Piezoelectric Ultrasonic Bone
Surgery: Benefits for the Interdisciplinary Team and Patients
Jeff Thomas, DDS, FICD, FACD
Abstract
Esthetics, technology, and an increase in the number of dentists performing complex therapies have driven interdisciplinary teams to develop higher levels of treatment planning and treatment options. With the increase in accessible education, such as study clubs, private education centers, courses at universities, and publications like this one, generalists and specialists have been stimulated to improve their team interactions. Piezoelectric bone surgery is a relatively new ultrasonic technology that facilitates a greater number of more complex procedures and positive outcomes for dentists and their patients. This article provides team members with an overview of how this technology may be of assistance with patient management.
Piezoelectric bone surgery is an ultrasonic technology that can be a great asset for the interdisciplinary team. Dr. Keith Rossein1 described the importance of the team as it relates to implant dentistry in Series 1 of Functional Esthetics & Restorative Dentistry, and this topic has been addressed by many others over the years. While many great educators developed the concept of interdisciplinary dentistry in academic environments, it is likely the work of Dr. Ralph O'Connor2 that has had the greatest effect on interdisciplinary dentistry as it relates to teams not practicing "under one roof." While everyone would benefit by reading the entire O'Conner article, in essence he defined interdisciplinary dentistry as:
The delivery of dental care that results from the most excellent treatment plan for a patient with complex dental needs through simultaneous interaction and treatment by all involved providers, who make the agreement to deliver their therapy in a mutually supportive fashion in order to meet or exceed the patient's vision.
When dental teams function in this manner, piezoelectric bone surgery becomes a valuable tool for obtaining excellent results in patient care.
Piezoelectric Bone Surgery
Ultrasound technology has been used in medicine and dentistry for many years, and in many different applications. In 2005, the US Food and Drug Administration extended the use of ultrasonics in dentistry to include bone surgery. This technology, known as piezoelectric bone surgery, has been used commercially in Europe since 2000, a year after it was invented by an Italian periodontist, Dr. Tomaso Vercellotti. In the United States, Vercellotti first published on this topic in 2000.3 The invention of and the extensive research on piezoelectric bone surgery by Dr. Vercellotti has resulted in an intense interest in this surgical technology.
Most dentists have used an ultrasonic scaler at some point in their careers to help in the removal of plaque and calculus from root structure. The ultrasonic (or ultrasound) frequency, as the name implies, is a frequency above the audible range for humans, usually above 20 kHz. In dental applications, the frequencies used range from 24 kHz to 36 kHz, the frequency range capable of cutting mineralized tissue. With piezoelectric ultrasonics, the frequency is created by driving an electric current from a generator over piezoceramic rings, which leads to their deformation. The resulting movement from the deformation of the rings sets up a vibration in a transducer and/or amplifier, which creates the ultrasound output. These waves are transmitted to a handpiece tip, also called an insert, where the longitudinal movement results in the cutting of osseous tissue by microscopic shattering of the bone (Figure 1). A typical unit is similar to an implant drilling system with a control panel, irrigant, and a handpiece with wire/tubing.
The technology's inventor, Dr. Vercellotti, developed it because of his desire to change bone surgery procedures to make results more predictable, improve healing, minimize trauma, and provide greater safety for patients.4 He also wanted to decrease stress for the surgeon, simplify the armamentarium, and as a result, facilitate more therapies for the interdisciplinary team.
This technology also is being used in medicine with very favorable results. Kotrikova and colleagues5 reported use of the Piezosurgery® unit (Piezosurgery®, Inc, Columbus, OH) in cranial surgery for osteoplasty and osteotomy. They noted that the dura mater was protected after the cranial bone cuts, even in surgical procedures typically deemed a high risk for perforation and damage to the dura. In 2006 Hoigne et al6 reported the use of the Piezosurgery unit in hand surgery to avoid nerve lesions, a frequent complication of this surgery. They noted that patients had excellent healing with the absence of neurovascular disturbances, and stated that the device had "great potential in the field of hand and spinal surgery."
Clinical Performance
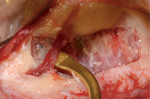
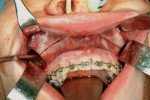
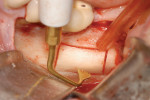
Piezoelectric units provide clinicians with the ability to cut the mineralized tissue selectively. The units' low kHz frequency allows the soft tissue to "move" with the vibrating insert, thus preventing incision or damage to soft tissue. With higher ultrasonic frequencies, this tandem movement does not occur, resulting in incision or other damage to soft tissue.4 This "selective cutting action" is very desirable in bone surgery. For example, with piezoelectric bone surgery, a lateral sinus window access can be created without cutting the Schneiderian membrane. Other soft tissues benefiting from this selective cutting action in surgery are nerves, blood vessels (Figure 2), and mucosa (Figure 3).
