Effects of Mouthpiece Use on Airway Openings and Lactate Levels in Healthy College Males
Dena P. Garner, PhD; Erica McDivitt, MS
Abstract: Research has described the use of mouthpieces not only in preventing oral-facial injuries, but linking use to improvements in muscular strength and endurance. However, the mechanisms by which these improvements occur have not been elucidated. The purpose of this study was to understand possible physiological explanations for improvements in exercise performance with the use of a mouthpiece. Specifically, this study focused on differences in lactate levels after 30 minutes of endurance exercise with and without a mouthpiece. In addition, computed tomography (CT) scans were taken of the cross-sectional area of the oropharynx in each participant (N = 10) with and without a mouthpiece. CT scans showed a significant difference in mean width (28.27 mm with the mouthpiece vs 25.93 mm without the mouthpiece, P = .029) and an increase in mean diameter with a mouthpiece (12.17 mm vs 11.21 mm, P = .096). Lactate levels were lowered with the mouthpiece at 1.86 mmol/L vs 2.72 mmol/L without mouthpiece. This research suggests that there is an improvement in endurance performance that may be linked to improved airway openings resulting from the use of a mouthpiece. Future studies should continue to clarify the possible mechanisms for these exercise outcomes as well as to understand the optimal mandibular advancement to elicit these exercise improvements.
Mouthpieces have been used for a variety of contact sports to prevent oral-facial injury.1 In a review of dental trauma literature, Glendor2 noted that participation in sports is the greatest cause of dental injuries. To minimize injury associated with contact sport participation, the American Dental Association (ADA) recommends the use of mouthguards to protect against dental trauma during contact sports.3 In addition to the recommendation of the ADA, such sport-governing bodies as the National Alliance of Football Rules Committee have mandated mouthguards for use in high school football in the United States.4 The 2008-2009 National Athletic Association (NCAA) Sports Medicine Handbook mandates mouthguards for athletes involved with football, field hockey, lacrosse, and ice hockey in order to minimize dental trauma during these sports.5
While there is compelling research to support the use of mouthguards to protect against oral-facial injuries during contact sports, there is also research to suggest that mouthpieces may enhance performance. Smith6,7 noted that professional football players exhibited greater arm strength with properly fitted mouthguards that resulted in changes in bite patterns. Smith also noted that those players with the most extreme overbite corrected with a mouthguard experienced the greatest increase in strength. Specifically, he observed that with a properly adjusted mouthguard, 66% of the players exhibited significant strength improvements on the isometric deltoid press.7 He stated that the increase in strength with a properly fitted mouthguard was because of decreased pressure in the temporomandibular joint (TMJ).
Not only has improvement in strength been noted, but Garabee8 described improvement in 7 runners’ endurance and recovery with use of a mouthpiece to promote proper occlusion. He observed that when runners wore a wax bite mouthpiece, there was an increase in mileage: 64 to 100 miles per week in one runner, and 50 to 80-100 miles per week in another. He also noted quicker recovery times and decreased perceived exertion with use of the mouthpiece vs without the mouthpiece. Garabee hypothesized that this improvement was because of decreased stress with mouthpiece use that reduced clenching and grinding of teeth during exercise.
As the research evolved, the possible reasons for improvements in performance were elucidated by Francis and Brasher.9 In a study of 10 men and 7 women, they found that wearing a mouthpiece during 20 minutes of high intensity cycling resulted in improvements in ventilation (average of 43.13 l/min with mouthpiece vs 50.98 l/min without mouthpiece). They noted that this improvement may be from pursed lips breathing which results in greater oxygen saturation. Ugalde and colleagues10 confirmed that pursed lips breathing resulted in increased oxygen saturation in myotonic muscular dystrophy patients, while Tiep11 stated that such breathing results in increased tidal volume, carbon dioxide removal, and oxygen saturation.
