Prosthetically-Based Implant Planning
Advances in digital imaging and bone augmentation allow implant position to be dictated by the final prosthesis
Jay B. Reznick, DMD, MD, Diplomate ABOMS
One of the most important criteria for the success of a dental implant is its initial primary stability at the time of placement. After tooth extraction, there must be an adequate volume and density of healthy bone remaining in the alveolus in order to support an immediately-placed implant.1,2 This required volume and location of bone may be difficult to assess preoperatively using 2-dimensional imaging. Oftentimes, the challenge in these cases is that the extraction site becomes compromised by bone loss due to chronic infection or inflammatory processes. This may cause loss of the facial plate of alveolar bone over the area where an implant fixture would be placed. Using traditional methods, after the tooth was extracted and the socket debrided, an initial osteotomy was created using direct visualization and freehand drilling. Because of the slope of the palatal wall of the extraction socket, the osteotomy drill has a tendency to drift facially, so the potential exists for the final osteotomy and subsequent fixture placement to deviate from the planned position. More often than many practitioners might like to acknowledge, implant placement and initial stability were less than ideal in an area where they are most critical.
Fortunately, technology has evolved to utilize 3-dimensional imaging to more accurately assess the pre-existing pathology, volume, and location of alveolar bone remaining after extraction and the likelihood of achieving initial primary implant stability. The development of software for implant planning combined with stereolithographic 3D printing and milling has resulted in the growth of fully-guided implant surgery, in which the position, angulation, and depth of each osteotomy and implant placement is precisely controlled to minimize deviation between the planned and actual location.3 Studies have shown that fully-guided surgery is significantly more accurate and efficient than freehand implant placement, even when performed by experienced implant surgeons.4,5 These advances have led to prosthetically-based implant planning, in which the implant position is dictated by the final prosthesis, not just by the available bone. If the bone volume is not sufficient at the desired site, it can be augmented prior to or at the time of implant placement. It can also be determined, in advance, whether it is feasible to perform immediate implant placement and provisionalization at the time of extraction or if the specific case warrants a delayed technique.
Case Report
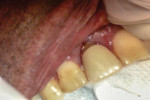
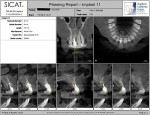
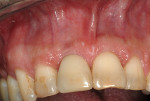
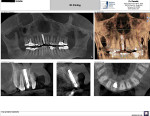
A healthy, 50-year-old male presented to the office with a tender, slightly mobile maxillary right central incisor. The tooth had been traumatized when he was a teenager, and over the years, it underwent endodontic treatment, a PFM crown, and apical surgery. In recent months, the tooth had become symptomatic and developed gingival recession and a small fistula at the facial attached gingiva (Figure 1). The tooth was diagnosed as fractured, and the patient was referred for removal and implant placement. The radiographic and clinical exams were found to be consistent with the clinical impression, and the option of an immediate implant and provisional restoration was discussed with the patient. His restorative dentist wished to use a cement-retained final prosthesis, so an Astra Tech OsseoSpeed™ TX S implant was planned with the appropriate position and emergence profile. A cone-beam computed tomography (CBCT) evaluation demonstrated that the apical half of the implant would be located in stable alveolar bone to allow for primary mechanical stabilization and that a facial bony defect would exist over the occlusal one-fourth of the implant fixture (Figure 2).
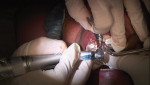
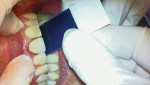
Tooth No. 8 was removed using an atraumatic technique. The socket was thoroughly debrided and irrigated, and then, utilizing the Astra Tech Facilitate™ computer guided surgery kit, osteotomies were performed, and a TX S implant was placed into the preplanned site (Figure 3). After placing a resorbable barrier membrane between the facial alveolar wall and the soft tissue, a particulate calcified corticocancellous allograft was packed between the implant and the alveolar walls as well as into the facial defect. Next, an immediate screw-retained polymethylmethacrylate provisional restoration was placed, and the abutment screw was tightened to 20 Ncm with a torque wrench. The provisional crown was then adjusted to be completely out of occlusion and functional contact (Figure 4). Postoperatively, a CBCT image was obtained, which showed perfect implant placement—parallel to the adjacent teeth, evenly spaced, and well-aligned for the provisional and final prostheses (Figure 5).
At the 1-year follow-up appointment, the implant was stable and non-tender. The facial fistula had completely healed, and there was no evidence of infection. In addition, there was adequate keratinized mucosa around the implant crown, and the interdental papillae were of sufficient contour (Figure 6). The final crown had been placed 6 months prior, and the patient was extremely happy with both the esthetic result and the overall experience.
References
1. Javed F, Romanos GE. The role of primary stability for successful immediate loading of dental implants. A literature review. J Dent. 2010;38(8):612-620.
2. Becker W, Sennerby L, Bedrossian E, Becker BE, Lucchini JP. Implant stability measurements for implants placed at the time of extraction: A cohort, prospective clinical trial. J Periodontol. 2005;76(3):391-397.
3. Dreiseidler T, Neugebauer J, Ritter L, et al. Accuracy of a newly developed integrated system for dental implant planning. Clin Oral Implants Res. 2009;20(11):1191-1199.
4. Vercruyssen M, Cox C, Coucke W, Naert I, Jacobs R, Quirynen M. A randomized clinical trial comparing guided implant surgery (bone- or mucosa-supported) with mental navigation or the use of a pilot-drill template. J Clin Periodontol. 2014;41(7):717-723.
5. Vermeulen J. The accuracy of implant placement by experienced surgeons: guided vs freehand approach in a simulated plastic model. Int J Oral Maxillofac Implants. 2016;32(3):617-624.
About the Author
Jay B. Reznick, DMD, MD, Diplomate ABOMS
Private Practice
Tarzana, California
For more information, contact:
Dentsply Sirona
800-659-5977
sirona3d.com