A Four-Unit Model-Free Restorative Case with Monolithic Zirconia
Maximizing digital workflow with advanced restorative materials
In the recent discussions of digital dentistry and the increased efficiency that it can bring, the focus has largely been on the digital tools themselves and new digital workflows. This is understandable, given that these technologies are the backbone for all other results in the digital procedure. But while digital tools for dentists and labs have been advancing, so have restorative materials, which deserve attention as well. The milling material chosen for a digital case is a vital part of the equation for the overall success of the workflow. If a material doesn’t perform as it should or offer the properties that dentists and labs need to achieve maximum productivity, it makes no contribution to the trends that are advancing dentistry workflows.
Fortunately, dentists and labs today have a number of choices in milling materials that help them achieve an ideal balance of strength, esthetics, and productivity. This is particularly true in the case of monolithic restorations. Although monolithic zirconia was formerly criticized for delivering mediocre esthetics,1,2 newer material options are giving dentists increased translucency without compromising the strength of zirconia.2
In any discussion of the esthetics of a monolithic zirconia crown, it’s worth noting that one of the chief alternative restorative materials—porcelain-fused-to-metal (PFM)—has its own issues with esthetics.3 Monolithic zirconia allows dentists to avoid the problems of metal showing at the gumline or a gray hue showing through the crown. Beyond esthetics, monolithic zirconia has several additional advantages over PFMs. It eliminates the risk of porcelain fracturing. It may also be lower in cost, thanks to the fact that a monolithic milled restoration typically requires less time from the laboratory technician than a layered PFM.2,4 Additionally, if adjustments are needed at the seating appointment, a dentist can work on a monolithic crown without the fear of exposing underlying metal structure.
The combination of a reliable monolithic zirconia material with an all-digital workflow is now giving labs and dentists an exciting opportunity to practice 21st century dentistry by going model free.5,6 While a model-free workflow demands outstanding accuracy from the dentist’s digital scans, as well as skilled use of CAD/CAM systems by the lab, when done well, it is a truly efficient and predictable process. The author and his laboratory, Synergy Ceramics, have been producing single-unit monolithic zirconia crowns using a model-free workflow for approximately 1 year. The team recently pushed this workflow a step further with the 4-unit crown case discussed below.
The material used in this case, Lava™ Plus High Translucency Zirconia (3M ESPE, www.3mespe.com), is a high-translucency version of the classic Lava zirconia with which many dentists are already familiar.7 Because the material is more translucent than other shaded zirconia, it is suitable for both monolithic restorations as well as traditionally layered restorations. Field evaluations conducted with dental labs comparing the material with other zirconia systems have found that lab technicians felt Lava zirconia offered better esthetics than other monolithic restorations (application test Lava™ Plus High Translucency Zirconia with 11 responding dental labs in Germany, Austria, Italy, Netherlands, and United States; unpublished data; 2011). Beyond its translucency, the zirconia also has a shading system that makes results predictable for the lab; it includes dyeing liquids that match the VITA Classical A1-D4 shades (Vident, www.vident.com), including bleached shades offered by 3M ESPE.
The case shown here will illustrate how this monolithic material was used in a model-free workflow to create four crowns. The combination of in-office scanning, digital design and milling, and use of an esthetic yet strong monolithic material enabled a predictable workflow with excellent results.
Case Presentation
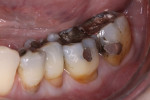
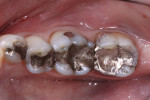
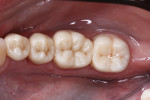
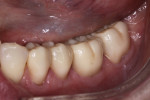
The patient was an approximately 65-year-old woman who presented to the office with discomfort while chewing on the left side. An examination revealed four large amalgam restorations on No. 18 through No. 21 with a poor marginal seal and recurrent decay. The teeth also displayed chipping and cracking, as well as recession on the buccal side (Figure 1 and Figure 2). The accepted treatment plan called for removal of the amalgam restorations and placement of four full-coverage monolithic zirconia crowns.
A disposable triple tray was used with Affinity Crystal (Clinician’s Choice, www.clinicianschoice.com) to capture preoperative impressions. The patient was anesthetized, and the amalgam restorations were removed, along with recurrent decay. Scotchbond™ Universal Adhesive (3M ESPE) was applied to the preps and Zircules™ (Clinician’s Choice) was used to perform core buildups. Standard preps were created with chamfer finish lines and 1 mm of reduction facially, lingually, interproximally, and occlusally.
