Esthetic Conservation: A Smile Makeover Does Not Always Have to Be Extreme
Leonard A. Hess
More and more patients are initiating the process of esthetic treatment. They are better informed about what can be accomplished through elective care. They understand how feeling better about themselves can improve their lives. But, at times, their exuberance can sometimes cloud our clinical judgment. Sound planning by the dentist must address functional and biological considerations, regardless of the patient’s readiness to proceed.
While patients are initiating treatment, this author has noted another trend. Patients are also becoming more concerned about the amount of tooth reduction necessary to achieve their goals. Dental care is being marketed to the general population more than ever before, and people want to believe they can get that care with no drill, no pain, and no needle. It may be difficult for a patient to understand why additional tooth reduction may be necessary to allow for proper function and biological needs, and how proper tooth reduction will allow better functional longevity for restorations and periodontal structures. It is the dentist’s role—and responsibility—to educate the patient.
When esthetic care is being planned, the patient deserves the most conservative approach possible that will still meet their goals. As the esthetic revolution presses onward, there seems to be a push back toward conservation of tooth structure. In certain instances, a conservative smile makeover can be a very challenging situation for the dentist and ceramist. To obtain a high-quality esthetic result, both need to have an intimate understanding of functional smile design. One must be able to recognize the deficits inhibiting the patient’s smile. Then the decision is made on whether an addition of restorative material or a subtraction of tooth structure is necessary to achieve the needed effect. They also must decide whether the changes will complement, improve, or detract from the patient’s occlusion and function.
LENGTH OF THE CENTRAL INCISORS
Diagnostic planning is crucial when determining the length of the incisors. These teeth will often be the starting point to establish the proportion, symmetry, and functional parameters of the remaining anterior teeth. Many factors will influence their final restored length. These include facial proportion, soft-tissue characteristics, envelope of function, upper lip characteristics, lip positions at rest, and the lower lip position during smiling.1
It is useful to evaluate the length of the central incisor at rest as it relates to the upper lip. Vig and Brundo2 determined that 3.4 mm of central incisor is visible in women at rest, and 1.91 mm is visible in men. Advancing age will also play a part by generally decreasing the amount of tooth shown.2 In a recent study of crown ratios, unworn central incisors average 11.69 mm in length, and worn centrals average 10.67 mm in length.3
INCISAL EDGE POSITION
Locating the correct position for the incisal edge is a crucial and often overlooked aspect of functional smile design. An error in this process can lead to broken restorations and disruption of the total occlusal scheme.
It is important that the incisal edge accommodates the patient’s anterior envelope of function. Errors in positioning can interfere with the lower teeth upon intercuspation, and catch the lower lip upon sealing the mouth. Such a “neutral zone” violation will disrupt the muscle and soft tissues of the peri-oral complex and create muscle fatigue and a “not quite right” sensation for the patient.4,5
In addition, the incisal edge position is important in relation to speech patterns. The edges must contact the wet inner vermillion border of the lower lip during pronunciation of the letters “F” and “V.” Contact on the dry cutaneous region of the lip would indicate an error to the buccal.6 The edge position must also allow the proper and effortless squeezing of air between the lower incisors and maxillary incisors that allow the “S” sound to be formed.7
This position is often determined during the diagnostic wax-up stage but it must be refined and tested by the provisional restorations. Problems encountered during the temporary phase of treatment, such as broken temporaries, are often related to an incorrect incisal edge position. Such occurrences should not be viewed as an irritation, but offer opportunities to correct positions before the final restorations.
COLOR
Communication in regard to color cannot be overlooked. First and foremost, know what the patient wants. No matter the quality of the restorative result, if the patient does not like the color, it is a failure.
Proper shading of the teeth may become a great challenge in conservative anterior cases. Many times restorations will be adjacent to natural teeth, and will need to blend in seamlessly. There are many digital shade-matching systems currently on the market to aid in color mapping. This is certainly an area where thorough digital photography is an asset to the technician. In the author’s opinion, monochromacity seems to be a common error in restoration fabrication. It becomes very visually distracting because of its unnatural appearance (Figure 1).
