Treatment Solutions for a Complex High-Risk Caries Patient
Planning for long-term success in a case of poor compliance
Joyce Bassett, DDS, FAACD, FAGD
Offering high quality dentistry is the goal of every dentist. Our responsibility is to evaluate the condition and gain a thorough understanding of the patient’s history, circumstances, and expectations, while assessing the risk, longevity, and liability of the proposed treatment modality. It may be difficult for the dentist to determine if an identified condition is progressing, regressing, or stable. Uncertainty is problematic because appropriate treatment often depends on an accurate understanding of oral conditions.
Case Presentation
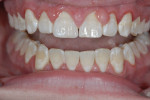
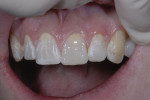
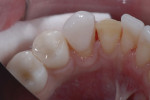
A 14-year-old male patient presented for a structural and esthetic assessment of his dental condition (Figure 1). He reported that his orthodontist decided that early debanding was required, leaving the buccal corridor undeveloped. He had been noncompliant with wearing elastics and had missed many appointments. The enamel exhibited many decalcified areas and plaque control was poor. The patient’s mother sought a conservative approach to his current situation. He was displeased with his appearance and stated that he detested all visits to the dentist.
The patient received a comprehensive exam, full-mouth series of radiographs, a panoramic x-ray, diagnostic photos, records, and a periodontal evaluation. Periodontal sulcus depths of 2 to 3 mm were noted. Plaque was rampant and his hypertrophied gingiva exhibited bleeding on probing. The panoramic x-ray revealed bone support within 2 mm of the cementoenamel junction. A clinical evaluation revealed white spot lesions and carious lesions on multiple surfaces of his dentition.
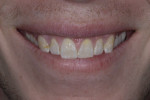
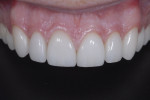
The patient exhibited a dental Class I malocclusion. The musculature and joints were not painful to loading or palpation. On a full smile, he demonstrated high lip dynamics on the maxillary arch and low lip dynamics on the mandibular arch (Figure 2).
The patient’s esthetic vision could not be addressed until caries control, caries removal, and hygiene compliance was attained.
Periodontal Re-Evaluation
Topical anesthetic was placed, and scaling and curettage was performed. The patient was given plaque management and oral hygiene instructions, along with reinforcing future monitoring of home care. The re-evaluation of the hyperplastic tissue 60 days after the initial periodontal therapy revealed the necessity to perform a gingivectomy and gingivoplasty on the maxillary incisors.
To ensure that the biologic width was respected, sounding to bone was performed after anesthetizing1 and before any tissue was removed to safeguard the health of the dentogingival complex. The NV® microlaser 810 Nm diode (DenMat, www.denmat.com) was used because the zone of necrosis is 3 to 5 cells thick and the healing was quick and painless.2
Caries Assessment
Caries is a disease of susceptibility. Bacterial plaque accumulation called biofilm creates an acid environment that allows caries disease to spread. Risk factors for developing caries include active orthodontics, a cariogenic diet, presence of biofilm, poor oral hygiene, and acquired enamel defects.
White spot lesions are caused by the demineralization of the subsurface enamel, either by the malformation of the enamel during tooth development or breakdown of the enamel due to acids and poor oral hygiene. Since the surface of the enamel is porous, phosphates can move out of the tooth.3
To offer the most conservative treatment, the Icon system was considered (DMG America, www.dmg-america.com), as MI Paste™ (GC America, www.gcamerica.com) and Icon have been successfully used in the early stages of white spot lesions. The Icon system involves microabrasion with hydrochloric acid, simultaneously eroding and abrading the enamel while saturating the enamel with hydrochloric acid and infusing it with liquid resin. The challenge for the dentist is diagnosing the lesion stage and its degree of activity. Visual assessment cannot determine the depth or activity of the lesion. It must be determined if anterior lesions are progressing, regressing, or remaining the same. After this HCl-infused microabrasion, the remaining enamel is dense and aprismatic and more resistant to acid challenges and plaque retention.4
A multifaceted intervention approach combining fluoride, xylitol, remineralization, resin infiltration, MI Paste, and antimicrobials was investigated.
