Preserving Natural Dentition in Endodontically Treated Teeth
In some cases, an implant isn’t the go-to solution
Today dentists are placing more implants than ever before. Implant advertisements seem to be everywhere—dental magazines, conventions, and meetings—with companies showcasing the ease of use and long-term predictability of new systems. Implants have come a long way in their relatively short history, and in some cases, they may be the preferred treatment modality. However, implants aren’t always the answer.
A dentist’s primary goal is to maintain the patient’s optimal oral health, including the natural dentition. Although some general dentists may believe implants are better than endodontically preserving natural teeth, this idea is not scientifically supported by the literature. In fact, most studies show that an implant and a single-rooted endodontically treated tooth have similar success rates, but implants lead to a higher rate of postoperative complications.1,2
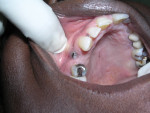
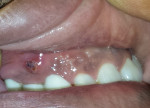
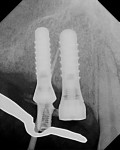
Table 13-11 provides several considerations for placing an implant verses saving the natural tooth, such as the location of the implant, the quality of available bone, and various systemic factors. For example, placing implants in the esthetic zone, especially in the anterior maxillary region, often presents a challenge (Figure 1).3 Systemic factors can contribute to peri-implantitis (Figure 2 and Figure 3) and reduce the survival rate for implants.9
In situations such as these, oral health care providers must consider what they would want if it was their tooth. This introspection may help the practitioner decide what is in the best interest of the patient and provide transparency. Because of the information proliferation on the Internet and social media, patients believe they are now better educated on dental options and services. If dentistry is to remain grounded in integrity, honesty, and trust, then dentists must provide patients with all options for making informed decisions.
Typically, implants are the best option if the natural tooth can’t be saved. However, many dentists will choose extraction following a previous root canal treatment without determining why it failed or whether the benefits of a nonsurgical retreatment can be realized. Sjogren et al12 in a 10-year follow-up study noted that the success rate for retreatment is 98% when the case has no apical periodontitis. Farzaneh et al13 reported in a 4-year follow-up study that the rate can be as high as 86% in cases with apical periodontitis. This article presents nonsurgical retreatment, issues leading to root canal failure, reasons for endodontic failure, and considerations and techniques for retreatment.
Reasons for Root Canal Failure
Endodontic failure occurs for several reasons, which include leaking or poorly sealed restorations, root fractures, untreated canals, inadequately cleaned canals, significant overfills, human error (eg, placement of posts), separated instruments, blocks, ledges, perforations, zips, and transportations.14 In addition, bacteria plaques outside the root, microorganisms such as Enterococcus Faecalis, viruses, yeasts, and foreign bodies may cause failure.15 Practitioners should consider these issues when rendering root canal therapy and retreatment.
Retreatment Considerations
Biological, esthetic, clinical, functional, and financial factors must be considered.
Periodontal Status
· Evaluate periapical and bitewing radiographs to ensure the tooth has a solid bone support.
· Confirm the attachment apparatus is intact unless it is widened due to infection or draining sinus tract.
· Ensure periodontal probing is within normal limits unless a sinus tract is draining from the sulcus.
· Determine if there is a good crown-to-root ratio.
· Ensure no significant mobility or depressibility unless due to a draining sinus tract.
Tooth Restorability
· Assess the strategic value of the tooth.
· Consider remaining tooth structure before and after treatment completed.
· Determine periodontal support.
Patient Concerns
· Compare costs for retreatment, post/core, and crown, if necessary, to those of implant and crown.
· Communicate the prospects of success and failure.
· Inspire motivation for follow-up visits.
Before retreatment, communicate clearly with the patient and the restorative dentist the diagnosis, prognosis, and treatment options if the tooth cannot be saved. In addition, discuss with the patient that no dental procedure is always successful. When patients are presented with the option of an implant or retreatment of a failing root canal, most would choose retreatment to retain the natural teeth. Retreatment is less invasive, less expensive, and less time consuming than the implant alternative.
