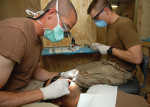
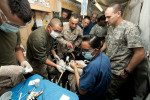
Dentist Deployed
With “mission readiness” more crucial than ever, military dentists play a vital role in making sure combat troops are in optimal dental health.
By Allison M. DiMatteo, BA, MPS
A young general dentist began his career in the military with the 1st Brigade, 101st Airborne Division in 1987 and was deployed to Desert Shield/Desert Storm, serving in the 326 Medical Battalion. He answered to the battalion commander, who answered to his brigade commander, who in turn answered to the division commander. It was a war-fighting mission.
His basic instruments were lightweight but durable and, along with his materials, fit in a bag no bigger than the size of a small gym bag. It could be carried with him when moving from one place to the next. If someone came to him with a broken tooth or a toothache, he could treat him or her quickly without having to pull what he needed out of a truck that might not even be in the same general vicinity as he was.
Everything was developed for dentists to use in an austere environment and could be thrown on the back of a truck, onto a helicopter, or inside an armored personnel carrier. Drills, headlights, and radiography equipment were all battery-powered and portable They still are today.
During the ramp up for the conflict, the types of injuries he would see most commonly were minor injuries to dentition and lacerations. When the conflict started, however, this dentist's role became that of triage officer for his brigade. That meant that as the soldiers or enemies were wounded and brought in to the Battalion Aid Station, his job was to sort them out into who should be treated first, who could wait, who was stable, and ultimately, if somebody was hurt to the extent that they weren't expected to survive, to make that call, too.
“The general dentists would identify somebody who had a facial injury, after which they would be evacuated further behind the lines to a Combat Support Hospital or MASH Hospital, where an oral and maxillofacial surgeon would be assigned,” recalls Thomas Borris, DDS, the retired Army Dental Corps officer sharing his stories about being a general dentist and oral and maxillofacial surgeon during wartime. “The mission at that point is to examine the injuries and stabilize the patient enough so they could be further evacuated out of the theater.”
The injuries that a deployed oral and maxillofacial surgeon would see included primarily facial trauma, and the trauma could be avulsive, loss of tissue injuries, or penetrating injuries. The first objective was ensuring that the airway was secured, that significant bleeding was stopped, and that further injury would be prevented through different surgical means of stabilizing those wounds, Borris explains. Then, once the patient's injuries were such that they were sufficiently stable and could withstand a long airplane flight from Iraq or Afghanistan to Germany, they would be flown back to the States, where the definitive surgeries and reconstructive element of dentistry occurs.
“Unfortunately, the body armor doesn't cover the head completely, especially the face, so those areas are more prone to injury, just like the extremities are,” Borris notes. “The types of injuries that are most common for our soldiers these days are extremity wounds or head and neck injuries, because those are the areas that you can't completely cover up.”
Dentally Ready, Combat Ready
Imagine. In the midst of a military mission in the Middle East, Lance Cpl. Smith, an experienced sniper, firing squad leader, and convoy turret security person, is distracted by a toothache, the same toothache that has come and gone for the past 3 months. Today he has a splitting headache and is not 100% focused on the mission due to his nagging tooth.
He is a crucial piece of today's mission. He either “toughs it out” or is sent back to a forward operating base for treatment. If he is sent back, then someone else takes his place who may be less knowledgeable and experienced than Lance Cpl. Smith, putting the mission at risk.
“Patients with high dental health/dental readiness have far fewer incidences of emergent dental pain, which decreases the incidence of unplanned manpower loss,” says Rear Adm. Elaine Wagner, Chief of the United States Navy Dental Corps. “Also, studies have shown that students with unmet oral health needs have a harder time concentrating in school and have decreased performance on standardized tests.”
Dental fitness has long been recognized as a vital component of mission readiness. Col. Shan K. Bagby, DC, explains that two things usually happen when a soldier experiences dental pain. First, he or she is less able to focus on their job and second, they usually must leave their work area to seek emergency care.
“This affects both the soldier and their unit, especially when that soldier is part of a small team or possesses a critical and unique skill,” Bagby elaborates. “Keeping soldiers dentally fit ensures that they can perform their military duties when called upon. In short, a dentally fit soldier is better able to serve their country by being mission-ready.”