MIDLINE LOCATION
In a perfect world, everyone’s maxillary midline would coincide with the midline of the face. Unfortunately, most people are full of asymmetry. Examples would include offset noses, canted pupillary lines, and asymmetric facial bones. Many times even the patient’s maxillary and mandibular midlines will not coincide.
During restorative treatment, every effort should be made to allow midline harmonies. Midline deviations become more noticeable when they are greater than 2 mm from center.8 Always be sure that the midline is vertical or perpendicular to the floor.9 Canting of the midline can also become quite noticeable. A properly recorded facebow is of vital significance in achieving a proper midline orientation.
AXIAL INCLINATION
Axial inclination refers to the long axis of the clinical crown as determined by the tooth’s anatomy. This is derived by drawing a line and connecting a point at the gingival zenith with a point at the incisal edge height of contour. The central incisors would have a nearly vertical orientation. As you move distally in the mouth, the axial inclinations of the teeth would have a mesial bias. When the axial inclination of many teeth is less than ideal, the smile can be quite unesthetic (Figure 2 and Figure 3).
WIDTH-TO-LENGTH RATIO
An acceptable width-to-length ratio is 80%.10 Many times the goal may be to achieve the “golden proportion” for the maxillary anterior teeth. In such a situation, when viewed from the direct anterior, the lateral incisor would be assigned a value of 1.0, the central 1.6, and the canine 0.6, giving the appearance that the adjacent distal tooth is 40% narrower.11 Diastemas and narrow arch forms can make this a difficult restorative goal and may necessitate orthodontic involvement.
INCISAL EMBRASURE
Incisal embrasures are the negative space created by the incisal to axial/interproximal contour transitions of adjacent teeth. The embrasure between the two maxillary central incisors would be the shortest and narrowest. As you progress to the distal, the embrasures should become wider and taller. This is dictated by the changing anatomy of the more posterior teeth.
CONTACT POINTS
The contact points of adjacent teeth will correlate with the incisal embrasures. The maxillary central incisors will have the longest amount of contact inciso-gingivally. Progressing to the distal, the contacts will become shorter inciso-gingivally and wider bucco-lingually. Again, this is dictated by the changing anatomy of the teeth as progressed to the posterior.
GINGIVAL FORM
The attention given to the gingival form will often be dictated by the patient’s lip mobility during a smile. Some patients may smile their biggest and not show any gingiva; others may show excessive amounts. Lack of gingival health and symmetry can certainly decrease the esthetic nature of a smile.
The gingival plane should be parallel to the horizontal reference plane, and perpendicular to the midline position. Ideally, the gingival zenith positions would form a sinuous pattern with the central incisor and canine zenith positions slightly gingival to the lateral incisor position. An additional acceptable variation would have the zenith position of all three of these teeth the same height. Allowing the canine and lateral zenith heights to be more gingival than the central is unesthetic and should be avoided.12
CASE PRESENTATION ONE
This case is an excellent example of less is more. The patient was a 17-year-old girl with “peg” maxillary lateral incisors. They had been successfully restored with bonded composite for many years. The bonding was beginning to show its age as a result of pitting, stain, and internal discoloration. The patient was feeling very self-conscious about the dark appearance of her teeth. She and her mother wanted a long-term fix to the esthetic problem without overtreatment.
Using the framework that functional smile design provides, the following smile deficiencies were determined:
- Color discrepancies
- Asymmetric incisal embrasures
- Incorrect and absent contact points
- Axial inclination asymmetries for teeth Nos. 7 and 10
- Asymmetric incisal edge positions
- Length discrepancies of the central incisors
- Lateral incisor width-to-length ratios could be better
- Tooth No. 9 had a slight facial enamel defect in the gingival one third
The treatment plan included the following:
- Bleaching with Professional Crest® Whitestrips® (Procter & Gamble, Cinncinati, OH)
- Composite bonding tooth No. 9 with Point 4™ (Kerr Corporation, Orange, CA)
- Esthetic recontouring of teeth Nos. 8 and 9
- Stacked HeraCeram® (Heraeus Kulzer, Armonk, NY) porcelain veneers on teeth Nos. 7 and 10
Once the bonding was removed from teeth Nos. 7 and 10, almost no further reduction of tooth structure was required. The end result was a highly esthetic smile at minimal cost and maximum tooth conservation. Because the smile deficiencies were identified in the planning stages, getting a “wow” smile was very predictable (Figure 4, Figure 5, Figure 6, Figure 7, Figure 8, Figure 9).
