Managing Esthetic Challenges with Anterior Implants. Part 1: Midfacial Recession Defects from Etiology to Resolution
Abstract
Dilemmas accompanying esthetic zone implants frequently involve a dehiscence type defect of the midfacial tissues. The challenge to the surgical-restorative implant team is to understand the etiology associated with such defects and the treatment options that can be offered lending to predictable outcomes. Etiologic factors are: 1) poor implant spatial positioning; 2) incorrect abutment contour; 3) excessive implant diameter; 4) horizontal biologic width formation; and 5) periodontal phenotype. Remediation treatment can involve: 1) burying the implant and allowing the soft tissues to heal naturally over the implant with a surgical cover screw known as “implant decoronation;” 2) augmentation of the soft tissues with a connective tissue graft, if needed; 3) stage 2 uncovering of the implant: and 4) controlling the abutment-crown contour appropriately with flat or even undercontour to maintain the soft tissues in a stable and healthy position long term.
Many factors must be considered when managing esthetic challenges associated with anterior implants in order to determine what procedure is best. Two challenges exist for practitioners on a daily basis: 1) remediation of existing esthetic deformities with esthetic zone implants, and 2) being more proactive in treating patients so that esthetic problems are avoided.
Currently, one of the most significant issues in dentistry is poor implant positioning in the esthetic zone, specifically, excessive facial angulation. Although prosthetic solutions can sometimes successfully “mask” a negative condition using strategies such as gingival shaded ceramics, the primary goal should be reconstitution of both the hard and soft tissues where indicated. Surgeons should know when and how to repair such a condition in addition to taking proactive steps to avoid future problems.
The three primary challenges that restorative dentists and surgical colleagues frequently encounter are midfacial recession, interdental recession, and combination defects of the aforementioned conditions. This article will focus specifically upon the etiology and treatment of midfacial recession defects.
Midfacial Recession
Midfacial recession involves exposure of the roots of teeth caused by loss of periodontal attachment (bone, cementum, and connective tissues) and/or retraction of the gingival margin from the tooth crown(s) whether natural or artificial.1 When dealing with the natural dentition, the amount of midfacial coverage of the exposed root is always dictated and defined by the height of the interproximal tissues, ie, the interdental papillae. There are several predictable surgical procedures to accomplish this goal,2,3 with the understanding that the graft will be adherent to the root being a vital biologic structure. With dental implants, the clinical scenario is significantly different with the implant and/or abutment surface being a non-vital structure absent of blood supply, possibly non-receptive for a coronal tissue flap or free connective tissue graft. The surface may also be embedded and contaminated with bacterial endotoxins, which would prevent tissue healing.
Etiology
With the natural dentition, it is not uncommon to see midfacial soft tissue recession of patients with 1) a thin periodontal phenotype, and 2) areas of root prominence. The same can be said of implants. In an article by Chen et al on implant placement,4,5 the primary reason that recession was encountered was poor implant positioning, specifically, excessive labial placement. An additional factor was having implants that were oversized or of greater diameter.6 This is not uncommon especially in post-extraction socket implant placement where larger diameter implants are needed to achieve proper primary stability. The practitioner must also be careful using a tissue-level implant when a bone-level implant is indicated in order to ensure there is adequate space and flexibility for restoration.
Excessive facial contour of a custom fabricated screw-retained abutment in combination with a cement-retained crown is another cause for midfacial recession. It is common that excessive abutment contour co-exists with excessive facial implant placement, by default. Poor implant positioning creates tremendous contour problems for the restorative dentist and ultimately the definitive prosthesis, whether a custom-abutment or one-piece restoration design is fabricated. In fact, excessive facial implant placement requires flat abutment contour or even undercontour.