Mission readiness is crucial today, especially considering that today's wars are fought with much smaller numbers of people performing a mission, explains Col. Gary Martin, DC, of the United States Air Force. If there are only five military personnel to do the mission and one has a dental emergency issue and is distracted, that really impacts the mission; in World War II, there were thousands fighting, so if one of the troops had a toothache, the mission still had a high probability of being accomplished.
“By reducing that need for dental treatment when they are deployed, it reduces their overall risk for injury,” Martin adds. “If a soldier has a dental emergency, most of the time we have to put them into some type of vehicle to get them to the dentist, and that puts them at significant risk of being injured by an improvised explosive device (IED). If they don't have that dental emergency that needs to be treated, they don't put themselves at risk.”
To this end, Wagner continually focuses on dental health and hygiene. Sailors and Marines are required to undergo yearly examinations and cleanings, during which patients are educated in oral hygiene, nutrition, and tobacco counseling.
“These are an integral part of the Navy's Oral Disease Risk Management Protocol,” Wagner says. “The instruction followed is BUMED INST 6600.16A.”
According to Col. Jeffrey Chaffin, DDS, MPH, MBA, MHA, of the United States Army Dental Corps and Chief of the Dental Care Branch of the TRICARE Management Activity (TMA), once military personnel are downrange or in-theater, somewhere away from normal medical and dental facilities, when they experience a dental problem, it's not easy to get that dental problem resolved and actually puts them and the people they serve with at risk. For this reason, the military maintains dental treatment facilities or military dental clinics, often called DTFs, stationed around the world, including in Iraq, Afghanistan, and deployed environments. Each service has military dentists working in those clinics, as well as some contractors.
Additionally, the military's Active Duty Dental Program, which is currently administered by United Concordia, provides purchased care for needed treatments without premiums or cost shares for the more than 100,000 service members living in remote areas—meaning more than 50 miles from a military dental clinic. These service people could be recruiters, going to school, or performing the many different jobs that take them away from a normal base, explains Chaffin. However, they still need to maintain their dental readiness, so the Active Duty Dental Program allows them to receive annual examinations at a network dentist at no cost to them, in addition to any dental care they need. The program also enables military personnel to be referred to a specialist if the demand for care exceeds what can be delivered within a specific military dental clinic, again at no cost.
“We have service members based in every country in the world. When we have military personnel in different countries, we have an overseas medical contract that can take care of their dental needs if they're in a remote area,” Chaffin adds. “We want to ensure that people can maintain their dental readiness, whether they're at a base in the United States, at a base overseas, or if they're in a remote area overseas or in a place in the country where we don't have a dental clinic.”
Preparing for Deployment
“Military dentists should be ready at all times. All of us have ongoing readiness skills verification throughout the year. In addition, we all share the deployment load,” explains Col. William J. Dunn, DDS, USAF. “Military dentists should know well in advance what their window of deployment is so they have plenty of time to prepare. The hardest portion is administrative and personal, such as getting their finances in order, appointing a power of attorney, addressing child care issues, and creating or updating their wills.”
The readiness skills verification program and readiness skills training includes a review of suturing technique and soft tissue management, current treatments for dental infection, triage training and surgical suite procedures review, and stabilization techniques for head and neck fractures, explains Jon M. Dossett, Col, USAF, DC. More senior dental officers will also practice their leadership skills and/or “commander” skills during these training exercises.
“We also have a special training course that puts our medical/dental personnel through a week of expeditionary medical support training. Attendees get experience in building a field hospital, working in that hospital, and then repackaging the facility for return transport,” says Dossett. “Any dental staff during this course will receive hands-on training with actual field dentistry equipment and instrumentation that might be commonly encountered in a deployed field dentistry environment.”
Virtually all deployed field dentistry units have digital intraoral radiographic capability and methods to store or transport information back to a major medical facility for consultation. Prior to deployment, soldiers receive briefings on the locale for deployment, capabilities or services available, and any equipment or communications issues that may be of concern, Dossett adds.