CASE PRESENTATION TWO
The patient in this case had been frustrated with her smile for many years. However, every time she had previously expressed her wishes she was told her only option was orthodontics. Because of what she had seen in the media, the patient did not understand why some other solution could not be offered. When she presented to the author’s office for an opinion, orthodontics was presented as the most conservative option. To the patient this was not an option at all. At this point, consideration was given to conservative restorative options. Her smile deficiencies were identified as:
- Midline diastema
- Width difference between teeth Nos. 8 and 9
- Axial inclination in tooth No. 8
- Incisal embrasure and contact point issues as a result of the rotational and axial inclination of tooth No. 8
Because this tooth was not in the maxillary arch form, the question became one of whether or not it could be prepared without over-reduction. Before a final treatment plan was presented to the patient, a mock preparation and wax-up was created to measure the amount of reduction that would be necessary (Figure 11 and Figure 12). The actual preparation was then not stressful because the amount of reduction was not left to a best guess.
The patient’s treatment was:
- Mesial slimming of tooth No. 9 to allow the centrals to be the same width
- Esthetic recontouring of tooth No. 9 to allow a more pleasing width/length ratio of the maxillary incisors
- A stacked HeraCeram porcelain veneer on tooth No. 8. The restoration was designed with a lingual wing to re-establish a symmetric lingual anatomy. This brought tooth No. 8 back into an idealized maxillary arch form without additional reduction necessitated by a full-coverage crown
The end result was a dramatic smile change by only restoring one tooth. The patient no longer felt self-conscious about her smile (Figure 10, Figure 11, Figure 12, Figure 13, Figure 14, Figure 15, Figure 16, Figure 17).
CONCLUSION
To become proficient in esthetic treatment, it is important to prepare for success. A mastery of functional smile design is needed not only for the dentist but also the ceramist. Careful planning and open communication can lead to conservative yet dramatic smile makeovers that fulfill both a dentist’s treatment plan and the patient’s wishes.
ACKNOWLEDGMENT
The author would like to thank Dental Arts Signature Lab (Peoria, IL) for the artistic restorations in this article.
REFERENCES
1. Hess L. Interdisciplinary synergy: managing complex treatment objectives for a predictable esthetic result. Advanced Esthetics and Interdisciplinary Dentistry. 2006;2(2):10-18.
2. Vig RG, Brundo GC. The kinetics of anterior tooth display. J Prosthet Dent. 1978;39(5):502-504.
3. Mange P, Gallucci GO, Belser UC. Anatomic crown width/length ratios of unworn and worn maxillary teeth in white subjects. J Prosthet Dent. 2003;89(5): 453-461.
4. Cranham J. The horizontal position of the maxillary incisal edge: the key to optimum esthetics, phonetics, and function. Contemporary Esthetics and Restorative Practice. 2006;10(2):22-24.
5. Dawson P. Evaluation, Diagnosis, and Treatment of Occlusal Problems. 2nd ed. St. Louis, Mo: Mosby; 1988:330.
6. Chiche, GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Hanover Park, IL: Quintessence Pub. Co; 1994:21.
7. Dawson P. Functional Occlusion: From TMJ to Smile Design. St. Louis, Mo: Mosby;2006:181.
8. Beyer JW, Lindauer SJ. Evaluation of dental midline position. Semin Orthod. 1998;4(3):146-152.
9. Thomas JL, Hayes C, Zawaideh S. The effect of axial midline angulation on dental esthetics. Angle Ortho. 2003;73(4):359-364.
10. Chiche GJ, Pinault A. The Esthetics of Anterior Fixed Prothodontics. Hanover Park, IL: Quintessence Pub. Co; 1994:23.
