Considerations for Diode Laser Surgery
Technology and technique play important roles in successful outcomes
Instruments used today to perform dental surgical techniques have evolved over hundreds of years, starting with the scalpel in the 1800s, electrosurgery in the 1920s, and various types of lasers over the course of the past 25 years. Besides the scalpel, today’s primary forms of instrumentation include electrosurgery, diode lasers, carbon dioxide (CO2) lasers, and erbium lasers. No one instrument is capable of fulfilling all the needs of dentists and patients for the entire range of surgical procedures. In fact, the optimal surgical instrument would have to comply with patient demand for comfortable procedures with esthetically appealing results and with the dental practitioner’s need for efficiency with predictable outcomes.
Surgical Technique Challenges
Dental practitioners face a number of challenges when using surgical equipment.
A challenge with laser instruments in particular can be achieving smooth, snagless cutting with tactile feedback. While a scalpel is usually easy to guide along a planned trajectory, some laser instruments are known for stalling and dragging during the cutting process. The laser fiber may intermittently lose its ability to cut and can catch on tissue. To remedy this, the fiber must be frequently reinitiated in order to cut. If not immediately noticed, stalling and dragging may result in unnecessary collateral thermal damage because the time on tissue is extended. Other laser devices work in a non-contact mode and have no tactile feedback, which precludes the dentist from being able to “feel” the tissue while cutting—a major drawback to the use of these lasers for soft-tissue surgery.
Controlling thermal collateral damage is another challenge for dentists. All surgical instruments with a thermal component—especially electrosurgery instruments—can tend to cause thermal damage during cutting. This is a function of the heat created and the speed at which the cutting instrument glides over tissue. Classic electrosurgery systems are known for extensive collateral thermal tissue damage,1 and they may also damage tissue and bone around implants if touched. Diode lasers can also produce thermal tissue damage that may potentially be extensive depending on cutting speed. Both of these modalities are technique-sensitive.
Reducing the time spent on tissue is another issue. For standard diode lasers with fixed power, collateral tissue damage greatly depends on the speed of cutting. With low speed caused by a snag or drag, the extent of collateral damage can exceed 1 mm. Hemostasis requires no more than 200 µm to 500 µm; therefore, 1 mm or more of tissue coagulation corresponds to a significant over-treatment. Extensive thermal tissue damage has multiple implications in the success of a procedure, the postoperative phase, and the esthetic outcome. Results may be similar to a third-degree skin burn—ie, extensive tissue necrosis, long healing times, scar tissue formation, and uncontrollable tissue recession.
Clinicians must also be cognizant of protecting sensitive structures from overheating. Removing soft tissue on or around structures—such as natural teeth, teeth with dental crowns, or dental implants—is a concern when using diodes and other lasers in the 800 nm to 1,100 nm range. This laser radiation can penetrate deep into tissues and heat up highly absorbent dental materials or dental implants that conduct heat to the surrounding soft tissue and bone. Extensive collateral thermal damage to these structures is possible. Monopolar electrosurgery is not recommended around metal objects, such as teeth with dental crowns or dental implants.
Another issue is maintaining hemostasis and wound sealing. Non-thermal cutting techniques like the scalpel require chemical and mechanical methods to stop bleeding and seal blood vessels. The resulting open wounds may also require some kind of wound closure, such as sutures, to enhance the healing process and avoid infection. Thermally oriented surgical instruments, such as electrosurgery, diode lasers, and CO2 lasers, cauterize as they cut to a depth of more than 200 µm, so blood and lymphatic vessels are sealed and wounds are protected from infection. An exception is the erbium cut, which does not provide sufficient cauterization (<50 µm) for many blood vessels and, therefore, requires additional methods of hemostasis.
Finally, clinicians must also be careful to avoid technique-related operative and postoperative discomfort. Different surgical techniques and procedures have varied requirements for pain control. Electrosurgery is perhaps the most pain-inducing technique due to the sometimes extensive burning of tissue. In some instances, excessive fumes and the smell of burning tissue might also have a psychological effect on patients and may enhance the pain perception. Moreover, the postoperative phase might be longer with considerable discomfort because of the excessive tissue damage.
