Material Choice for the Posterior: Function, Longevity, or Esthetics?
Bruce W. Small, DMD, MAGD
Years ago, there were not many choices for restorative materials, particularly in the posterior. Cast and direct gold restorations have been very successfully used since the turn of the century, and the use of porcelain as a restorative material was first reportedin 1903 by Dr. Charles Land.1 Land described the use of porcelain for veneers, inlays, and crowns, and predicted that, “Porcelain as an aid to operative dentistry is gradually developing into one of the most important and valuable branches of the art...it will take the place of many other materials and in numerous instances will prove to be far superior.” This article will primarily discuss the use of gold, ceramic, and direct composite for posterior restorative materials.
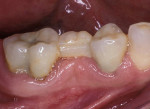
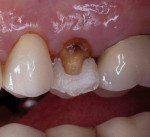
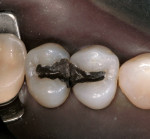
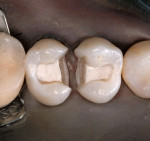
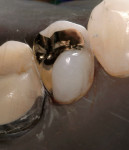
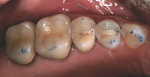
Other materials have been used in the posterior, including various types of amalgam and plastics with varying degrees of success. Direct composites have become popular for smaller restorations, particularly after the introduction of Bis-GMA resins2 and the bonding of these composites to enamel.3 Dentin bonding became commonplace in the 1980s and helped to initiate the esthetic explosion, which still continues. Indirect porcelain systems were introduced to be used as inlays, onlays, and full crowns. In some cases, porcelain was used to replacean entire tooth as a pontic. At the same time, a direct composite (Fulfil, Dentsply Caulk, York, PA) was approved by the American Dental Association as the first composite resin to be used as a posterior restorative material. The floodgates were then opened for researchers, companies, and lecturers to tout tooth-colored posterior restorations. New dental associations and new dental journals were begun and a whole new world of posterior restorative products began to emerge onto the dental marketplace. Unfortunately, frustration and embarrassment came for the practicing dentist who was looking for the promised panacea, and found only partial success (Figure 1 and Figure 2). Many products came and went (eg, Variglass, Artglass, Optec, Mirage, Targis), but the search continues today for a longer lasting composite or ceramic material.
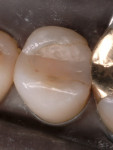
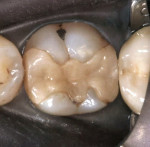
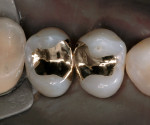
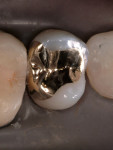
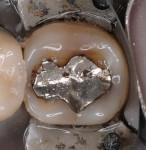
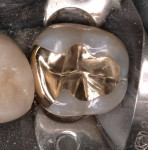
One of the important factors in clinical success or failure is the fit or marginal gap between the restoration and the cavo-surface margin. In a clinical evaluation of 2 ceramic materials, Coelho Santos and colleagues4 reported that the average gap after 2 years was 120 µm. This was primarily a result of washout of the resin cement and the restorations not fitting well enough (Figure 3 and Figure 4).In an unpublished pilot study, Carr and Johnson measured the gap of a cast gold inlay and report a space of and 6).
Functional Decisions
Occlusal function should be the first factor in determining what kind of material should be used in both the anterior and posterior. For a heavy bruxer or a patient with obvious signs of occlusal wear, cast gold should be considered. Cast gold has withstood the test of time and remains the treatment of choice of many dentists. In a Web-based survey, Rosenstiel and colleagues5 asked dentists’ opinions regarding material choice for their own teeth and to estimate longevity. The results were that most dentists have not replaced their traditional metallic restorations with esthetic alternatives. In addition, dentists still choose nonesthetic options (cast gold) for significant numbers of their own restorations. Christensen6 reported that in a poll of members and guests at a meeting of the American Academy of Restorative Dentistry asking what material they prefer in their own mouths, cast gold was the choice for mandibular first and second molars and maxillary first molars. Unfortunately, Heinikainen and coworkers7 reported that when re-treating failed posterior restorations, 92% of dentists in their study chose direct composite. In a related article, Haj-Ali and colleagues8 stated that, unfortunately, the current material choice patterns of restorative dentists “suggest a low reliance on evidence-based informational resources in the practice of clinical dentistry.”
Strength is needed in many if not all posterior cases because of the forces of occlusion, and cast gold offers the strongest option. Contacts remain in the ideal morphology when cast gold is used and allow for easily cleansable surfaces (Figure 7, Figure 8, Figure 9, Figure 10 and Figure 11). Pressed or fired ceramics do not have the strength of gold and should not be promised as a solution for patients. As previously mentioned, some newer products have shown early promise (Figure 12) and look acceptable when first placed, but none have the long-term literature to support their routine use in clinical practice, particularly when used in heavy function (Figure 13 and Figure 14).
Longevity Decisions
If the restorative dentist and patient are interested in longevity, there is only one choice according to the dental literature. In an evaluation of 1,314 cast gold restorations in a single dental practice, Donovan and Simonsen9 found that the castings had an overall survival rate of 95.4% for restorations in vivo for up to 52 years. Mjor and Medina10 reported on 2,564 gold restorations (1,689 cast gold and 875 direct gold) and found the mean age of all restorations in situ was 18.5 years.
