Treating Maxillary Central Incisors Following a Significant Traumatic Event
A 28-year treatment history
Joseph R. Greenberg, DMD, FAGD
Much can be learned from the sequelae of treatment decisions played out over these 28 years. Good decision-making may be more important than treatment skills or materials employed, and both good and questionable ones are displayed in this case.
Restorative dentistry is technically demanding, and even the best dentists make errors at times. When these mishaps occur, it may be difficult or ill advised to correct them. The consequences that ensue can stimulate hindsight recommendations, but also show that there are few statistics or evidence bases that trump the requests and needs of each individual patient as events unfold.
Case Presentation
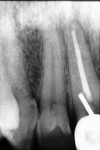
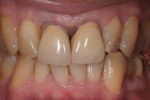
This patient first presented in 1988, having suffered coronal fractures and related trauma to both maxillary central incisors in a train accident the year prior. The patient was previously treated with endodontic therapy, a post/core foundation, and a crown for the right central incisor, and a matching crown for the left central incisor. A radiograph taken in 1991 (Figure 1) shows that the post placed in the right central incisor does not follow the path of the root canal filling. The patient was asymptomatic and satisfied with the appearance of both crowns. There was no apparent periodontal, pulpal, or periapical pathology other than marginal gingivitis, which was treated. Published guidelines for teeth that have experienced concussion recommend no treatment for teeth that are asymptomatic and show positive response to pulp testing, as was the case with the maxillary left central incisor. The monitoring period is listed as at least one year.1
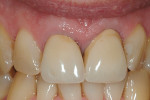
In 1994, the maxillary left central incisor became symptomatic and required endodontic treatment. There was no other explanation for this pathology, other than the traumatic injury of 1987. The endodontist examined the status of the right central incisor and opined that there was no fracture or perforation related to the post, although he did find some apical resorption. This would have been the time to remove and redirect the post in the right central incisor, as new crowns were planned and the previous crown removed. The end of the post was buried in the core material and the entire complex seemed secure in the tooth. The overriding concern was that an attempt to remove the misdirected post might result in root fracture and loss of that tooth. As a result, it was left undisturbed and new porcelain-fused-to-metal (PFM) crowns were placed for both central incisors in 1996 (Figure 2).
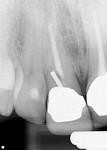
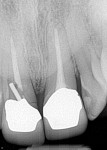
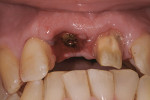
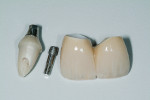
A follow-up radiograph of the maxillary central incisors in 2011 suggested pathologic changes related to the aberrant post, but the patient was asymptomatic at that time (Figure 3). In 2013, the tooth became “sore and achy,” a lingual probing was found, and a flap was lifted on the lingual aspect, revealing an area of resorption. The tooth structure was made sound and was restored with a glass ionomer/resin. The patient was comfortable for nearly 2 years and then became symptomatic again. A radiograph suggested horizontal/vertical fracture of the tooth apical to the cementoenamel junction (CEJ) (Figure 4). The coronal portion of the tooth was mobile and sore to palpation. With local anesthesia, the fractured portion was removed (Figure 5). It seemed that the post did contribute significantly to the fracture.
Important diagnostic factors for consideration at that time were:
• Low lip line/smile esthetic display 2
• Thick, flat periodontal architectural biotype3
• The incisal lip of the labial bony socket was intact as was the labial socket wall.4
These factors were favorable for various treatment options:
• Extraction of the remaining root of the maxillary right central incisor and placement of a dental implant, abutment, and new crowns
• Extraction of the remaining root of the maxillary right central incisor and fabrication of a fixed dental bridge from the right lateral incisor to a new abutment crown on the left central incisor
• Soft and hard tissue surgery to expose sound tooth structure, new post and core, and a new crown for the right central incisor.
The patient understood that the last option had the most risk and the poorest prognosis.