Biologic width, both vertical and horizontal along the implant, should also be noted and understood because it can negatively impact the definitive esthetic outcome of treatment. The horizontal component of biologic width has an equal influence on the outcome, as excessive facial placement will lead to the loss of facial bone and soft tissue.7 For non-platform–switched implant systems, there is a horizontal component of biologic width, roughly 1.5 mm in distance. Consequently, if an implant is placed too close to the facial plate of bone, the horizontal component of biologic width will cause the facial bone plate to resorb, and a hard and soft-tissue dehiscence defect can be the resultant effect.
Lastly, it is well known that the periodontal phenotype of the patient plays a significant role in the potential for or resistance to gingival recession. A thin phenotype is more prone to recession; conversely, a thick phenotype is more resistant to recession.8-11
Remedial Treatment
When treating midfacial recession associated with an anterior dental implant, one must consider the angulation and facial position of the implant within the dental arch. Proper spatial implant positioning makes restoration easier and potentially allows screw-retention, thereby eliminating cementation and the associated potential peri-implantitis dilemmas.
Remedial treatment is required when an anterior implant is poorly placed with a concomitant gingival dehiscence defect. These authors find that midfacial recession associated with excessive facial implant angulation associated with a healthy implant (ie, no bone loss) is more predictably treated versus implant positioning approximating or outside the confines of the labial bone plate. The latter clinical condition usually requires implant removal with ridge reconstruction. Diagnosis of such clinical conditions is predictable with current cone beam computed tomography.
Clinical Example of Excessive Implant Angulation
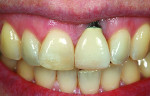
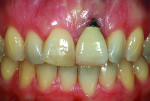
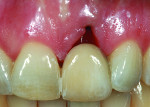
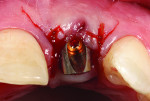
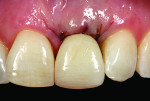
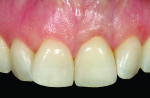
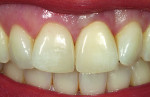
A young woman presented with a midfacial recession defect of roughly 4 mm to the junction of the abutment-implant interface (Figure 1) that was also present in her smile (Figure 2). She had previously consulted several surgeons who were hesitant to treat her because of the defect and high smile line. A cosmetic dentist subsequently referred her to the authors.
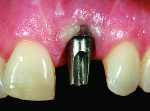
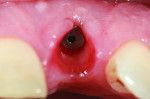
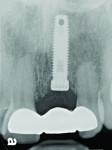
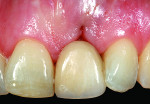
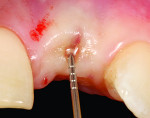
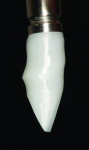
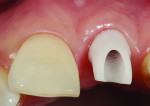
Before a clinician can decide on treatment, a diagnosis must be made whether the implant is healthy or not, meaning normal bone levels around the implant. Another decision of concern was whether to retain the dental implant. It was determined that the implant was healthy, however the recession defect was due to an overcontoured custom abutment secondary to excessive facial implant angulation (Figure 3). The tendency for most surgeons when presented with such a recession defect is to think of a “root” coverage type surgical procedure. Patients with a thin or intermediate phenotype may not respond well to such a technique. It was also mentioned previously that an exposed implant abutment is absent of blood supply and may be contaminated with endotoxins that would constrain the predictability of healing with a coronal positioned connective tissue flap. One of the tactics to predictably ensure primary flap closure of the defect is to “decoronate” or bury the implant12,13 by removing the existing implant abutment and placing a surgical cover screw (Figure 4). Consequently, the soft tissues will heal and cover the head of the implant—“nature’s connective tissue graft” or spontaneous in-situ gingival augmentation. A resin-bonded–retained bridge was used as a provisional transitional restoration (Figure 5 and Figure 6). After a 2-week period, closure of the tissue was evident but de-epithelialization was required to ensure completion (Figure 7). Three-months post-ridge healing, sounding to the implant head with a periodontal probe revealed 5 mm of coronal soft tissue thickness (Figure 8). It was then decided that a secondary ridge augmentation procedure was not necessary, only second-stage implant uncovering surgery was needed with a crestal incision biased toward the palate. The shape of the patient’s pre-existing abutment was modified creating a flat facial contour, disinfected, and replaced as a provisional abutment (Figure 9). The original crown was also used as a temporary following an acrylic reline (Figure 10). After 1-month post-implant exposure, a new acrylic provisional restoration was fabricated and used to re-shape and sculpt the soft tissues to match those of the contralateral natural tooth14 (Figure 11). The flat contour concept of the abutment restoration is followed throughout the definitive abutment (Figure 12) and crown restoration (Figure 13 and Figure 14). Figures 15 and 16 show the intraoral and smile view of this patient, respectively, receiving remedial treatment at 5-years post-surgical treatment.
