A New Sequence for Fully Guided, Fixed, Immediate Load Full-Arch Dental Implant Reconstruction
Revolutionary CAD/CAM technology enhances patient treatment outcomes and clinical efficiency
Steven R. Tucker, DMD | Samuel Schmitz, DDS
Fully guided CAD/CAM dental implant surgery as defined by the author is an implant vendor-based software/surgical protocol that allows the surgical insertion of a dental implant into a prepared osteotomy site using a custom patient specific template or jig, which replicates a predetermined x, y, and z axis path of insertion at a prescribed depth. The planning and execution of the surgical plan requires preoperative computed tomography (CT)/cone-beam CT (CBCT) patient data, implant planning software, digitized representation of the dentoalveolar structures, and an implant platform specific instrument kit. The patient data sets use open source DICOM (Digital Imaging and Communications in Medicine) .dcm and STL (STereoLithography) .stl file formats. The digitally planned guided implant surgery innovations—Simplant (Dentsply Sirona, www.dentsply.com) and NobelGuide (Nobel Biocare, www.nobelbiocare.com)—replaced Nobel Biocare’s model-based guided protocol when CBCT scanners were introduced.1
The convergence of digital technologies in the field of dentistry has created a paradigm shift in the profession’s clinical protocols and procedures regarding treatment modalities for the restoration of “form and function.” Today’s technological innovations include advances in 3D diagnostic radiography, clinical photography, additive manufacturing, subtractive manufacturing, surface mapping, material science, and CAD/CAM computer software engineering. This case presentation explores today’s new digital dentistry revolution and how the convergence of technologies has improved patient outcomes by enhancing safety, accuracy, efficiency, and timeliness.
The All-on-X treatment concept is a cost-efficient, graftless solution that provides patients with a fixed full-arch prosthesis on the day of surgery. The concept includes the following:
1. Full-arch rehabilitation with only four implants: Two axial anterior implants and two implants tilted up to 45˚ in the posterior
2. Immediate function (fixed acrylic bridge) for patients meeting criteria for immediate loading of implants
3. A graftless procedure 2,3,4,5
When treating the maxilla, one should consider additional implants secondary to the issues of bone quality and quantity in the maxilla, hence the All-on-X concept. In addition, Drs. Jivraj and Zarrinkelk advocate the six S’s of success: space, spread, stability, skill, speed, and sequence.6,7
While the surgical component has seen innovations in implant design, implant planning software, guided surgery, and autologous biologics, the prosthetic component, other than material science, has lagged behind clinically and been laborious to execute. The chairside prosthetic conversion is time consuming and demanding. A new patented laboratory process by Daniel Llop, CDT, nSequence (www.nsequence.com), has merged fully guided dental implant surgery with cutting edge CAD/CAM dental implant prosthetics. His protocol simplified the conversion process, improved accuracy, increased efficiency, and reduced chairtime for the patient, staff, and doctor significantly.
The case presentation below is an example of how the accuracy of CAD/CAM guided dental implant surgery coupled with CAD/CAM guided dental implant prosthetics improves the clinical parameters of care. It will emphasize the diagnostic, treatment planning, surgical, and prosthetic aspects of this new treatment modality.
Case Presentation
A 67-year-old woman presented with a chief complaint of mobile teeth and an ill-fitting maxillary removable partial denture. She wanted a more esthetic smile and improved retention of her maxillary prosthesis. Dental history revealed that the patient always had an “underbite.” Medical history was positive for hypertension and occasional smoking.
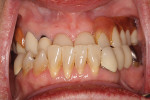
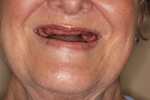
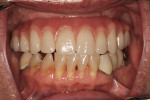
The clinical and radiographic examination revealed horizontal alveolar bone loss in the maxilla and mandible, mobile tooth No. 5, furcation bone loss involving No. 19, nonfunctional tooth No. 15, chronic periapical inflammation of tooth No. 31 (abutment tooth for fixed partial denture Nos. 29 through 31) with root fracture, gingival recession, super eruption of teeth Nos. 23 through 26, maxillary removable partial denture with x-bite, bilateral hyperplastic maxillary tuberosities, and Class III malocclusion (Figure 1). It was thought that the Class III malocclusion could either be acquired as a result of posterior bite collapse or a true mild skeletal mandibular prognathism, or a combination (Figure 2). A phased treatment plan was formulated.
