Maximizing Laser Use
Get on the same wavelength as successful laser practitioners
Robert A. Convissar, DDS, FAGD
How does one maximize laser use in their practice? The answer is quite simple: education. The only way to maximize the use of any high-tech device is through education and training. A practitioner must learn the ins and outs of the equipment and exactly how the equipment works—knowing how to adjust the settings, when to adjust the settings, and why to adjust the settings. Looking around the typical dental operatory, one will find a wide range of technology and devices, most of which require training. That digital radiography system came with a few good, solid hours of in-office training, as did that CAD/CAM optical impression device. What about those syringes of Botox and fillers? Dentists learn how to properly inject through plenty of hands-on training before injecting their first patient. So why does that laser sitting in the corner, which is used a few times a week, only come with a webinar, a CD, and a workbook?
Too many dentists are under the impression that a laser is a plug-and-play device. They believe that you can just take it out of the box, plug it in, and go to work; however, nothing could be further from the truth. A laser is a high-tech device that demands training.1 Unfortunately, many laser companies do not bother to provide any training beyond that webinar, CD, and workbook. This is precisely the reason that many laser users barely recoup their investment on this remarkable technology. There are thousands of dentists who purchase inexpensive lasers, use them a few times, then put them back in the box, never again to see the light of day. This is why so many lasers are for sale in the classified sections of dental journals and on eBay and other online retailers.
In a questionnaire given to attendees of 2-day Academy of Laser Dentistry Standard Proficiency Certification training programs, an astounding 95% of the dentists who own diode lasers could not correctly answer the question of why the tip must be initiated—the most important procedure in preparing the laser immediately prior to placing it in the patient’s mouth.
Virtually 100% of laser owners also responded to the question, "how do you initiate the tip," by stating that they use either articulating paper or cork, neither of which provides ideal initiation. Less than ideal initiation leads to less than ideal heat distribution on the laser tip, which leads to far less than ideal clinical results. So why does a diode laser need to be initiated?
Lasers are optical devices. The dentist steps on the foot pedal and a stream of light energy is emitted. This beam of light energy does the work, including ablation, vaporization, or coagulation of the target tissue. Many lasers are used "out of contact" with the tissue so that the beam of amplified light energy can exit the handpiece and interact with the target tissue.The key to the laser’s interaction with the target is that the target tissue must be able to absorb the specific wavelength of the laser being used. If the target tissue can absorb the laser energy, the desired therapeutic effect will be achieved. CO2 (carbon dioxide) and erbium lasers are examples that utilize this type of laser-tissue interaction.
Unfortunately, not all dental lasers work this way. Diode laser wavelengths are not absorbed by the oral mucosa. Although it sounds counterintuitive, a practitioner makes a diode laser work by NOT using it as a laser. Yes, diode lasers are classified as lasers because they emit beams of collimated, monochromatic, coherent energy; however, the beam is not permitted to interact with the tissue. In a process called initiation, a material such as ink, articulating paper, or cork is placed on the tip of the laser fiber to prevent the laser energy from exiting the handpiece. This material causes the laser tip to heat up. In this manner, the diode laser is no longer acting like a laser. Because the laser energy is converted to pure thermal energy, the practitioner isn’t using the light to do the work, he or she is using the handpiece as a "hot tip."
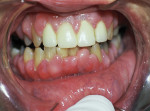
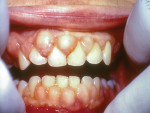
A few states mandate training for dentists and hygienists before they are permitted to use lasers on patients, but most states have no such regulations. As a result, too many dentists purchase lasers, receive insufficient training, and never maximize their use of the device. Figure 1 and Figure 2 illustrate the importance of laser training. Both figures feature kidney transplant patients who take cyclosporine to prevent rejection of the transplanted organ and calcium channel blockers to help maintain a healthy blood pressure. Each of these drugs can cause gingival hyperplasia as a side effect, and the treatment plan for both patients is simple enough: a gingivectomy. For the untrained dentist, the thought process involved in setting the parameters for both cases is also simple: (1) click on the list of preset parameters programmed into the laser; (2) click on "gingivectomy"; and (3) perform the procedure. After all, a gingivectomy is a gingivectomy, right? Unfortunately, if these two kidney transplant patients are treated with the same exact laser parameters, one of the cases will turn out well and the other will turn out horribly wrong. Why? Because every laser procedure is based on two criteria: the wavelength emitted from the laser device and the chromophore content of the target tissue.