Non-Contact vs. Contact Cutting
While most surgical instruments contact the tissue to be cut, some laser systems require that a certain distance from the surgical site be maintained. The most prominent non-contact laser devices are CO2 lasers and erbium lasers. Both of these laser systems have good absorption in soft tissue, ie, the laser light interacts directly with oral tissues to create the cutting effect. The direct laser light absorption by oral soft tissues also means that laser energy remains localized and focused, leading to lower heat generation in surrounding tissues and virtually no penetration of laser light into deeper tissue layers. The cuts obtained with these lasers are clean and, depending on the mode used, exhibit a small coagulation zone around the cut, with a depth ranging from 5 µm to 500 µm. However, because the specific laser wavelengths travel through standard quartz glass fibers, both CO2 and erbium lasers require complicated light transport systems and optical handpieces with specific focal points to work in a clinical environment. The handpiece must be held at a certain distance to achieve a good focal point that cuts tissue, similar to using a magnifying glass to focus sunlight. This is counterintuitive to many dentists. Also, the absence of tactile feedback means that observation alone defines the field of operation, cutting depth, and width, which may require a steep learning curve for the clinician.
Except for the scalpel, most soft-tissue contact-cutting technologies use some form of heat to produce a cut. The electrosurgery device uses an electrical current to create heat and perform a cut; other variants of the electrosurgical device use radio waves to create heat.
Another and very popular device for contact surgery is the near-infrared diode laser. Near-infrared lasers, such as diode or Nd:YAG lasers, have wavelengths ranging from 800 nm to 1,100 nm and use quartz fibers to transport laser light from the laser source to the target tissue. The fiber walls have a reflective cladding that keeps the laser light inside the fiber; the laser light bounces back and forth from wall to wall, and finally exits at the distal end, or the fiber tip. If the fiber tip has a clean fresh cleave, the laser light will exit freely and penetrate into the tissue below. When tissue effectively absorbs the laser light—as with CO2 and erbium lasers—most of the light is absorbed in the top tissue layer, leading to a rupture of the tissue, ie, cutting. For near-infrared lasers, light tissue interaction is completely different. For soft tissue, such as the reticular layer of mucosa with 70% water and 5% blood, total absorption coefficient is as low as 0.2 cm-1 to 0.65 cm-1. In the 800 nm to 940 nm range, the dominating absorption occurs in blood, and for the 970 nm to 1,100 nm range, the absorption in water and blood are comparable. Because the tissue is a poor absorber of the near-infrared laser light—for example, oral soft tissue for a diode or Nd:YAG laser—the light will then penetrate into deeper layers of the tissue.2 This may lead to heat build-up in larger tissue areas and damage sensitive structures beneath the soft-tissue layer being irradiated.
A New Option
A new generation of diode laser technology, Thermo-Optically Powered (TOP) surgery has been developed with the goal of meeting the challenges and issues associated with conventional contact surgical technologies. TOP surgery technology cuts, cauterizes, and disinfects soft tissue for oral surgery3-5 using a computer-controlled semi-conductor laser as a power source whose power is converted into thermo-optical power in the system’s thermo-optically powered tip. A regulating mechanism continuously adjusts the output power of the laser to ensure constant preset temperature at the tip, thus maintaining constant cutting conditions for soft tissue that are almost independent of the speed of cutting.
The power source of the TOP surgery system is a laser. Laser light is monochromatic, ie, light of one specific wavelength, with low absorption in oral soft tissue.6 In the TOP system, this light is transported to the unique tip, where the laser light undergoes a conversion from monochromatic light to thermal power and polychromatic light with wavelengths in the range of 1,400 nm to 11,000 nm. The thermal power that is created in the system’s tip constitutes the primary cutting mechanism. During surgery, the tip is in direct contact with soft tissue, and thermal power is transported to the soft-tissue surface conductively for a thermo-mechanical cut. The dentist maintains tactile feedback at all times during the cutting process.
The tip is a quartz glass fiber with sintered particles and ions integrated into the glass structure, highly absorbing laser light. Laser irradiation is highly absorbed at the distal end of the tip, with the tip heating up to 500°C to 900°C.
Since this temperature is the temperature of the tip, and not of the tissue, the tissue temperature is much lower during cutting. The TOP surgery system allows the user to set the tip temperature anywhere within this range, or preprogrammed presets for the most common dental surgical procedures with optimized temperature settings can be used. Additionally, for safety the surgery system is capable of sensing a stop in hand movement and shuts down the power to avoid tissue overheating.