In a recent article by Wagner and colleagues,11 the longevity of partial coverage cast gold was compared to similar ceramic restorations. The median length of time in vivo was only 60 months, but the results showed little statistically significant differences between the longevity of the 2 materials.
Unfortunately, there are very few long-term clinical reports on indirect composite or ceramic restorations. A favorable trend is appearing for indirect ceramics; however, more randomized long-term clinical trials are necessary. Many factors are being studied regarding ceramics, including preparation syle,12 different core materials,13 and mode of failure.14 Only time will tell if ceramics—or some new type of material which has not yet been developed—will take the place of cast gold regarding longevity.
Esthetic Considerations
For most (but not all) patient populations, esthetics is a factor in choosing dental restorations in the posterior. Some patients do not mind showinga little gold during a full smile, while others are bothered by it and insist on only tooth-colored restorations. Part of the problem in this area begins with the restorative dentist and his or her lack of education concerning cast gold, particularly in preparation techniques.When a previously placed maxillary restoration flares out to the buccal enough to be seen, then gold may not be an esthetically acceptable option. If the mesiobuccal wall is close to being visible and that wall is prepared first, it is possible to prepare the remainder of the preparation to draw with that wall and finish with a restoration that can hardly be seen. In addition, by keeping the mesiobuccal wall very straight and parallel to the long axis of the tooth, the restoration often blends into the buccal line angles of the teeth in the quadrant.
Other influences that affect patients’ esthetic decisions are television, Hollywood, and magazines, which show models and actors with perfectly straight, white teeth. Of course, this does not occur often in reality and is at times difficult to attain; however, white and bright is requested by many patients. It then becomes the restorative dentist’s responsibility to inform the patient of the positives and negatives of using tooth-colored restorative materials and/or whitening techniques.
Conclusion
During the last 25 years, many esthetic alternatives to cast gold and porcelain-fused-to-metal crowns have been introduced. Very few of them have survived the test of time. When compared with the longevity of gold, no esthetic product can compare. The dental literature has few, if any, long-term studies that have a 95% success rate after 52 years.As previously mentioned, the large majority of practicing dentists do not use the refereed dental literature as an information source. The author has placed many tooth-colored restorations over the years and has found that many have fractured. After learning, watching, reading, and placing many cast gold restorations, the author has experienced very few remakes along with explanations and excuses to patients.
Material choice in the posterior comes down to the dentist’s philosophy of dentistry and his/her courage to not place a composite or ceramic restoration in any area of the mouth where it may fracture prematurely. That leads to the second factor, which is the patient’s expectation. Some dentists feel, as do insurance companies, that a restoration should only last 5 years and then be replaced with something larger and often times more invasive. The goal of restorative dentistry in some practices is to construct a restoration that may last as long as possible,thereby conserving tooth structure and limiting endodontics and crowns (not necessarily in that order). The choice is yours. Read the literature, watch your patients, and decide what is best for your mouth as well as your patients—hopefully it will be the same.
References
1. Land CH. Porcelain dental art. Dental Cosmos. 1903;45(8);615-620.
2. Bowen RL. Dental filling materials comprising vinyl silane treated fused silica and a binder consisting of the reaction product of bis phenol and glycidyl acrylate. US Patent 3 066 112. 1962
3. Buonocore MG. A simple method of increasing the adhesion of acrylic filling materials to enamel surfaces. J Dent Res. 1955;34(6):849-853.
4. Coelho Santos MJ, Mondelli RF, et al. Clinical evaluation of ceramic inlays and onlays fabricated with two systems:two-year clinical follow up. Oper Dent. 2004;29(2): 123-130.
5. Rosenstiel SF, Land MF, Rashid RG. Dentists molar restoration choices and longevity: a web-based survey. J Prosthet Dent. 2004;91(4): 363-367.
6. Christensen G. Ask Dr. Christensen. Dent Economics. 2006;96(1):78.
7. Heinikainen M, Vehkalahti M, Murtomaa H. Retreatment decisions for failed posterior fillings by Finnish general practitioners Community Dent Health 2002;19(2):98-103.
8. Haj-Ali RN, Walker MP, Petrie CS, et al. Utilization of evidenced-based informational resources for clinical decisions related to posterior composite restorations. J Dent Educ. 2005;69(11): 1251-1256.
9. Donovan T, Simonsen RJ, Guertin G, et al. Retrospective clinical evaluation of 1,314 cast gold restorations in service from 1-52 years. J Esthet Restor Dent. 2004;16(3):194-204.
10. Mjor I, Medina J. Reasons for replacement and age of gold restorations in selected practices. Oper Dent. 1993;18(3):82-87.
11. Wagner J, Hiller KA, Schmalz G. Long term clinical performance of gold alloy vs ceramic partial crowns. Clin Oral Investig.2003;7(2): 80-85.
12. De Jager N, Pallav P, Feilzer AJ. The influence of design parameters on the FEA-determined stress distribution in CAD/CAM produced all ceramic dental crowns. Dent Mater. 2005;21(3):242-251.
13. Vult von Steyern P. All ceramic fixed partial dentures. Studies on aluminum oxide and zirconium dioxide-based ceramic systems. Swed Dent J Suppl 2005;(173):1-69.
14. Guazzato M, Proos K, Sara G, et al. Strength, reliability, and mode of fracture of bilayered porcelain/core ceramics. Int J Prosthodont 2004;17(2): 142-149.
About the Author
Bruce W. Small, DMD, MAGD
Private Practice
Lawrenceville, New Jersey