How BioDental Models Help Dentists Visualize, Plan, and Place Dental Implants
Although the use of 3-dimensional (3-D) computer modeling is becoming a standard protocol for implant procedures, many surgeons and restorative dentists are taking the next step, using the anatomically accurate BioDental Modeling System™ (Biomedical Modeling, Inc, Boston, MA) to assist in the visualization, planning, and placement of dental implants to help ensure predictable outcomes.
Like the 3-D software images that are now widely used in implant planning, BioDental models of a patient’s mandible or maxilla are created from a multi-slice or cone-beam computed tomography (CT) scan. The models are translucent so they clearly show bone density as well as bone height, the condition of the adjacent teeth, and the sinus features. They also distinguish between bone and soft tissue and highlight the inferior alveolar nerve channel to assist in planning implant placement.
The models are accurate to within 0.5 mm, and work with all implant systems with no special software for the surgeon, the restorative dentist, or the dental laboratory (Figure 1). Dentists are not locked in to one particular vendor and they do not have to be radiologists. It is much faster and easier to see features in a model that can be held in the hand than to discern them on a computer screen.
Setting Patient Expectations
BioDental models are communications tools. The use of state-of-the-art models when explaining implant procedures to a patient can help build a feeling of trust. It is important that patients understand the implant procedure. A BioDental model can help set patient expectations concerning the outcome as well as the time and cost of the surgery and restoration.
Creating the BioDental Model
The guidelines for taking a CT scan for making a BioDental model are basically the same as those required by 3-D software programs. Scanning stents should be used and two separate CT scans should be taken: One scan of the jaw gently biting on the radiographic guide and a second scan of the guide alone. A BioDental model can then be made from the CT data using a laser to sculpt photopolymer resin into an anatomically accurate, stereolithographic model. The model can be marked to indicate implant placement and angulation and the radiographic scanning guide may be converted into a simple surgical stent (Figure 2; Figure 3; Figure 4; Figure 5).
Collaborative Planning
Implant dentistry requires a high level of collaboration involving the surgeon, the restorative dentist, and the dental laboratory. Although 3-D software can provide an accurate picture of the mandible or maxilla, a BioDental model creates a tactile and visual connection.
For example, the model will show if there is enough bone to support immediate loading or whether bone grafts will be needed before implant surgery. According to Sammy Noumbissi, DDS, of Burtonville, Maryland, “Using a BioDental model, you can have a high level of confidence that the stent is in the right position. By sitting the stent in the model you can see if the bone is deficient.”
The importance of advanced planning is demonstrated in a case where there was danger of hitting the inferior alveolar nerve bundle. According to Dix Densley, DDS, of Hillsboro, Oregon, “Even with a CT scan, it was difficult to determine the correct surgical approach. Having the 3-D model, I was able to perform a complete mock-up. In this particular case, I determined that a much greater lingual approach would be needed than I expected from the CT scan and oral exam. In the clinic, with the model and the stent, having completed a dry run, I was able to place the implant successfully with minimum risk.”
Drill Guides
With a BioDental model there is no need to send the digital file of the CT to your dental laboratory or to the implant manufacturer to fabricate the drill guide. BioDental models are vendor neutral, which means that you can continue to work with the dental labortory you have come to depend on and no software investment is required.
Vendor-supplied 3-D software is both expensive and complex and, although it can provide an accurate and detailed picture, it is difficult and time-consuming to use in making the measurements needed to pinpoint the exact location, angulation, and depth of each drill site. A BioDental model saves time and possible error, and can help the dentist determine whether a bone, mucosa, or tooth-supported drill guide is needed. At the same time, the model clearly shows gingival soft tissue to simplify the planning of flapless surgery if necessary.
According to Densley, “BioDental models minimize guesswork and improve communications with the laboratory. Instead of giving the laboratory measurements of so many millimeters from a reference point, I can now drill a hole in the BioDental model to show exactly where the implant will go so that the drill guide can be made to the exact position, depth, and angle required [Figure 6]. This can be critical. For example, when working close to the sinus, a 5-degree angle change can make a significant difference, and by drilling just a fraction too deep there could be a possibility of breaking into a sinus cavity.”
Immediate Loading
Immediate loading with a premade, implant-supported prosthesis is becoming more and more popular with both patients and clinicians because it eliminates a long, drawn-out procedure. Computer simulation and rapid prototyping with BioDental models reduce chairtime and are invaluable in both one- and two-stage immediate loading procedures because surgery can be planned ahead of placement and stereolithographic models and drill guides can replace the prosthetic impression in the preparation of a premanufactured, customized prosthesis.
According to Jaime Lozada, DDS, director of the graduate program in implant dentistry at Loma Linda University Dental School, Loma Linda, California, “BioDental models absolutely facilitate immediate loading. By using them for surgery, a prosthesis can be made ahead of time and the stability of the implant can be predetermined by looking at the model.”
The Restoration
The model can serve as the foundation in building the optimum esthetic solution. It clearly identifies soft tissue, bone, and existing teeth and can be used to check occlusion. The laboratory, restorative dentist, and patient can all see exactly how the restoration will look.
Conclusion
Dentists who have used stereolithographic models are also adopting them as a standard modality for totally edentulous cases on the mandible and distal extension extractions where the molars have been missing for years and there has been bone shrinkage. According to Robert W. Emery, DDS, co-director of the Washington Institute for Mouth, Face, and Jaw Surgery in Washington, DC, “Stereolithographic modeling has become an essential part of oral and maxillofacial surgery. It allows accurate diagnosis and measurements to be made before surgery is begun.”
For More Information
Biomedical Modeling, Inc
Web: www.biomodel.com
Phone: 1-888-246-6633
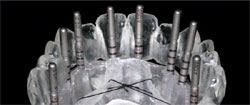 | ||
| Figure 1 Epoxy model showing depth gauge pins, including millimeter markings. | ||
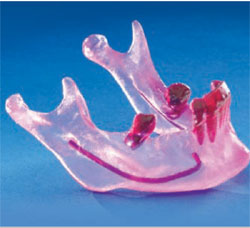 | 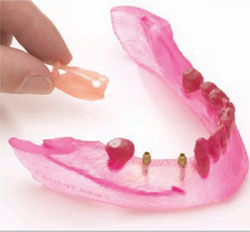 | |
| Figure 2 Acrylic model of a mandible showing the aveolar nerve bundle. | Figure 3 Acrylic model of a patient's mandible and the soft-tissue model of the patient's gums. | |
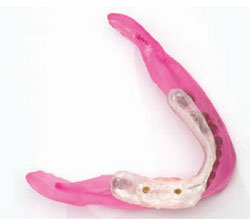 | 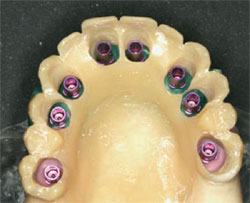 | |
| Figure 4 Acrylic model of a mandible with drill guides and the prosthesis in place. | Figure 5 Acrylic model of a maxilla with an immediate-load prosthesis. | |
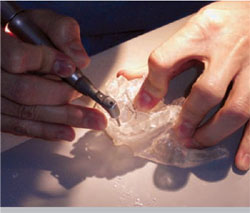 | ||
| Figure 6 A dentist drills the model to show exactly where the implant will go. |