Phase I
Phase I would proceed with a maxillary full mouth extraction of the terminal dentition involving teeth Nos. 5 through 9, and No. 15 with insertion of a maxillary immediate complete denture. In addition, the right mandibular fixed partial denture would be sectioned, and fractured tooth No. 31 would be surgically extracted. This approach would allow the patient to try a full palatal coverage removable prosthesis and would allow the dental reconstructive team the chance to assess lip support and correction of her anterior posterior discrepancy by either opening the vertical dimension of occlusion (VDO) or advancing the prosthetic dentoalveolar segment anteriorly to correct her Class III relationship. If the latter was planned, it was obvious that either the super erupted mandibular incisors would have to be extracted or a reduction enameloplasty would be required to allow advancement of the maxillary prosthesis. The advancement would require a fixed immediate load full arch prosthesis via an All-on-X concept.
Phase II
Phase II began after adequate healing of Phase 1. Acquisition of diagnostic data included CBCT, digital impressions, digital extra-oral, and intraoral photography, cephalometric analysis, active smile analysis, and reassessment of mould and shade selections. In addition, ridge display on smiling with the prosthesis out of the patient’s mouth was recorded with digital photography. Ridge display on smiling was crucial in determining if vertical bone reduction would be necessary to hide the transition line of the prosthesis on smiling (Figure 3). The CBCT scan was evaluated as per the Bedrossian Zone I, Zone II, and Zone III bone quantity assessment.8 It was determined that adequate bone was present in Zones I and II and that vertical alveolar bone reduction would be necessary based on the patient displaying residual ridge when smiling without her maxillary denture. The case presentation was reviewed with the patient for Phases II and III, which use guided implant surgery with immediate load protocol—“Teeth in a Day” with an All-on-X concept and nSequence guided prosthetics. Phase II called for the advancement of the maxillary dentoalveolar prosthetic complex to create an end-to-end Class III anterior posterior relationship. Following the maxillary immediate load protocol of Bedrossian, the temporary maxillary prosthesis was worn for 6 months before removal.2 The prosthesis was removed, ultrasonically cleaned, and replaced following resonance frequency analysis (Implant Stability Quotient, ISQ) using an Osstell Smart Peg (www.osstell.com) specific for Nobel Biocare Multi-unit Abutments. The final maxillary fixed screw retained full arch prosthesis was delivered before commencing mandibular reconstruction. MAVEN Pro dental implant planning software (nSequence) was used and a planning session conducted via Go to Meeting.
Phase III
Phase III will follow the same protocol, but for the mandible. Because the maxillary incisal edge and incisal position had been established, the mandibular dentition will be extracted during the same surgery as implant placement. Again the nSequence guided prosthetic protocol will be followed. The mandibular dentoalveolar prosthetic complex will be positioned posteriorly, completing the correction of the anterior posterior discrepancy. The treatment plan is to extract teeth Nos. 19 and 22 through 29, and reduce the mandibular alveolar bone to create restorative space as indicated using the foundation/bone reduction guide, and the guided All-on-4 treatment concept.
Surgical Procedure
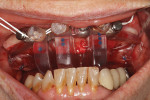
Following satisfactory deep IV sedation with nitrous oxide/oxygen and local anesthesia, the patient’s nSequence start bite was inserted to confirm her occlusal setup. A slightly palatal crest of the ridge incision was made from the right second molar area to the left second molar area. A lateral vertical releasing incision was extended toward the third molar area bilaterally. A buccal and palatal mucoperiosteal flap was elevated to expose the maxillary alveolar ridge. The nasopalatine neurovascular bundle was sacrificed to allow for complete seating of the foundation/bone reduction guide. The right and left side of the palate flap was sutured together to create better access to the depth of the hard palate (Figure 4).
The foundation guide was seated anteriorly and rotated posteriorly into position to allow for the undercut of the anterior maxilla (anterior-posterior path of insertion). When the foundation guide was fully seated the mandible was auto rotated to check the occlusal index of the mandibular incisors on the foundation guide struts. Once the proper positioning of the foundation guide was confirmed, it was anchored to the maxilla with three 1.5 mm Nobel Biocare Anchor pins (Figure 5). The transalveolar osteotomy anchor pin sites were prepared with a 1.5 mm twist drill in a contra-angle handpiece at 2,000 RPMs with copious irrigation. The three struts of the foundation guide were removed, exposing the alveolar ridge that was planned for reduction.
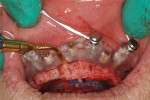
A piezosurgery unit with a self-contained irrigation system and a microsaw blade was then used to perform an anterior maxillary ostectomy as prescribed by the foundation/bone reduction guide (Figure 6). The maxillary surgical implant guide was then snapped on to the foundation guide using the indexed seating cogs. The NobelGuide drilling protocol for the NobelActive implants was then used to create the five osteotomy sites for the implants.9 This was again done with copious irrigation at 2,000 RPMs. Drill stops had been placed on the twist drills at the prescribed depth using the Nobel Biocare Guided Drill Stop Kit. Depth control was accomplished when the stops hit the guided drill guide insert for each osteotomy site.