Case Presentation
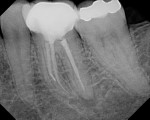
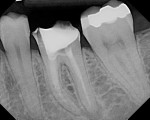
A 34-year-old female presented with pain to the dental office. A root canal had been performed 3 months ago by a general dentist. Previous endodontic treatment with acute apical periodontitis was the diagnosis. The patient did not exhibit swelling. She reported taking over-the-counter pain medications but no antibiotics. She had no contributory medical history. Clinically, a crown was present but no visible redness or inflammation around the gingiva. Radigraphically, root canal treatment was evident, with a separated file in the middle of the mesiobuccal (MB) root, short fills on the mesial and distal roots, and a missed distal canal. Periapical lesions were present at the apex of the mesial and distal roots (Figure 4).
The Retreatment Technique
Profound Anesthesia
An inferior alveolar nerve block was used with two carpules of 2% xylocaine 1:100,000 epinephrine (Cook-Waite, www.carestreamdental.com). This achieved profound anesthesia for this case.
However, if the nerve block is not sufficient for causing complete anesthesia, infiltration with articaine 1:100,000 epinephrine (Septodont, www.septodontusa.com) can help.
Rubber Dam
Use of the rubber dam is the legal, ethical, and clinical standard of care in North America. It allows isolation of the tooth from bacteria in the oral environment, enhances visualization, and protects the patient from iatrogenic errors such as bur slips and swallowing or aspirating items such as rubber dam clamps, endodontic files, and restorative materials.
Access
An SS White Great White Z round diamond high-speed bur (SS White, www.sswhiteburs.com) was used to initiate access through the ceramic crown. They are also good for access through zirconium crowns. The Great White 2 fissured carbide high-speed bur was used to gain access through the metal and de-roof the pulp chamber.
Visualization
Perform endodontics, especially retreatment, at the highest visualization level, ideally with the use of a surgical operating microscope (Global Surgical Microscope, www.globalsurgical.com) (Figure 5). Working without optimal visualization or magnification will increase the chance for missed canals, recurrent decay, and iatrogenic events of all types. Upon access, the crown came off due to recurrent decay but the rubber dam remained intact for isolation.
Gutta Percha Removal
The gutta percha was removed with Gates Glidden drills (DENTSPLY, www.dentsply.com) sizes 4, 3, and 2, in that order. The removal of existing gutta percha is not intended to enlarge the canal space. Chloroform and ProTaperTM files (ProTaper Universal S1, DENTSPLY Tulsa Dental Specialties, www.tulsadentalspecialties.com) at 350 RPM were used to remove the remaining gutta percha in the apical third. Chloroform should be used sparingly and introduced into the canal one drop at a time. At all costs, chloroform should be prevented from passing through the apex.
Patency to the Apex
K-files sizes 8 and 10 were used to gain patency to the apex where the previous attempt was 2 mm to 3 mm short. Achievement of apical patency in retreatment is laborious and time consuming; it should not be done too quickly because a zip or canal transportation may occur. Hand K-filesTM (Endo Technic, www.endotechnic.com) should be precurved to give the clinician tactile control over blockages or ledges that might be encountered and inserted with gentle, but intentional pressure into the canal to gain apical length until patency is assured, but always with the use of an irrigant.
Once the gutta percha was removed, a second distal canal was located. The canal was easy to find using the surgical microscope. The mesiolingual , distolingual , and distobuccal working lengths were established with the apex locator. The canals were completely cleaned and shaped with Vortex Blue® 25 mm/0.04 (DENTSPLY Tulsa Dental Specialties) rotary files using 6% sodium hypochlorite. A small cotton pellet was placed in the orifices of these three canals.
Separated Instrument Removal
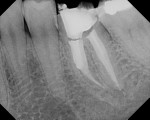
The separated instrument from the previous root canal treatment in the apical third of MB root canal was then addressed. A size 3 Gates Glidden drill was modified by dissecting the cutting edge in half (Figure 6). Using the surgical microscope, the modified drill was inserted down the MB canal with straight-line access to create a platform on top of the broken file. Ultrasonics (ENAC Osada, www.osadausa.com) was used with a SP-19 tip very carefully counter clockwise. The broken file disengaged and was successfully removed (Figure 7). The MB canal was cleaned and shaped with Vortex Blue 25 mm 0/.04 taper as well. The cotton pellet that was placed in the other three canals prevented the separated instrument from popping out of the MB canal and entering one of the other canals.