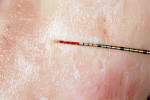
Another characteristic of Piezosurgery units is the microvibration of the inserts. These microvibrations allow clinicians to make precise and narrow bone incisions (Figure 4 and Figure 5), with cuts as small as 0.5 mm to 0.7 mm. The surgeon also benefits from good tactile sensation. Bone saws and dental drills do not have this level of control, precision, and tactile sensation because greater force often is needed with many rotary instruments and/or there is partial or complete loss of control of some parts of the cutting surface at any given time. This loss of control can result in damage to underlying structures, especially soft tissue, such as nerves and the sinus membrane in dentistry and other tissues in medical surgery. The microvibrations and selective cutting action therefore result in greater patient safety.4
Piezosurgery units use chilled saline as an irrigant, which serves several functions. Because the irrigant is chilled, it provides a cooling effect to the insert and mineralized tissue to help prevent overheating of the bone and bone cells. This cooling combined with the specific waveform of the unit's insert cutting edge causes minimal inflammation or necrosis in the bone.7 The combined effect of the insert's waveform and irrigation efficiently clears cut bony particles, resulting in very good cutting efficiency at low power. Traditional ultrasonic units do not have such a waveform movement or other appropriate movement of the insert. This allows cut bone particles to accumulate and overheating of the uncut bone and its fragile cells to occur, resulting in necrosis.
Piezoelectric Bone Surgery and the Interdisciplinary Team
Piezoelectric bone surgery helps the interdisciplinary team by helping its patients. As noted in the previous section, patients benefit from faster and more predictable healing, reduced surgical trauma, and greater safety. In the author's opinion and experience, piezoelectric bone surgery not only reduces the team surgeon's armamentarium, but also facilitates the adoption of more complex procedures. This equates to more options for patients, likely, with high-quality reconstructive and restorative results.
As shown in Figure 5, harvesting bone block grafts for lateral and vertical ridge augmentation is greatly simplified with the angled saw-like insert. This tip eases the making of precise bone incisions, especially the inferior cut, with minimal risk of injury to the inferior alveolar nerve and blood vessels. Piezosurgery technology was the reason the author returned to performing block graft procedures. In the author's experience, the harvesting procedure became greatly simplified, much less stressful, and more predictable. Comments and results such as these were reported by Happe8 in 2007 on 40 consecutive block graft procedures.
As reported by Blus and Szmukler-Moncler,9 ridge splits to facilitate increasing horizontal ridge dimensions, as well as to idealize implant placement (Figure 6), can be performed with piezoelectric bone surgery. Bone incisions can be made at slightly less than 1 mm, which results in minimal loss of osseous tissue during these procedures. With the ability to expand the osseous ridge by 1 mm to 2 mm easily, the interdisciplinary team can augment ridges and place implants simultaneously, especially in posterior areas but also in select cases in the esthetic zone.
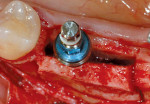
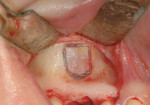
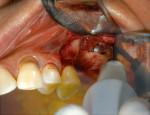
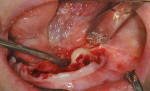
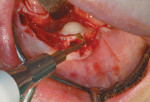
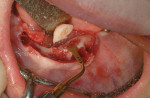
Subantral augmentations (also known as sinus lift procedures), both crestal and lateral approaches, are facilitated with piezoelectric bone surgery. Figure 7A and Figure 7B show an osteoplasty performed in the window area with a Piezosurgery unit. The sinus graft was filled exclusively with the collected autogenous bone, and the device's implant tips were delicately used to prepare the implant osteotomy site. The elephant foot type insert rapidly assisted in the initial separation and elevation of the Schneiderian membrane over the first 2 mm to 2.5 mm at the edge of the window osteotomy (Figure 8). By using piezoelectric bone surgery, these three steps were performed in a single surgical procedure, along with a simultaneous removal of the primary tooth.
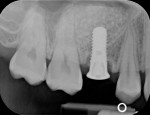
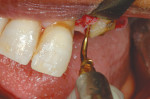
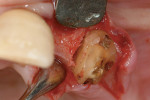
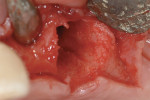
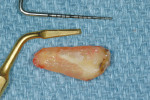
Because soft tissue is not cut with this technology, there is preservation of the sinus membrane and a minimal risk of perforations.10,11 Management of septa and other anatomic challenges also is improved. Piezoelectric bone surgery also can assist with the extraction of roots to minimize trauma to the hard and soft tissues. Atraumatic extraction can be extremely useful to the interdisciplinary team because with minimal extraction trauma, implants can be placed in sites that may otherwise need grafting. Figure 9A, Figure 9B, Figure 9C and Figure 9D show a case in which a fractured canine with very thin facial bone, no mobility, and dense proximal bone was removed easily. This atraumatic extraction allowed for simultaneous implant placement with an attachment to help retain a recently fabricated partial denture. Traumatic extraction and thin facial bone would present a challenge to the team to do extensive bone grafting under a removable prosthesis without any retention on that side of the dental arch.
