Management of Advanced Caries
Control anxiety, conserve resources, repair and preserve teeth esthetically
Atraumatic restorative treatment (ART) relies on manual, non-rotary excavation of caries, reducing—if not eliminating—the need for anesthesia and rotary or other expensive equipment for cavity preparation. The conservatively prepared ART cavity is then restored with glass ionomer cement (GIC),1,2 which chemically bonds to tooth structure, exchanging ions shown to remineralize caries-affected dentin.3,4
ART is a minimally invasive, patient-friendly protocol for expeditiously restoring caries lesions.1,4 Mean survival for single-surface ART restorations in permanent teeth at the 5-year mark is 80%, with 60% survival of multiple-surface deciduous restorations at 2 years.5 It is understandable that the American Academy of Pediatric Dentistry has endorsed ART for interim therapeutic restorations (ITRs). ITRs are placed when definitive restorative care cannot be completed due to a lack of resources and/or patient cooperation. The effective management of early childhood caries through the placement of ITRs has become common practice in modern dental settings (deciduous teeth code CDT 2941). The use of ITRs to manage caries in permanent teeth (sedative filling code CDT 2940) is less common, perhaps because of the limited durability and esthetic shortcomings of GICs.
The negative impact of early childhood caries and the psychological and social advantages of ITR management of severe early childhood caries have been assessed and reported.6-8 No reports of caries management using ITRs in adolescent or adult mouths were found, although psychological impact and social judgments associated with visible caries have been published.8 GICs used for ART lack the esthetic characteristics and physical properties needed for large restorations in permanent teeth. The case report presented here highlights ITR caries management through a modified ART technique using a novel, bioactive, dual-cure, resin-modified glass ionomer with the esthetic characteristics and physical properties of today’s most advanced composite resin formulations.9
A Modified Technique
Whenever resin-modified glass ionomers (RMGIs) are used in place of traditional auto-setting GICs, changes to the traditional ART technique are required. A curing light is needed and rotary instrumentation is required for occlusion and contour adjustment, finishing, and polishing; neither of these is needed in the traditional ART protocol. RMGIs offer improved esthetics and physical properties compared to conventional GICs, but they are impractical in underdeveloped regions without access to curing lights and rotary instrumentation.
In modern dental settings, however, the benefits of RMGIs justify a modified ART technique. These benefits include halting the caries process and preserving pulp health while improving the patient’s self-esteem and social interactivity. Expeditiously placed ITRs halt the destruction of healthy enamel and dentin, protecting the pulp and improving the patient’s ability to practice effective oral hygiene while remineralization ensues.
Case Presentation
A healthy but anxious 28-year-old single mother of four presented to the author’s office. Her teeth had recently become so “sensitive” and “ugly” that she contacted the author seeking a denture. “I hate my teeth,” she said. “I’m wasting money trying to fix them.”
Review of the patient’s medical history and lifestyle revealed no systemic or behavioral causes for her advanced cervical caries other than consumption of sweetened ice tea and infrequent professional care. Her plaque control was acceptable, except in the areas around the demineralized and cavitated lesions that were “too sensitive to brush.” The patient had followed the recommendation of a friend who suggested she substitute xylitol for granulated sugar in her sweetened tea. Thermal sensitivity and discomfort during brushing and eating as well as the compromised esthetics prompted the patient to seek professional help.
Treatment Protocol
Patient-centered dentistry must take into account the effects of skepticism and anxiety on treatment decisions. Patients with limited resources can be tempted by quick-fix options without fully considering long-term consequences. Tooth extraction followed by complete denture therapy is one such example. Following a brief discussion of the treatment time and cost for placing ITRs, the patient consented to treatment of maxillary anterior lesions as part of her consultation visit.
The patient consented to 20% benzocaine topical anesthetic followed by approximately 1 mL articaine 4% 1:100k epinephrine infiltrated sparingly over the roots of teeth Nos. 6 through 11. ACTIVA® BioActive-Base/Liner and ACTIVA® BioActive-Restorative materials (Pulpdent, www.pulpdent.com) were selected to provide an expeditious, inexpensive option addressing the sensitivity and esthetic concerns. The effect this simple approach had on the patient’s feelings toward her dental health, self-confidence, and social interactions will be discussed following the treatment steps.
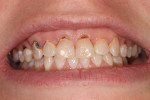
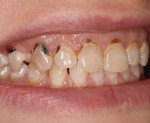
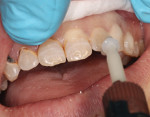
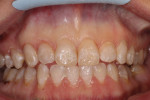
The preoperative photographs illustrate the advancing caries lesions (Figure 1 and Figure 2). Manual caries excavation using a spoon excavator rapidly debrided each lesion prior to high-speed rotary finishing of the cavo-surface margin (Figure 3). Treating a few teeth at a time, beginning with hand excavation, gradually introduced the patient to tooth instrumentation. Caries excavation and cavity preparation were tolerated well by the patient despite the fact this was her first restorative visit to a dentist.
A clean, caries-free, cavo-surface margin is essential for long-term ITRs. Complete removal of caries-affected dentin against the pulpal wall is not necessary, however. Mineral exchange between the tooth and glass ionomer formulations can restore caries-affected dentin to hardness levels surpassing healthy dentin. Preservation of pulp vitality has been touted as a benefit of ITRs. This author’s experience suggests pulpitis and necrosis are rare after placement of GICs, but should be presented as known risks when remaining dentin thickness is less than 0.5 mm.