Drawing from the research by Frances and Brasher,9 the possible reasons for improvements in endurance performance while wearing a mouthpiece provide insight into the physiological mechanisms that may be occurring. In order to first understand if there were improvements in performance, the authors’ laboratory conducted a series of pilot studies primarily to determine if lactate levels were affected by the use of a mouthpiece. If, as Frances and Brasher9 suggested, there was improvement in ventilation (ie, increased oxygen saturation and removal of carbon dioxide), then there could consequently be an improvement in lactate levels. The authors found that with 24 participants, there was improvement in lactate levels after 30 minutes of running on a treadmill at 85% of maximal heart rate (4.01 mmol/L with mouthpiece vs 4.92 mmol/L without mouthpiece).12
With this data suggesting a physiological improvement when a mouthpiece is used, the next step was to clarify further the possible reasons for this improvement. Trenouth and Timms13 found a positive association between the orpharyngeal airway opening and mandibular length, with a narrower opening associated with a shorter mandibular length. They cited previous research that suggested repositioning the mandible in an anterior position, thereby opening airways and promoting respiratory gas exchange to and from the lungs. In the literature associated with sleep apnea (where airway openings are diminished during sleep) and mouthpieces, it can be noted that there is significant improvement in airway openings for patients wearing a mouthpiece (a device that fits like a retainer and forces the lower teeth to relax in a forward position). Kyung and colleagues14 advanced the mandible forward with an oral appliance in 12 sleep apnea patients and found a reduction of the apnea-hypopnea index from 44.9 (without appliance) to 10.9 (with appliance). Gale and colleagues15 also found a significant improvement in mean airway opening with an anterior mandibular device while patients were supine in a conscious state. Specifically, Gale et al15 found that in 32 participants, the mean minimal pharyngeal cross-sectional area was increased 28 mm2 with the mouthpiece vs without the mouthpiece. Gao and collegues16 stated that for their participants, the mandibular advancement was 7.5% with a mouthpiece. They specifically found a significant opening of the oropharynx (P = .0258) and velopharynx areas (P = .006). Zhao et al17 also found that the velopharynx opening increased significantly with an adjustable mandibular custom mouthpiece, from 3.27 mm2 at 0 mm, to 8.45 mm2 at 2 mm, 17.73 mm2 at 4 mm, 24.45 mm2 at 6 mm, and 35.82 mm2 at 8 mm. This research suggests that the positioning of the mouthpiece will impact the degree of airway opening, with greater movement of mandible in a forward position resulting in a greater opening of the velopharynx. With the findings of previous studies as well as those in the authors’ laboratory, the hypothesis of this study is that there will be increased airway opening and a decrease in lactate levels with the use of a mouthpiece.
Methods
For this pilot study the authors recruited 10 participants to determine if there were differences in airway openings with the use of a mouthpiece and if there were differences in lactate levels after 30 minutes of running. The mouthpiece used was a boil and bite upper mouthpiece which had a greater bite opening distal vs proximal (EDGE, Bite Tech Inc, Minneapolis, MN). Participants were 18–21 years old, male, and from The Citadel. Each participant completed a computed tomography scan (i-CAT 3D Dental Imaging System, Imaging Sciences International, Hatfield, PA) with and without a mouthpiece, and the mean oropharynx area was measured in each. Participants then completed two 30 minute runs on the treadmill at 75%–85% of their maximum heart rate, and lactate levels were assessed at 0, 15, and 30 minutes of the run (Accutrend Lactate Analyzer, Sports Resource Group, Inc, Minneapolis, MN). Participants were randomly assigned a mouthpiece during each running trial and were required to refrain from exercising the day before and the day of testing. If participants failed to cooperate, they were asked to return on a subsequent day when compliance was met.
Results
The results of this study displayed a significant increase in mean width value of the oropharynx at 28.27 mm with the mouthpiece vs 25.93 mm without the mouthpiece (P = .029) (Figure 1). In addition, the mean value of the diameter was increased with a mouthpiece vs without a mouthpiece (12.17 mm vs 11.21 mm, P = .096) (Figure 1). As previous studies had suggested, the difference in lactate levels from pre- to post-exercise was lowered with the mouthpiece vs without the mouthpiece, though not at the level of significance (1.86 mmol/L with mouthpiece vs 2.72 mmol/L without mouthpiece) (Figure 2).
Discussion
There is a plethora of research to suggest that the upper airway of patients with sleep apnea is improved with a custom-fit oral device, due specifically to the forward movement of the mandible.13-18 Ryan and colleagues18 found improvement in the cross-sectional area of the velopharynx and in the apnea index with the use of a mandibular advancement oral appliance. Kyung et al14 also found reduced apnea-hypopnea indices, reducing the average index from 44.9 to 10.9 with an oral appliance.
Research continues to elucidate the degree of forward movement which would be most beneficial. In the research by Zhao and colleagues17 there was a range of improvement in the airway opening for participants: as the mandible was moved to a more forward position, the opening of the airway increased. It should also be noted that a specific mouthpiece was used for this present study. This particular mouthpiece offered minimal obstruction for the participants as they ran, yet was also designed to bring the mandible to a forward position. The mouthpiece was easy to use and mold to participants, who noticed no impairment in their breathing patterns during use. Further research to understand how different mouthpieces could affect the airway openings is warranted. Such studies should focus on measuring the movement of the mandible with the use of a mouthpiece and how this may affect airway openings in healthy participants.