A pediatric dental specialist expert and an initial tester for the Icon resin infusion system was employed to perform a diagnostic evaluation to see if the Icon product would repair this situation in a conservative manner. He reported that the penetration and destruction was so advanced, the minimally invasive resin infiltration was not a possible solution. Therefore, the treatment with the best long-term predictable outcome was removal of the damaged enamel and affected dentin. The carious lesions were so widely distributed that full-mouth reconstruction was necessary.
A 5000-ppm toothpaste, a fluoride rinse, and MI Paste were prescribed in the interim.
Bleaching and Caries Removal
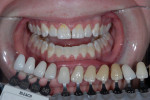
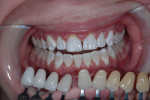
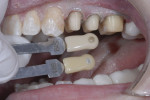
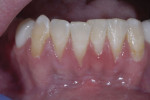
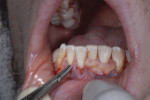
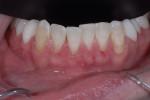
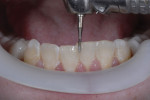
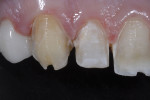
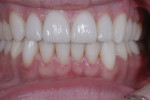
Since this patient was only 14 years old at the initial visit and nervous about dental treatment, it was important to arrest the disease while gaining his confidence and keeping appointments as short and pain free as possible. At-home bleaching trays had been fabricated during initial periodontal therapy, but he was not satisfied with the home tray protocol and admitted he was noncompliant. He desired the quickest solution to attain the whitest smile, so in-office power bleaching (Philips Zoom WhiteSpeed, Philips Oral Healthcare, www.philipsoralhealtcare.com) was chosen (Figure 3 and Figure 4).
During bleaching, the teeth desiccate, and the white spots appear more prominent. It is important to inform the patient that as the tooth rehydrates, the white spot color may blend in with the new whiter surrounding enamel or the white spot color may become visually intensified, requiring an additional procedure of either composite resin or microabrasive techniques.5 In this case, the body color of the tooth became whiter and blended in more harmoniously with the bleached tooth.
For the restorative portion of the treatment, nitrous oxide in concert with local anesthetic was used. Quadrant posterior dentistry was accomplished. Caries removal and glass ionomer placement (Vitrebond™ Plus, 3M ESPE, www.3mespe.com) were followed by composite build-up foundational restorations in preparation for future definitive full coverage.
A recare interval of 3 months was set, to which the patient complied. Consistent reinforcement of his at-home hygiene regimen and usage of adjunct fluoride products occurred along with monitoring of the white spot lesion. Cavitation was noted on the enamel surrounding the foundational composite restorations. Subsequent posterior full-coverage restorations (Lava™ Zirconia, 3M ESPE) were fabricated in quadrants (Figure 5). Due to his high caries index, all preparation margins were placed subgingivally, respecting biologic width principles. The zirconia restorations were cohesively cemented with a glass ionomer cement (RelyX™, 3M ESPE) because of its fluoride release and retrievability. Degradation of the dentogingival complex in the anterior segment was occurring and a periodontal referral and treatment was deemed necessary (Figure 6).
Periodontal Surgery
The surgeon believed this was an anatomic problem created by crowding that altered where the teeth erupted into the arch. The Miller classification of the soft tissue defect was Class I, so 100% root coverage was expected.
A subepithelial connective tissue graft was performed to attain root coverage and thicken the facial tissue. A tunnel technique was employed.
A sulcular incision was made from No. 22 to No. 27 and a partial thickness dissection was performed to create a deep pouch beyond the mucogingival junction. The interproximal papilla was kept intact just below the proximal contact point of the teeth. The connective tissue was harvested using a single incision technique with a partial thickness dissection and sutured closed with 4-0 chronic gut. The roots were flattened and planed slightly at the recipient site before placement of the graft. The graft was then inserted into the pouch with 6-0 chromic gut sutures (Figure 7). A combination of 6-0 chromic gut and 6-0 Vicryl® sutures (Ethicon, www.ethicon.com) were used to stabilize the flap. Healing progressed uneventfully and the gingival recession was covered (Figure 8).