“Deployment dentistry is not much different than any other kind of dentistry because we're able to bring most of our equipment into the theater, and most of the dental clinics now are in a hardened facility with actual walls, whether it's in a trailer or actually in a building,” Dunn explains. “There are mobile dental delivery units that can fit inside an eighteen-wheeler, and we have the same kind of dental chair, delivery devices, and can perform almost any kind of dental procedure.”
Although the dental equipment used in the field will either be a portable unit that military dentists have previously trained on, or a standard chair in a hardened facility, most deployed locations will have little prosthodontic capability, and most likely no laboratory support. Therefore, tooth preparation for crowns and bridges is avoided, but military dentists in the field can handle any emergency procedure.
The US Army's current concept of deployed dental support is outlined in a document in Army Field Manual 8-10-19, “Dental Service Support in a Theater of Operations,” which provides the framework for doctrine, tactics, techniques, and procedures required in order to provide dental service support in a theater of operations. “It is a living document that is regularly reviewed and improved upon as necessary to reflect changes in technology,” Bagby says.
“Before deployment, our providers are trained in a number of areas. Not only are they trained to provide care utilizing field dental equipment, but they also go through a 10-day Tactical Combat Casualty Care (TCCC) course which provides both didactic and hands-on training in the area of triage and emergency medicine,” Wagner explains. “Field exercises focus on combat scenarios dealing with establishing hemostasis, immobilizing joints, chest tubes, airway establishment, needle decompression, etc.”
Additionally, some deployers receive further emergency medicine training. This training takes TCCC to another level, going further in-depth, looking at the anatomy, physiology, form, and function of each emergency maneuver. Providers also go through Battle Skills Training School (BSTS), which provides training that helps them support the infantry Marines, Wagner elaborates.
“They learn the basics of land navigation, security patrols, convoy operations, base security operations, search and seizure, Military Operations on Urban Terrain (MOUT), training on various weapon operations, etc,” Wagner adds.
In terms of how dentists are actually chosen to deploy, Bagby says soldiers are normally either already assigned to a deployable unit or called up based on their place in a centrally managed provider queue named the Professional Filler System (PROFIS). PROFIS looks at the total inventory of available personnel to ensure equitable distribution of assignments and avoid repetitive individual deployments. Once identified, the deploying dentist is given all the requisite field training, medical care, and equipment he or she will need to be successful during their operational tour in a deployed environment, Bagby adds.
In terms of dental readiness, Marines and sailors are prepared for deployment by addressing their active dental disease. Sailors and Marines are required to be Dental Class 1 or 2 (ie, no dental emergencies expected within a year) prior to deployment, Wagner says.
The Oral and Facial Trauma of Conflict
Some of the most traumatic injuries in the field are blast injuries from IEDs, combat operations, and small arms, among others, which can cause a wide array of oral trauma, observes Wagner. Dental personnel are an integral part of the healthcare team and are often utilized to help triage and stabilize the patient.
“At Camp Korean Village, Iraq, one dentist operated out of a hut where the primary goal was sustaining life. If a Marine sustained a blast injury to the head or neck region, the goal was to stop the bleeding, if possible immobilize/splint, and send to the next echelon of care,” Wagner recalls, adding that there are levels of dental capabilities at each base. Smaller bases may only have an Independent Duty Corpsman, but larger posts have more dental trauma capability and often include oral surgeons. “These injuries can often lead to post-traumatic stress (PTS) and mild traumatic brain injury (mTBI); military dentists are practiced in treating patients with these unseen injuries. From our shared experience, we can relate more effectively to Marines and sailors who may need more patience and understanding.”
Today's military are well protected, except for the face. Today's modern soldier wears a helmet, often goggles, a flak jacket, and gloves. They are covered from head to toe, except for their face. As a result, many traumatic injuries would be penetrating blast injuries to the face, Dunn comments. After life-saving procedures and stabilization, these patients require many significant invasive surgeries to rebuild the hard and soft structure of the jaws.
“The military has some maxillofacial prosthodontists who have gone through significant training as far as making prostheses,” Borris elaborates. “We can still surgically do many repairs using bone grafting and reconstructive techniques to maybe eliminate a lot of the need for maxillofacial prosthetics, but if somebody lost an eye, there are people really good at making prostheses to replace those and make the soldier look normal again.”
