A Complete Ceramic for Chairside CAD/CAM Restorations
NOTE: Since this article was published, 3M has removed the crown indication for Lava™ Ultimate CAD/CAM Restorative. The product continues to be indicated for inlays, onlays (with an internal retentive design element), and veneer restoratives, per new instructions for use.
Manufacturers work diligently to provide all-ceramic materials suitable for CAD/CAM fabrication techniques. Although these materials have advantages, incongruent characteristics have led to distinct variations among physical properties, consequently designating particular materials as more ideal for specific indications. CAD/CAM machining parameters and procedures are crucial factors affecting the clinical success of resulting restorations. Equally important is material choice.
The success of all-ceramic restorations, especially in the posterior, is limited by the likelihood of near-surface damage, functional occlusal fatigue, stress areas within the supporting tooth structure or the chosen adhesive material, and post-fabrication adjustments. The high fracture rate of ceramic materials results from their inherently brittle nature and low tensile strength.1 A dditional challenges associated with previous CAD/CAM all-ceramic materials have included adaptation and marginal fit, fracture resistance, durability, esthetics, and longevity. Any damage reduces restoration strength, increasing the probability of catastrophic failure. When using all-ceramic materials, clinicians must manage various limitations.
A new resin nano-ceramic material (Lava™ Ultimate Restorative, 3M ESPE, www.3mespe.com) eliminates many of the disadvantages associated with conventional all-ceramic materials. Consisting of 80% ceramic and 20% composite resin with nano-technology, the resin nano-ceramic is neither a resin, a composite, nor a pure ceramic, but a combination of all three, demonstrating a non-brittle and fracture-resistant nature.2,3 The material is indicated for chairside or laboratory CAD/CAM fabrication of full-coverage crowns, crowns over implants, inlays, onlays, and veneers.2,3
Because of an elastic modulus similar to dentin, masticatory forces are absorbed, decreasing restorative stress. The resin nano-ceramic demonstrates exceptional resiliency from a flexural strength of more than 200 MPa. The combination of resin and nano-technologies processed via a specialized high-heat–controlled, proprietary manufacturing process generates a more wear-resistant material than resin, yet with the same optical properties, polish retention, and lasting esthetics of a glass ceramic.2,3
Available in eight shades (A-LT to D2-LT, and a bleach shade) and high and low translucencies (HT and LT), Lava Ultimate Restorative enables efficient creations of easy, predictable, and esthetic restorations for a variety of natural tooth shades.
Presentation and Treatment Plan
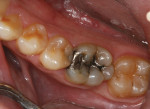
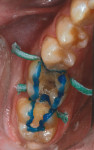
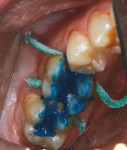
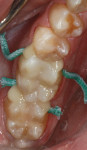
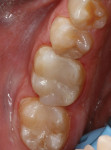
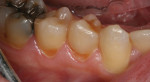
A 36-year-old man presented with interproximal decay on tooth No. 31 and a large failing amalgam restoration on tooth No. 30, with interproximal decay on the mesial (Figure 1). He also had abfractions/erosion lesions on teeth Nos. 28 and 29 that required gingival/cervical restorations (Figure 2). On closer evaluation and excavation, inlays were planned for teeth Nos. 30 and 31. These would be fabricated in-office using CAD/CAM and Lava Ultimate Restorative.
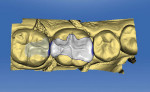
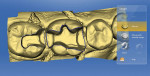
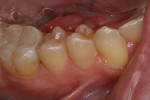
An opaquing spray was applied to teeth Nos. 28 through 31, and preoperative impression scans were taken using CEREC to digitally design the restorations (Figure 3). The spray was cleaned from the teeth, and they were prepared using a 557 carbide bur to remove the amalgam restoration. A series of coarse and fine tapered diamonds created a smoother preparation and appropriately flared walls. To ensure removal of all decay, a caries detection agent was used. Once the decay was excavated, there was no need to remove cusps, which allowed the restoration/preparation to remain in the occlusal table. Remaining enamel and dentin surrounded the preparation buccally and lingually, simplifying shade selection for the new resin nano-ceramic material.
Shade
A VITA shade guide was used to determine the general color, and a high-translucency block was chosen for its blending capacity. The high-translucency block blends into existing dentition, so margins are imperceptible. If deviating by one shade is necessary, a slightly lighter shade should be chosen to provide an effectively esthetic restoration. Available in monochromatic low- and high-translucency blocks, the resin nano-ceramic low-translucency blocks are ideal for masking the perimeter for full-crown restorations. High-translucency blocks can be used for intercoronal restorations (ie, inlays or one-cusp onlays) based on their chameleon effect. This author uses low-translucency blocks for full-coverage and high-translucency blocks for partial-coverage restorations.
Impressions and Design
When fabricating chairside CEREC restorations, impressions are taken with the CEREC AC camera. In the author’s practice, restorations are generally designed in two ways. The Biogeneric Individual process scans adjacent teeth morphology, analyzing cusp tips and fissure heights and depths to re-create the overall morphology for the restoration. The Biogeneric Copy mode uses existing tooth morphology to re-create the restoration.