The results of the study suggest that the use of a mouthpiece increases airway openings in these healthy participants and that the use of a mouthpiece while exercising may improve lactate levels. While previous studies with sleep apnea populations indicated improvements in airway openings with the use of a mouthpiece, there were limited data on a younger, healthy population (age 21 +/- 1.1 years). This study, however, is similar in a study by Gao and colleagues16 which took magnetic images of 14 healthy Japanese men (age 27.7 +/- 1.9 years). Gao et al16 saw improvements in airway opening with a custom-fit oral device that was specifically designed to move the mandible in a more forward position. Their study found significant improvements in the velopharynx (P = .0006) and the oropharynx (P = .0258), while the current study noted a significant improvement in the oropharynx width (P = .029).
Because of the financial costs of obtaining 2 CT scans for each participant, this study was limited in the number of participants. In addition, this was designed as a pilot study to determine: 1) if there were changes in airway openings with a mouthpiece in healthy participants; and 2) if this could translate into lowered lactate levels. The results suggest there may be a link, which could be one possible physiological explanation for performance improvement with a mouthpiece.
It may be surmised that the lack of significant differences in lactate levels in this study may be because of the low number of subjects, even though the trend was lower lactate levels with the mouthpiece vs no mouthpiece. As the authors’ previous study suggested (N = 24), lactate levels were significantly lower with a mouthpiece vs without a mouthpiece after 30 minutes of running on a treadmill (4.01 mmol/L mouthpiece vs 4.92 mmol/L no mouthpiece) (Figure 3).
Research has consistently noted the correlation between exercise fatigue and higher lactate levels. As one increases exercise intensity, the glycolytic pathway is highly utilized to meet energy needs. The end product of this pathway is the production of lactic acid. Lactic acid is broken down into lactate and hydrogen ions, and it is this increase of hydrogen ions that is negatively associated with metabolic processes, leading to fatigue.19-20 Thus, any mechanism which elicits lowered hydrogen levels resulting from lactic acid should increase an athlete’s time to fatigue. For example, if the pathways used during exercise rely more on oxygen, then lactate levels will be lowered. Yet understanding this link between lowered lactate levels and increased airway openings is a complex issue needing further investigation.12
Previous studies have noted that an improvement in breathing work rates leads to improved exercise time because of reduced oxygen uptake and ventilation.21-22 Specifically, if breathing mechanics are improved, then there is a decreased need for oxygen and blood flow by the respiratory muscles which typically require approximately 10% of the oxygen needs during strenuous exercise. Less blood flow to the respiratory muscles suggests an increase of blood flow to the exercising skeletal muscles, which would prolong time to fatigue. Specifically, Harms and colleagues found that when respiratory muscle work was decreased (via a proportional-assist ventilator), time to exercise exhaustion was increased in 76% of the trials by an average of 1.3 minutes (+/-0.4 minutes).22
Improvement in respiratory muscle function may not be the only mechanism that occurs during mouthpiece use. An interesting study by Kilding and colleagues23 examined response time of oxygen kinetics in endurance runners (N = 36) to understand its possible effect on a 5 kilometer time trial. An important finding from their study was that a faster phase II oxygen uptake kinetic response at the onset of moderate intensity exercise resulted in faster 5 kilometer performance. Thus, they concluded that those runners who had a shorter oxygen deficit at the onset of exercise (as indicated by shortened phase II response) could increase time to exhaustion, as indicated by the better 5 kilometer performance. Kilding cited previous work by Casaburi and colleagues24 stating a decrease in oxygen deficit at the onset of exercise could result in decreased lactate production, which could potentially improve endurance performance. This present study suggests mechanisms by which lactate production may be improved with increased airway openings, thereby improving oxygen kinetics such as lowered oxygen deficit and/or improved breathing work rates.
Conclusion
This study found that the use of a mouthpiece significantly improves airway openings in participants as compared with these same participants who do not wear the mouthpiece. In addition, lactate levels are improved when participants wear the mouthpiece vs when they do not wear the mouthpiece. One explanation for the decrease in lactate levels may be an improvement in oxygen kinetics at the onset of exercise or improvement in breathing work rates which may be prompted by enhanced airway openings with the use of a mouthpiece. Previous research in the field of mouthpiece use and its effect on human performance suggests that mouthpieces improve performance. However, these studies have been unable to elucidate the possible physiological mechanisms for this improvement. This research is novel in the area of human movement because it suggests a possible physiological explanation for the improvement in performance as noted by athletes. Further studies should focus on the reasons for these improvements, noting differences in jaw morphology and airway dynamics for individuals who may benefit from a mouthpiece during exercise and sport.
Disclosure
Dr. Garner has received an honorarium from Bite Tech Inc.
References
1. Hughston JC. Prevention of dental injuries in sports. Am J Sports Med. 1980;8(2): 61-62.
2. Glendor U. Aetiology and risk factors related to traumatic dental injuries—a review of the literature. Dent Traumatol. 2009;25(1):19-31.