Implant mounts were then attached to each implant and hand inserted into the osteotomy site through the surgical guide at each site. The implants were rotated counterclockwise until they fell into the tapped grooves at each site. In the nSequence protocol, the lack of intimate contact between the original NobelActive Guided Implant Mount and the surgical guide sleeve is overcome by using NobelReplace Conical Connection Implant Mounts. NobelReplace Conical Connection Implant Mounts are in intimate contact with the surgical guide sleeves, thus assuring more accurate x, y, and z axis 3D positioning and depth control. Next, each implant was manually torqued with the NobelActive 70 ncm torque wrench until the implant mount came into contact with the guide sleeve. 35 ncm manual torque or mechanical readings (per implant) are considered adequate for immediate load when cross-arch stabilization is utilized in All-on-X immediate load cases.4,10,11 Drs. Jensen and Adams have advocated that, if the 4-implant scheme has a composite insertion torque of 120 N-cm and vertical stability of all 4 implants is present, immediate function can be allowed.12
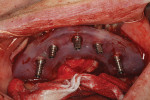
A flat surface of the implant mount was aligned with the prescribed blue markings on the surgical guide (Figure 7). The implant mounts were then loosened and removed from the implants with the surgical guide still in place on the anchored foundation guide. The surgical guide was then removed, leaving the foundation guide in place. Then, the surgical site was irrigated.
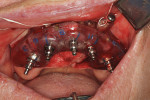
The multi-unit abutment (MUA) rotation guide was snapped into the foundation guide using the cog index (Figure 8). The MUAs, temporary coping multi-unit titanium with prosthetic screw (Temporary Ti Cylinders), and block-out rods all come packaged by nSequence in trinket plastic boxes. They are specific for each implant site and the Ti cylinders have been precut for correct height in relation to the prosthesis. These have to be cataloged, packaged, and autoclaved prior to surgery. The screw holes of the angled MUAs were aligned with the blue marks on the MUA rotation guide. Angled MUAs (17˚ and 30˚) were torqued to 15 ncm while 0˚, straight MUAs, were torqued to 35 ncm. Once all the MUAs had been placed, the guide was removed.
The temporary Ti cylinders were placed on their prescribed MUA and the prosthetic screw was hand tightened. The flat surface of the temporary Ti cylinder with the etched implant site number was oriented to the buccal surface. Block-out rods were placed in the cylinders to prevent acrylic from getting in the cylinder.
The maxillary gasket was then placed on the foundation guide using the index cogs (Figure 9). The silicone gasket prevents acrylic from locking the prosthesis to the MUAs under cuts, averting its irretrievability. The prosthesis was tried on after each temporary Ti cylinder was placed to check for passivity of fit between the cylinder and the hole in the prosthesis. The prosthesis was nested in the foundation guided with the gasket between them.
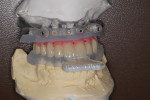
The bite maxillary bridge to mandibular teeth index was then inserted and the patient’s mandible rotated closed into the bite index (Figure 10). This position represents maximal intercuspation. When the bite index verified the occlusal setup, the prosthesis was ready to be bonded (luted) to the temporary Ti cylinders. Vaseline was lightly coated on the prosthesis in all areas except the injection holes and luting holes (Figure 11).
The prosthesis was again placed over the cylinders and gasket. The bite index was inserted and the mandible rotated into the bite index. Dual cure denture repair/reline acrylic was injected into the injection holes while the patient’s mandible was secured in the bite index. A curing light was then used to accelerate the polymerization of the acrylic. After curing, the bite index was removed. Now that the palatal surface of the prosthesis was visible, additional acrylic was injected as needed. The block-out rods were removed from the Ti cylinders and the prosthesis was removed. Resonance frequency analysis with an Osstell unit was performed on each MUA to obtain baseline readings.
MUA healing caps were placed on the MUAs. The surgical site was copiously irrigated and the incision closed in an interrupted fashion with chromic gut sutures. A tissue punch in a contra-angle was used over the healing caps on the palatal aspect to remove excess palatal tissue.
The MUA Healing Caps were removed and the prosthesis was seated over the MUAs. The prosthesis was then secured to the MUAs using the prosthetic screws of the temporary Ti cylinders. The screws were hand tightened. Cotton pellets were placed and covered with injectable fine body PVS impression material. The occlusion was checked and adjusted. Marcaine .5% with 1:200,000 epinephrine was infiltrated over the maxillary surgical site for postoperative analgesia. A postoperative radiograph was obtained (Figure 12).