Four individual size 00 retraction cords were placed around the teeth and then removed, and the preps were digitally scanned. After confirming the completeness of the digital impression, the case was submitted to Synergy Ceramics. Provisionals were then fabricated using Luxatemp (DMG America, www.dmg-america.com) in shade A3. The provisionals were trimmed and the occlusion was adjusted, followed by polishing. The provisionals were cemented with Cling2® Temporary Cement (Clinician’s Choice).
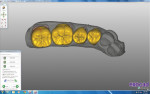
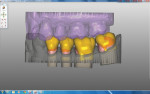
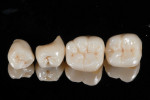
At the lab, Exocad (Impressum, https://exocad.com) software was used to design the monolithic restorations (Figure 3). The software is capable of creating secondary anatomy and compensating for occlusion and contacts; therefore, no model was needed (Figure 4). The crowns were milled using a Lava mill and Lava Plus zirconia. After milling, the crowns were refined and surface-stained, followed by sintering. An additional staining liquid was used after sintering, and the crowns were hand-polished (Figure 5).
The restorations were returned to the dental office without a model, and the patient returned for placement. The provisionals were removed, and each crown was then tried in individually. The crowns were then tried in two at a time, three at a time, and finally all four at once. The marginal fit, contacts, and occlusion were evaluated, and it was determined that no adjustments were necessary.
The crowns were removed from the mouth and Ivoclean cleaning paste (Ivoclar Vivadent, www.ivoclarvivadent.us) was used to clean the inside surfaces. The crowns were then rinsed and dried out. It should also be noted that 3M ESPE recommends that the bonding surfaces of the restorations be sandblasted prior to seating.
The preparations were cleaned and isolated, and the four crowns were then seated at the same time using RelyX™ Luting Plus Cement (3M ESPE). A light was used to tack-cure the cement for 20 seconds on the buccal and facial sides, and any excess amounts of cement were then removed and interproximal flossing was performed (Figure 6). The patient was instructed to bite down on a cotton roll for 4.5 minutes while the cement auto-cured, and final cleanup was then performed with scalers, curettes, and floss. Final x-rays were then taken to confirm the seat.
The patient was very pleased with the final result, thanks not only to the improved esthetics, but her improved overall comfort (Figure 7 and Figure 8).
Discussion
Agreeing to attempt a model-free procedure in a single-unit case, let alone four units, requires that the dentist place a great amount of trust in the laboratory. However, in this case, the long working relationship between the author and the lab, as well as their successful track record with single-unit model-free cases, made taking this step seem like a logical evolution of the digital workflow.
The improving esthetics of monolithic zirconia are making it an increasingly versatile option, particularly in the hands of a skilled lab technician. This material—with its easy matching to VITA shades—can produce very predictable and consistent results, as demonstrated in this case. Because additional staining can be performed after sintering, as was done here, the lab maintains a great deal of control and flexibility at all stages in the creation of the crowns.
Not every lab or dental office has the tools to go model-free, but those that do should consider whether they are ready to attempt this workflow. If digital scanning and design tools are applied well and combined with reliable and esthetic materials, they can further optimize the workflow to increase efficiency while producing strong and lifelike restorations.
References
1. Fahl N Jr, McLaren EA, Margeas RC. Monolithic vs. layered restorations: considerations for achieving the optimum result. Compend Contin Educ Dent. 2014;35(2):78-79.
2. Griffin JD Jr. Combining monolithic zirconia crowns, digital impressioning, and regenerative cement for a predictable restorative alternative to PFM. Compend Contin Educ Dent. 2013;34(3):212-222.
3. Christensen GJ. The confusing array of tooth-colored crowns. J Am Dent Assoc. 2003;134(9):1253-1255.
4. Ronay V, Bindl A, Sahrmann P, Schmidlin PR. Retrospective evaluation of CAD/CAM cantilever reconstructions to restore compromised posterior teeth: a preliminary report. Int J Prosthodont. 2014;27(2):165-168.
5. Bunek S, Brown C, Yakas M. The evolving impressions of digital dentistry. Inside Dentistry. 2014;10(1):35-39.
6. Ceranic D. Trends in implant dentistry: model-less restorations. Inclusive Implant Magazine. 2013;4(2). www.glidewelldental.com/inclusive-magazine/volume4-2/implant-dentistry-trends.aspx. Accessed May 9, 2014.
7. 3M ESPE. Lava Plus High Translucency Zirconia System, Technical Product Profile. 3M ESPE website. https://multimedia.3m.com/mws/mediawebserver?mwsId=SSSSSuH8gc7nZxtUPx_Bo8mUevUqe17zHvTSevTSeSSSSSS--&fn=Lava_Plus_tpp.pdf. Accessed May 9, 2014.
About the Author
Robert G. Ritter, DMD
Private Practice
Jupiter, Florida