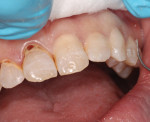
ACTIVA Base/Liner has a lower pH than ACTIVA Restorative. It is also less filled and therefore has more free monomer on the surface. As a result, the Base/Liner is slightly more active than the Restorative and bonds to dentin without etching or bonding agents. When dentin thickness was suspected to be less than 0.5 mm, a thin insulating liner of ACTIVA Base/Liner was placed using the static mixer tip and light cured for 20 seconds with FLASHlite Magna® 4.0 (DenMat, www.denmat.com) (Figure 4).
Next, the enamel margins were etched with 38% phosphoric acid for 15 seconds before rinsing and lightly air-drying without desiccating the tooth surfaces. Using a mylar matrix when necessary to contour approximal surfaces, ACTIVA BioActive-Restorative was placed bulk fill, contoured, and cured (Figure 5). Each restoration was light cured for 20 seconds and allowed to continue polymerization in dual-cure mode for 3 minutes before finishing. Both the ACTIVA Base/Liner and Restorative formulations adapt well to tooth surfaces without trapping air. Finishing was done with rotary instrumentation using six-fluted finishing burs followed by Enhance® Polishing Cups (DENTSPLY Caulk, www.caulk.com). The ITRs placed at the patient’s initial visit are shown in Figure 6.
A 24-hour follow-up call confirmed no sensitivity, and the patient expressed thanks for encouraging her to keep her teeth. Three days later, the patient called requesting permission to use at-home whitening, confirming absolutely no sensitivity to chemical, thermal change, or brushing, and said she was looking forward to her next appointment.
Discussion
Each new restorative challenge opens the door to new possibilities, sometimes with pleasant surprises. Control of advanced caries requires expeditious restorative intervention as well as discussion of diet, lifestyle, and homecare practices. Preservation of pulpal health should be the highest priority, and remineralization of caries-affected enamel and dentin is essential for tooth preservation. Historically, the best tooth preservation approach to managing advanced caries has been ART, using either conventional or resin-modified GICs. While survival of ART restorations can rival that of traditional materials requiring more invasive techniques, unfavorable esthetics, poor physical properties, and wear and tear on restored surfaces have limited the acceptance of GIC ART restorations in modern dental settings.
ACTIVA BioActive Base/Liner and Restorative materials are formulated using a proprietary rubber-toughened, biocompatible, urethane derivative with GIC ion exchange properties shown to remineralize enamel and dentin. These are the first super tough, base/liner and restorative materials for restoring all tooth surfaces in all cavity classifications. The remarkable esthetics, durability, high surface luster, and simplified handling and placement of ACTIVA materials make them ideally suited for minimally invasive as well as traditional restorative approaches.
For caries control, the ionic exchange and remineralization potential surpass that of traditional materials. From a clinical perspective, excellent functional and esthetic results have been achieved using ACTIVA, and the remarkable infrequency of pulpitis and pulpal necrosis is most surprising. Another surprise is the change in the patient’s attitude regarding her natural teeth. Although the restorative technique used went beyond conventional ART, the minor cost difference between ACTIVA and GIC or RMGI restorations was more than offset by timesavings and patient satisfaction with the results.
Conclusion
Traditional glass ionomers and RMGIs have been important materials for caries management, atraumatic restorative treatments, and interim therapeutic restorations. As the author continues to observe these bioactive ACTIVA restorations, he is intrigued by the possibility of extending the service of what was previously classified as interim or temporary restorations to possibly provide long-term therapeutic restorations with esthetics and durability comparable to today’s complex composite restorative systems. Tough, durable, esthetic, bioactive composites offer an exciting new approach for tooth preservation and management of advanced caries in the adult dentition.
Disclosure
Nels Ewoldsen, DDS, MSD, received an honorarium from Pulpdent as well as material support in the form of samples of ACTIVA product
For more information, contact:
Pulpdent
800-343-4342
activabioactive.com
About the author
Nels Ewoldsen, DDS, MSD
Owner, Conservative Dental Solutions
Private Practice
Waveland, Indiana
References
1. Lopez N, Simpser-Rafalin S, Berthold P. Atraumatic Restorative Treatment for Prevention and Treatment of Caries in an Underserved Community. Am J Public Health. 2005;95(8):1338-1339.
2. Mount GJ. A new paradigm for operative dentistry. J Conserv Dent. 2008;11(1):3-10.
3. Ngo HC, Mount G, McIntyre J, Do L. An in vitro model for the study of chemical exchange between glass ionomer restorations and partially demineralized dentin using a minimally invasive restorative technique. J Dent. 2011;39(suppl 2):S20-S26.
4. Schriks MC, van Amerongen WE. Atraumatic perspectives of ART: psychological and physiological aspects of treatment with and without rotary instruments. J Community Dent Oral Epidemiol. 2003;31(1):15-20.
5. de Amorim RG, Leal SC, Frencken JE. Survival of atraumatic restorative treatment (ART) sealants and restorations: a meta-analysis. Clin Oral Investig. 2012;16(2):429-441.
6. Martinis-Júnior PA, Vieira-Andrade RG, Corrêa-Faria P, et al. Impact of early childhood caries on the oral health-related quality of life of preschool children and their parents. Caries Res. 2013;47(3):211-218.
7. Somani A, Newton JT, Dunne S, Gilbert DB. The impact of visible decay on social judgements: comparison of the effects of location and extent of lesion. Int Dent J. 2010;60(3):169-174.
8. Scarpelli AC, Oliveira BH, Tesch FC, et al. Psychometric properties of the Brazilian version of the Early Childhood Oral Health Impact Scale (B-ECOHIS). BMC Oral Health. 2011;11:19.
9. Jefferies S, Lööf J, Pameijer CH, et al. Physical properties and comparative strength of a bioactive luting cement. Compend Contin Educ Dent. 2013;34(spec no 8):8-14.