A small perforation was in the area where the file was engaged. This was addressed upon completion. Knowing how to manage all these events is critical for endodontic retreatment. Calcium hydroxide (UltraCal®, www.ultradent.com) was placed inside all four canals (Figure 8). A cotton pellet and Cavit were placed. The crown was left off per the patient’s request and to prevent leakage. She was told her general dentist can make a temporary crown for her to wear before completion. The patient was scheduled to return in 2 weeks to complete treatment and was told to take 800 mg of ibuprofen for pain control. No antibiotics were prescribed.
Completion Visit
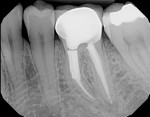
The patient returned and reported no symptoms. She was anesthetized with two carpules of 2% xylocaine 1:100,000 epinephrine, and a rubber dam was applied. Access was made through the Cavit, and the cotton pellet was removed. The canals were irrigated with 6% sodium hypochlorite to remove the calcium hydroxide. The working length was reestablished, and canals were recleaned and shaped with Vortex Blue 25 mm/0.04 taper. A cone fit was established on all four canals. The smear layer was removed by a 1- to 2-minute rinse of 17% liquid EDTA (Henry Schein, www.henryschein.com), irrigated with 6% sodium hypochlorite, then dried with alcohol and paper points. A warm, vertical obturation technique using Kerr EWT (Sybron Endo, www.sybronendo.com) sealer was performed on all four canals. However, the MB canal perforation was repaired with white ProRoot® MTA (DENTSPLY Tulsa Dental Specialties) and filled to the orifice. A cotton pellet and Cavit G (3M ESPE, www.3m.com) was placed, and the patient was told to have the tooth restored within 30 days. She was also scheduled for a 6-month recall to evaluate healing using radiograph (Figure 9).
Postendodontic Coronal Seal
The importance of the restoration cannot be overstated, especially after retreatment. In the endodontic literature, coronal microleakage is correlated with clinical failure. Studies show leakage into the canal space can occur if the tooth is not permanently restored within 30 days.
The patient returned in 6 months to evaluate healing. According to studies, 6 months is the minimal time to see distinct radiographic healing. She reported she had no symptoms. In addition, she had had a new core and crown placed. Radiographic healing was evident (Figure 10).
Discussion
When considering an implant, ethical questions should arise as to whether a previously treated root canal tooth can be retreated. Health care professionals must offer patients all options in a nonbiased way to empower them with educated and informed decision-making. Although the use of an implant is highly effective when the natural tooth is hopeless, an implant option should not be the default when a previous root canal does not heal. Practitioners may be misguided by the perception that single-tooth implants have high success rates and have easier protocols for insertion compared to endodontic treatment. Consequently, endodontic care as part of the treatment plan is often overlooked. This may be a mistake, particularly with new materials and technologies in endodontics leading to better success rates.
Research has shown a restored endodontically treated tooth and single-tooth implant restorations have comparable failure rates but both treatments have high success rates if performed correctly. However, these studies have also shown that patients receiving implants tend to have more issues related to maintenance and postoperative complications. Goodacre et al2 and Torabinejad et al17 in separate studies reported these complications may include hemorrhage, neurosensory disturbances, bisphophonates, adjacent tooth devitalization, mandibular fracture, air emboli (sometimes fatal), and implant abutment screw loosening/breakage.2,17
Conclusion
Endodontic retreatment is inherently complex. The highly skilled endodontist is usually always challenged when facing cases such as these. Findings from a survey18 of endodontically treated teeth by endodontists and general practitioners showed that endodontists had higher success rates of 98.1% compared with general dentists who had a success rate of 89.7%. Retreatment should be considered before apical surgery. Studies show that reteatment can increase the success rates of apical surgery if necessary.19 However, understanding which teeth are restorable and which should be extracted is key before endodontic retreatment is to be considered.
For the endodontist, a vertical root fracture is an ever-present challenge. These usually will result in extraction. However, many teeth can be saved by endodontic retreatment and/or apical surgery. Furthermore, the ultimate fate of retreatment procedures rests largely in the clinician’s ability to achieve a tight coronal seal with the final restoration. Endodontic retreatment is generally a microsurgical specialist procedure, and attempting it without the correct equipment, training, and supplies can be disastrous. Performing retreatment without the needed skills and equipment usually creates further iatrogenic events and tooth loss. The American Association of Endodontists has a free clinical decision guide called Treatment Options for the Compromised Tooth, which has a plethora of information to help the dentist evaluate and make a sound clinical decision on whether a tooth should be saved or extracted. It can be found at http://www.aae.org/uploadedfiles/clinical_resources/treatment_planning/2014treatmentoptionsguidefinalweb.pdf.