The patient had immediate business obligations, which influenced his decision-making. He also had a close friend who had recently endured a rather negative experience with dental implant treatment, so he opted for surgical exposure and repair of the fractured tooth, with the understanding that either of the other two options might still be pursued at a later time. He promised to reconsider the other two options should the need arise. He was informed that the soft and hard tissues removed during the crown exposure surgery might compromise the gum line and interdental esthetics of any dental prosthetic option later on. He understood that his normal smile display did not reveal most of the gum line areas of his front teeth. The clinical situation did allow for a primarily palatal approach to the crown exposure surgery, but the lingual aspects of the interdental papillae were compromised. A short-term postoperative photograph of the area is shown in Figure 6.
Unfortunately, a fistula developed 2 months following treatment and an apical fracture was diagnosed. The patient agreed to extraction and dental implant placement for the maxillary right central incisor and a new crown for the left central incisor. This allowed an immediate provisional prosthetic solution and a more predictable final dental esthetic outcome. He did not want his maxillary left lateral incisor prepared for an abutment crown, as would have been required for the three-unit fixed prosthesis option.
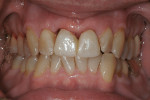
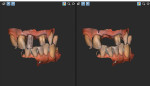
The fractured tooth was extracted and a 6 mm x 13 mm dental implant (Hiossen, www.hiossen.com) was immediately placed with a 6 mm x 4 mm healing abutment (Figure 7). No flap access, graft materials, or sutures were used. Because the treatment plan included a new crown for the adjacent left central incisor, a fixed cantilevered provisional prosthesis was fabricated, which placed no load on the new implant (Figure 8). Fourteen weeks later, the provisional bridge was removed, final preparation for the natural central incisor made, and impression scans for the tooth and dental implant were recorded (Figure 9). The patient was very pleased with the scanning process experience and most appreciative of our investment in this technology.
Obtaining Dental Impressions
Recent reports5 state concerns about the growing shortage of traditionally trained dental laboratory technicians worldwide. This counters the increasing numbers of dental school graduates and the rise in retirement age of practicing dentists.6,7 It seems that there will be fewer dental technicians prepared to service dentists who use elastomeric impressions and require solid models, dies, waxing, casting, and various stages of metal work. One answer invites dentists to purchase and learn the use of intraoral impression scanners and get into the digital workflow. Clinicians can be confident in the accuracy of CAD/CAM based on intraoral scanner data as described in recent publications.8,9
There are many intraoral impression scanners in the dental marketplace today; a recent publication lists a total of eight, all with different requirements, specifications, and warranties.10 The CS 3500 (Carestream Dental, www.carestreamdental.com) is a compact intraoral scanner that can take 2D and 3D color images. It is portable with a USB cable that can be plugged into any workstation. It has an ergonomic shape, a slim scanner head and requires no powder. The CS 3500 captures still images, which are stitched together by the software until a complete dimensional impression is made. A light guidance system aids in the data capture during the image acquisition process. The speed of image capture can be adjusted by the operator. The software generates a stereolithic (STL) file, which can be electronically sent to the dental laboratory for uploading and restorative fabrication. Solid models and dies, waxing, and casting procedures become optional in this process.
The treatment plan for this patient included a custom abutment (zirconia body with titanium metal screw insert), and splinted final crowns for the central incisors.11 The patient was not averse to splinting and was not comfortable with the possibility of future incisal edge discrepancies or open tooth contacts resulting from migration of the natural teeth adjacent to the dental implant, as have been reported.12,13
At the first try-in of the new work, the custom abutment was evaluated and overall healing assessed. The interdental papilla between the right lateral incisor and the new dental implant was diminished by the crown exposure surgery, as previously described. The patient did notice this “dark space” between the right lateral incisor and the pontic of the provisional prosthesis, so it was decided to augment the contour of the mesio-labial surface of the maxillary right lateral incisor with direct composite resin (Point4™, Kerr Dental, www.kerrdental.com) to facilitate space closure of the gingival embrasure between the natural lateral incisor and the dental implant restoration (Figure 10). The final restoration would be designed to follow the recommended guidelines for the distance from the bottom of the contact point to the bony crest for both papillae—mesial and distal to the implant.14
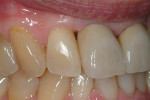
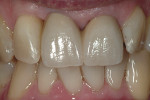
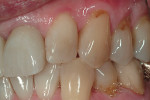
A short-term follow-up of the final restoration is pictured in Figure 11 through Figure 13.