Fabrication and Delivery
At this point in treatment, the patient spontaneously decided that during his college winter break he would like his anterior teeth esthetically enhanced with veneers. His home care was still not optimal and the gingival complex was inflamed upon examination. More important than the lack of plaque control was the noncompliance in wearing any retentive devices. Rotations and facial shifting were advancing. The anterior enamel cavitation with decay was progressing and was paramount in the decision to proceed in a less than optimal unhealthy gingival environment.
Time constraint did not allow for a laboratory diagnostic wax-up; consequently, an intraoral direct composite mock-up was performed. The goal was to keep the original shape and form of his anterior teeth, remove the affected enamel and decay, and brighten up the color. On evaluation of facial volume and fullness, it was noted that all maxillary teeth were in proper alignment except for the left maxillary incisor.
To obtain desired facial volume, flowable composite (Herculite™ Ultra Flow,, Kerr Dental, www.kerrdental.com), was placed on the facial surface of the left central incisor No. 9 (Figure 9). The mandibular centrals were rotated and overlapped. Preparation design parameters dictate that the contact must be broken. The width of the two central incisors must be identical to and thinner than the width of the lateral incisors. The mandibular midline was not in the esthetic zone, but the facial and maxillary tooth midline needed to be evaluated to attain proper alignment of the maxillary and mandibular midlines.
Local anesthesia was administered and a slice preparation (Brasseler #169 carbide, http://brasselerusadental.com) was accomplished, with most tooth reduction being performed on tooth No. 25 (Figure 10). Flowable composite was placed on both lower incisors and recontouring occurred until ideal shape and form was obtained. The patient previewed and approved these direct prototypes. Depth-cut diamonds (Brasseler RWMIN.3/.5/.7) were placed across the gingival and middle thirds to establish the amount of facial reduction, followed by depth cuts on the incisal to guide 2 mm removal of enamel from the definitive approved incisal edge.6,7 The facial veneer preparation revealed that the lesions were deep into the dentin (Figure 11). Caries detector was placed and photographs taken to be used for patient education.
Due to the patient’s age, tooth banking was chosen over full-coverage preparation. Since most of the facial enamel was diseased and had been removed, a chamfer design was prepared and carried 2 mm onto the lingual surface. This design provided for availability of more lingual enamel for bonding and enhanced the resistance form of the preparation.8
A face-bow, polyvinyl siloxane impression (Imprint™ 4, 3M ESPE), and provisionals (Luxatemp®, DMG America) were fabricated and documented with photographs. The patient returned 2 days later with the composite prototype of tooth No. 27 broken. The composite was repaired, and all prototypes were evaluated. Because the composite prototypes were not contralaterally identical from a facial perspective, the patient was asked to determine which outline form, length, and incisal embrasure he would like the porcelain to mimic. Symmetry is the mirror image of parts and components around an axis. Harmony is a recurring theme. Some patients want the final contours to be identical contralaterally and symmetrical, whereas others are comfortable with a harmonious theme. A detailed laboratory prescription and an approved provisional model were sent to the ceramist.
The patient fractured the provisional of tooth No. 22 twice more over the next 7 days.
Prototypes are trial runs and breakage or loosening is a gift. Design correction can be accomplished before final fabrication.
Evidence of nocturnal bruxism was verified and the canine guidance was shallowed. Essix retainers (DENTSPLY Raintree Essix, www.essix.com) were fabricated and worn over the prototypes at night. The remaining mandibular composite prototypes remained intact, and a full-coverage restoration was prepared for tooth No. 27 only. Records were taken of this full-coverage preparation with the remaining composite prototypes on the other mandibular dentition kept intact. This would allow the laboratory to accurately fabricate the full-coverage restoration for tooth No. 22 without requiring the re-impressioning of the mandibular anterior veneer preparations.
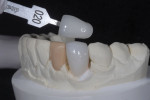
The ceramist had fabricated the mandibular veneers and used the new impression to fabricate the canine crown against the existing veneers. She fabricated the lower units from the first impression and duplicated in wax the adjacent lateral incisor so contacts and form could be created (Figure 12). This contact may need adjusting on final cementation of the definitive restorations. As a strategy to minimize the risk of future fracture or chipping, the restoration (IPS e.max®, Ivoclar Vivadent, www.ivoclarvivadent.com) on the contralateral left lateral canine was feather-edged to the recommended minimum thickness required by the manufacturer 0.3 mm and was carried on to the lingual 3 mm shy of the free gingival margin (Figure 13).9,10
At the delivery appointment, the six maxillary and six mandibular restorations were tried in, the esthetics evaluated and approved, and followed by cementation (RelyX; All-Bond Universal®, BISCO, www.bisco.com).