3. ADA Council on Access, Prevention and Interprofessional Relations; and ADA Council on Scientific Affairs. Using mouthguards to reduce the incidence and severity of sports-related oral injuries. J Am Dent Assoc. 2006;137(12):1712-1720.
4. Bureau of Dental Education, American Dental Association. Evaluation of mouth protectors used by high school football players. J Am Dent Assoc. 1964;68: 430-442.
5. Klossner D, ed. 2008-2009 NCAA Sports Medicine Handbook. 19th ed. Indianapolis, IN: NCAA; 2008:94-95.
6. Smith S. Muscular strength correlated to jaw posture and the temporomandibular joint. N Y State Dent J. 1978;44(7):278-285.
7. Smith SD. Adjusting mouthguards kinesiologically in professional football players. N Y State Dent J. 1982;48(5):298-301.
8. Garabee WF. Craniomandibular orthopedics and athletic performance in the long distance runner: a three year study. Basal Facts. 1981;4(3):77-81.
9. Francis KT, Brasher J. Physiological effects of wearing mouthguards. Br J Sports Med. 1991;25(4):227-231.
10. Ugalde V, Breslin EH, Walsh SA, et al. Pursed lips breathing improves ventilation in myotonic muscular dystrophy. Arch Phys Med Rehabil. 2000;81(4):472-478.
11. Tiep BL. Pursed lips breathing—easing does it. J Cardiopulm Rehabil Prev. 2007;27(4):245-246.
12. Garner DP, McDivitt E. The effects of mouthpiece use on salivary cortisol and lactate levels during exercise. MSSE Suppl. In press.
13. Trenouth MJ, Timms DJ. Relationship of the functional oropharynx to craniofacial morphology. Angle Orthod. 1999;69(5):419-423.
14. Kyung SH, Park YC, Pae EK. Obstructive sleep apnea patients with the oral appliance experience pharyngeal size and shape changes in three dimensions. Angle Orthod. 2005;75(1):15-22.
15. Gale DJ, Sawyer RH, Woodcock A, et al. Do oral appliances enlarge the airway in patients with obstructive sleep apnea? A prospective computerized tomographic study. Eur J Orthod. 2000;22(2): 159-168.
16. Gao X, Otsuka R, Ono T, et al. Effect of titrated mandibular advancement and jaw opening on the upper airway in nonapneic men: a magnetic resonance imaging and cephalometric study. Am J Orthod Dentofacial Orthop. 2004;125(2): 191-199.
17. Zhao X, Liu Y, Gao Y. Three-dimensional upper-airway changes associated with various amounts of mandibular advancement in awake apnea patients. Am J Orthod Dentofacial Orthop. 2008;133(5):661-668.
18. Ryan CF, Love LL, Peat D, et al. Mandibular advancement oral appliance therapy for obstructive sleep apnoea: effect on awake caliber of the velopharynx. Thorax. 1999;54(11): 972-977.
19. Green HJ. Neuromuscular aspects of fatigue. Can J Sport Sci. 1987;12(3): 7S-19S.
20. Westerblad, H, Lee JA, Lännergren J, Allen DG. Cellular mechanisms of fatigue in skeletal muscle. Am J Physiol. 1991;261(2 pt 1): C195-C209.
21. Harms CA, Wetter T, McClaran SR, et al. Effect of respiratory muscle work on cardiac output and its distribution during maximal exercise. J Appl Physiol. 1998;85(2):09-618.
22. Harms CA, Wetter TJ, St Croiz CM, et al. Effect of respiratory muscle work on exercise performance. J Appl Physiol. 2000;89(1):131-138.
23. Kilding AE, Winter EM, Fysh M. Moderate-domain pulmonary oxygen uptake kinetics and endurance running performance. J Sports Sci. 2006;24(9): 1013-1022.
24. Casaburi R, Storer TW, Ben-Dov I, Wasserman K. Effect of endurance training on possible determinants of VO2 during heavy exercise. J Appl Physiol. 1987;62(1): 199-207.
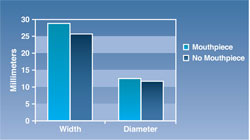 | 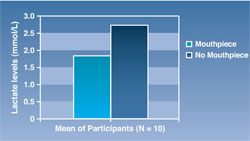 | ||
| Figure 1 Mean values of oropharynx width and diameter with and without a mouthpiece. | Figure 2 Mean lactate levels after 30 minutes of running at 75%-85% of maximum heart rate. | ||
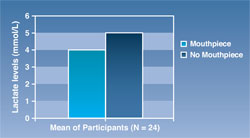 | Figure 3 Mean lactate levels after 30 minutes of running at 85% of maximum heart rate. | ||
| |||



