Interocclusal Registration
More than just a bite, it is a critical piece of diagnostic information.
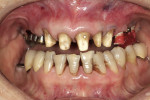
Dr. Ken Rudd1 said it best, “Most laboratory technicians experience little difficulty in making a restoration that will fit the master cast. Fitting the restoration to the patient’s mouth can become a problem for the dentist.” Successful rehabilitation dentistry is a composite of many accurate steps coming together in synergy. An often-overlooked and yet critical piece to a successful rehabilitation is the interocclusal registration. Capturing the tooth-to-tooth and arch-to arch relationship accurately is extremely demanding. Small errors will lead to significant intraoral adjustments. When implants are involved, the difficulty is magnified. It is the purpose of this article to provide a guideline for predictable interocclusal registrations including complex implant restorations.
Six Keys to an Accurate Registration and Articulation
Material
Most dentists use polyvinyl siloxane (PVS) bite registration material. It is easy to dispense and trim. PVS is highly accurate and it is available in a variety of rigidities. Personal preference and historical success rather than science may dictate the choice of material. Many prefer a very rigid material (eg, Regisil® PB™, DENTSPLY International, https://www.dentsply.com; Futar®, Kettenbach, https://www.kettenbachusa.com) for the security of seating. Other technicians will prefer a more elastic PVS for its ease of trimming (President Jet Bite, Coltène Whaledent, https://www.coltene.com). The PVS material is not as important as the technique.
Wax registrations can produce accurate mountings. However, the risk of distortion during removal, trimming, and transfer limit its use. Polyether registration material (Ramitec™, 3M ESPE, www3mespe.com) is available but provides a difficult delivery system and limited choice of rigidity.
Dry Field
PVS bite registration suffers from the same hydrophilicity issues as PVS impression material. As with a final impression, the entire field must be dried and isolated to maintain the dryness. If not, the material will not capture detail. This lack of detail may lead to a lack of support for the cast and a poor mounting.
Delivery
Always introduce material onto the maxillary arch. By injecting on the maxillary arch, the maxillary lingual cusps will be captured completely. This allows the laboratory to more easily mount the casts. Without complete tooth coverage, the casts tend to rock on the registration and may become altered in position.
Trimmed
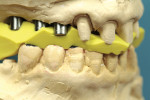
The bite registration must be properly trimmed or the casts will not seat correctly. The transverse, sagittal, and/ or vertical change will be transferred to the mounting and, ultimately, the final restoration. The excess material must be removed to verify seating on the casts. The PVS captures pit-andfissure detail that will not be produced on the cast. The anatomy should be trimmed leaving only the depths of the cusp tips (Figure 1). If a bite registration is untrimmed, the odds are very low that the cast was mounted correctly.
Sequence
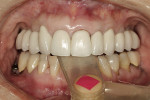
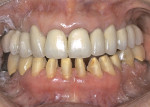
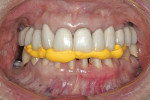
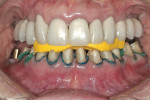
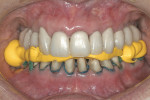
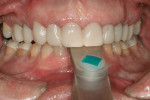
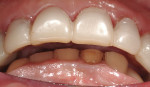
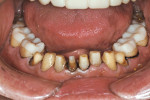
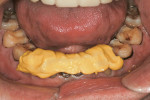
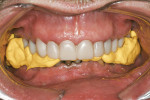
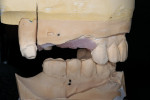
Practitioners must have a strategy for capturing the correct interocclusal registration before preparing teeth. If all of the teeth are prepared before thinking about the bite registration, a dentist may be faced with attempting to locate and record a vertical dimension and centric position free hand. This is less than predictable and will routinely begin a cycle of frustration with the laboratory. Leaving teeth unprepared or producing accurately adjusted provisionals will assist in transferring the correct position. An effective strategy in registering a quadrant is to leave the second molar unprepared when working at the same vertical dimension (Figure 2, Figure 3, Figure 4, Figure 5, Figure 6) or provisionalize the molar at an altered vertical dimension (Figure 7, Figure 8, Figure 9, Figure 10, Figure 11). Make the interocclusal record and then complete the preparation. The second molar may be added into the bite registration secondarily. It should be noted that interocclusal registrations are always made against prepared teeth and never over the provisionals.
Force
When the most posterior stops are prepared, dentists must be careful to avoid heavy bite forces during the bite registration. Removing contact on a single second molar can cause a significant cranial condylar movement of the ipsilateral condyle.2 Therefore, excessive force on a shortened arch can over-seat the condyle, artificially shortening the interocclusal space. Patients should be asked to bite “half-hard” into the interocclusal record. Because of the asymmetry of the biting pressure, the most difficult case is a unilateral prepared arch. Patients numb on the prepared side tend to over-compensate for the lack of contact by over-closing.
