the final restoration to the die/preparation.
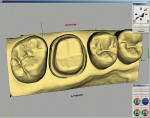
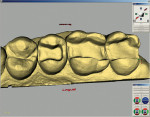
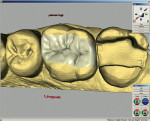
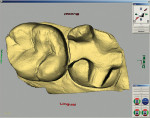
After all of this information was input, the computer began to search among the tooth database libraries to acquire the correct tooth form. At this point, the computer had all of the information it needed to work with the working model: the preparation and the occlusion parameters (from the antagonistic image). The three-dimensional virtual model was then presented on-screen and could be rotated and viewed from any perspective (Figure 14).
The first step in designing the restoration was to virtually section the model and remove the die. The parameters and borders of the final restoration were then defined using the antagonist information, the adjacent teeth, contact areas and, finally, the gingival margins of the preparation. The desired contact areas were marked electronically on the adjacent teeth and the preparation margins were identified and outlined, all of which was greatly assisted by the computer.
The computer places the restoration in the most appropriate position (based on all input), but the operator’s experience and knowledge of form and function is needed to manually position and contour the restoration to the clinically preferred location.
With a few mouse clicks, the position and rotation of the crown was altered as desired, and the software’s cusp setting application automatically readjusted each individual cusp tip and triangular ridge, as well as the restoration’s contours, contacts, and marginal ridges based on the preferences and antagonistic information according to the newly desired position and rotation. The virtual restoration responded and adapted all of the parameters immediately as they related to the new position. The position and intensity of each contact point was graphically demonstrated and color mapped immediately on the screen and could be adjusted easily pending operator and clinical preference.
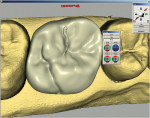
Customized aspects and artistic creativity are also possible through an array of virtual carving and waxing tools. These can be used to manipulate occlusal anatomy, contours, and occlusal preferences, basically mimicking the actual laboratory methods and armamentarium. Each step is immediately updated on-screen so that the operator can see the effect of any changes (Figure 15).
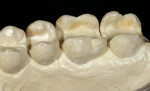
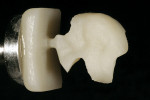
When the final virtual restoration was designed, the milling chamber was loaded with the predetermined shade and size of ceramic or composite block, an on-screen button was pressed and, in approximately 15 minutes, an exact replica of the design was reproduced in ceramic (Figure 16, Figure 17, and Figure 18).
Restoration Placement
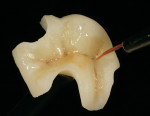
The restoration arrived back in the dental office 2 days later and the patient arrived for her appointment. The temporary was removed and the tooth was cleaned with chlorhexidine solution and water. The restoration was tried in and the margins and proximal contacts were checked for proper fit (Figure 19).
The restoration was bonded in place using Multilink® resin cement (Ivoclar Vivadent), following the manufacturer’s recommended protocol. The occlusal contacts were checked and harmonized in static occlusion and excursive pathway freedom was verified. The adjusted areas were repolished using Diashine (VH Technologies Ltd, Bellevue, WA) and a prophy brush. The degree to which these adjustments were necessary was minimal (Figure 20).
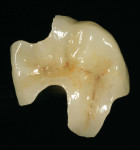
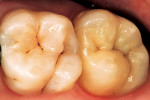
The finished restoration, which was designed and created by the laboratory without the aid of an impression, was found to be in functional and esthetic harmony (Figure 21). The total treatment time was 75 minutes.
Conclusion
Although this restoration could have been completed chairside with stain and glaze in approximately 90 minutes, this case was used to demonstrate that the option of using a virtual CAD laboratory is now available, which opens up several possibilities for enhanced workflow and variable hand-off points. For example, if a dentist needs assistance with a design or preparation evaluation, he or she could transfer the restoration file for evaluation and design completion. Within minutes, the restoration file could be transferred back to the dentist for milling, allowing completion of the restoration in one visit. Alternately, in a large clinical setting, such as a university or military installation, the restoration file could be transferred to a central laboratory for processing.
If a case presented with esthetic or design challenges that were beyond the comfort level of the dentist with moderate CAD/CAM experience (eg, multiple anterior restorations), then the same workflow would prove beneficial. During the learning process, the same dentist with little experience could use the transfer of images for design completion and evaluation to the laboratory and use these services as a progressive learning tool.
The dental profession currently regards CAD/CAM technology as a machine that fabricates frameworks or full-contour ceramic restorations. Digital dentistry represents a new way to diagnose, treatment plan, and create functional, esthetic restorations for patients in a more productive and efficient manner. CAD/CAM dentistry will only further enhance the dentist–technician relationship as they move together into this new era of patient care.
Disclosure
The authors are stock consultants for Sirona Dental Systems and Patterson Dental.
References
1. Hickel R, Manhart J. Longevity of restorations in posterior teeth and reason for failure. J Adhes Dent. 2001;3(1):45-64.
2. Reiss B, Walther W. Clinical long-term results and 10-year Kaplan-Meier analysis of CEREC restorations. Int J Comput Dent. 2000;3(1):9-23.
About the Authors
Lee Culp, CDT
Mosaic Studios, Inc.
Institute for Oral Art and Design
Bradenton, FL
Alex Touchstone, DDS
Private Practice
Hattiesburg, Mississippi