11. Ascheim KW, Dale BG. Esthetic Dentistry: A Clinical Approach to Technique and Materials. 2nd ed. St. Louis, Mo: Mosby; 2001:31.
12. Carranza F, Takei H, Newman M. Clinical Periodontology. 9th ed. Philadelphia, Pa: Saunders; 2001:943-948.
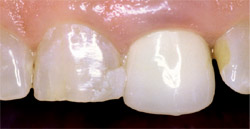 | |||||||
| Figure 1 Much could be said with regard to the esthetic nature of these teeth. However, the most striking feature is the unnatural appearance caused by the monochromatic nature of the crown. | |||||||
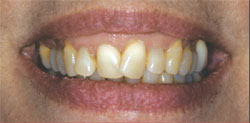 | 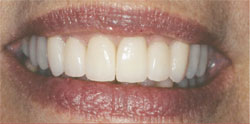 | ||||||
| Figure 2 and Figure 3 This case illustrates the dramatic contribution proper axial inclination can make in a smile. | |||||||
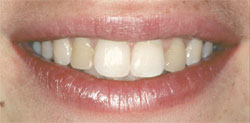 | 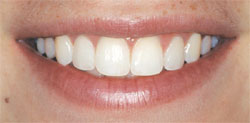 | ||||||
| Figure 4 and Figure 5 The full smile before and after photos for Case Presentation One. | |||||||
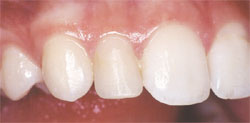 Figure 6 | 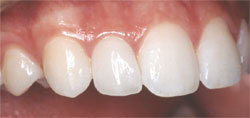 Figure 7 | ||||||
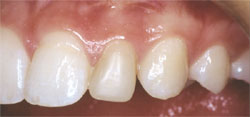 Figure 8 | 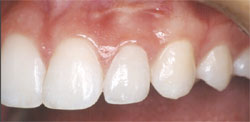 Figure 9 | ||||||
| Figure 6 through Figure 9 The final restorations. Note how the matching surface texture and marginal gingival health allows a seamless integration of the veneers. Incisal embrasures, axial inclination, contact points, length, color, and incisal edge anatomy have all been improved. | |||||||
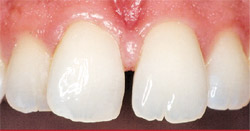 | 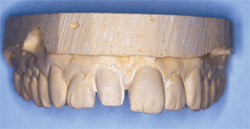 | ||||||
| Figure 10 The preoperative condition of Case Presentation Two. Incorrect rotation and axial inclination of tooth No. 8 has degraded the esthetic nature of the smile. | Figure 11 Because of the uncertain nature of this case, a trial preparation was performed on a model. This allowed a measure of the necessary tooth reduction. | ||||||
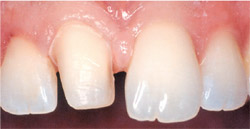 | |||||||
| Figure 12 The final preparation of tooth No. 8. Notice how close the actual preparation was to the prepared model. The preparation remained almost entirely in enamel. | |||||||
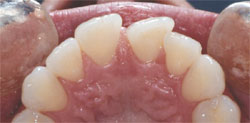 Figure 13 | 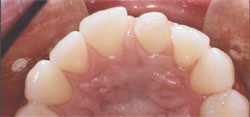 Figure 14 | ||||||
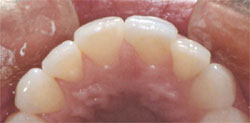 Figure 15 | |||||||
| Figure 13 through Figure 15 The occlusal views preoperatively, at preparation, and at final restoration. Tooth No. 8 was reduced in the necessary areas and a porcelain wing was added to the lingual. The tooth is now in the proper arch form facially and lingually. | |||||||
 |  | ||||||
| Figure 16 and 17 Notice the profound difference in the smile by only restoring one tooth. Restoring proper symmetry has removed the resulting visual distraction, and the patient is free to smile with confidence. | |||||||
| |||||||