What’s a chromophore? Understanding chromophores and their significance in laser dentistry is one of the most fundamental lessons learned in laser dentistry training. Why do people wear light colors in the summer and dark colors in the winter? Light colors reflect sunlight and help keep people cool, whereas dark colors absorb sunlight and help keep people warm. Light energy is either absorbed or reflected by surfaces. This is similar to how chromophores work. The textbook definition of chromophore is "a light absorbing compound or molecule normally occurring in tissues that absorbs specific wavelengths of laser energy." 2
So what does this have to do with dental laser treatment? Each and every laser wavelength used in dentistry is unique and absorbed to different extents by the target tissue due to the type and amount of chromophores in the tissue. Two of the main chromophores (ie, light absorbing molecules/compounds) in the oral cavity are Hemoglobin/Oxyhemoglobin and water. The chromophore for erbium and CO2 lasers is water; therefore, tissue with a high water content (the oral mucosa is 75% to 90% water) will absorb these two wavelengths quite efficiently. 3,4 Alternatively, the chromophore for diode and Nd:YAG (neodymium-doped yttrium aluminium garnet) lasers is hemoglobin/oxyhemoglobin; therefore, deeply pigmented or highly vascular tissues will absorb all of these wavelengths efficiently.3
Well-trained laser dentists who understand how to use their devices will have very different thought processes of how to set the ideal parameters for the cases presented in the figures. The steps for the trained dentist would begin with an evaluation of the tissue. Is the tissue pink or red? Is it edematous or fibrotic? Red, edematous tissue has a higher water content than pink, fibrotic tissue. The conduction of heat energy also proceeds more quickly in watery tissue than in fibrotic tissue. Red, inflamed tissue also has higher hemoglobin content when compared to pink, fibrotic tissue. Depending on the laser used, hemoglobin content will also affect the absorption of laser energy.
After evaluating the tissue, the thought process of the trained laser user is to: (1) click on the list of preset parameters; (2) click on "gingivectomy"; (3) modify the parameters based on the amount/type of chromophore present in the tissue; and (4) perform the procedure.
So, how would a well-trained laser dentist evaluate the patients in Figure 1 and Figure 2? The patient presented in Figure 1 has less vascularity (more pink, fibrotic tissue) and less water content (non-edematous) in her gingiva, whereas the patient illustrated in Figure 2 has more vascularity (much more red tissue) and more water content (more edematous) in her tissue. If the dentist is using a diode or Nd:YAG laser, how should the parameters be modified for each of these patients? The greater the amount of chromophore present, the more the wavelength will be absorbed and the faster the tissue will be removed; hence, the lower the strength needed. Therefore, the patient in Figure 1 would require higher settings with a diode or Nd:YAG laser because there is less chromophore in the tissue, and this tissue is more fibrotic, thus it will take more energy to heat up and remove than the watery tissue depicted in Figure 2. Conversely, The patient in Figure 2 would require lower settings because there is more chromophore in the tissue, and the tissue is much more watery, thus it will take less energy to heat up and remove than the fibrotic tissue depicted in Figure 1. If the settings successfully used for the patient in Figure 1 were also used on the patient in Figure 2, the tissue would cut much more rapidly—probably too rapidly—resulting in thermal damage to the tissue and all of its accompanying problems (eg, delayed wound healing, postoperative discomfort, tissue recession, etc.). Conversely, if the settings successfully used on the patient in Figure 2 were also used on the patient in Figure 1, the laser would lack the power needed to deliver effective treatment.
This same thought process would occur if the dentist were using a CO2 or an erbium laser. The patient in Figure 1 has very little water content in her gingiva when compared with the patient in Figure 2 who has far more water due to the edema in her tissue. If the settings with a CO2 or an erbium laser successfully used in Figure 1 were used in Figure 2, the tissue would cut much more rapidly, possibly resulting in the same thermal damage and accompanying problems that could occur with the diode or Nd:YAG laser.
Selection of ideal laser settings based on chromophore content is only one of many lessons that the untrained laser dentist needs to understand before being ready to successfully use a laser and maximize its potential. In addition, critical factors such as correct spot size selection, proper initiation technique, appropriate hand speed, and other issues need to be discussed in detail as part of laser training.
References
1. Weiner G. Laser Dentistry Practice Management. Dent Clin North Am. 2004;48(4):1105-1126.
2. Catone G, Alling C. Laser Applications in Oral and Maxillofacial Surgery. Philadelphia, PA: WB Saunders Company; 1997.
3. Coluzzi D, Convissar R, Roshkind D. Laser Fundamentals. In: Principles and Practice of Laser Dentistry 2nd edition. St. Louis, MO: Elsevier; 2016:12-26. .
4. Rossmann, J (ed). Lasers in Periodontics. J Periodontal. 2002;73(10):1231-1239.