The maxillary prosthesis was worn for 6 months, removed, and cleaned. Implant stability was examined and Osstell testing repeated. The prosthesis was replaced and the patient was referred back to their general dentist for fabrication of the final prosthesis.
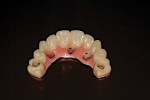
To date, Phase I and II have been completed. The final maxillary fixed screw retained prosthesis has been delivered (Figure 13). The patient’s quality of life has improved significantly from the restoration of form and function (Figure 14). The new prosthetic concept allowed a second pick up with the Clear Denture component of the nSequence Guided Prosthetic kit. The duplicate pick up allowed the Clear Denture to serve as a verification jig, occlusion rim, try-in, and open tray fixture level impression. Therefore, the number of prosthetic appointments was reduced. The patient is awaiting completion of Phase III of her treatment plan.
Conclusion
A new surgical/prosthetic protocol has been developed merging CAD/CAM fully guided dental implant surgery with CAD/CAM full arch immediate load prosthetics. The nSequence Guided Prosthetic protocol has delivered on its break through technologic innovation to improve patient outcomes by enhancing safety, accuracy, efficiency, timeliness, and patient satisfaction (Figure 15).
Disclosure
The authors have no relevant financial relationships to disclose.
References
1. Orentlicher G, Abboud M. Guided surgery for implant therapy. Oral Maxillofac Surg Clin North Am. 2011;23 (2):239-256.
2. Bedrossian E. Systematic Pretreatment Evaluation of the Edentulous Maxilla. In: Bedrossian E. Implant Treatment Planning for the Edentulous Patient; A Graftless Approach to Immediate Loading. St. Louis, MO: Mosby Elsevier;2011:33-42.
3. Dada K, Daas M. All-on-4 Concept. In: Malo P, et al. Esthetic Implant Restoration in the Edentulous Maxilla, A Simplified Protocol. Hanover Park, IL: Quintessence;2014:175-194.
4. Malo P, de Araujo Nobre M, Lopes A, et al. A longitudinal study of the survival of All-on-4 implants in the mandible with up to 10 years of follow-up. J Am Dent Assoc.2011;142(3):310-320.
5. Nobel Biocare. All-on-4® Treatment Concept Procedures Manual. https://www.nobelbiocare.com/content/dam/GMT/Produced%20Material/Manual/840/PRODMTRL_0009871_1_231973.pdf.download/79360B_All-on-4%20treatment%20concept%20manual%2015.1_GB_US.pdf. Accessed May 1, 2017.
6. Jivraj S, Zarrinkelk H. Graftless Solutions in Implant Dentistry: Part 1. Implants: The International C.E. Magazine of Oral Implantology. 2012;3:8-19.
7. Jivraj S, Zarrinkelk H. Graftless Solutions in Implant Dentistry: Part 2. Implants: The International C.E. Magazine of Oral Implantology. 2012;4:8-16.
8. Bedrossian E, Sullivan RM, Fortin Y, et al. Fixed-prosthetic implant restoration of the edentulous maxilla: a systematic pretreatment evaluation method. J Oral Maxillofac Surg. 2008;66(1):112-122.
9. Babbush CA, Kutsko GT, Brokloff J. The All-on-four immediate function treatment concept with NobelActive Implants: a retrospective study. J Oral Implantol. 2011;37(4):431-445.
10. Maló P, Friberg B, Polizzi G, Gualini F, Vighagen T,Rangert B. Immediate and early function of Brånemark System implants placed in the esthetic zone: a 1-year prospective clinical multicenter study. Clin Implant Dent Relat Res. 2003;5(Suppl 1):37-46.
11. Cooper LF, De Kok IJ, Rojas-Vizcaya F, Pungpapong P, Chang SH. The immediate loading of dental implants. Compend Contin Educ Dent. 2007;28(4): 216-225.
12. Jensen OT, Adams MW. Anterior Sinus Grafts for Angled Implant Placement for Severe Maxillary Atrophy as an Alternative to Zygomatic Implants for Full Arch Fixed Restoration: Technique and Report of 5 Cases. J Oral Maxillofacial Surg. 2014;72 (7):1268-1280.
About the Authors
Steven R. Tucker, DMD
Private Practice
Oral and Maxillofacial Surgery
Owensboro, Kentucky
Assistant Professor
Division of Oral and Maxillofacial Surgery
University of Kentucky
College of Dentistry
Lexington, Kentucky
Samuel Schmitz, DDS
Private Practice
Newburg, Indiana