In summary, when managing midfacial soft tissue recession defects, the primary steps of treatment include: 1) implant decoronation; 2) soft-tissue augmentation, if required; 3) stage 2 implant uncovering; and 4) managing the abutment contours with flat or undercontoured subgingival profiles.
Proactive Treatment
Proactive treatment requires prior understanding of the potential etiology for midfacial recession defects, and subsequently avoiding them. Placing an implant more to the palatal aspect of an edentulous ridge or post-extraction socket can circumvent the potential of midfacial recession. The only risk with such placement is fenestration of the ridge or socket at the apical area due to the anatomy of the anterior maxilla.
Restorative platform-switching can also serve as one method and treatment strategy to potentially evade midfacial recession. The reason for this effect is that platform-switched implants have half (0.6 mm to 0.7 mm) the horizontal effect of biologic width15-17 because the restorative platform interface is moved inward or medial toward the restorative connection. Therefore, a platform-switched implant inadvertently placed too far to the facial aspect of a ridge or post-extraction socket may not cause a dehiscence defect since the horizontal influence of biologic width is only half that of a non-platform–switched implant.
Immediate Placement of Implants into Anterior Post-Extraction Sockets
The authors emphasize that surgeons should be familiar with a classification of different socket types18 in order to prevent midfacial recession with immediate implant placement. This classification was created to identify potential esthetic risks associated with post-extraction socket implants in the esthetic zone. There are three types of sockets. In type 1 sockets, the facial soft tissue and bone are both present. In type 2 sockets, the tissue may appear normal and may look like a type 1 socket from the outside, but part of the buccal plate is absent. This is the most deceptive type of socket to treat as it can fool the surgeon into believing that the socket is intact because the soft tissue level appears normal. In type 3 sockets, the soft tissues and the buccal plate of bone are both noticeably reduced because midfacial recession and attachment loss is already present. Type 3 sockets should not be difficult to identify, and the surgeon should not attempt an immediate placement. The primary goal in treatment of type 1 sockets is to preserve the buccal plate.
For type 1 sockets, the authors recommend performing an immediate implant placement in the esthetic zone. This should not be performed in types 2 and 3 sockets as midfacial recession is a risk factor in such case types. For types 2 and 3 sockets, it is recommended that the surgeon reconstruct the labial plate at a later date using a delayed protocol.
There are a few primary points to consider when placing implants into anterior post-extraction sockets; the major one being atraumatic tooth removal without flap elevation. This is because there are three sources of blood supply to the buccal plate. The periodontal ligament will be gone after the tooth is removed. The second source of blood supply is the periosteum. An issue with the periosteum is if there is flap elevation, there is a risk of impacting the blood supply. The third source of blood supply is the marrow, which is minimal-to-none in the labial bone plate of anterior extraction sockets, which are usually less than 1 mm in thickness.19
Conclusion
When managing esthetic challenges on anterior implants, many factors must be considered prior to treatment. One of the primary challenges facing restorative dentists and surgeons alike is midfacial recession. Using prior experience and evidence-based studies, these authors have reviewed their preferred methods for treating this condition. In addition, the authors emphasize the importance of being proactive during treatment periods in order to prevent later problems that patients might encounter. By employing these methods, patient issues can be resolved more quickly and have lasting impact.