New inserts, specific to a variety of implant systems, are being developed for implant site preparation. Preliminary results presented by Dr. Vercellotti at the 2007 American Academy of Periodontology Annual Meeting show biological advantages related to faster healing and less bone trauma using Piezosurgery implant tips as compared with conventional implant instrumentation. Reports on this are forthcoming, and additional research is needed.
Piezoelectric bone surgery also is helpful in harvesting bone graft particles and chips, which often can be accomplished in the area of the surgical focus, preventing the need for a second surgical site for autogenous donor material. Piezosurgery also is useful with apical surgery and uncovering impacted teeth, all without the risk of damaging adjacent soft tissue structures. Many other procedures, such as removal of tori (Figure 10A, Figure 10B and Figure 10C), ridge reduction, and bone cuts associated with various orthodontic surgical treatment modalities,12 are possible for the interdisciplinary team to incorporate into their treatment plans.
Conclusion
Piezoelectric bone surgery is a less traumatic and safer bone surgery technology than conventional technology, especially drills. It is very useful technology for the dental surgeon who performs more advanced bone surgery procedures for the interdisciplinary team, and piezoelectric bone surgery most likely will facilitate more complex procedures for the patients of the team.
As a note to users and future users, piezoelectric bone surgery should be considered only after completion of hands-on training and a course on the use of the technology to insure proper results in patient care. Before performing piezoelectric bone surgery in a clinical setting, a full day of training is strongly recommended.
Acknowledgement
The author is grateful to Dr. Tomaso Vercellotti for his contributions to this article, including the use of some images, as well as his generous sharing of knowledge and his passion for this technology.
Disclosure
In the past, Dr. Thomas has been paid by Piezosurgery, Inc to provide full-day and partial-day educational courses in the clinical use of piezoelectric ultrasonic bone surgery. He receives no other financial compensation by Piezosurgery, Inc nor is a stockholder or has any other financial arrangements with the company.
References
1. Rossein K. Teaming up for successful implant dentistry. Functional Esthetics & Restorative Dentistry. 2007;1(2):8-10.
2. O'Connor RV. The exciting world of interdisciplinary dentistry. Int J Periodontics Restorative Dent. 2000;20(4):334-335.
3. Vercellotti T. Piezoelectric surgery in implantology: a case report—a new piezoelectric ridge expansion technique. Int J Periodontics Restorative Dent. 2000;20(4):358-365.
4. Vercellotti T. Technological characteristics and clinical indications of piezoelectric bone surgery. Minerva Stomatol. 2004;53(5):207-214.
5. Kotrikova B, Wirtz R, Krempien R, et al. Piezosurgery—a new safe technique in cranial osteoplasty. Int J Oral Maxillofac Surg. 2006;35(5):461-465.
6. Hoigne DJ, Stübinger S, Von Kaenel O, et al. Piezoelectric osteotomy in hand surgery: first experiences with a new technique. BMC Musculoskelet Disord. 2006;7:36.
7. Vercellotti T, Crovace A, Palermo A, et al. The piezoelectric osteotomy in orthopedics: clinical and histological evaluations. Mediterranean Journal of Surgical Medicine. 2001;9:89-95.
8. Happe A. Use of a piezoelectric surgical device to harvest bone grafts from the mandibular ramus: report of 40 cases. Int J Periodontics Restorative Dent. 2007;27(3):241-249.
9. Blus C, Szmukler-Moncler S. Split-crest and immediate implant placement with ultrasonic bone surgery: a 3-year life-table analysis with 230 treated sites. Clin Oral Implants Res. 2006;17(6):700-707.
10. Vercellotti T, De Paoli S, Nevins M. The piezoelectric bony window osteotomy and sinus membrane elevation: introduction of a new technique for simplification of the sinus augmentation procedure. Int J Periodontics Restorative Dent. 2001;21(6):561-567.
11. Wallace SS, Mazor Z, Froum SJ, et al. Schneiderian membrane perforation rate during sinus elevation using piezosurgery: clinical results of 100 consecutive cases. Int J Periodontics Restorative Dent. 2007;27(5):413-419.
12. Vercellotti T, Podesta A. Orthodontic microsurgery: a new surgically guided technique for dental movement. Int J Periodontics Restorative Dent. 2007;27(4):325-331.
About the Author
Jeff Thomas, DDS, FICD, FACD is an adjunct professor in the Department of Periodontics at the University of North Carolina School of Dentistry at Chapel Hill. He is a member of the American Academy of Esthetic Dentistry and is a Fellow, International Team for Implantology (ITI). He maintains a full-time private practice limited to periodontics in New Bern, North Carolina, with a focus on interdisciplinary dentistry and anterior implants. He has used piezoelectric bone surgery in his practice for more than 4 years.