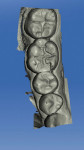
In this case, the teeth were sound and functional, and the anatomy did not require alterations. The patient’s preoperative condition was excellent, with flawless anatomy on tooth No. 31 and a satisfactory amalgam restoration on tooth No. 30. If the teeth were in poor condition, the Biogeneric Individual process would have been used, and the computer would have created new functional and esthetic restorations. As there was no need to change this patient’s tooth morphology, images were taken before preparation and the CEREC technology was used to duplicate anatomical landmarks, which would ultimately provide the patient with a restoration equivalent to his original teeth. Opaquing spray was applied to the preparations, and impression scans were taken (Figure 4) to guide restoration design, resulting in restorations remarkably comparable to the patient’s preexisting natural dentition (Figure 5).
Material Choice and Fabrication
Lava Ultimate Restorative mills exceptionally well. Marginal integrity is excellent because of the resin matrix, and its chairside handling characteristics are exceptional compared to other ceramics available today. An advantage when dealing with a resin matrix or a resin hybrid material is the ease and capability of a composite repair should the necessity arise. Replacing direct composite posterior restorations with the new resin nano-ceramic technique provides an accurate and easy way to provide interproximal restorations that look and fit exceptionally well, straight from the milling unit, and even more so once they are polished.
In this case, during the milling process the gingival/cervical direct composite restorations for teeth Nos. 28 and 29 were placed to maximize efficiency and minimizing time. After milling, there was no need to fire the restorations, which can save time when doing multiple-unit, partial-coverage restorations.
Finishing and Polishing
The sprues were polished back, creating a smooth surface, and the inlays were tried in. The CEREC Virtual Fit Checker can highlight areas that may be binding. In this case, under 4.5x magnification, a battery-operated overhead light confirmed that the restorations were seated properly. An explorer was used to verify that the margins were intact, and there were no open gaps interproximally or occlusally.
A challenge with interproximal resin restorations is creating consistent, controllable contacts. If the fit is tight, the teeth are usually adjusted interproximally and extraorally by polishing them back using a polishing bur. The ability to perform these adjustments chairside and extraorally is a major advantage. The need to use sectional matrix bands back-to-back for restorations such as those for teeth Nos. 30 and 31 is eliminated, along with the stress of creating precise contacts. Once the restorations were seated and the interproximal and occlusal margins were correct, the restorations were steam cleaned to remove debris or oils from the milling chamber, then polished.
Bonding and Cementation
The preparations were isolated before seating to prevent moisture contamination. The polished restorations were placed back in the mouth to confirm proper contacts. The dental assistant roughened the intaglio surface of the restorations via air abrasion with 27-µm aluminum-oxide powder at 30 psi. The powder was rinsed using an air/water stream and dried.
A silane-like coupling agent was placed on the internal of the restorations and dried. Using a microbrush, a universal bonding material (Scotchbond™ Universal Adhesive, 3M ESPE) was placed on the intaglio of both restorations. The restorations were air-dried and light-cured. Although light-curing was not required, per the manufacturer’s advice the author performed this step to improve bond strength.
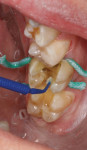
Meanwhile, the enamel rim of both preparations was etched with phosphoric acid for 15 seconds (Figure 6), while etching the dentin for 10 seconds (Figure 7). The double preparation was rinsed and blotted dry, taking care not to over-desiccate. The enamel and dentin of both preparations were scrubbed for 20 seconds each with Scotchbond Universal Adhesive, air-dried very thin for 5 to 10 seconds, and light-cured (Figure 8).
Adhesive resin cement (RelyX™ Ultimate Adhesive Resin Cement, 3M ESPE) was placed in the internal aspects of the inlays and seated. To set the cement, facilitate immediate flossing, and prevent contact closure, a tack-cure of a second or less was performed because of the light sensitivity of the resin cement (Figure 9). A thin, fine-tipped scaler followed by a soft pick was used to remove excess cement from the interproximal areas. The contacts were flossed with satin floss. The restorations were completed to the patient’s satisfaction (Figure 10 and Figure 11).
Conclusion
The evolution of dental materials and technologies advances dentistry by helping clinicians provide patients with indirect restorations fabricated chairside. CAD/CAM restorations created and placed using the Trifecta Method from 3M ESPE (eg, Lava Ultimate Restorative, Scotchbond Universal Adhesive, and RelyX Ultimate cement) can be more efficient to produce because the firing step is eliminated, and the cementation and adhesive application procedures are simple. Lava Ultimate Restorative eliminates many of the drawbacks associated with traditional dental ceramics by combining resin and nano-technologies, and produces CAD/CAM restorations that demonstrate exceptional fit, function, and esthetics.
About the Author
Rich Rosenblatt, DMD, is a CEREC basic trainer for Patterson Dental, a faculty member on the CERECdoctors.com website, and a CAD/CAM faculty member at the Scottsdale Center for Dentistry in Scottsdale, Arizona. He also founded the Northern Illinois CEREC study club, one of the largest CAD/CAM study clubs in the United States.
Disclosure
Dr. Rosenblatt received honoraria and material support from 3M ESPE for this article.
References
1. Shenoy A, Shenoy N. Dental ceramics: an update. J Conserv Dent. 2010 ;13(4):195–203.
2. DeLong R, Douglas WH. Development of an artificial oral environment for the testing of dental restoratives: bi-axial force and movement control. J Dent Res. 1983 ;62(1):32-36.
3. Fasbinder DJ, Dennison JB, Heys D, Lampe K. Clinical evaluation of CAD/CAM-generated polymer ceramic inlays. J Dent Res. 2001 ;80(AADR Abstracts #1882).