The occlusion was evaluated by having the patient close into maximum intercuspation to verify that all posterior teeth displayed bilateral, simultaneous forces. Movement in all excursive directions was evaluated and adjustments were made by recontouring the porcelain on the mandibular dentition.
Clearance between the incisors in maximum intercuspation was verified by shim stock and thick articulating paper with the patient sitting up and mimicking the chewing cycle. The lateral streaks on the canines were left, and any lateral streaks on the posterior teeth were removed. Streaks on the lingual of the central incisors in the chewing envelope were adjusted along with the facials of the lower incisors, with special consideration to preserving the length. Siblant sounds were tested followed by finishing and polishing of all surfaces of ceramic (Dialite® points, Brasseler). Postoperative photos (Figure 14 and Figure 15) and records for a maxillary flat plane occlusal splint and Essix retainers were acquired.
An indefinite retention period will be necessary to maintain the results achieved and compliance with the flat plane splint nightly is paramount to the longevity of the reconstruction.
The surface of the nightguard will be assessed at subsequent hygiene recare appointments for the presence of parafunction.
Conclusion
This case shows that even a noncompliant, anxious teenager with a high caries rate and high esthetic demands can receive dental care that will lower his risk of disease and provide excellent long-lasting esthetic result. The cornerstones of this success were the building of trust to change noncompliant habits, continual re-evaluation during procedures and recare appointments, and designing restorations to be as conservative as his disease state allowed.
Disclosure
Joyce Bassett, DDS, FAACD, FAGD, has no relevant financial relationships to disclose.
Acknowledgment
The concepts demonstrated were learned at the Kois Center and through many courses presented by the American Academy of Cosmetic Dentistry (AACD). The author would like to thank Sandra Cook, CDT, AAACD, from CMR Dental Lab in Idaho Falls, Idaho, for the ceramic artistry for the anterior veneers, Rick Durkee, CDT, AAACD, from Lafayette Dental Lab in Phoenix, Arizona, for the posterior zirconia crowns, and Ralph Wilson, DDS, for the periodontal surgery.
About the author
Joyce Bassett, DDS, FAACD, FAGD
Private Practice
Scottsdale, Arizona
References
1. Kois JC. Predictable single tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2001;22(3):199-208.
2. Kalsi HJ, Hussain Z, Darbar U. An update on crown lengthening. Part 1: Gingival tissue excess. Dent Update. 2015;42(2):144-146, 149-150, 153.
3. Croll TP, Segura A, Donly KJ. Enamel microabrasion: new considerations in 1993. Pract Periodontics Aesthet Dent. 1993;5(8):19-28.
4. Croll TP. Enamel microabrasion in conjunction with carbamide peroxide bleaching. Dent Today. 1992;11(3):56-57.
5. Bassett J. Foundation for a successful smile makeover: understanding bleaching choices and techniques. Dent Today. 2015;34(1):120-123.
6. Magne P, Belser UC. Novel porcelain laminate preparation approach driven by a diagnostic mock-up. J Esthet Restor Dent. 2004;16(1):7-18.
7. Gürel G. The Science and Art of Porcelain Laminate Veneers. Hanover Park, IL: Quintessence Publishing; 2003:241-251, 261-276.
8. Chaiyabutr Y, Phillips KM, Ma PS, Chitswe K. Comparison of load-fatigue testing of ceramic veneers with two different preparation designs. Int J Prosthodont. 2009;22(6):573-575.
9. Anusavice KJ. Standardizing failure, success, and survival decisions in clinical studies of ceramic and metal-ceramic fixed dental prostheses. Dent Mater. 2012;28(1):102-111.
10. Bühler-Zemp P, Völkel T, Fischer K. Scientific documentation IPS e.max® Press. Schaan Liechtenstein: Ivoclar Vivadent; 2011:1-40.