Implant Interocclusal Registration
It is hard enough to think through a complex rehabilitation without adding the tedium of implant prosthetics. So many of the procedures are unique to implants and the dentist’s system of choice. Open- vs closed-tray impressions, prefabricated vs custom abutment, regular emergence or platform switch are but a few of the restorative decisions that must be made. The interocclusal registration can become an afterthought. Many times using dentate techniques on an implant bite registration will transfer interocclusal dimensions inaccurately, leading to excessive adjustment and remakes.
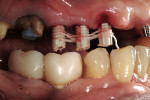
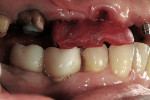
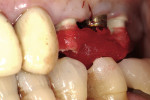
Final implant abutments may serve as platforms for the best registration. If final abutments are not placed at the time of the bite registration, technique modifications must be made to create an accurate bite registration. This is especially true in unilateral and/or bilateral distal extensions and completely implant-supported restorations. Even with final abutments placed, the contour of the occlusal platform of the abutment can make mounting unpredictable. Tapered final abutments may not provide a sufficient platform for mounting, especially if there is a hole in the occlusal surface. Simply injecting bite registration material over soft tissue, or soft tissue and underexposed healing heads, is not acceptable. A bite registration does not accurately capture soft-tissue detail. The tissue compression during the final impression will not be mimicked in the interocclusal registration (Figure 12 and Figure 13). The impact of such an error can be catastrophic.
There are two techniques recommended to capture the interocclusal position for implant rehabilitation cases: the interocclusal jig and a healing head registration.
Technique 1— Interocclusal Jig
Originally described in the literature by Parel,3 the interocclusal jig technique calls for fabrication of an implant-supported platform on which a bite registration may be fabricated. Parel3described an extraoral laboratory technique where the jig is fabricated on a duplicate cast. The expense and time is much too high for the majority of practitioners. A simpler and more cost-effective technique is to fabricate the jig intraorally. Non-engaging provisional abutments are reduced to clear in occlusion. They are linked together with floss to produce a latticework for the addition of acrylic (Figure 14). The acrylic should be added to both ends and allowed to polymerize, leaving a small gap between the sections. After curing, the ends may be joined by a small amount of acrylic. The fit of the jig will be altered if the sections are joined in mass due to the 6% to 10% polymerization shrinkage of dental acrylics.4After joining the sections, additional acrylic is added to produce an occlusion platform (Figure 15). Care must be taken to prevent acrylic from flowing into the screw access. This platform is designed to hold centric position and vertical dimension. The occlusal registration may be relined with a wash of PVS during the final registration to improve accuracy of mounting. The interocclusal jig is most advantageous for registrations of large edentulous implant segments. It allows a positive seat for the patient to bite and, thus, provides greater repeatability (Figure 16 and Figure 17). In addition, the interocclusal jig can act as a verification jig to ensure that the impression of the implant platforms is accurate.
Technique 2—Healing Head Registration
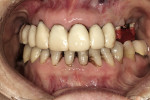
Tall healing heads may be used to register centric relation more predictably than tapered abutments or tissue-level healing heads. The abutments must completely clear the tissue but not be in occlusion (Figure 18). The exact healing abutments used for the final bite must be transferred to the laboratory. This means that the practitioner is required to have two sets of healing abutments. As a member of the implant team, the surgeon placing the healing abutments can be asked to provide duplicate healing abutments for this procedure. In the laboratory, the technician will place the abutments on the working cast analogs and trim the registration for mounting. The abutment heights for each implant must be noted so that the laboratory replaces them in the proper analog. Because the healing heads have a larger surface area and are above the tissue, mounting is more accurate (Figure 19 and Figure 20).
Conclusion
Prosthodontics is a study in minimizing error so that the restoration fits more than just the cast. While every step in dentistry is fraught with error, the successful practitioner works to efficiently manage the items within their control. A properly constructed interocclusal record is one item that may be controlled. Proper planning of the centric position and vertical dimension as well as careful handling of the material will reduce remakes, adjustments, and frustrations. While the six keys to success apply to implants, implants add a unique element to the bite registration. These cases require further planning and materials. Two options were presented to improve implant case articulation and reduce errors introduced by the dentist.
References
1. Rudd KD, Morrow RM, Strunk RR. J Prosthet Dent.1969;22:294-300.
2. Seedorf H, Seetzen F, Scholz A, et al. J Oral Rehabil. 2004:31:759-763.
3. Parel SM, Lewis S ed. The SmiLine System. Dallas, Texas: Taylor Publishing Co; 1991.
4. Mojon P, Oberholzer JP, Meyer JM, Belser UC. Polymerization shrinkage of index and pattern acrylic resins. J Prosthet Dent.1990: 64:684-688.
About the Author
Jeffrey S. Rouse, DDS, Private Practice, Prosthodontics, San Antonio, Texas