REFERENCES
1. For the dental patient. Gingival recession: causes and treatment. J Am Dent Assoc. 2007;138(10):1404.
2. Miller PD Jr. Root coverage with the free gingival graft. Factors associated with incomplete coverage. J Periodontol. 1987;58(10):674-681.
3. Zadeh HH. Minimally invasive treatment of maxillary anterior gingival recession defects by vestibular incision subperiosteal tunnel access and platelet-derived growth factor BB. Int J Periodontics Restorative Dent. 2011;31(6):653-660.
4. Chen ST, Darby IB, Reynolds EC. A prospective clinical study of non-submerged immediate implants: clinical outcomes and esthetic results. Clin Oral Implants Res. 2007;18(5):552–562.
5. Caneva M, Salata LA, de Souza SS, et al. Influence of implant positioning in extraction sockets on osseointegration: histomorphometric analyses in dogs. Clin Oral Implants Res. 2010;21(1):43-49.
6. Caneva M, Salata LA, de Souza SS, et al. Hard tissue formation adjacent to implants of various size and configuration immediately placed into extraction sockets: an experimental study in dogs. Clin Oral Implants Res. 2010;21(9):885-890.
7. Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol. 2000;71(4):546-549.
8. Olsson M, Lindhe J. Periodontal characteristics in individuals with varying form of the upper central incisors. J Clin Periodontol. 1991;18(1):78-82.
9. Kan JY, Rungcharassaeng K, Umezu K, Kois JC. Dimensions of peri-implant mucosa: an evaluation of maxillary anterior single implants in humans. J Periodontol. 2003;74(4):557-562.
10. Linkevicius T, Apse P, Grybauskas S, Puisys A. The influence of soft tissue thickness on crestal bone changes around implants: a 1-year prospective controlled clinical trial. Int J Oral Maxillofac Implants. 2009;24(4):712-719.
11. Linkevicius T, Apse P, Grybauskas S, Puisys A. Reaction of crestal bone around implants depending on mucosal tissue thickness. A 1-year prospective clinical study. Stomatologija. 2009;11(3):83-91.
12. Langer B. Spontaneous in situ gingival augmentation. Int J Periodontics Restorative Dent. 1994;14(6):524-535.
13. Salama, M, Ishikawa T, Salama H, et al. Advantages of the root submergence technique for pontic site development in esthetic implant therapy. Int J Periodontics Restorative Dent. 2007;27(6):521–527.
14. Zamzok J. Avoiding ridge laps through nonsurgical soft tissue sculpting on implant restorations. J Esthet Dent. 1996;8(5):222-228.
15. Lazzara RJ, Porter SS. Platform switching: a new concept in implant dentistry for controlling postrestorative crestal bone levels. Int J Periodontics Restorative Dent. 2006;26(1):9-17.
16. Vela X, Méndez V, Rodríguez X, et al. Crestal bone changes on platform-switched implants and adjacent teeth when the tooth-implant distance is less than 1.5 mm. Int J Periodontics Restorative Dent. 2012;32(2):149-155.
17. Cocchetto R, Resch I, Castagna M, et al. The abutment duplication technique: a novel protocol for cementable implant-supported restorations. Int J Periodontics Restorative Dent. 2010;30(4):415-424.
18. Elian N, Cho SC, Froum S, et al. A simplified socket classification and repair technique. Pract Proced Aesthet Dent. 2007;19(2):99-104.
19. Huynh-Ba G, Pjetursson BE, Sanz M, et al. Analysis of the socket bone wall dimensions in the upper maxilla in relation to immediate implant placement. Clin Oral Implants Res. 2010;21(1):37-42.
Editor's Note: Parts 2 and 3 are expected to be published in Compendium in 2014.
About the Authors
Stephen J. Chu, DMD, MSD, CDT
Clinical Associate Professor, Director of Esthetic Education, Columbia University College of Dental Medicine, New York, New York
Dennis P. Tarnow, DDS
Clinical Professor, Director of Implant Education, Columbia University College of Dental Medicine, New York, New York