Forward-deployed facial trauma care is primarily the domain of oral and maxillofacial surgeons assigned to field hospitals, Bagby explains. Army oral surgeons are trained in performing full-scope facial trauma care and thus are tasked with stabilizing hard and soft tissue facial injuries so that patients can either be returned to duty or evacuated for definitive care at fixed-base US military hospitals worldwide, he adds.
“Military oral and maxillofacial surgeons have done an exemplary job of caring for these wounded warriors,” Dunn emphasizes.
“Advancements in deployable medical equipment technology facilitate the effective delivery of comprehensive care in austere environments. Additionally, rapid patient evacuation systems have led to decreased morbidity and improved outcomes,” Bagby emphasizes. “Lessons learned in deployment are brought back to the Army dental community and shared through officer professional development and residency training programs.”
Traumatic injuries would also include loss of limb, notes Dossett. Three-dimensional cone-beam computed tomography (CBCT) and stereolithography are very useful tools in managing the significant head and neck trauma seen in war-type injuries, he adds.
Collaboration Among Dental Branches
Despite advancements in equipment, training, and technology, full-thickness facial burns and blast injuries consistently challenge both the limits of surgeons' skills and current reconstructive armamentarium. Colonel Robert Hale currently heads the US Army Dental and Trauma Research Detachment, a division of the US Army Institute of Surgical Research, explains Bagby. Dr. Hale and his team are pursuing militarily relevant research and solutions for the prevention, treatment and rehabilitation of craniofacial trauma and infectious dental diseases. Their current working projects in wound healing and soft tissue regeneration aim to improve outcomes in patients suffering from facial burns and blasts.
“Research at the Institute for Surgical Research (ISR) at Ft. Sam Houston, Texas, and the Dental Trauma Research Detachment (DTRD) under the direction of Col. Hale are investigating procedures in mandibular regeneration,” Dunn adds. “This novel procedure would be much less invasive than the current standard of care, with fewer surgeries to obtain a satisfactory result.”
“Our military services not only serve together at many bases, both information and ideas are shared in research and education symposiums,” notes Wagner. “There are numerous domestic and international Tri-Service Dental Symposia held annually that deal with the full range of restorative and surgical dental treatment. Many of these venues include Coast Guard, Public HealthVA dentists, and support staff as well.”
In fact, all branches of the military meet regularly at national meetings (Association of Military Surgeons of the United States) and the Tri-Service Dental Educator's Conference to discuss items of importance. Although each service has its own specific culture that makes it unique, they are starting to see a joint environment where they are blending members of all services.
“Most of the issues relate to recruiting and retention of our dentists, the implementation of the electronic dental record, and always the potential for improving dental readiness,” Dunn observes. “Particular attention is given to training our dentists in residency programs. The military feels that dental school was the first step and that additional training in military residency programs is a force multiplier.”
Conclusion
Military dentistry is no different from routine civilian dentistry. Military dentists all graduated from a civilian university, and most received additional training in one year Advanced Education in General Dentistry (AEGD) programs. All of the specialties are represented, and the military requires graduates of postgraduate specialty programs to challenge their respective Board examinations.
“The biggest difference is the emphasis on the readiness mission. In other words, the most disqualifying conditions are treated first,” explains Dunn. “Often, in private practice, a patient will demand a cosmetic procedure before complete control of caries. The doctor–patient relationship is still a one-on-one personalized encounter.”
According to Borris, military dentists, by and large, have more experience doing a much wider assortment of procedures than their classmates from dental school at the same point in their careers. Under very adverse circumstances, they are called upon to make many decisions in a short period of time that have significant ramifications.
“They bring a lot when they leave the military and go into private practice, and if there was the opportunity to employ one, that would be a decision I would make very quickly,” Borris says. “They would be good additions to any practices looking for associates, and they're very strong members of the community.”
Author's Note:
As we went to press, my son-in-law, Army SPC. Brian K. Teal from B Company, 3BSTB, 3rd Brigade Combat Team, 10th Mountain Division (LI), stationed at Fort Drum, New York, was deployed to FOB PASAB in Afghanistan for his second tour. This article is dedicated to him and all the brave men and women who serve in the Armed Forces, with wishes and prayers for their safe return home and much gratitude for preserving liberty and freedom throughout the world.