Same-Day Monolithic Lithium Disilicate Ceramic Bridges
An esthetic and practical alternative to PFM bridges
Dhaval Patel, DDS
For a long time, porcelain-fused-to-metal (PFM) bridges were the treatment of choice for fixed prosthetics for patients missing one or more teeth. However, through the progress made with CAD/CAM systems1,2 and products within the last few years, we now have the ability to make same-day bridges in practice. There are many benefits of making the bridge this way. The patient does not have to wear a temporary for a few weeks and a second visit is not required, saving valuable time for the patient and the dental office. e.max® (IPS e.max, Ivoclar Vivadent, www.ivoclarvivadent.com) is a highly esthetic material, and with the help of a little customization, the final result can be made to look more esthetic in most cases than an opaque looking PFM bridge.
Case Presentation
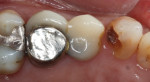
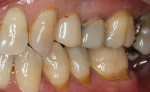
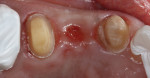
A 52-year-old healthy patient presented to the practice with the chief complaint of a broken tooth on the upper left. Upon examination, it was discovered that a large composite filling had fallen off tooth No. 11 with recurrent decay (Figure 1). Tooth No. 12 had a cantilever bridge supported by tooth No. 13. There was recurrent decay under the abutment of tooth No. 13 and the patient was not very happy with the esthetics of the acrylic-fused-to-metal bridge that was done more than 20 years ago (Figure 2). All treatment options were discussed with the patient, including an implant, and the patient chose to replace the cantilever bridge with a three-unit bridge from tooth Nos. 11 through 13.
Teeth Preparation
All the recurrent decay was removed from tooth No. 11 and a composite build-up was completed. The cantilever bridge on tooth No. 13 was removed and the recurrent decay at the margins was cleaned and prepped for an abutment. The preparations were properly evaluated to make sure it had enough reduction both on the axial and occlusal to meet the requirements of the restorative material, IPS e.max. The central fissure requires 1.5 mm of reduction, along with 2 mm of reduction on the cusps and about 1 mm on the axial walls. A heavy chamfer or a shoulder margin is acceptable. Care was also taken to make sure there were no undercuts on the preparations of the abutment teeth.
Scanning and Designing Process
For this case, CEREC Biogeneric Individual software (Dentsply Sirona, www.sironausa.com) was chosen as the design technique.3,4 This technique analyzes neighboring and adjacent teeth, then calculates and proposes a restoration design that has the form and shape of the other teeth in the arch. More information yields a more successful calculation.
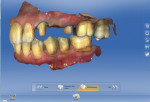
The prepped teeth, along with the adjacent teeth, were scanned into the upper arch folder while the opposing teeth were scanned into the lower arch folder. The patient was instructed to bite into maximum intercuspation, and the bite relation was captured in the buccal bite folder. The software then compiled the three scans to mimic the patient’s bite in maximum intercuspation (Figure 3).
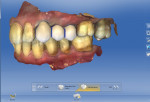
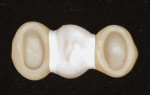
In the model phase, teeth Nos. 11 and 13 were marginated and the correct insertion axis selected. The software then proposed a bridge from Nos. 11 through 13. Software tools were used to make adjustments to the design, make sure that the shape and form of the bridge fit within the arch, and ensure harmonious occlusion (Figure 4). To maintain the strength of the bridge, it is advised that the connector size between the teeth be at least 16 mm2.
Material Selection
IPS e.max LT shade A2 was chosen to mill the bridge. IPS e.max lithium-disilicate restorations offer excellent durability, featuring 360 MPa to 400 MPa of flexural strength.5 According to the manufacturer, the opalescence, translucency, and light diffusion properties of IPS e.max lithium disilicate were all designed to replicate natural tooth structure for beauty and undetectable restorations. Using the CEREC inLab MC XL CAD/CAM milling machine (Dentsply Sirona Dental, www.dentsplysirona.com), it took approximately 18 minutes for the restoration to be milled. The sprue was removed and the restoration was tried in. Once the fit and occlusion are verified in the blue stage, e.max requires a crystallization process to stain and glaze.
Staining, Glazing, and Cementation
In this case, it was noted during the planning stage that there was a definite change in chroma from the gingival to the incisal edge. The value shade was A2 so this shade was selected. However, the gingival third was closer to A3; therefore, this third was stained with a darker A3 to achieve the gradation in color from the gingival third to the cuspal third.
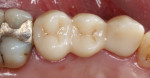
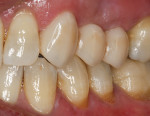
Before bonding, the intaglio of the bridge was etched with 4.5% hydrofluoric acid-etch for 20 seconds. The enamel at the margin was selectively etched for 15 seconds, washed, and dried. The adjacent teeth and the pontic of the bridge were wrapped in teflon tape to avoid any cement getting stuck in the embrasures or the contact area (Figure 5 and Figure 6). An adhesive resin dental cement (NX3 Nexus™, Kerr Dental, www.kerrdental.com) and a self-etch, light-cure adhesive bonding system (OptiBond™ XTR, Kerr Dental) were used to cement the restoration. When the cement reached gel stage, the restoration was tack-cured for 2 seconds and excess cement was removed with an explorer. All surfaces were then light-cured for 20 seconds each. The proximal surfaces were flossed and any remaining cement was removed. Occlusion was checked, the margins were polished, and the final restoration was evaluated from the occlusal (Figure 7) and the buccal (Figure 8).
Final Thoughts
The CEREC Omnicam system and the e.max bridge block allow the clinician to deliver same-day bridges. In the author’s experience, patients have always been pleased to receive this kind of same-day service, as it eliminates the need for the patient to wear a temporary and return for a second visit. As a result, these patients have often become a good source of referrals for the practice.
Fabricating a fixed prosthesis using chairside CEREC CAD/CAM technology has been shown to be predictable, accurate, durable, and esthetic. Being able to achieve this in the same day with the CEREC Omnicam scanning process can be a pleasurable experience for the practitioner while, more importantly, serving the needs and wants of patients.
References
1. Skramstad M, Fasbinder DJ. Full-contour zirconia fixed partial dentures as chairside applications: a case report. Compend Contin Educ Dent. 2016;37(9):648-654.
2. Miyazaki T, Hotta Y. CAD/CAM systems available for the fabrication of crown and bridge restorations. Aust Dent J. 2011;56 Suppl 1:97-106.
3.Kuhr F, Schmidt A, Rehmann P, Wöstmann B. A new method for assessing the accuracy of full arch impressions in patients. J Dent. 2016;55:68-74. Epub 2016 Oct 4.
4.Arslan Y, Karakoca Nemli S, Bankoğlu Güngör M, et al. Evaluation of biogeneric design techniques with CEREC CAD/CAM system J Adv Prosthodont. 2015;7(6):431-436.
5. Albero A, Pascual A, Camps I, Grau-Benitez M. Comparative characterization of a novel cad-cam polymer-infiltrated-ceramic-network. J Clin Exp Dent. 2015;7(4):e495-500.