Final Considerations
Although a long-term postoperative photograph is not yet available, it seems that the interdental papillae between the maxillary right lateral and central incisors, and between the two central incisors are filling in. In this case, the patient had the option of choosing shade matching with the maxillary lateral incisors or with the four mandibular incisors. He chose the latter.
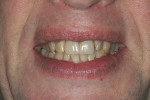
The patient seems well satisfied with the final outcome and we anticipate a favorable long-term prognosis. His low lip line smile display continues to forgive most prosthetic dental shortcomings (Figure 14).
Acknowledgment
The author wishes to thank Mr. John Aguirre, Carestream Dental laboratory representative, for his technical advice and for preparation of the image shown in Figure 9.
Disclosure
The author has no relevant financial relationships to disclose.
References
1. Dental trauma guidelines, International Association of Dental Traumatology, 2012. www.dentaltraumaguide.org.
2. McLaren E, Culp L. Smile analysis. J Cosmet Dent. 2013;29(1):94-108.
3. Sanavi F, Weisgold AS, Rose LF. Biologic width and its relation to periodontal biotypes. J Esthet Dent. 1998;10(3):157-163.
4. Tarnow DP, Chu SJ, Salama MA, et al. Flapless postextraction socket implant placement in the esthetic zone: part 1. The effect of bone grafting and/or provisional restoration on facial-palatal ridge dimensional change—a retrospective cohort study. Int J Periodontics Restorative Dent. 2014;34(3):323-331.
5. Sailer I. Digital Technologies – New Materials, New Restorative Options, Unlimited Indications. Presentation to the Greater New York Academy of Prosthodontics. 2015. New York, New York.
6. Solomon E. The future of dental practice: demographics. Dental Economics. http://www.dentaleconomics.com/articles/print/volume-105/issue-4/macroeconomics/the-future-of-dental-practice-demographics-patients-professionals-and-procedures.html. Accessed November 1, 2016.
7. 2013 Survey of Dental Practice. American Dental Association Health Policy Resources Center.
8. Patzelt SB, Bishti S, Stampf S, Att W. Accuracy of computer-aided design/computer-aided manufacturing-generated dental casts based on intraoral scanner data. J Am Dent Assoc. 2014;145(11):1133-1140.
9. Masri R, Driscoll CF, Kim SJ, Wahle WM. Digital dentistry: the golden age for diagnosis and treatment planning. Inside Dentistry. 2016;12(1):30-38.
10. Intraoral Scanners/Digital Impressions. Digital Workflow Product Resource Guide. Inside Dentistry. 2015;11(7 Suppl):6-7.
11. Greenstein G, Cavallaro J, Smith R, Tarnow D. Connecting teeth to implants: a critical review of the literature and presentation of practical guidelines. Compend Contin Educ Dent. 2009;30(7):440-453.
12. Daftary F, Mahallati R, Bahat O, Sullivan RM. Lifelong craniofacial growth and the implications for osseointegrated implants. Int J Oral Maxillofac Implants. 2013;28(1):163-169.
13. Greenstein G, Carpentieri J, Cavallaro J. Open contacts adjacent to dental implant restorations: etiology, incidence, consequences, and correction. J Am Dent Assoc. 2016;147(1):28-33.
14. Choquet V, Hermans M, Adriaenssens P, et al. Clinical and radiographic evaluation of the papilla level adjacent to single-tooth dental implants. A retrospective study in the maxillary anterior region. J Periodontol. 2001;72(10):1364-1371.
About the Author
Joseph R. Greenberg, DMD, FAGD
Clinical Professor, Restorative Dentistry
The Kornberg School of Dentistry at Temple University
Philadelphia, Pennsylvania
Clinical Professor of Periodontics
The University of Pennsylvania School of Dental Medicine
Philadelphia, Pennsylvania
Private Practice
Villanova, Pennsylvania