Conclusion
Developments in soft-tissue contact laser surgery are resulting in the creation of a new generation of lasers. New technology is enabling consistent use of thermal power generated from poorly absorbed laser radiation; computer-controlled, highly reproducible fiber initiation; and the ability to maintain a pre-selected temperature of the fiber tip with automated power control. These innovations in diode laser technology are aimed at significantly reducing dependence on operator technique, particularly for cutting speed; they allow consistent cutting and minimize snag, drag, and collateral thermal damage of the tissue. This may improve the clinical outcome in soft-tissue surgery while controlling the side effects in wound healing.
References
1. Goharkhay K, Moritz A, Wilder-Smith P, et al. Effects on oral soft tissue produced by a diode laser in vitro. Lasers Surg Med. 1999;25(5):401-406.
2. Romanos GE, Pelekanos S, Strub JR. Effects of Nd:YAG laser on wound healing processes: clinical and immunohistochemical findings in rat skin. Lasers Surg Med. 1995;16(4):368-379.
3. Feldchtein FI, Magid KS, Belikov AV, et al. Soft tissue surgery with a 980 nm diode laser: direct laser cutting or hot tip? [abstract]. ALD 2011 Annual Meeting. San Diego CA: Academy of Laser Dentistry; 2011. Abstract TH-13.
4. Magid KS, Belikov AV, Pushkareva A, et al. Soft tissue surgery with thermo-optical tips with a real-time temperature control [abstract]. ALD 2010 Annual Meeting. Miami FL: Academy of Laser Dentistry; 2010. Abstract TH 27-28.
5. Altshuler G. Thermo Optically Powered (TOP) Surgery: A new opportunity for the dental practice. ALD 2012 Annual Meeting. Scottsdale, AZ: Academy of Laser Dentistry; keynote lecture 2012.
6. Manni JG. Dental Applications of Advanced Lasers (DAAL). Burlington, MA: JGM Associates, Inc.; 2007:240.
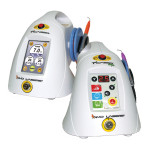
Figure A | Picasso®
The Picasso® line of soft tissue dental lasers from AMD Lasers, a DENTSPLY International Company, enables every dental practice to provide treatment for soft tissue surgery, periodontal treatment, endodontic treatment, and laser whitening. Ideal for both first-time and experienced laser practitioners, Picasso offers the convenience of disposable tips and strippable fiber.
866-999-2635
amdlasers.com
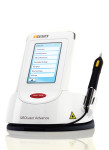
Figure B | WaterLase iPlus™
The Waterlase iPlus™ system dual-wavelength all-tissue laser from Biolase Technology is designed to provide improved cutting speed and precision for broader applications. It features the highest pulse energy at short pulses among all erbium-based, 3-micron lasers. With an intuitive user interface, it also allows for fast removal of hard tissue with no patient discomfort.
888-424-6527
biolase.com
Figure C | SIROLaser Advance
SIROLaser Advance, the battery-operated 980-nm soft tissue diode laser from Sirona offers a unique concept combining intuitive user navigation, individual customizable settings, and programmable PIN codes along with preset therapy programs in endodontics, periodontics, and oral surgery. It also features favorite settings for fast execution and an integrated finger switch.
800-659-5977
sironausa.com/us
Figure D | SOL®
The SOL® Laser from DenMat is a highly versatile and completely customizable soft-tissue diode laser. SOL offers accuracy and efficiency through a high-contrast aiming beam that can be used for gingival contouring, tissue retraction, and laser-assisted periodontal therapy. This lightweight, portable laser is designed for both novice and experienced users.
800-4DENMAT
denmat.com
Figure E | PerioLase® MVP-7™
Millennium Dental Technologies PerioLase® MVP-7™ for the LANAP Protocol is first laser in the dental industry to incorporate an Android-based digital display and control system. The PerioLase MVP-7 combines its advanced laser components with the latest LCD display technology and a 360° mounting system for the optimal operating experience.
888-638-5262
lanap.com
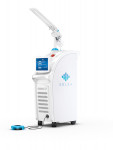
Figure F | Solea™
Solea™ from Convergent Dental, Inc. is the world’s first computer-aided CO2 laser system to be cleared by the FDA for both hard and soft tissue procedures. Dentists perform over 94% of their Solea procedures without anesthesia and over 98% of those patients report feeling no pain, with 100% preferring Solea over the drill.
800-880-8589
convergentdental.com
ABOUT THE AUTHOR
Georgios E. Romanos, DDS, PhD, Prof Dr med dent
Professor, Department of Periodontology
Stony Brook University School of Dental Medicine
Stony Brook, New York