This author urges dentists to carefully consider whether an endodontically treated tooth should be retreated. Typically, nonsurgical retreatment can preserve the natural tooth or lead to an apical surgery, if needed. Saving the natural tooth can also be less expensive and biologically more effective. Advances in technology such as ultrasonics, apex locators, intracanal irrigation, and magnification has made nonsugical retreatment possible and highly successful.20
References
1. Doyle SL, Hodges JS, Pesun IJ, et al. Retrospective cross sectional comparison of initial nonsurgical endodontic treatment and single-tooth implants. J Endod. 2006;32(9):822-827
2. Goodacre CJ, Bernal G, Rungcharassaeng K, Kan JY. Clinical complications with implants and implant prostheses. J Prosthet Dent. 2003;90(2):121-132.
3. Chee W, Jivraj S. Failures in implant dentistry. Br Dent J. 2007;202(3):123-129.
4. Noack N, Willer J, Hoffmann J. Long-term results after placement of dental implants: longitudinal study of 1,964 implants over 16 years. Int J Oral Maxillofac Implants. 1999;14(5):748-755.
5. van Steenberghe D, Quirynen M, Molly L, Jacobs R. Impact of systemic diseases and medication on osseointegration. Periodontol 2000. 2003;33(1):163-171.
6. Becktor JP, Isaksson S, Sennerby L. Survival analysis of endosseous implants in grafted and nongrafted edentulous maxillae. Int J Oral Maxillofac Implants. 2004:19(1):107-115.
7. August M, Chung K, Chang Y, Glowacki J. Influence of estrogen status on endosseous implant osseointegration. J Oral Maxillofac Surg. 2001;59(11):1285-1289.
8. Kan JY, Rungcharassaeng K, Kim J, et al. Factors affecting the survival of implants placed in grafted maxillary sinuses: a clinical report. J Prosthet Dent. 2002;87(5):485-489.
9. Klokkevold PR, Han TJ. How do smoking, diabetes, and periodontitis affect outcomes of implant treatment? Int J Oral Maxillofac Implants. 2007;22 Suppl:173-202.
10. AAE Special Committee on Bisphosphonates. Endodontic implications of bisphosphonate-associated osteonecrosis of the jaws. AAE Position Statement. https://www.aae.org/uploadedfiles/clinical_resources/guidelines_and_position_statements/bisphosonatesstatement.pdf. Accessed June 22, 2015.
11. Morris HF, Ochi S, Winkler S. Implant survival in patients with type 2 diabetes: placement to 36 months. Ann Periodontol. 2000;5(1):157-165.
12. Sjogren U, Hagglund B, Sundqvist G, Wing K. Factors affecting the long-term results of endodontic treatment. J Endod. 1990;16:498-504.
13. Farzaneh M, Abitbol S, Friedman S. Treatment outcome in endodontics: the Toronto study. Phases I and II: orthograde retreatment. J Endod. 2004;30(9):627-633.
14. Sjogren U, Hagglund B, Sundqvist G, Wing K. Factors affecting the long-term results of endodontic treatment. J Endod. 1990;16(10):498-504.
15. Lin LM, Skribner JE, Gaengler P. Factors associated with endodontic treatment failures. J Endod. 1992;18(12):625-627.
16. Siqueira JF Jr. Aetiology of root canal treatment failure: why well-treated teeth can fail. Int Endod J. 2001;34(1):1-10.
17. Torabinejad M, Anderson P, Bader J, et al. Outcomes of root canal treatment and restoration, implant-supported single crowns, fixed partial dentures, and extraction without replacement: a systematic review. J Prosthet Dent. 2007;98(4):285-311.
18. Alley BS, Kitchens GG, Alley LW, Eleazer PD. A comparison of survival of teeth following endodontic treatment performed by general dentists or by specialists. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2004;98(1):115-118.
19. Bergenholtz G, Lekholm U, Milthon R, et al. Retreatment of endodontic fillings. Scand J Dent Res. 1979;87(3):217-224.
20. Friedman S, Mor C. The success of endodontic therapy--healing and functionality. J Calif Dent Assoc. 2004;32(6):493-503.